The Influence of Intrapleural Fibrinolytic Therapy on the Treatment Outcome of Complicated Pneumonia in Children
The Influence of Intrapleural Fibrinolytic Therapy on the Treatment Outcome of Complicated Pneumonia in Children
Milosevic K *1,2, Radulovic S 1, Jahic K 3, Jovanovic B 1, Rsovac S.1,2
1. University Children’s Hospital, Belgrade, Serbia.
2. Faculty of Medicine, University of Belgrade, Serbia.
*Correspondence to: Milosevic Katarina, Department of Pulmology and allergology, Faculty of Medicine University of Belgrade, University Children’s Hospital, Belgrade, Serbia.
ORCID: 0000-0002-5806-9284.
Copyright
© 2023 Milosevic Katarina. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 10 August 2023
Published: 01 September 2023
Abstract
Introduction: Pneumonia is the most common infectious lung disease characterized by inflammation and infiltration of lung tissue by microorganisms. The most common viral cause of pneumonia in children is a respiratory syncytial virus, while the most common bacterial cause is Streptococcus pneumoniae. The clinical picture of complicated pneumonia is developed in 3% of children, which includes the presence of local and systemic complications (pleural effusion, pleural empyema, lung abscess, bacteremia, etc.). Antibiotic therapy, drainage and intrapleural fibrinolytic therapy are methods used for treatment of complicated pneumonia.
Objective: The objective of our study was to evaluate the impact of intrapleural fibrinolytic therapy on the treatment outcome of complicated pneumonia in children.
Material and methods: This was a retrospective study conducted on 69 patients with complicated pneumonia, treated at the Department of Pulmonology and Allergology, University Children's Hospital in Belgrade, during the period from January 2015 to December 2022.
Results: The majority of patients of the study population were male (58%), with an average age of 54 months (range: 1-228). Pleural effusion, lung abscess, pleural empyema, necrotizing pneumonia and other complications were developed in 85.5% of patients with complicated pneumonia. Most of the patients had a thoracic drain (ICC drain) placed on the tenth day after the onset of illness, because up to that time they had been managed with conservative treatment in another secondary care institution. If the Children's Hospital was the first institution where the patient was hospitalized with the signs of complicated pneumonia, most of the patients had a pleural drain placed on the first or second day of hospitalization. A highly statistically significant difference regarding the need for intrapleural fibrinolytic therapy was observed in the group of patients who developed pleural empyema in comparison with the group of patients whose primary disease was not complicated by the development of pleural empyema.
Conclusion: Pleural empyema, necrotizing pneumonia and lung abscess are the most serious local complications of pneumonia. The early diagnostics of complicated pneumonia proved to be critical for the final treatment outcome and the total length of stay. The prognosis of complicated pneumonia, with the use of adequate and timely therapy, is generally good, which is also supported by the fact that there were no death outcomes in the studied population.
Keywords: pneumonia; complications of pneumonia; pleural empyema; intrapleural fibrinolytic therapy
Abbrevations
ICC -drain intercostal drain
RSV respiratory syncytial virus
VATS video-assisted thoracentesis
rTPA recombinant tissue plasminogen activator
LE leucocyte count
CRP C reactive protein
UCH University Children’s Hospital.
The Influence of Intrapleural Fibrinolytic Therapy on the Treatment Outcome of Complicated Pneumonia in Children
Introduction
Pneumonia is the most common infectious lung disease (there is also aspiration pneumonia, which is not an infectious lung disease) characterized by inflammation and infiltration of the lung tissue by microorganisms. In about 40-60% of cases, the causal factors of pneumonia in children are viruses (a respiratory syncytial virus, adenoviruses, parainfluenza virus, human metapneumovirus, corona virus etc.) (4). The Pneumonia Etiology Research for Child Health (PERCH) study showed that a respiratory syncytial virus (RSV) is the most common cause of pneumonia in children aged 1-59 months (12). About 10-30% of cases are caused by bacteria (Streptococcus pneumoniae, Haemophilus infuenzae type b, Staphylococcus aureus etc.) (5). Atypical causes (Mycoplasma pneumoniae, Chlamydophila pneumoniae, Legionella pneumophila etc.) are the main causes of pediatric pneumonia in about 10-20% of cases (6). Pneumonia remains the single biggest cause of morbidity and mortality in children from the age of 28 days of life (i.e. after a neonatal period) to the age of 5 years (1, 11).
Although the majority of children affected with pneumonia do not develop complications, a certain number of children (3%) develop the clinical picture of complicated pneumonia according to the literature data (3, 11). Complicated pneumonia should be suspected in every child with lung inflammation who does not respond to the appropriate antibiotic therapy within 48-72 hours (11). The clinical picture of complicated pneumonia includes the presence of local (pulmonary) and systemic complications. Local complications include a parapneumonic effusion, pleural empyema, necrotizing pneumonia and lung abscess. Systemic complications include sepsis and septic shock, metastatic infection, multiple-organ failure, acute respiratory distress syndrome, disseminated intravascular coagulation and death (2). The choice of antibiotics for therapy of complicated pneumonia should be based on the international and local guidance documents, considering the local patterns of resistance to antibiotics, clinical experience, as well as the possibility of the presence of comorbidity in children (16, 17). The first-line treatment for complicated pneumonia includes penicillin and beta- lactam antibiotics with antistaphylococcal agents (7). A parapneumonic effusion is the most common manifestation of complicated pneumonia in children (11). It occurs in 57% of cases as a pneumonia complication in the adult population (Sahn 1993), progressing to empyema in 5% to 10% of patients (Strange 1999). A pleural empyema is defined as the presence of the pus content in the pleural space and in the largest number of cases occurs as a complication of the bacterial pneumonia (8). In children, who developed complications of pneumonia such as pleural effusion and empyema, Streptococcus pneumonia was isolated in the highest number of cases (13, 14, 15). Light’s criteria (ph≤7.2, glucose≤40mg/dl and LDH≥1000 U/L in the pleural punctate) define the complicated pleural effusion which also includes a pleural empyema, and thus are used as one of the criteria for pleural drain procedure (9). Thoracic drainage is performed through an intercostal catheter (ICC) with parenteral empiric antibiotic therapy, as well as the symptomatic therapy (8). A simple ICC drain procedure is often inefficient because of the presence of fibrous septae in the pleural space, which hinder the free drainage of the infected pleural fluid. The literature data indicate that insufficient efficacy of the ICC drainage preceded the need for video-assisted thoracentesis (VATS) or rather, decortication in order to remove the fibrous septae and the pus content (8). Video-assisted thoracentesis (VATS) and decortication are surgical methods of treatment. The non-surgical method of treatment includes the use of intrapleural chemical fibrinolysis.
The fibrinolytic agents, including streptokinase, urokinase, alteplase and recombinant tissue plasminogen activator (rTPA) are inserted into the intrapleural space through an ICC catheter (8). The lung abscess, as an important complication of pneumonia, is an infection of the lung parenchyma manifested by pus-filled cavity (abscess) formation in the lung tissue. The most common causes of the lung abscess are Streptococcus pneumoniae and Staphylococcus aureus. The treatment includes parenteral use of antibiotics, drainage and ultimately, a surgical intervention (10). The aim of this retrospective study was to estimate the influence of intrapleural fibrinolytic therapy on the outcome of treatment for complicated pneumonia in children.
Material and Methods
This was a retrospective study conducted on 69 patients with complicated pneumonia. The patients were treated at the Department of pulmonology and allergology of the University Children’s Hospital, during the period from January 2015 until December 2022. The patient data were obtained using the Heliant Health health information system. Heliant health information system is a centralized registry of clinical data which contains clinical and laboratory patient data. The criteria for patient inclusion were as follows: 1) patients with the diagnosis of complicated pneumonia on the basis of clinical data, laboratory analyses, radiological methods and/or cytological analyses, 2) patients who simultaneously underwent laboratory tests, ultrasonography, X-ray and CT examinations. The criteria for exclusion from the study were: 1) patients younger than 1-month-old, 2) patients with the diagnosis of malignant tumor, 3) patients with lymphproliferative diseases. The study was conducted in accordance with the rules of the Research Ethics Committee of the University Children’s Hospital in Belgrade and in accordance with the principles of Helsinki declaration (1989).
The set of data collected for each patient included: age (in months), gender, absolute leukocyte count (Le), C-reactive protein (CRP) level, proof of the previous hospitalization (other than Children’s Hospital), duration of previous hospitalization, radiography during the previous hospitalization, antibiotic therapy administered during the previous hospitalization, day of illness during admission to the University Children’s Hospital (UCH), radiography at UCH, ultrasonography and CT examination at UCH, antibiotic therapy administered at UCH, proof of the intercostal (ICC) drain insertion at UCH, day of illness when an ICC drain was placed at UCH, day of hospitalization when an ICC drain was placed at UCH, proof of the performed decortication and intrapleural fibrinolytic therapy, total length of hospital stay (other than UCH and at UCH) and disease outcome.
Statistical analysis
The data analysis was performed in SPSS system. The demographic and clinical characteristics of the patients are presented through the basic descriptive statistics, including the mean value, median, standard deviation, range, percentage and percentiles. Non-parametric statistical methods were used for statistical analysis: Mann-Whitney test, hi-square test and Spearman’s range correlation coefficient. The p-value, less than 0.05, was considered statistically significant.
Results
The research covered 69 patients with complicated pneumonia who fulfilled the inclusion criteria. During the period from January 2015 until December 2022 the number of hospitalized patients with pneumonia was 568. Out of this number, 69 (12.15%) patients developed the clinical picture of complicated pneumonia. The majority of patients in the study population were male (58%) (Figure 1). The average patient age was 54 months (range: 1-228). The majority of patients with complicated pneumonia were hospitalized at the University Children’s Hospital (UCH) on the seventh day after the onset of illness (range: 2-90) (Table 1).
Out of the total number of subjects with complicated pneumonia, only 16% of hospitalized patients were not in need of thoracic drainage. Most patients had an ICC drain placed on the tenth day after the onset of illness because until then they had been on the conservative treatment in the other healthcare facility of the secondary level (range: 3-38). If the University Children’s Hospital was the first facility where the patient was hospitalized, most of them had a pleural drain placed on the second day of hospitalization (range: 1-21) (Table 1).
Pleural effusion, lung abscess, pleural empyema, necrotizing pneumonia and other complications were developed in 85.5% of patients with complicated pneumonia, whereby the lung abscess was verified in 13% of cases, pleural empyema in 37.7%, and pleural effusion in 40% of hospitalized patients. Necrotizing pneumonia was verified in 3% of patients, while 1.5% of patients were diagnosed with a bronchial fistula. Intrapleural fibrinolytic therapy was indicated in 31.9% of patients, while decortication was conducted in 18.2% of patients. Monitoring of the inflammatory process was verified on the basis of the follow-up measurement of laboratory indicators (absolute count of leukocytes, C reactive protein level) (Table 1). The mean length of hospitalization was 17 days (range: 3-191) (A Table 1).
Regarding the lung abscess development, a statistically significant difference was noted between the group of patients who were given a thoracic drainage at a later stage after the onset of illness (the patients who were initially treated only with the conservative therapy in the secondary level facilities) and the group of patients who underwent ICC drainage within the first two days after the beginning of hospitalization (the patients who were initially admitted to the Children's Hospital at the Department of pulmonology and allergology) (p=0.026) (Figure 2). A statistically significant difference was noted regarding the lung abscess development between the group of patients who did not receive intrapleural fibrinolytic therapy and decortication, and the group of patients who underwent the mentioned procedures (p1= 0,028, p1=0,002).
A highly statistically significant difference regarding the need for provision of intra-pleural fibrinolytic therapy was noted in the group of patients who developed a pleural empyema in comparison with the group of patients whose primary disease was not complicated by development of pleural empyema (p?0,001). A highly statistically significant correlation was noted between the day of illness at the time of admission to the University Children's Hospital and the day of illness when an ICC drain was inserted (p?0,001) (Figure 3).
Discussion
One of the greatest challenges for a clinician treating patients with pneumonia is how to prevent the occurrence of complications of the primary disease and decrease the mortality of these patients. Out of the total number of hospitalized patients with the diagnosis of pneumonia at the University Children's Hospital, 69 (12.15%) patients developed the picture of complicated pneumonia. Our research results differ from the results in the available studies, in which 3% of the patients developed the clinical picture of complicated pneumonia (3,11). The inadequate use of oral antibiotics (the inadequate recommended dose of amoxicillin and oral therapy with third-generation cephalosporin as the first-line treatment) could account for this increased incidence of complicated pneumonia. Complications of pneumonia such as pleural effusion, lung abscess, pleural empyema, necrotizing pneumonia etc. were developed in 85.5% of patients, whereby the lung abscess was verified in 13% of cases, pleural empyema in 37.7%, and pleural effusion in 40% of hospitalized patients, which makes these results consistent with those of previous studies (2). These results may be explained by late referral of patients into the tertiary healthcare facility, i.e. University Children's Hospital in Belgrade (UCH). This is suggested by the fact that majority of patients were hospitalized at UCH between the 7th and 11th day after the onset of illness, although they had already at the beginning of their illness fulfilled the criteria for the use of thoracic drainage at other facility. The need for intercostal drainage (ICC drainage) was shown in 84% of patients. Such a high number of patients can be explained by severity of the clinical picture at the time of admission to the UCH, as well as by indications and recommendations for performing ICC drainage (11, 22, 23). The clinical indicators which suggest the need for ICC drainage include localization of the lung parenchymal consolidation, increased duration of pneumonia, an inadequate response to the antibiotic therapy within 48-72 hours, presence of comorbidities and presence of anaerobic microorganisms in the blood culture. Radiological criteria include an effusion which involves over 50% of the thorax and the presence of fibrous septae on the basis of radiography, ultrasonography or CT findings (23). The mean length of stay was 17 days, which is in accordance with the results of the available studies (18, 19, 20). Kurt et al. conducted a small-scale prospective study with 18 patients and obtained the mean length of stay of 13 days, which can be explained by the fact that the treatment was carried out in a highly specialized healthcare center, and that the United States has a very specific health-care system (21).
Intrapleural fibrinolytic therapy is indicated in case of the presence of fibrous septae within the pleural cavity which hinder adequate drainage, as well as for the therapy of complicated pleural empyema (11). Our study demonstrated a highly statistically significant difference regarding the need for provision of intrapleural fibrinolytic therapy, in the group of patients who developed a pleural empyema, in comparison with the group of patients whose primary disease was not complicated with the development of pleural empyema, which is in accordance with the available studies (8, 11, 18, 24). The use of intrapleural fibrinolytic therapy significantly improved drainage of the pleural fluid in our patients, prevented further development of local and systemic complications, reduced the length of hospital stay and decreased the need for parenteral use of antibiotics, and also reduced the cost of treatment.
Conclusion
Pleural empyema, necrotizing pneumonia and lung abscess are the most severe local complications of pneumonia. The early diagnostics of complicated pneumonia proved to be crucial for the ultimate outcome of treatment and the total length of hospital stay. Complicated pneumonia in children should be treated in a tertiary healthcare facility, or in secondary healthcare facilities which are equipped with adequate technical and human resources for provision of pleural drainage and intrapleural fibrinolytic therapy. The early provision of pleural drainage and intrapleural fibrinolytic therapy significantly decreased the probability of occurrence of pneumonia complications in children. The development of complicated pneumonia should be suspected in every patient who does not respond to the antibiotic therapy within 48-72h. Microbiological verification of causal agents of complicated pneumonia remains a challenge, which is also indicated by a negligible number of our patients who had adequate microbiological diagnostics, and thus this information had to be excluded from the research. The previous studies suggest that routine immunization with PCV13 vaccine significantly decreased the burden of complicated childhood pneumonia. Our further research will be expanded with the data on immunization of children with PCV13 vaccine and its influence on the development of pneumonia complications, the length of hospital stay and the ultimate outcome. The prognosis of complicated pneumonia, with the use of an adequate and timely therapy, is generally good, which is also supported by the fact that there was not one death case registered in the studied population. The use of innovative therapeutic procedures in the treatment of complicated pneumonia in children did not lead to a significant decrease of the recovery time of these patients, in outpatient settings.
Reference
1. GBD 2016 Lower Respiratory Infections Collaborators. Estimates of the global, regional, and national morbidity, mortality, and aetiologies of lower respiratory infections in 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Infect. Dis. 2018; 18:1191–210.
2. Pabary R, Balfour-Lynn IM. Complicated pneumonia in children. Breathe. 2013; 9:210–22.
3. Legg J, Rampton C. British Thoracic Society pediatric pneumonia audit. National audit period: 1 November 2016–31 January 2017. BTS. 2018;
4. Jain S, Williams DJ, Arnold SR, Ampofo K, Bramley AM, Reed C, et al. Community-acquired pneumonia requiring hospitalization among U.S. children. N Engl J Med. 2015; 372(9):835-845.
5. Scott JA, Wonodi C, Moïsi JC, Deloria-Knoll M, DeLuca AN, Karron RA et al. The definition of pneumonia, the assessment of severity, and clinical standardization in the Pneumonia Aetiology Research for Child Health study. Clin Infect Dis. 2012; 2:109-116.
6. Michelow IC, Olsen K, Lozano J, Rollins NK, Duffy LB, Ziegler T, et al. Epidemiology and clinical characteristics of community-acquired pneumonia in hospitalized children. Pediatrics. 2004; 113(4):701-707.
7. Waterer GW, Somes GW, Wunderink RG. Monotherapy may be suboptimal for severe bacteremic pneumococcal pneumonia. Arch Int Med. 2001; 161:1837–1842.
8. Altmann ES, Crossingham I, Wilson S, Davies HR. Intra-pleural fibrinolytic therapy versus placebo, or a different fibrinolytic agent, in the treatment of adult parapneumonic effusions and empyema. Cochrane Database Syst Rev. 2019; 2019(10):e002312
9. Fischer GB, Mocelin HT, Andrade CF, Sarria EE. When should parapneumonic pleural effusion be drained in children? Paediatr Respir Rev. 2018; 26:27-30.
10. Madhani K, McGrath E, Guglani L. A 10-year retrospective review of pediatric lung abscesses from a single center. Ann Thorac Med. 2016; 11(3):191-6.
11. Benedictis FM, Kerem E, Chang AB, Colin AA, Zar JJ, Bush A. Complicated pneumonia in children. Lancet. 2020; 396(10253):786-798.
12. O’Brien K, Baggett HC, Brooks WA, Feikin DR, Hammitt HL, Higdon MM, et al. Causes of severe pneumonia requiring hospital admission in children without HIV infection from Africa and Asia: the PERCH multi-country case-control study. Lancet. 2019; 394:757–79.
13. Erlichman I, Breuer O, Shoseyov D, Cohen-Cymberknoh M, Koplewitz B, Averbuch D et al. Complicated community acquired pneumonia in childhood: different types, clinical course, and outcome. Pediatr Pulmonol. 2017; 52:247-54.
14. Grijalva CG, Nuorti JP, Zhu Y, Griffin MR. Increasing incidence of empyema complicating childhood community-acquired pneumonia in the United States. Clin Infect Dis. 2010; 50:805–13.
15. Strachan RE, Cornelius A, Gilbert GL, Gulliver T, Martin A, McDonald T, et al. Bacterial causes of empyema in children, Australia, 2007–2009. Emerg Infect Dis. 2011; 17:1839-45.
16. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, et al. Executive summary: the management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clin Infect Dis. 2011; 53:617–30.
17. Harris M, Clark J, Coote N, Fletcher P, Harnden A, McKean M, et al. British Thoracic Society guidelines for the management of community acquired pneumonia in children: update 2011. Thorax. 2011; 66(suppl 2): ii1–23.
18. Segerer FJ, Seeger K, Maier A, Hagemann C, Schoen C, Streng A, et al. Therapy of 645 children with parapneumonic effusion and empyema—a German nationwide surveillance study. Pediatr Pulmonol. 2017; 52:540–47.
19. Picazo J, Ruiz-Contreras J, Casado-Flores J, Negreira S, Del Castillo F, Hernandez-Sampelayo T, et al. Laboratory-based, 2-year surveillance of pediatric parapneumonic pneumococcal empyema following heptavalent pneumococcal conjugate vaccine universal vaccination in Madrid. Pediatr Infect Dis J. 2011; 30:471–474.
20. Grisaru-Soen G, Eisenstadt M, Paret G, Schwartz D, Keller N, Nagar H, et al. Pediatric parapneumonic empyema: risk factors, clinical characteristics, microbiology, and management. Pediatr Emerg Care. 2013; 29:425–429.
21. Kurt BA, Winterhalter KM, Connors RH, Betz BW, Winters JW. Therapy of parapneumonic effusions in children: video-assisted thoracoscopic surgery versus conventional thoracostomy drainage. Pediatrics. 2006; 118:547–553.
22. Balfour-Lynn IM, Abrahamson E, Cohen G, Hartley J, King S, Parikh D, D Spencer, et al. BTS guidelines for the management of pleural infection in children. Thorax. 2005; 60:1-21.
23. Sahn SA. Diagnosis and management of parapneumonic effusions and empyema. Clin Infect Dis. 2007; 45(11):1480-6.
24. Barthwal MS, Marwah V, Chopra M, Garg Y, Tyagi R, Kishore K, et al. A Five-Year Study of Intrapleural Fibrinolytic Therapy in Loculated Pleural Collections. Indian J Chest Dis Allied Sci. 2016; 58(1):17-20.
Figure 1
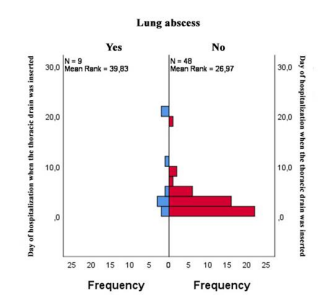
Figure 2
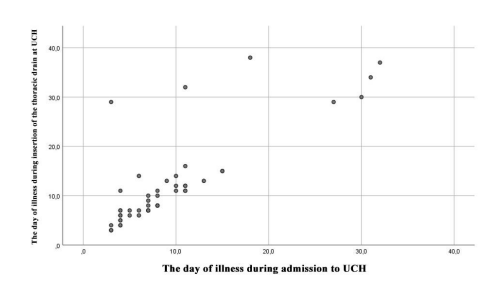
Figure 3
