Prevalence of Vitamin D Deficiency Among Obese Children from 1-13 Years and its Relation to Metabolic Syndrome Risk Factors
Prevalence of Vitamin D Deficiency Among Obese Children from 1-13 Years and its Relation to Metabolic Syndrome Risk Factors
Dr. Layla Abdulrahem 1, Dr. Rand Mudhafar Abdulghafoor MD *2
1. M.B.Bch, M.SC(Pediatrics), Doctorate degree (Paediatrics). Pediatrics Endocrinology, Latifa Hospital - Dubai Health Authority.
2. Pediatric Resident, DHA, Latifa Hospital - Dubai Health Authority.
*Correspondence to: Dr. Rand Mudhafar Abdulghafoor, Pediatric Resident, DHA, Latifa Hospital - Dubai Health Authority.
Copyright
© 2023: Dr. Rand Mudhafar Abdulghafoor. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 18 August 2023
Published: 01 September 2023
Abstract
Obesity and vitamin D deficiency are common among children all over the world. The aim of this study is to identify the prevalence of vitamin d deficiency among obese children and better identify the association between vitamin D deficiency and metabolic syndrome risk factors in those children and compare the result with the available published data. This study is a quantitative retrospective study from single tertiary center (Latifa hospital) over 1 year period. The sample of the study consists of N=100 respondents of age between 1-13 years. Among 100 children 55% were female child and 45% were male.
All Patients received vitamin D supplement after the 1st visit to the clinic. The Vitamin D sufficiency in children before treatment is 26.2%, and Vitamin D deficiency is 23.7%. While the Vitamin D insufficiency before treatment is 50%. After the treatment vitamin D sufficiency is 70.0%. The Vitamin D deficiency after the treatment is 7.5%, and insufficiency 22.5%. The vitamin D sufficiency remarkably improved after the treatment. The Insufficiency level of Vitamin D before and after treatment has changed from high to low.
The effect of Vitamin D deficiency in other studies shows a slight difference in the level of BMI, similar is the case with the results of the present study, which shows slight reduction in the obesity of children after the treatment. The impact of Vitamin D in reducing the Triglycerides levels among children after treatment is remarkable. The HDL level among obese children after treatment increased. The HBA1C among children before treatment and after treatment also changed, as the pre-diabetics were greater in number before treatment and after the treatment, the number of children having pre-diabetics levels reduced to normal. The results of the study showed that Vitamin D is effective in the manner of reducing obesity rates and the risk of developing high blood pressure, hypertriglyceridemia and diabetes, which which are risk factors for developing metabolic syndrome.
Prevalence of Vitamin D Deficiency Among Obese Children from 1-13 Years and its Relation to Metabolic Syndrome Risk Factors
Introduction
Prevalence of obesity in children has risen remarkably worldwide. Despite a known genetic contribution, the increase in pediatric obesity has been attributed mainly to diet and sedentary lifestyle. Obesity is one of the most important modifiable risk factors for the prevention of number of chronic diseases. The resulting socioeconomic and public health burden due to its consequences (development of hypertension, diabetes mellitus, social discrimination etc.) is growing steeply, Although obese individuals are thought to be adequately nourished, micronutrient deficiencies have been identified to be prevalent possibly due to the large fat mass acting as a reservoir for fat-soluble vitamins and nutrients or due to consumption of food rich in calories but poor in other nutrients [1].
Vitamin D is a fat-soluble vitamin with a half-life of 4–6 weeks and its deficiency was observed in obese individuals in several studies although the exact reason is not known, Several possibilities have been suggested to explain the lower 25(OH)D levels observed in children with obesity, including decreased sun exposure due to sedentary lifestyle, poor diet(skipping breakfast, increased soda intake, and increased juice intake) and increased clearance of 25(OH)D due to storage in adipose tissue [1].
Several definitions are important for clarity in the discussion of Obesity, Vitamin D deficiency and metabolic syndrome risk factors. First The following definitions are used to categorize weight status for children between 2 and 20 years of age: Underweight – BMI <5th percentile for age and sex, Normal weight – BMI between the 5th and <85th percentile for age and sex, Overweight – BMI between >85th and 95th percentile for age and sex, and Obese – BMI ≥95th percentile for age and sex. [2].
Significant controversy has been associated with determining standards of vitamin D sufficiency, insufficiency, and deficiency. the following standards for defining vitamin D status in healthy children and adolescents, based on serum concentrations of 25OHD as per Global Consensus Recommendations on Prevention and Management of Nutritional Rickets: Vitamin D sufficiency – 20 to 100 ng/mL (50 to 250 nmol/L), Vitamin D insufficiency – 12 to 20 ng/mL (30 to 50 nmol/L and Vitamin D deficiency – <12 ng/mL (<30 nmol/L) [3].
Definition of metabolic syndrome in pediatrics In 2007, a consensus report was published by the IDF group, including three age groups: 6 to < 10, 10 to < 16 and 16 + years (adult criteria). Based on this report, obesity is defined as waist circumference or BMI ≥ 90th percentile, ≥ 150 mg/dl for triglycerides, < 40 mg/dl for HDL and < 50 mg/dl in females older than 10, ≥ 130 mmHg for systolic and ≥ 85 mmHg for diastolic blood pressure and fasting plasma glucose ≥ 100 mg/dl or known type 2 diabetes. The rationale of using absolute numbers as cut-offs is based on the heterogeneity of clinical, biochemical and hormonal values during childhood and adolescence, as well as, on the large diversity of proposed percentile cut-offs of different definitions [4]. The summary of the International Diabetes Federation (IDF) definition for pediatric metabolic syndrome ( MeS) is outlined in table 1.
Table 1
Vitamin D deficiency and obesity among children have become a major health problem worldwide. The classical and most widely understood biological functions of vitamin D involve calcium homeostasis and bone mineralization; however, vitamin D is also necessary for many other cellular processes and vitamin D receptor (VDR) has been identified in nearly every cell type [5]. Data accumulated over the last decade have led researchers to speculate that the vitamin D deficiency epidemic may be a major contributor to many obesity-associated complications such as the metabolic syndrome and diabetes [6]. Metabolic syndrome is a clinical condition that consists of several cardio metabolic risk factors such as obesity, hypertension, dyslipidemia, and insulin resistance that occur in obese children [7,8]. Previous research has found evidence for an association between metabolic syndrome and cardiovascular risk factors (impaired fasting glucose, low-density lipoprotein (LDL) cholesterol, hypertriglyceridemia) among children and adolescents [9]. Obese children were at greater risk of vitamin D deficiency and metabolic risk factors than normal weight children [10]. Previous cross-sectional studies found that low serum 25(OH)D level was associated with abnormal glucose metabolism and increased HOMA-IR levels dyslipidemia [11], impaired fasting glycaemia , low plasma adiponectin levels , increased systolic blood pressure [12], decreased high-density lipoprotein-cholesterol and accelerated atherosclerosis in obese children aged 5–20 years when compared to normal weight children[13]. Previous researches also showed that severe hypovitaminosis D was associated to a worse HbA1c in diabetic patients and to higher insulin requirement, but this metabolic effect cannot be explained by an immune role alone as Vitamin D may act directly on β cell, promoting insulin secretion and regulating calcium homeostasis or through a peripheral action, increasing the insulin sensitivity of target cells, or regulating the activation of several calcium-dependent enzymes involved in glucose metabolism. [14].
Since Vitamin D deficiency and metabolic syndrome risk factors are growing in numbers and as Obese children are increasingly becoming a major portion of the population, it is important to have our national figures about the prevalence of vitamin D deficiency among obese children and the evidence supporting the association between vitamin D deficiency and metabolic syndrome for this population. Moreover, it is important to compare our national figures of with international figures to take an idea where we are standing and help in improvement of our clinical practice with better identification and management of obesity related metabolic derangement and vitamin D deficiency.
Research Question
What is the prevalence of vitamin D deficiency among obese children and what is the association between vitamin D deficiency and metabolic syndrome risk factors in those patients who visited Latifa Hospital pediatrics endocrine clinic in Dubai between January 2018 to January 2019.
Hypotheses
Vitamin D deficiency is very common in obese children and it can lead to metabolic syndrome risk factors; high BP, Lipid profile, fasting blood glucose and HBA1C, and by correcting the deficiency with Vitamin D supplementation it can Improve.
Aims of the study
The aim of this study is to identify the prevalence of vitamin d deficiency among obese children and better identify the association between vitamin D deficiency and metabolic syndrome risk factors in those children in Latifa hospital. Obesity and vitamin D deficiency represent major health problems among UAE children, and have been linked to chronic diseases. Obese children are at risk of developing vitamin D deficiency, which appears to have negative influences on energy homeostasis, impeded bone mineralization, insulin resistance and inflammation.
Evidence supporting the association between vitamin D deficiency of obese children and metabolic syndrome has not specifically been studied in early childhood in the UAE. The mechanisms through which vitamin D deficiency is associated with metabolic syndrome in obese children needs further elucidation. This will give physicians in the UAE particularly and in the other Arab countries in general a practical intuition in understanding the roles vitamin D may play in obesity and obesity-associated metabolic conditions with a particular emphasis on pediatric obesity in this part of the region and can help in better identification and management of obesity related metabolic syndrome and vitamin D deficiency.
Objectives of the study
- To Identify the prevalence of Vitamin D deficiency among obsess children
- To Assess the relation between Vitamin D deficiency and metabolic syndrome risk factors in obsess children.
- To Identify the effect of Low Vitamin D Levels On weigh, BMI, Blood pressure, HBA1C level, Blood glucose levels (fasting) and lipid profile.
- To compare between Obese children who have low vitamin D levels and those with normal Vitamin D levels in relation to their weight BMI, blood pressure, HBA1C level, Blood glucose levels (fasting) and lipid profile.
- To assess the effect of treating/ raising Vitamin D deficiency on weight BMI, blood pressure, HBA1C level, Blood glucose levels (fasting and random) and lipid profile
Research Design and Methods
Study Design
This is a retrospective, descriptive, record-based study that is conducted in the Latifa Hospital in Dubai health Authority. Patients’ medical records will be reviewed by the main investigator.
Site
The study was done in Latifa Hospital, which was established in 1986, and is a government organization under Dubai Health Authority. It has a specialized Pediatric unit that offers its services to the population of Dubai as well as the Northern Emirates including locals and expatriates.
Population and Study Sample
Target population: Obese children presenting to Pediatrics endocrinology clinic in Latifa hospitals. The sample of the study consists of N=100 respondents.
Inclusion criteria
- Children from 1-13 year of age
- Diagnosed with childhood Obesity
- Visited pediatrics endocrinology clinic in Latifa hospital between 01/01/2018 to 01/01/2019.
Exclusion criteria
- Children visited pediatrics endocrinology clinic outside the study period.
- Children with clinical and/or laboratory evidence of hypothyroidism or other endocrine disorders.
- Children with clinical and/or laboratory evidence of genetic or metabolic disorders.
Study period
Data will be collected between 01/01/2018 to 01/01/2019 for patients visited pediatrics endocrinology clinic in Latifa hospital.
Sources of Data Collection
Data is collected from medical files and electronic records from SALAMA system, using ICD coding for Obesity for children visited pediatrics endocrinology clinic in Latifa hospital between 01/01/2018 to 01/01/2019. Data collection will include MRN/PID number, Demographic details (age and gender), weigh, BMI, vitamin D levels, Blood pressure, HBA1C level, Fasting Blood glucose levels and lipid profile.
Data Analysis Strategies
- Data is collected and the data entry is done on the Excel sheet file, which is later converted in SPSS for further analysis.
- The Prevalence of Vitamin D deficiency and its distribution according to the socio- demographic characteristics (age, gender) of the sample was analyzed.
- Each variable (weigh, BMI, vitamin D levels, Blood pressure, HBA1C level, Blood glucose levels (fasting) and lipid profile will be added to the Excel Sheet and it will be analyzed to percentages.
- All variables will be added to a chart and will be summarized in order from the highest to the lowest percentage.
- Variables will be compared to the 1st results (before treatment) in Children with improved vitamin D levels (by receiving vitamin D supplementation) to assess the effect of treatment on metabolic syndrome risk factors.
Time frame
1-2 years
- Literature review 1-2 month
- Proposal/Ethical approval 1-2 months
- Data collected 2-4 months
- Data analysis 3-6 months
- Writing paper 3-6 months
Scientific and ethical approval
The study was undertaken after receiving approval from the Dubai Scientific Research Ethics Committee.
Results
Profile of the respondents:
Figure 1 Age and Gender of the respondents
The above-mentioned Graph shows the age of the respondents with respect to their gender. The Age is divided into two groups, 1-5 years of age, and 6-13 years of age. The Female respondents of the research of age between 1 to 5 are 9 (45%), and of age between 6 to 13 are 46 (57.5%). The Male respondents of the research with age between 1 to 5 years are 11 (55%) and between 6 to13 years are 34 (45.2%). The maximum number of the male and female respondents of the research belong to age above 6 years and less than 13 years.
In the Table, the percentage of obese children having vitamin D deficiency is given according to their Age and Gender. The Age has two groups, 1-5 years of age, and 6-13 years of age. The results show that The Insufficiency of Vitamin D in Children of Age 1-5 Years among Female 3 (5.6%) and Male 3 (7.7%). Children of Age 1-13 years have having Vitamin D Insufficiency Female 25 (46.3%), and Male 11 (28.2%). The total Female having Vitamin D insufficiency are 28 (51.9%), and Total Male having Vitamin D insufficiency are 14 (35.9%).
Vitamin D deficiency in Age 1-5 among Female is 0% and Male 2 (5.1%). In Age between 6- 13 years, Vitamin D deficiency among Female is 13 (24.1%) and Male 5 (12.8%). The Total Females having vitamin D deficiency are 13 (24.1%), and Male 7 (17.9%).
The Sufficiency of Vitamin D Sufficiency in Age 1-5 years among Female 5 (9.3%), and Male 6 (15.4%), and age 6-13 years among Female 8 (14.8%), and 12 (30.8%). The Total Female having Vitamin D insufficiency are 13 (24.1%), and Male 18 (46.2%).
Figure 1 Vitamin D level as Insufficiency, Sufficiency, and Deficiency in terms of Gender and Age of the respondents
Figure 2 Vitamin D level before treatment
The Vitamin D level among children of age between 1-5 years: sufficiency 12 (60%), Deficiency 2 (10%), and Insufficiency 6 (30%). The Vitamin D level between the age of 6-13
years: Sufficiency 21 (26.2%), Deficiency 19 (23.7%), and insufficiency 40 (50%). The level of Vitamin D sufficiency between the age of 1-5 years is high, and between the age of 6-13 years the level of vitamin D Insufficiency is high.
Figure 3 HBA1C level before treatment
The HBA1C level among the age of 1-5 years: Pre-diabetes 4 (20%) and Normal 16 (80%). In age between 6-13 years: pre-diabetes 7 (8.75%) and Normal 73 (91.2%). Majority of the children of age between 1-5 years and 6-13 years have Normal HBA1C level.
Figure 4 Fasting Blood Glucose level before treatment
Fasting blood glucose level among children of age between 1-5 years of age having Vitamin D sufficiency with High FBG 15.7% (3), Vitamin D deficiency with High FBG 10.5% (2). The children having vitamin D insufficiency have High FBG 16% (12) and vitamin D deficiency children have High FBG 14.8% (11).
Figure 5 Triglycerides level before treatment
The Triglycerides is normal in children of age between 1-5 years to 20 (100%), and between the age of 6-13 years, the Triglycerides level is high in 5 (6.25%) and Normal in 75 (93.7%). The Triglycerides level is normal to a maximum extent in both age groups up to 100%.
Figure 6 HDL Cholesterol level before treatment
The HDL cholesterol level in children of age between 1-5 years is Low in 5 (25%) and High 15 (75%). The HDL cholesterol level in children of age between 6-13 years is low in 19 (23.75%) and High in 61 (76.25%). The HDL cholesterol level in high in both groups up to 77%.
Figure 7 Body mass index before treatment
The Body Mass Index (BMI) level in children of age between 1-5 years: Overweight is 1 (5%) and Obese 19 (95%). The BMI level in children of age between 6-13 years, Normal 2 (2.5%), Overweight 4 (5%), and Obese 74 (92.5%). In BMI the level of Obesity is higher in both groups up to 92%.
Figure 8 Systolic Pressure before treatment
The systolic blood pressure has no accuracy in statistical terms, but the level of systolic in Age between 1-5 Years, Normal 2 (10%) and Hypertension 18 (90%), and in age between 6-13 years, Normal 5 (5.2%), Prehypertension 2 (2.5%) and Hypertension is 73 (91.2%). In both age groups, the Hypertension is highest to 91.2%.
Figure 9 Diastolic pressure before treatment
The Diastolic level in children of age between 1-5 years is Normal 20 (100%), and in children of age between 6-13 years, Normal 77 (96.2%) and Hypertension 3 (3.75%). The Diastolic Pressure is Normal to a maximum extent in both age groups up to 96.2%.
Table 2 Body Mass Index and Vitamin D levels in Obese Children
The table shows the Vitamin D level in comparison to Body Mass Index preselected as ‘obese’ in terms of age between 1-5 years and 6-13 years. The results show that obese children having Vitamin D insufficiency of age 1-5 years are 14.3% (6) and of age 6-13 years 85% (36). Obese children with Vitamin D deficiency of age 1-5 years are 10% (2) and age 6-13 years 90% (18). The Children having Vitamin D sufficiency in age 1-5 years are 35% (11) and 6-13 years are 64% (20). The results show that Vitamin D Insufficiency in Obese children is higher before treatment.
Table 3: Systolic Pressure in Obese children Before Treatment
In the above table, the systolic pressure with respect to age and gender is given. It shows that High blood pressure among the children of age 1-5 years in Female and Male is 17 (20%) and the high blood pressure in children of age between 6-13 years among Female is 68 (80%). These results show the systolic pressure in obese children. Only 1% of the population have prehypertension in both groups and the level of normal systolic pressure among both groups is 7%.
Table 4 Diastolic Pressure in Obese children Before Treatment
In Table, Diastolic pressure is given as per Age and gender. Among children of age 1-5 years, Normal diastolic pressure is 19 (21.1%), and among children of age 6-13 years 71 (78.9%). The hypertension is 3 (4.1%). While there is no child of prehypertension. The diastolic pressure results show that hypertension is 4.1% and only 3 children have it. The Normal diastolic pressure is 96.8% (90).
Table 5: Vitamin D Level and High Hba1c Among Obese Children
The table shows the HBA1C level as Normal and Pre-Diabetes. Although the Diabetic scale showed no value in the table. The Vitamin D deficiency, insufficiency and sufficiency are shown with respect to Age groups (1) 1-5 years and (2) 6-13 years. The results of the study show that obese children having Vitamin D insufficiency among the age group 2: Normal HBA1C is 33 (91.7) and Pre-diabetes 3 (16.7%). The Vitamin D deficiency with normal HBA1C is 15 (83.3%) and Pre-diabetes are 3 (8.3%). The Overall results shows that Pre- diabetics children with Vitamin D insufficiency are less in number.
Figure 10 Vitamin D level and High HBA1C among Obese Children
The Pre-Diabetes HBA1C level among obese children with Vitamin D insufficiency is 27.2%, Vitamin D deficiency 27.2% and Vitamin D sufficiency 9%.
Table 6: Vitamin D Level And Fasting Blood Glucose In Obese Children
In the table above, the fasting blood Glucose has two levels (1) Normal, (2) High. The Body Mass Index has three levels (1) Normal Weight (2) Over Weight (3) Obese, in which level 3 is selected in the above table. The Age has Two groups (1) 1-5 years, and (2) 6-3 years.
The results show that Obese children having Vitamin D insufficiency between the age of 6-13 years with high Fasting blood glucose are 12 (33.3%) and Normal blood Glucose are 24 (66.7%). The Children having Vitamin D deficiency with High Fasting Blood Glucose level is 11 (61.1%) and with normal Fasting blood glucose are 7 (38.9%).
Figure 11 Graphical representation of Obese Children with High Fasting Blood Glucose levels
The graphical representation shows that BMI scale is selected as 'obese' and HBA1C level as 'high'. The results show that respondents with Vitamin D insufficiency are 42.8%, Deficiency 42.8% and Sufficiency 14.2% respectively.
Table 7: Vitamin D Deficiency, Insufficiency And High Triglycerides Level In Obese Children
The results of the table have specific BMI as obese with Triglycerides level as high. The results show that among the respondents of age between 6-13 years, with vitamin D insufficiency, High Triglycerides are 3 (4.3%) and low is 33 (44.5%). With vitamin D deficiency the Low triglyceride level is 17 (22.97%) and high is 3 (4.6%). The results show that majority of the respondents among Vitamin D deficiency and Insufficiency have Normal level of Triglycerides among obese children.
Figure 12: Triglycerides level and Vitamin D level in Obese Children
In the graph given above, the BMI level is selected as; Obese children only with High and Low Triglycerides level in comparison to Vitamin D deficiency and insufficiency before treatment.
Table 8: Vitamin D Deficiency or Insufficiency and HDL Level in Obese Children
Figure 1 HDL Level in Obese Children with Vitamin D Insufficiency
The percentage of obese children having vitamin D insufficiency of age between 1-5 years with low HDL is 2 (4.76%), Normal 4 (66.7%). The Children of age between 6-13 years having Vitamin D insufficiency with Low HDL are 6 (14.2%), Normal 30 (71.43%).
Figure 2 HDL Level in Obese Children with Vitamin D Deficiency
The Obese children with Vitamin D deficiency with Low HDL is 0% and 2 (10%) have normal HDL level. In age group 6-13 years, the obese children with Vitamin D deficiency with Low HDL is 8 (40%) and Normal HDL level is 10 (50%).
Table 9: Vitamin D level comparison before and after treatment
Vitamin D level before treatment, the results shows that insufficiency is 46%, Deficiency 21% and Sufficiency 33%. Vitamin D level after treatment, the results shows that Insufficiency is 29%, Deficiency 6%, and Sufficiency 65%.
The Vitamin D insufficiency, Deficiency before treatment is greater than after treatment. The Vitamin D sufficiency before treatment is lesser than after treatment. There is a change between the three levels of vitamin D, as Vitamin D sufficiency after treatment is greater, while Insufficiency are Deficiency are lower as compared to before treatment results.
Figure 14: Vitamin D level before treatment
A comparative Graph of 'Before treatment' shows the Vitamin D level. There are two age groups 1-5 years, and 6-13 years. In the first Age group of 1-5 years, there are 20 respondents. The Vitamin D sufficiency is 12 (60%), Vitamin D deficiency is 2 (10%), and Vitamin D insufficiency is 6 (30%).
In Second age group of 6-13 years, there are 80 respondents. The Vitamin D sufficiency is 21 (26.2%) Vitamin D deficiency is 19 (23.7%), and Vitamin D insufficiency is 40 (50%).
Figure 15: Vitamin D level after treatment
A comparative Graph of 'After treatment' shows the Vitamin D level. There are two age groups 1-5 years, and 6-13 years. In the first Age group of 1-5 years, there are 20 respondents. The Vitamin D sufficiency is 9 (45%), and Vitamin D Insufficiency is 11 (55%).
In the second group there are 80 respondents. In Second age group of 6-13 years, the Vitamin D sufficiency is 56 (70%), Vitamin D deficiency is 6 (7.5%), and Vitamin D insufficiency is 18 (22.5%).
Table 10 Paired T-Test Before and After Treatment
A paired sample t-test was conducted to compare the values of before and after treatment. The results of the study show that there was a significant difference between Vitamin D level before treatment (M=1.87, SD=.88) and after treatment (M=1.41, SD=.60) under the conditions of t (99) =7.34, p=.000 The HBA1C before treatment (M=1.1, SD=.31) and after treatment (M=1.0, SD=.25) shows a minute difference as the value of HBA1C after treatment decreased. The Fasting blood Glucose level before treatment (M=1.0, SD=.21) and after treatment (M=1.9, SD=.28) shows a significant difference between the values, where p=.000. The fasting blood glucose level decreased after the treatment. The Triglycerides before treatment (M=1.0, SD=.21) and after treatment (M=1.9, SD=.14) shows a significant difference between Triglycerides values before and after treatment, with p=.000. The HDL Cholesterol before treatment (M=1.7, SD=.42) and after treatment (M=1.83, SD=.37) shows insignificant difference as the Cholesterol level before the treatment was low, and after the treatment increased. There is a minute difference in the BMI level before and after treatment.
Table 11 Vitamin D Impact Before and After Treatment
In the above table, Vitamin D impact on HBA1C, FBG, Triglycerides, HDL, and BMI. The results show that HBA1C Pre-diabetes before treatment were 11%, and after treatment 7%. The HBA1C normal are 89% and after treatment 93%. The Fasting Blood Glucose level, before treatment the Normal Glucose 64.5% and after treatment, Normal Glucose percentage is 72.0%. Before treatment, the High Glucose level is 35.5%, which reduced to 28.0% after treatment. The triglycerides level is divided into Normal and High. Before treatment the ratio of normal triglycerides is 95.0% and after treatment, the ratio of normal triglycerides is 98.0%. The ratio of High Triglycerides before treatment is 5.0% and after treatment 2.0%. The HDL cholesterol level is either low or high. The Low HDL before treatment is 24.0% and after treatment it reduced to 17.0%. The High HDL before treatment is 76.0% and after treatment it increased to 83.0%. The results before treatment shows that BMI (Body Mass Index) of the respondents before treatment and after treatment changes. The Normal weight before treatment is 2.0% and after treatment increased to 3.0%. The overweight children before treatment were 5.0% and after treatment it increased to 7.0%. The obese children were 93% and after treatment, it decreased to 90.0%. This study observed that if vitamin D level is lower, the values are worse.
Discussion
Several studies have reported the association between obesity and vitamin D deficiency worldwide [15]. There are no previous studies on the prevalence of vitamin D deficiency in children with obesity in the UAE. Some published studies were from USA and different part of Asia like Seri Lanka and Turkey and they were single center–based studies with small sample size and with no focus on the effect of vitamin D deficiency on the risk factors of metabolic syndrome; Thus, they have been inadequate to outline the problem nationwide.
In this study the Male children were 45 (45.0%) and female children were 55 (55.0%). These children were categories as 1-5 years of age and 6-13 years of age. The Children of age 1-5 years were 20 (20.0%) and the children of age 6-13 years were 80 (80%). The greater number of the children of the study were above >6 years of age.
The high BMI level before treatment in obese children is 93.0% and after the vitamin D treatment it reduced to 90.1%. The BMI level also changed to a minimum point after the treatment. The results show that BMI level reduced after the treatment. Although several factors have impact on the BMI level.
A study conducted by Soudarssanane (2006) shows BMI is directly attached to the blood pressure. It is evident that BMI predisposes the adolescent to higher blood pressure and hypertension [19]. Although a study shows that there is no possible relationship between Vitamin D and BMI, as there are no explicit results on the vitamin D increase or decrease with obesity. But the study also shows that overweight and obese children have limited Vitamin D. Other researches show that vitamin D does have effect on obesity in healthy and unhealthy population [20].
The percentage of normal Triglycerides level before treatment among children is 93.75% and High Triglycerides 6.25%. The normal HDL cholesterol level among children before treatment is 76.2% and low HDL is 23.7%. It further shows that Vitamin D has positive impact on the reduction of high triglycerides among children. The results of Triglycerides before and after treatment shows that Normal Triglycerides level improved after the treatment and the High triglycerides level reduced. Another research shows that a low serum vitamin D levels in children is associated with high triglyceride levels [22, 23, 24].
The fasting blood glucose before treatment among obese children is high in 35% of children and after the treatment the ratio lowers to 28%. It shows that the number of patients having high fasting blood glucose levels decreased after the vitamin D treatment. The Normal Fasting Blood Glucose level prevails after the treatment, which shows that Vitamin D has positive impact on Glucose level. Also, the High Blood Glucose level decreased after treatment.
The High fasting blood glucose in obese children with Vitamin D insufficiency is 48.0%, with Vitamin D deficiency 24.0% and with vitamin D sufficiency 27.0%. The Pre-diabetics obese children have vitamin D sufficiency 14.2%, vitamin D deficiency 42.8% and Vitamin D insufficiency 42.8%. The study conducted by Adikaram and Samaranayake (2019) shows that there is no significant relationship between Vitamin D deficiency and fasting blood glucose and lipid profile [18].
Normal HBA1C before treatment is 91.2% and Pre-diabetics 8.75%. The results showed the impact of vitamin D before and after treatment on the metabolic syndrome risk factors. Vitamin D has a significant impact on HBA1C. It shows that normal HBA1C among children before treatment is less and after the treatment the normal HBA1C increased in number of children. The Pre-diabetic HBA1C children before treatment were greater in number and after the vitamin D treatment their number decreased.
Before treatment the High HDL cholesterol among children is 76% and after the vitamin D treatment it increased to 83%. The research results show that HDL cholesterol level increased after the Vitamin D treatment. In a study The vitamin D deficiency is directly related to the low HDL cholesterol level [21].
The results of the systolic pressure show that the level of High BP in obese children of age 1-5 years before treatment is 20% (17) and the in children of age between 6-13 years the level is 80% (68). Only 1% of the population have prehypertension in both groups and the level of normal systolic pressure among both groups is 7%. The diastolic pressure results show that High BP is 4.1% and only 3 children have it. The Normal diastolic pressure is 96.8% (90).
Almost all the variables go on change before and after treatment. This study observed that some variables have minute change. The HBA1C level has minimal change after treatment, similar is the case with HDL cholesterol increase to a minute point after the treatment.
The Vitamin D sufficiency in children before treatment is 26.2%, and Vitamin D deficiency is 23.7%. While the Vitamin D insufficiency before treatment is 50%. After the treatment vitamin D sufficiency is 70.0%. The Vitamin D deficiency after the treatment is 7.5%, and insufficiency 22.5%. The vitamin D sufficiency remarkably improved after the treatment. The Insufficiency level of Vitamin D before and after treatment has changed from high to low. The prevalence of vitamin D deficiency and insufficiency in the study before treatment is high. Among female children before treatment the Vitamin D Insufficiency is 51.9%, Male 35.9%, which shows that vitamin D insufficiency among female children is higher than male children. The Vitamin D deficiency among female children is 24.1% and male 17.9%, which shows that vitamin D deficiency among female children is higher than male children. The Vitamin D sufficiency before treatment among female children is 24.1% and male 46.2%, which shows that vitamin D sufficiency among female children is lesser than male children. The over all results shows that Vitamin D levels are lower in female children than Male children. The results showed that Female children have greater Vitamin D insufficiency than Male children. Similar is the case with Vitamin D deficiency among female children greater than male children.
The results show that Vitamin D has positive impact on several factors. The HBA1C level after vitamin D treatment shows remarkable change as the level of HBA1C dropped in children after vitamin D intake. The fasting blood glucose level at normal condition in children increased after taking vitamin D supplement. The high blood glucose level in children after vitamin D intake reduced, which shows that vitamin D has impact on the fasting blood glucose level. The triglycerides level after vitamin D intake decreased in children. The HDL cholesterol level increased in children after vitamin D intake. The ratio of obese children after vitamin D intake is lower than the results of before treatment. Which shows that vitamin D intake has effect on obesity as well.
The similar results have been reported in a study conducted by Salek and Hashemipour (2008). According to the results, the vitamin D deficiency is much higher among the young children age group. It may be due to the supplementation of Vitamin D, as the woman take multivitamin tablets. The results may also have effect with clothing habits, lifestyle modification and many other reasons. The physical activity and going outdoor for walk and exercise among youth has effect on the level of Vitamin D. The findings show that environment has effect on vitamin D. Also, the effect of weather is visible on the vitamin D results. In Summer the vitamin D is higher. The prevalence of Vitamin D is higher in Winter season [16]. Several possibilities have been suggested to explain the lower 25(OH)D levels seen in obesity, including decreased sun exposure due to sedentary lifestyle, poor diet, and increased clearance of 25(OH)D due to storage in adipose tissue [17].
Another study conducted by Adikaram and Samaranayake (2019) shows that Vitamin D level is affected by the insulin resistance and adiposity measures [18]. It says that 75% of the children have vitamin D deficiency and 21.4% have vitamin d insufficiency. The vitamin D level has several effects. Sometimes, it is due to the weather, and most the times it is due to exercise and physical activity. While some studies reported that Insulin level also has effect on vitamin D. The effect of vitamin D levels in Obese children on different metabolic syndrome risk factors before treatment with vitamin D supplement has been studied. The cardiovascular disease is directly related to the vitamin D deficiency in some studies. [18]
Conclusion
Our findings indicate that the prevalence of vitamin D deficiency is high among obese children. It also shows a significant association between Vitamin D level with several factors like th BMI, HBA1C, HDL cholesterol, Fasting blood Glucose, Triglycerides, and Blood Pressure, which shows slight reduction in the obesity of children after the treatment. The impact of Vitamin D in reducing the Triglycerides levels among children after treatment is remarkable. The HDL level among obese children after treatment increased. The HBA1C among children before treatment and after treatment also changed, as the pre-diabetics were greater in number before treatment and after the treatment, the number of children having pre-diabetics levels reduced to normal. The results of the study showed that Vitamin D is effective in the manner of reducing obesity rates and the risk of developing high blood pressure, hypertriglyceridemia and diabetes, which are risk factors for developing metabolic syndrome.
(Please refer attached pdf to view all tables and figures)
Reference
1. Wortsman J, Matsuoka LY, Chen TC, Lu Z, Holick MF. Decreased bioavailability of vitamin D in obesity. Am J Clin Nutr. 2000 ;72:690–3
2. Prevalence of Obesity and Severe Obesity in US Children, 1999-2016., Skinner AC, Ravanbakht SN, Skelton JA, Perrin EM, Armstrong SC, Pediatrics. 2018;141.
3. Global Consensus Recommendations on Prevention and Management of Nutritional Rickets. Munns CF, Shaw N, Kiely M, Specker BL, Thacher TD, Ozono K, Michigami T, Tiosano D, Mughal MZ, Mäkitie O, Ramos-Abad L, Ward L, DiMeglio LA, Atapattu N, Cassinelli H, Braegger C, Pettifor JM, Seth A, Idris HW, Bhatia V, Fu J, Goldberg G, Sävendahl L, Khadgawat R, Pludowski P, Maddock J, Hyppönen E, Oduwole A, Frew E, Aguiar M, Tulchinsky T, Butler G, Högler W, J Clin Endocrinol Metab. 2016 Feb;101(2) :394-415. Epub 2016 Jan 8.
4. Zimmet P, Alberti KG, Kaufman F, Tajima N, Silink M, Arslanian S, Wong G, Bennett P, Shaw J, Caprio S. IDF Consensus Group. The metabolic syndrome in children and adolescents - an IDF consensus report. Pediatr Diabetes. 2007;8:299–306. doi: 10.1111/j.1399-5448.2007.00271.x. [PubMed]
5. Shils ME, Shike M. Modern Nutrition in Health and Disease. 10th ed. Philadelphia: Lippincott Williams & Wilkins; 2006.
6. Turer CB, Lin H, Flores G. Prevalence of vitamin D deficiency among overweight and obese US children. Pediatrics. 2013;131(1):e152–161. [PubMed] [Google Scholar]
7. Cruz M.L., Goran M.I. The metabolic syndrome in children and adolescents. Curr. Diabetes Rep. 2004;4:53–62. doi: 10.1007/s11892-004-0012-x. [PubMed] [CrossRef] [Google Scholar]
8. Weiss R., Bremer A.A., Lustig R.H. What is metabolic syndrome, and why are children getting it? Ann. N. Y. Acad. Sci. 2013;1281:123–140. doi: 10.1111/nyas.12030. [PMC free article] [PubMed]
9. Taha D., Ahmed O., Sadiq B.B. The prevalence of metabolic syndrome and cardiovascular risk factors in a group of obese Saudi children and adolescents: A hospital-based study. Ann. Saudi Med. 2009;29:357–360. doi: 10.4103/0256-4947.55164. [PMC free article] [PubMed]
10. Turer C.B., Lin H., Flores G. Prevalence of vitamin D deficiency among overweight and obese US children. Pediatrics. 2013;131:e152. 10.1542/peds.2012-1711. [PubMed]
11. Erol M., Bostan Gayret Ö., Hamilç?kan ?., Can E., Yi?it Ö.L. Vitamin D deficiency and insulin resistance as risk factors for dyslipidemia in obese children. Arch. Argent. Pediatr. 2017;115:133–139. [PubMed]
12. Pacifico I., Anania C., Osbom J.F., Ferraro F., Bonci E., Olivero E., Chiesa C. Low 25(OH)D3 levels are associated with total adiposity, metabolic syndrome, and hypertension in Caucasian children and adolescents. Eur. J. Endocrinol. 2011;165:603– 611. doi: 10.1530/EJE-11-0545. [PubMed]]
13. Atabek M.E., Eklioglu B.S., Akyürek N., Alp H. Association between vitamin D level and cardiovascular risk in obese children and adolescents. J. Pediatr. Endocrinol. Metab. 2014;27:661–666. doi: 10.1515/jpem-2013-0379. [PubMed]
14. 1,25-Dihydroxyvitamin D3 evokes oscillations of intracellular calcium in a pancreatic beta- cell line. Sergeev IN, Rhoten WB Endocrinology. 1995 Jul; 136(7):2852-61. [PubMed]
15. Turer CB, Lin H, Flores G. Prevalence of vitamin D deficiency among overweight and obese US children. Pediatrics. 2013;131(1):152–61.
16. Salek, M., Hashemipour, M., Aminorroaya, A., Gheiratmand, A., Kelishadi, R., Ardestani, P. M., ... & Zolfaghari, B. (2008). Vitamin D deficiency among pregnant women and their newborns in Isfahan, Iran. Experimental and clinical endocrinology & diabetes, 116(06), 352-356.
17. Wortsman J, Matsuoka LY, Chen TC, Lu Z, Holick MF 2000 De- creased bioavailability of vitamin D in obesity. Am J Clin Nutr 72:690 – 693
18. Adikaram, S. G. S., Samaranayake, D. B. D. L., Atapattu, N., Kendaragama, K. M. D. L. D., Senevirathne, J. T. N., & Wickramasinghe, V. P. (2019). Prevalence of vitamin D deficiency and its association with metabolic derangements among children with obesity. BMC pediatrics, 19(1), 186.
19. Soudarssanane, M. B., Karthigeyan, M., Stephen, S., & Sahai, A. (2006). Key predictors of high blood pressure and hypertension among adolescents: a simple prescription for prevention. Indian Journal of Community Medicine, 31(3), 164.
20. Syliwia wieder-Huszla, Anna Jurczak (2019) Relationship between Vitamin D and Metabolic Syndrome, International Journal of Environmental Research and Public Health.
21. Sarmiento-Rubiano, L. A., Angarita Ruidiaz, J. A., Suarez Dávila, H. F., Suarez Rodríguez, A., Rebolledo-Cobos, R. C., & Becerra, J. E. (2018). Relationship between Serum Vitamin D Levels and HDL Cholesterol in Postmenopausal Women from Colombian Caribbean. Journal of nutrition and metabolism, 2018, 9638317.
22. Rodríguez-Rodríguez E, Ortega RM, González-Rodríguez LG, López-Sobaler AM; UCM Research Group VALORNUT (920030). Vitamin D deficiency is an independent predictor of elevated triglycerides in Spanish school children. Eur J Nutr. 2011;50(5):373-378. doi:10.1007/s00394-010-0145-4
23. Hestiantoro A, Karimah PD, Shadrina A, Wiweko B, Muharam R, Astuti BPK.F1000Res. 2019 Jan 23;8:94. doi: 10.12688/f1000research.16815.1. eCollection 2019.PMID: 30881692
24. Hauger H, Laursen RP, Ritz C, Mølgaard C, Lind MV, Damsgaard CT. Eur J Nutr. 2020 Apr;59(3):873-884. doi: 10.1007/s00394-019-02150-x. Epub 2020 Feb 14. PMID: 32060613
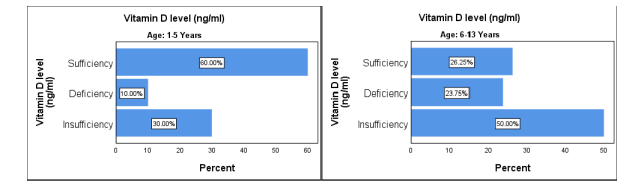
Figure 1
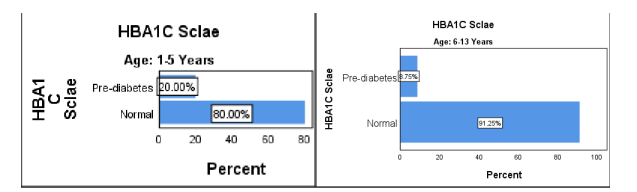
Figure 2
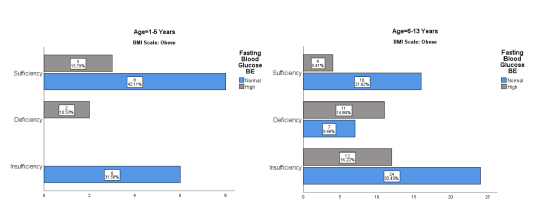
Figure 3
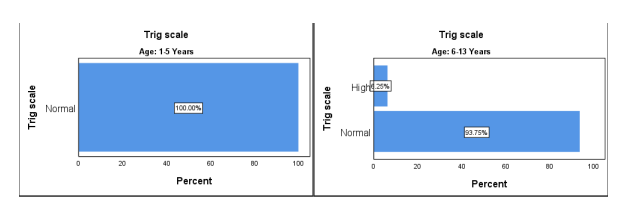
Figure 4
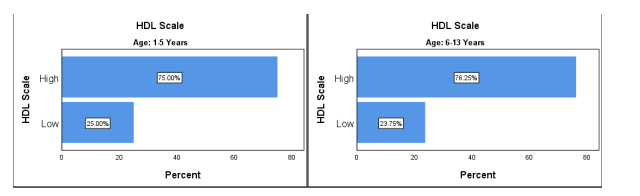
Figure 5
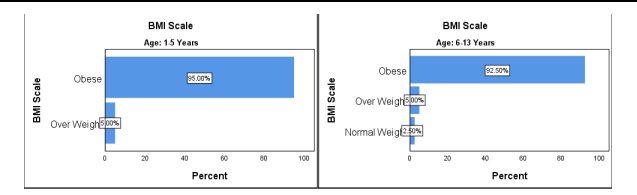
Figure 6
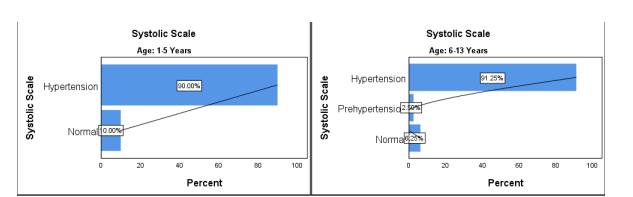
Figure 7
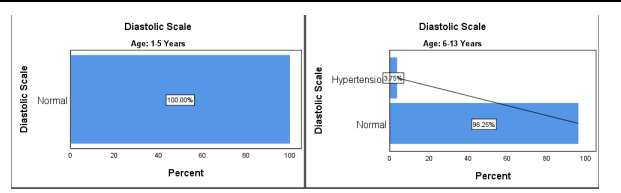
Figure 8
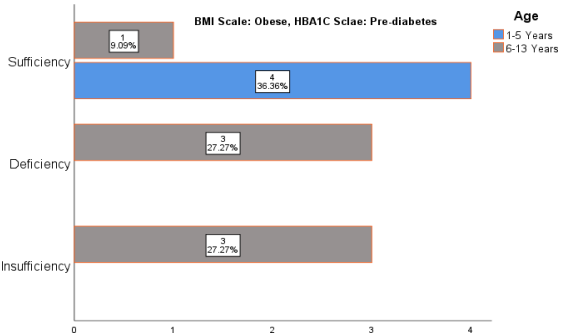
Figure 9
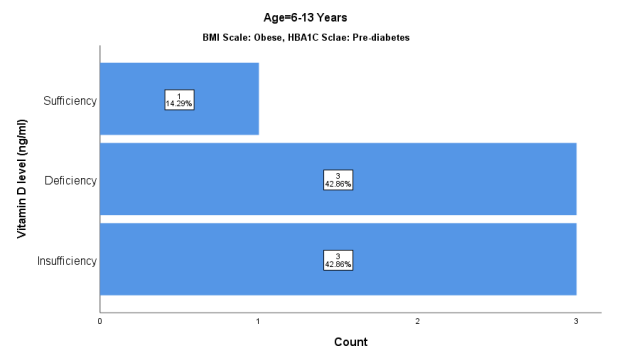
Figure 10
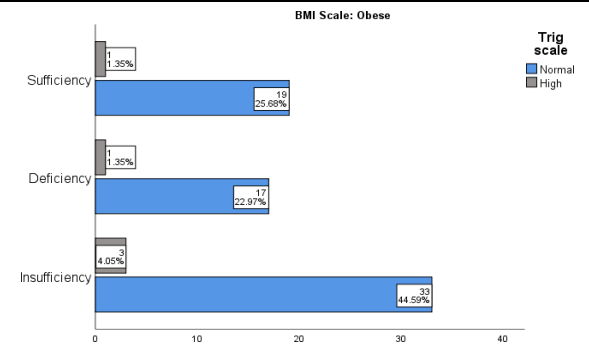
Figure 11
