Assessment of Plastibell Circumcision Outcomes at Glasgow Children's Hospital: A Retrospective Analysis
Assessment of Plastibell Circumcision Outcomes at Glasgow Children's Hospital: A Retrospective Analysis
Wisam Abbas 1, Angela Docherty 2
1,2. Paediatric Surgery Department, Royal Hospital for Children, 1345 Govan Rd, Glasgow G51 4TF Scotland, United kingdom.
*Correspondence to: Wisam Abbas, Paediatric Surgery Department, Royal Hospital for Children, 1345 Govan Rd, Glasgow G51 4TF Scotland, United kingdom.
Copyright
© 2024: Wisam Abbas. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 26 March 2024
Published: 01 May 2024
Abstract
Background: Platibell circumcision is new service at Glasgow Children's Hospital established in May 2023. This retrospective study conducted aiming to assess the outcomes in infants who underwent non therapeutic Plastibell circumcision for religious or cultural purposes.
Objective: The objectives include evaluating surgical success and to review the complications of Plastibell circumcision reported in our cohort to determine the safety of the procedure.
Method: Retrospective analysis was undertaken, reviewing the medical records of infants who underwent Plastibell circumcision over the period from May 2023 to February 2024.
Results: Total number of patients was 167. 139 underwent the procedure. median gestational age (GA) of 39 weeks. The mean age at the time of the procedure was 53 days. Additionally, the mean weight of 4.25 kg. Most common size used was 1.5 cm. Overall complications rate was 5.04%.
Conclusion: Plastibell circumcision performed in Glasgow Children Hospital is safe and our results are comparable to published literature. The study also constitutes a foundation for future studies.
Assessment of Plastibell Circumcision Outcomes at Glasgow Children's Hospital: A Retrospective Analysis
Introduction
Plastibell circumcision is widely utilized technique in paediatric surgical practices, demonstrating an advantage in terms of ease of use and reduced postoperative complications. The service is established in May 2023 at Glasgow Children's Hospital due to growing need for nontherapeutic circumcision. Furthermore, we recognize the benefits of avoiding general anaesthetic and reduce pressure on routine inpatient waiting list.
This study aiming to assess the outcomes of Plastibell circumcision preformed for religious and cultural indications.
Plastibell circumcision involves the application of a plastic ring to facilitate the removal of the foreskin. as with any medical intervention, the comprehensive evaluation of its outcomes is imperative to ensure the safety, efficacy, and overall well-being of the paediatric patients undergoing the procedure.
Understanding the potential outcomes of Plastibell circumcision in our institute is crucial in providing evidence-based information for informed decision-making. By conducting a retrospective analysis of cases, we seek to provide an understanding of the procedure's success rates and identify potential complications.
Method
Retrospective study. Electronic medical records of infants who underwent Plastibell circumcision over the period from May 2023 to February 2024 were reviewed. Data analysed include:
Gestational age
Age and weight at the time of procedure
Size of plastibell used
Procedure outcome.
Complications reported until the ring falls off. Any patient required hospital review following procedure is recorded as complication.
All the circumcisions performed by consultant paediatric surgeon or advanced nurse practitioner under consultant supervision.
Results
Demographic characteristics reveal a median gestational age (GA) of 39 weeks. The mean age at the time of the procedure was 53 days (circumcision performed up to 12 weeks’ age). Additionally, the mean weight of 4.25 kg.
Total number of patients referred was 167 with 139 undergoing the Plastibell circumcision procedure, while 28 did not proceed with the intervention (Table-1).
|
Indication for Cancellation |
n=28 |
|
URTI Including Covid |
13 |
|
Hypospadias |
1 |
|
Penoscrotal Web |
2 |
|
Congenital Adrenal hyperplasia |
1 |
|
Buried penis |
8 |
|
Noisy breathing Awaiting ENT review |
1 |
|
Cardiac Murmur |
1 |
|
Parental Refusal |
1 |
Most common plastibell size used was 1.5cm (Graph-1)
Graph-1 Plastibell sizes.
Patients followed up until the plastibell ring fall off. Complications recorded and their outcome described in table-2
|
Complications |
5.04% n=7 |
Outcome |
|
Granulation |
1.44% n=2 |
Clinic review. Spontaneous resolution |
|
Small glans Hematoma |
0.72% n=1 |
Spontaneous resolution |
|
Ring retained for more than 2 weeks |
0.72% n=1 |
Review, fell out later |
|
Incomplete foreskin removal |
0.72% n=1 |
Plan for review in 1 year |
|
Ring retraction |
1.44% n=2 |
Removed in A/E |
Discussion
In our study, all the plastibell circumcisions performed for religious or cultural indications.
The reasons for the 28 babies not undergoing the Plastibell circumcision procedure provide insights into the nature of paediatric healthcare decision-making ensuring all children undergoing the procedure are in maximum optimised health condition (table-1). Furthermore, parental refusal constituted one case, highlighting the importance of involving all caregivers in the decision-making process.
Appropriate plastibell size is selected by visual assessment of the glans width. This is important as inappropriate size rings may result in retained plastibell or proximal ring migration. The commonest plastibell size used in our study was 1.5 cm (39% n=54) (Graph-1). A study from Pakistan by Samad A et al. reported commonest size used was 1.4 (n=772 63.1%)(1). The size commonly used in Multi-centre study from Nigeria by Jimoh BM et al. was 1.3 (n=1,040, 45.7%) (2). Al-Marhoon MS, Jaboub SM from Oman reported 1.3 as most common size (3).
Complications recorded in 7 (5.04%) (table-2). Two patients had granulation tissue at the skin margins and one patient had small glans hematoma from edge of the plastibell. Both groups required no further intervention and had spontaneous resolution. Ring retained for more than 2 weeks in one patient who required hospital review. The ring fell out spontaneously two days following review with no intervention required. One patient had inadequate circumcision due to incomplete foreskin removal. Further follow up plans arranged for redo circumcision. Two patient had Ring migration proximally to penile shaft. Both patient seen in emergency department and underwent plastibell removal under local anaesthetic. Circumcision already was completed. No post circumcision bleeding complication in out cohort. The Overall rate of complications for infant circumcision reported by Mousavi SA, Salehifar E from Iran was 7.08% (4). Jimoh BM et al. reported overall complication rate of 1.1% (2). The overall complication rate was 7.4% from a study from Pakistan by Samad A et al. (1).
Conclusion
The findings from this analysis provide insights into the efficacy and safety of Plastibell circumcision. This retrospective analysis reflects thoughtful assessment of the procedural outcomes ensuring that our clinical practice is safe and our results are comparable to published literature. The study also constitutes a baseline for future studies and provide information that can be discussed with families during consent process for informed decision making.
References
1. Samad A, Khanzada TW, Kumar B. Plastibell circumcision: A minor surgical procedure of major importance. J Pediatr Urol [Internet]. 2010;6(1):28–31. Available from: http://dx.doi.org/10.1016/j.jpurol.2009.05.006
2. Jimoh BM, Odunayo IS, Chinwe I, Akinfolarin OO, Oluwafemi A, Olusanmi EJ. Plastibell circumcision of 2,276 male infants: A multi-centre study. Pan Afr Med J. 2016;23:1–8.
3. Al-Marhoon MS, Jaboub SM. Plastibell circumcision: How safe is it?: Experience at Sultan Qaboos university hospital. Sultan Qaboos Univ Med J. 2006;6(1):17–20.
4. Mousavi SA, Salehifar E. Circumcision Complications Associated with the Plastibell Device and Conventional Dissection Surgery: A Trial of 586 Infants of Ages up to 12 Months. Adv Urol. 2008;2008(January):1–5.
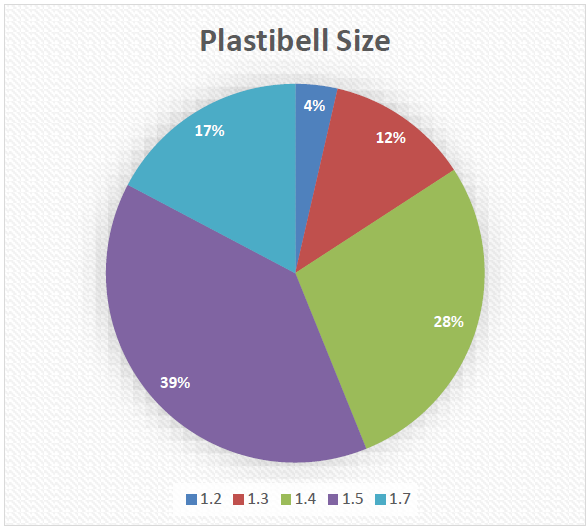
Figure 1
