Diagnosis and Management of Pediatric Multisystem Inflammatory Syndrome Related to COVID-19 in a Resource-Limited Country
Diagnosis and Management of Pediatric Multisystem Inflammatory Syndrome Related to COVID-19 in a Resource-Limited Country
Marie Claire Milady Auguste1*, MD, Paul Bruno Jean Baptiste2, MD, Joelle Cynthia Denis2, MD, Rénault Louis1, MD, Jean Ophane Alouidor1, MD
1: University Hospital of Mirebalais.
2: Bernard Mevs Hospital.
*Correspondence to: Marie Claire Milady Auguste,, University Hospital of Mirebalais.
Copyright
© 2024: Marie Claire Milady Auguste. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 24 April 2024
Published: 16 May 2024
Abstract
The WHO first described Pediatric Multisystem Inflammatory Syndrome related to COVID-19 (MIS-C) in 2020 during the COVID-19 pandemic. This severe and emerging condition is likely underdiagnosed in Haiti. Here, we report the clinical case of a 12-year-old adolescent meeting the WHO diagnostic criteria for MIS-C. She was primarily treated with corticosteroids, and her outcome was favorable. This demonstrates that adequate management of this condition is possible in a resource-limited country without access to IVIG and anti-interleukins.
Keywords: MIS-C, COVID-19, children, Kawasaki-like syndrome, shock, and Kawasaki-like syndrome
Diagnosis and Management of Pediatric Multisystem Inflammatory Syndrome Related to COVID-19 in a Resource-Limited Country
Introduction:
A novel respiratory infection emerged in December 2019 in Wuhan, officially named COVID-19 by the WHO on February 11, 2020[i]. The WHO Director-General declared the pandemic on March 11, 2020 1. Initially, the disease was more severe in adults. However, in April 2020, severe pediatric cases were reported in England, France, and the Dominican Republic[ii]. Pediatric patients exposed to COVID-19 presented with a syndrome combining clinical features of septic shock and Kawasaki-like syndrome 2. This condition was termed Multisystem Inflammatory Syndrome in Children related to COVID-19 (MIS-C), and diagnostic criteria were defined by the WHO to differentiate it from Kawasaki disease2 [iii]. As of now, Haiti has yet to report any epidemiological data on MIS-C to the PAHO-WHO3.
Case Presentation:
We present the case of a 12-year-old female adolescent transferred from the capital of Haiti to the pediatric emergency department at the University Hospital of Mirebalais. She presented with a fever, generalized malaise, edema of the upper and lower limbs, skin lesions, and severe abdominal pain. Her symptoms began approximately ten days before her arrival, starting with a sore throat, fever, erythematous lesions on the upper and lower limbs, palms of the hands (image 1), and soles of the feet. She had undergone surgical intervention for an atrial septal defect at the age of 3 and had no previous symptoms resembling COVID-19. However, a positive contact history was found (her uncle had COVID-19 symptoms) two weeks before her illness onset. On arrival, she exhibited general malaise with vital signs: temperature 38.4°C, blood pressure 80/40 mmHg, oxygen saturation 95% on 3 liters of oxygen, and a Glasgow Coma Scale score of 15/15. Examination of the ear, nose, throat, lymph nodes, and the cardiopulmonary system was within normal limits. Abdominal examination revealed a hepatomegaly with a liver palpable just 1 cm below the costal margin. There were also mild edemas on the dorsal aspect of the feet, and her skin's capillary refill time was less than 3 seconds. Erythematous macular lesions were found on her thighs (Image 2). The rest of the clinical examination was unremarkable.
Image 1: erythematous lesions on the palms of the hands
Image 2: Erythematous macular lesions on the thighs
Intervention:
Initial complete blood count showed moderate normochromic and macrocytic anemia (hemoglobin: 8.9 mg/dL, MCV: 91.6 fL, MCHC: 32.6 g/dL), leukocytosis (white blood cells: 18,800/mm3), lymphopenia (lymphocyte count: 11.5% with an absolute lymphocyte count [ALC] of 2,162 cells/mm3), elevated inflammatory markers (CRP: 96 mg/L, ESR: 80 mm/h), elevated creatinine (0.93 mg/dL), abnormal coagulation parameters (D-dimer: 1,947 ng/mL, INR: 4.07, PT: 38.3 s), and abnormal liver function tests (total bilirubin: 0.42 mg/dL, AST/GOT: 50 U/L, ALT/GPT: 107 U/L). The post-COVID-19 Multisystem Inflammatory Syndrome diagnosis was made, even though COVID-19 PCR and serology results for IgM were negative, as IgG was positive. Other tests, including troponin I, COVID-19 antigen, and rapid malaria test, were also negative. Urine and blood cultures were sterile. She underwent two echocardiograms: the first one before her transfer showed mild to moderate mitral regurgitation, right coronary artery dilation at 6 mm, left coronary artery dilation at 5 mm, and a z-score of 5 (Images 3 and 4). The second echocardiogram, performed one week later, indicated probable post-infectious myopericarditis. Chest radiography revealed infiltrates.
Image 3: mitral regurgitation
Image 4: right coronary artery dilation at 6 mm, left coronary artery dilation at 5 mm, and a z-score of 5
Results:
Upon her arrival at the emergency department, the patient was treated with vancomycin (20 mg/kg IV every 6 hours), ceftriaxone (75 mg/kg/24 hours IV every 12 hours), omeprazole (20 mg IV every 24 hours), aspirin (60 mg/kg/day orally every day), enoxaparin (0.5 mg/kg/dose subcutaneous every 12 hours), and dobutamine (7.5 mcg/kg/min). After two days, the shock resolved, and dobutamine was gradually tapered and discontinued. Twelve days later, she developed sinus bradycardia, but troponin remained negative. Due to the unavailability of intravenous immunoglobulin (IVIG), she was solely treated with methylprednisolone at 1 mg/kg/dose IV every 6 hours, and bradycardia improved approximately nine days later. Hematological follow-up showed persistent leukocytosis and lymphopenia (white blood cells: 13,400/mm3 at ten days and 22,800/mm3 at 20 days of hospitalization) and lymphopenia (lymphocytes 3.4% [ALC: 455.6 cells/mm3] and 14.6% [ALC: 3,328.8 cells/mm3] at 10 and 20 days of hospitalization, respectively), until her discharge at one month of hospitalization (white blood cells: 18,600/mm3, lymphocytes: 10.5% [ALC: 1,953 cells/mm3]). CRP also gradually improved to less than six at discharge. The patient was discharged on oral corticosteroids with follow-up appointments with an endocrinologist and a cardiologist. Her last echocardiogram showed moderate concentric left ventricular hypertrophy, for which she did not receive treatment.
Follow-up with the endocrinologist revealed no abnormalities after the gradual withdrawal of corticosteroids. Follow-up with the cardiologist showed moderate concentric left ventricular hypertrophy for which no treatment was administered. To date, the patient remains in excellent health.
Discussion:
In terms of diagnosis, WHO criteria1 for MIS-C include children and adolescents aged 0 to 19 years with a fever lasting more than three days and two of the following elements: rash or non-purulent bilateral conjunctivitis or mucocutaneous inflammatory signs (oral, hands, or feet). Hypotension or shock is indicative of myocardial dysfunction, pericarditis, valvulitis, or coronary abnormalities (including ECHO findings or elevated troponin/NT-proBNP). Evidence of coagulopathy (elevated PT, PTT, or D-dimers). Acute gastrointestinal problems (diarrhea, vomiting, or abdominal pain). Elevated inflammatory markers such as ESR, C-reactive protein, or procalcitonin. No other evident microbial cause of inflammation, including bacterial sepsis and staphylococcal or streptococcal shock syndromes. Finally, evidence of COVID-19 (RT-PCR, antigen test, or positive serology) or probable contact with COVID-19 patients.
From an epidemiological perspective, 58% of MIS-C patients in the USA were of African American or Latino origin, as reported in several case reports from France, England, Africa, and Switzerland [[iv]‘[v]’ 13 ]. Clinically, persistent fever and erythematous maculopapular lesions on the upper and lower limbs, palms of the hands, and soles of the feet have been reported in many cases[5,[vi],8]. Abdominal pain associated with tenderness in the right upper quadrant was also described in three patients in a case report from an Italian hospital[vii]. However, it is noteworthy that most MIS-C patients had gastrointestinal symptoms, particularly diffuse abdominal pain[viii]. Hypotensive shock (blood pressure 80/40) associated with erythematous non-pruritic rash, initially appearing on the trunk and spreading to the rest of the body, was also reported in a case report published in Cureus. Other reports also mentioned the combination of hypotension and erythematous skin lesions [8’[ix]’[x]’[xi]’[xii]’[xiii]’[xiv]’[xv]].
On a laboratory level, negative results for COVID-19 biological tests, including rapid antigen tests and PCR, have been reported in the literature [8’9’12,13,15]. This was associated with lymphopenia, elevated inflammatory markers, sterile blood and urine cultures, unremarkable immune panels, and positive IgG serology for COVID-19[6’8’9’13’14]. Coronary dilation on echocardiography was found in two out of six patients in a case presentation from a Swiss hospital13, one patient in a case report from Brazil15, five patients in a retrospective observational study published in France2, and mitral regurgitation in many other patients described in the literature. Other echocardiographic reports showed myopericarditis15.
Regarding therapy, an article published in the New England Journal on MIS-C management concluded no evidence that recovery from MIS-C differed after primary treatment with IVIG alone, IVIG combined with glucocorticoids, or glucocorticoids alone16.
Conclusion:
Our patient's clinical and laboratory findings were consistent with most previously published case reports on MIS-C patients. Due to the unavailability of IVIG and anti-interleukins in Haiti, high-dose corticosteroids (methylprednisolone) were used. This demonstrates that this novel syndrome can be managed in a resource-limited country without access to IVIG and anti-interleukins, primarily using corticosteroids, with the expectation of a favorable outcome. This clinical case of MIS-C is the first confirmed case at the University Hospital of Mirebalais.
Acknowledgments:
We want to thank the healthcare team at the pediatric departments of Bernard Mevs Hospital and the University Hospital of Mirebalais. We also thank the patient's family and the University Hospital of Mirebalais, research coordination team.
References
i.Shelley R. ‘et al’.2020’Hyperinflammatory shock in children during COVID-19 pandemic’, Lancet 395(10237):1607-1608.
[ii] Toubiana J. ‘ et al’. 2020,’ Kawasaki-like multisystem inflammatory syndrome in children during the covid-19 pandemic in Paris, France: prospective observational study’, The BMJ 369
[iii] Ruvinsky S.’ et al’. 2022 ‘ Multisystem Inflammatory Syndrome Temporally Related to COVID-19 in Children From Latin America and the Caribbean Region: A Systematic Review With a Meta-Analysis of Data From Regional Surveillance Systems’, Front Pediatr10:881765
[iv] CDC. 2023. Health Department-Reported Cases of Multisystem Inflammatory Syndrome in Children (MIS-C) in the United States. Available at : https://covid.cdc.gov/covid-data-tracker/#mis-national-surveillance ( Accessed: 30/01/2023)
[v] Moodley P.’ et al.’ 2021 ‘ A case of multisystem inflammatory syndrome in an African adolescent male: a case report’ Pan Afr Med J 38:174
[vi] Kathane, U.P. and Vagha, K. 2022, ‘ A Case Report on Multisystem Inflammatory Syndrome After COVID-19 Infection in a 12-Year-Old child’, Cureus 14(9):e29061
[vii] Meneghel, A. ‘et al.’ 2022’ Case report: Exploring under the tip of the iceberg: A case series of “self-limiting” multisystem inflammatory syndrome in children’, Front Pediatr 10:1012582
[viii] Jurkiewicz, B. ‘ et al’. 2021, ‘Pediatric Multisystem Inflammatory Syndrome in Children as a Challenging Problem for Pediatric Surgeons in the COVID 19 Pandemic—A Case Report’, Front Pediatr 9:677822
[ix] Verdoni, L. ‘ et al’. 2020’An outbreak of severe Kawasaki-like disease at the Italian epicentre of the SARS-CoV-2 epidemic: an observational cohort study’, Lancet 395(10239):1771-1778.
[x] Fouriki, A. ‘ et al .’ 2021, ‘Case Report: Case Series of Children With Multisystem Inflammatory Syndrome Following SARS-CoV-2 Infection in Switzerland’, Front Pediatr 8:594127
[xi] Nguyen, D. C. ‘ et al.’ 2020’ Pediatric Case of Severe COVID-19 With Shock and Multisystem Inflammation’, Cureus 12(6):e8915
[xii] Greene, A. G . ‘ et al ‘. 2020 ‘Toxic shock-like syndrome and COVID-19: Multisystem inflammatory syndrome in children (MIS-C)’, Am J Emerg Med 38(11):2492.e5-2492.e6.
[xiii] Riphagen, S. ‘ et al ‘.2020, ‘ Hyperinflammatory shock in children during COVID-19 pandemic’, Lancet 395(10237):1607-1608.
[xiv] Carraro, M. ‘ et al’ . 2020,’ Case Report: Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with SARS-CoV-2 with Coronary Involvement’, Fortune journals
[xv] Beaudry, J.T. ‘ et al ‘ . 2021’ Fatal SARS-CoV-2 Inflammatory Syndrome and Myocarditis in an Adolescent: A Case Report’ , Pediatr Infect Dis 40(2):e72-e7
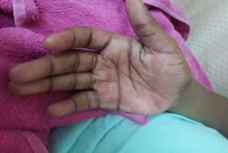
Figure 1
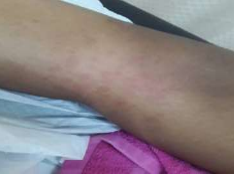
Figure 2
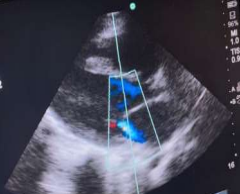
Figure 3
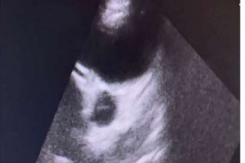
Figure 4
