Management of Cutaneous T-lymphoma (Fungoid Mycosis): A Case Report
Management of Cutaneous T-lymphoma (Fungoid Mycosis): A Case Report
H. Benabdesselam1*, S.Mhirech1, M.Ait erraisse1, FZ. Farhane1, Z. Alami1, T.Bouhafa1
1. Radiation and brachytherapy department, oncology hospital, HASSAN II University Hospital in Fez.
*Correspondence to: H. Benabdesselam, Radiation and brachytherapy department, oncology hospital, HASSAN II University Hospital in Fez
Copyright.
© 2024 H. Benabdesselam. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 21 October 2024
Published: 01 November 2024
DOI: https://doi.org/10.5281/zenodo.14160005
Abstract
Fungal mycosis is a rare form of T cell skin lymphoma. It usually manifests as red plaques, spots or nodules, its diagnosis is anatomopathological, treatment is based on topical treatments, radiation and/or systemic therapies according to disease staging.
We report a case of fungal mycosis (MF) in a 32-year-old patient and discuss the specifics of management in this case. Our patient had nodular lesions in the face and back, a biopsy with anatomopathological study and immunohistochemically were in favor of an MF, for which the patient received monochemotherapy based on Gemcitabine and methotrexate and given the local progression of her disease and the installation of a drug-induced hepatitis following Gemcitabine, the decision to radiotherapy the lesions was retained, with a dose of 30Gy in 10 fractions on the different lesions.
Management of Cutaneous T-lymphoma (Fungoid Mycosis): A Case Report
Introduction
MF has an incidence of 6 to 9 cases/million inhabitants/year in the United States. It affects subjects of median age 55-60 years (but all ages may be affected, including children), with a male/female ratio of 2/1 [1]. In the initial stages, it is present as itchy patches. The diagnosis of MF is based on clinical and histopathological criteria.
Close multidisciplinary collaboration between the teams of dermatology, anatomopathological and radiotherapy is essential for optimal management; radiotherapy (RT) is an important treatment: given the radio sensitivity of lymphomas, it can be considered a reference treatment for single or localized lesions of indolent primary skin lymphoma (PCL). (2) Fungal mycosis often progresses slowly, and the prognosis depends on the response to treatment and whether systemic symptoms are present.
Observation
One patient, 32 years old, without specific pathological HTA, who is referred for widespread squamous and pruritic lesions the physical examination revealed widespread squamous erythematous plaques with large nodules on the face and back (Fig.1)
The patient was given a skin biopsy of the different lesions with an anatomopathological and immunohistochemically study in favor of a folicullotropic type fungal mycosis with cervical thoracic abdomino pelvic scan performed as part of the extension assessment: presence of the adeno-pathological, bilateral cervical axillary classifying the tumor: a stage IIB according to the classification EORTC; then she received systemic treatment with methotrexate and corticosteroid infiltrations for facial lesions, and given the increase in size of the face and back, a Gemcitabine-based mono-chemotherapy was administered, However, as the patient had an allergic reaction similar to a drug-like hepatitis following the introduction of two courses of Gemcitabine, the decision to have external radiotherapy was made. The latter was made by three-dimensional conformational technique: at a dose of 30 Gy in 10 fractions on the lesions of the face and on the lesions of the back with good tolerance and almost complete regression of the lesions described above. (Fig2)
Fig. 1 : clinical image before treatment of our patient
Fig. 2 : post-therapeutic clinical image of our case
Fig. 3: Dosimetry image of our patient showing the coverage of different volumes.
Discussion
Fungal mycosis is also called primitive T cell skin lymphoma or Alibert’s disease because of its description by the French dermatologist Jean-Louis Alibert in 1832, is a hemopathy characterized by infiltrates in the skin of small and medium-sized T cells with cerebriform nuclei, called Sézary cells, It is the most common primary T cell skin lymphoma and accounts for more than half of all primary skin lymphomas (3).
The most affected patients are aged 55-60 years, although the disease has been more rarely seen in children and adolescents. The sex ratio for Male: Female is 2:1 (4). Clinical symptomatology can evolve in four phases: going to skin spots limited in the surface at the appearance of cells at the blood level (syndrome de sézary). The diagnosis is made by a biopsy with immunohistochemically study to differentiate from other skin lesions especially for the beginner forms. The CT or MRI is done as part of the extension check-up, which allows to stadify the disease: visceral involvement and adenopathy research. (5)
According to the recommendations of the European Organization for Research and Treatment of Cancer (EORTC), for stages IIB, it is recommended to start with systemic treatments such as local corticosteroids, low-dose methotrexate, and interferon alpha and if escaping from these, has an interest to start a monochemotherapy type: Gemcitabine, doxorubicin ... localized radiation therapy. (6) The latter remains an important treatment: given the radio sensitivity of lymphomas, it can be considered as a reference curative treatment for single or localized lesions of indolent PCL. The use of low doses of radiation for palliative purposes (pain, bleeding, tumor progression...) has also been reported for disseminated forms (7).
Low energy X-photon radiation therapy with interest in using hypo-fractionated patterns has been reported by the French society of Radiotherapy and Oncology (SFRO) (8). In addition, as a therapeutic novelty: total skin electrontherapy, which is an interesting technique in the treatment of MF, but it, remains little used because it is not accessible and very time consuming (8) (9).
Conclusion
Fungal mycosis is a rare form of skin lymphoma that manifests itself primarily through skin lesions, often confused with other dermatological conditions. It is a slow-developing disease requiring a therapeutic approach adapted to its evolution. Radiation therapy is particularly beneficial, especially for localized lesions, by combining it with other topical or systemic therapies, we can optimize the management of this type of tumor, and the prognosis varies, depending on the stage of the disease.
References:
1. Foss, FM and Girardi, M. (2017). Mycosis fongoide et syndrome de Sézary. North American Hematology/Oncology Clinics, 31(2), 297. doi:10.1016/j.hoc.2016.11.008 (sciencedirect)
2. D. Canu, M. Beylot-Barry, S. Ingen-Housz-Oro, N. Ouhabrache, NH To Place radiation therapy in the treatment of skin lymphomas Annales de Dermatologie et de Vénéréologie – FMC DOI.org/10.1016/j.fander.2021.08.006 (sciencedirect)
3. Willemze R, Cerroni L, Kempf W et al. The 2018 update of the WHO-EORTC classification for primary cutaneous lymphomas [archive], Blood, 2019; 133:1703-1714
4. M. Beylot-Barry, O. Dereure, B. Vergier and S. Barete, “Management of Cutaneous T-Lymphomas: Recommendations of the French Group for the Study of Cutaneous Lymphomas”, Annales de Dermatologie et de Vénéréologie, vol. 137, no 10, October 2010, p. 611–621 (DOI 10.1016/yy.year.2010.06.021, read online [archive], accessed on June 18, 2020)
5. Cutaneous T lymphomas: management recommendations Based on the communication of Dr Marie Beylot-Barry (Dermatology Department, Haut-Lévèque hospital, Bordeaux University Hospital)
6. Johanna Latzka a,b,* , Chalid Assaf c,d,e , Martine Bagotf , Antonio Cozzio g , Reinhard Dummer h EORTC consensus recommendations for the treatment of mycosis fungoides/S ezary syndrome – Update 2023
7. D. Canu a, M. Beylot-Barry a b c, S. Ingen-Housz N. Ouhabrache e, N.H. To Place radiotherapy in the treatment of skin lymphomas (direct science)
8. A. Taverniers, B. Guillot, C. Kerr, O. Dereure Total body electrontherapy and fungal mycosis: a future treatment? (direct science)
9. C. Hennequina*, E. Riob, L. Quéroa, P. Clavère: Radiotherapy of skin cancers (French Society for Oncological Radiotherapy)
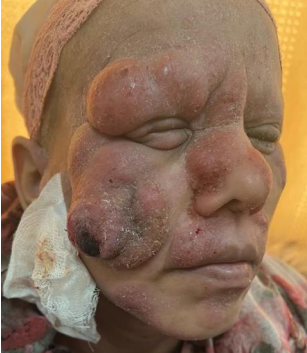
Figure 1
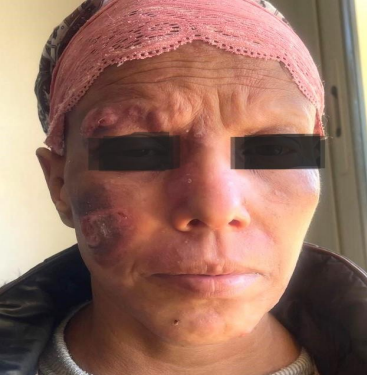
Figure 2
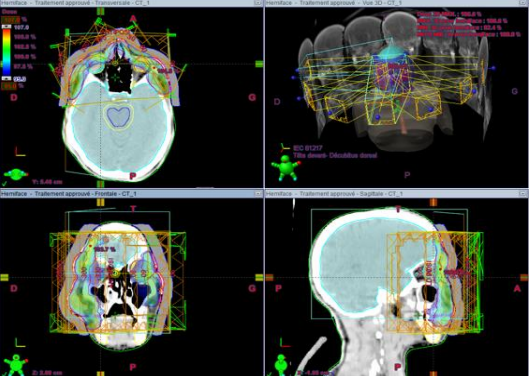
Figure 3
