Systematic Review of Mucormycosis Cases in COVID-19 Patients in a Tertiary Care Hospital
Systematic Review of Mucormycosis Cases in COVID-19 Patients in a Tertiary Care Hospital
Walinjkar Rajas1, Fernandes Tracy Maria2, Shinde Rashmi 3, Gala Harshita Kanti 4, Chaurasia Ekta5
1. M.B.B.S.M.D.(GENERAL MEDICINE), Consultant, Seven hills hospital, Mumbai.
2, 4. M.B.B.S, RegisteredMedicalOfficer, Seven hills hospital, Mumbai.
3. M.B.B.S, DA. DNB (ANESTHESIA), Consultant, Seven hills hospital, Mumbai.
5. B.H.M.S., Physician Assistant, Seven hills hospital, Mumbai.
Correspondence to: Dr. Rajas Walinjkar, Consultant, SevenHills Hospital, Marol-Maroshi Road, Andheri East, Mumbai, Maharashtra, India -400059.
Copyright
© 2024: Dr. Rajas Walinjkar. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 20 Nov 2024
Published: 01 Dec 2024
Abstract
Background-COVID-19 caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been associated with a wide range of opportunistic bacterial and fungal infections. Both Aspergillus and Candida have been reported as the main fungal pathogens for co-infection in people with COVID-19. Several cases of mucormycosis in people with COVID-19 have been increasingly reported world-wide, in particular from India during the second wave of COVID-19.
Objective-To conduct a systematic review of Mucormycosis cases in COVID-19 patients.
Materials and methods-This retrospective study was carried out at Seven Hills Hospital located at Mumbai, in which all cases that reported confirmed mucormycosis in COVID-19 positive cases were included. Clinical observations along with laboratory and radiological investigations were observed and analyzed.
Result-Out of the total study population of 16 in patients for COVID-19 disease, all were reported for mucormycosis after culture and radiological investigations. 56% was seen in elderly age group of more than 60 years. Pre-existing Diabetes Mellitus was seen in 81% of the cases. Rhizopus oyzae was found in 75% of people infected with mucormycosis. Most common organ involved with mucormycosis was nose and sinus (100%). Overall mortality was noted in 75% of the cases.
Discussion - Pre- existing diabetes, rampant use of corticosteroid for COVID-19appears to increase incidence of mucormycosis. All efforts should be made to maintain optimal blood glucose and only judicious use of corticosteroids in patients with COVID-19. Moreover Early detection strategies to be implemented which would allow prompt treatment leading to better outcomes.
Keywords- Mucormycosis, COVID-19, SARS COV2.
Systematic Review of Mucormycosis Cases in COVID-19 Patients in a Tertiary Care Hospital
Introduction
Coronavirus disease 2019 (COVID-19) caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has been associated with a wide range of opportunistic bacterial and fungal infections[1]. Both Aspergillus and Candida have been reported as the main fungal pathogens for co-infection in people with COVID-19[2]. Several cases of mucormycosis in people with COVID-19 have been increasingly reported world-wide, in particular from India during the second wave of COVID-19. The primary reason that appears to be facilitating Mucorales spores to germinate in people with COVID-19 is an ideal environment of low oxygen (hypoxia), high glucose (diabetes, new-onset hyperglycemia, steroid-induced hyperglycemia), acidic medium (metabolic acidosis, diabetic ketoacidosis [DKA]), high iron levels (increased ferritins) and decreased phagocytic activity of white blood cells (WBC) due to immunosuppression (SARS-CoV-2 mediated, steroid-mediated or background comorbidities) coupled with several other shared risk factors including prolonged hospitalization with or without mechanical ventilators.[3]
Mucormycosis is an angio- invasive disease caused by mold fungi of the genus Rhizopus, Mucor, Rhizomucor, Cunninghamella and Absidia of Order- Mucorales, Class- Zygomycetes. The Rhizopus oryzae is most common type and responsible for nearly 60% of mucormycosis cases in humans and also accounts for 90% of the Rhino-orbital-cerebral (ROCM) form. Mode of contamination occurs through the inhalation of fungal spores.This then infect the lungs, sinuses, and extend into the brain and eyes. Less often, infection may develop when the spores enter the body through a cut or an open wound.[4] Mucormycosis is not a contagious disease, as it cannot be spread from one person to another. It mainly affects people who are immunocompromised, or patients already infected with other diseases. High risk groups include people with diabetes (especially diabetic ketoacidosis), solid organ transplantation, neutropenia (low neutrophils), long-term systemic corticosteroid use, and iron overload (hemochromatosis). The risk is also high for people living with HIV, and those using immunomodulating drugs. Clinical presentation is classified according to the organ involvement. It can be rhino-orbital cerebral, pulmonary, cutaneous, gastrointestinal, or disseminated.
Fungal infections, including mucormycosis, aspergillosis and invasive candidiasis, have been reported in patients with severe COVID-19 or those recovering from the disease and have been associated with severe illness and death. India has reported a recent surge in mucormycosis cases. Following the surge of COVID-19 associated mucormycosis and the Government of India directive, several states in India made mucormycosis a notifiable disease in May 2021. This provided better insights into the disease burden, population characteristic, risk factors, clinical spectrum and outcomes of these patients .Current trends indicated that the surge is higher in those with pre-existing diabetes, those on systemic corticosteroids, and is being observed in both people with COVID-19, and those recovering from the disease.[4]
Though there is detailed data available regarding mucormycosis in covid-19 patients, real world data regarding characteristics, risk factors, clinical manifestations and outcome of these patients in India is relatively sparse. Hence, this study was carried out to review the incidence, clinical manifestations, risk factors, and outcome of patients affected with mucormycosis and Covid-19.
Materials and Methods
This study was carried out at Seven Hills Hospital, located at Mumbai. This is a retrospective study in which all cases that reported confirmed mucormycosis in COVID-19 positive cases were included. Routine laboratory investigations with radiological investigations like HRCT scan were performed along with KOH mount test with nasal swab culture to confirm species for mucormycosis. The treatment was administered to the patients for COVID infection as well as mucormycosis. Recovered patients were discharged from the hospital. Characteristics of each patient was collected on excel sheet and analyzed on various endpoints and outcomes.
Observations &Results
A total of 16 cases were included in this study, all reported for mucormycosis in confirmed Covid-19 patients by positive RTPCR (Reverse-Transcription polymerase chain reaction) report. Table 1 summarizes the 16 cases. Higher incidence of 56% was seen in age group more than 60 years. Pre-existing DM accounted for 81% of cases with mucormycosis and COVID-19. History of corticosteroid intake for the treatment of COVID-19 was present in 100% of cases, followed by Remdesivir (100%) and Tocilizumab (6.25%). Rhizopus oyzae was found in 75% of people infected with mucormycosis. Most common organ involved with mucormycosis was nose and sinus (100%), followed by rhino-orbital (87.5%). Overall mortality was noted in 75% of the cases. Table 2 summarizes the characteristics from 16 cases of mucormycosis with COVID-19.
Table 1- Summary of 16 cases that were reported with Mucormycosis
Table 2: Characteristics of 16 cases of Mucormycosis with COVID-19
|
Total confirmed Mucormycosis cases(N)=16 |
n (%) |
Remarks |
|
|
Age(in years) |
0 to 18-0 19 to 45- 04 46 to 60- 03 >60 -09 |
0 25 18.75 56.25 |
Higher incidence in age more than 60 years |
|
Gender |
Male- 11 Female- 05 |
68.75 31.25 |
Higher incidence in males |
|
Co-morbidities |
Hypertension- 06 Diabetes Mellitus- 13 Hypothyroidism- 04 Acute Kidney Injury- 01 Tuberculosis-02 |
37.50 81.25 25 6.25 12.50 |
Strong positive correlation with diabetics |
|
Covid-19 RTPCR |
Positive- 16 |
75
|
Strong correlation with COVID-19 |
|
Treatment history of COVID-19 |
Steroids- 16 Remdesivir-16 Tocilizumab- 01 |
100 100 6.25 |
All cases received Steroid and Remdesivir |
|
Mucormycosis |
Confirmed- 16 |
100 |
All confirmed cases |
|
Location of mucormycosis |
Nasal/ Sinus- 16 Rhino-orbital- 14 Others- 00 |
100 87.50 0 |
An overlap was seen with rhino-orbital in patients with nasal/sinus mucormycosis |
|
Side affected |
Right- 11 Left- 04 Bilateral- 01 |
68.75 25 6.25 |
More involvement in right than left |
|
HRCT score |
0 to 7- 04 8-14- 05 15-25- 06 Unknown-01 |
25 31.25 37.50 6.25 |
More than half had Moderate to severe scores |
|
Mode of oxygenation |
Non-Invasive Ventilation (NIV)- 03 Face Mask- 06 Nasal Prongs- 03 None- 04 |
18.75 37.50 18.75 25 |
75% required O2 support |
|
KOH MOUNT (Nasal Swab Culture) |
Rhizopus oyzae - 12 Mucorales mycetes- 04 |
75 25 |
Majority were infected with Rhizopus species |
|
Outcome |
Improved- 04 Death-12 |
25 75 |
Poor prognosis |
Discussion
With the data from this study, we observed that mucormycosis was related with covid-19 infection, diabetes, rampant use of corticosteroid, prolonged hospitalization with mechanical ventilation. Mucormycosis is extremely rare in healthy individuals but it can predispose in immunocompromised conditions.
It mainly affects nose, sinuses, and orbit but can also involve central nervous system (CNS), skin, bones, heart, kidney and other organs. Rhino-orbital-cerebral mucormycosis (ROCM) is the commonest variety seen in clinical practice worldwide.It includes entire spectrum ranging from sino-nasal, rhino-orbital to rhino-orbital-cerebral disease. Even in this study, we observed that 100% patients had nasal and sinus involvement of which 87.5% patients had rhino-orbital involvement. Microbiological identification of the hyphae based on diameter, presence or absence of septa, branching angle (right or acute branching), and pigmentation, differentiates it from other fungal infections.
The 1950 Smith and Krichner criteria for the clinical diagnosis of mucormycosis are still considered to be gold standard and include-
(i)Black, necrotic turbinate's easily mistaken for dried, crusted blood,
(ii) Blood-tinged nasal discharge and facial pain, both on the same side,
(iii) Soft peri-orbital or peri-nasal swelling with discoloration and induration,
(iv) Ptosis of the eyelid, proptosis of the eyeball and complete ophthalmoplegia and, (v) Multiple cranial nerve palsies unrelated to documented lesions. [5]
Compared to results of other similar studies conducted globally, these findings suggest familiar relation of mucormycosis, diabetes and steroid use, in people with covid-19 infection.
Conclusion
All the previously recognized high-risk factors for mucormycosis were observed in our study such as increase incidence in diabetics, patients with immunocompromised state due to chronic illness or rampant use of corticosteroids, prolonged duration of hospitalization, elderly age. Since only 16 patients were included in this study, the results cannot be generalized for the local population of the country. Also, all patients included were COVID-19 positive, had history of steroid intake, it is difficult to establish a relationship between mucormycosis in non- diabetic COVID-19 who did not receive steroids. There was loss of follow up with the four recovered and discharged patients, hence post mucormycosis complications could not be concluded.
References
1. Kubin CJ, McConville TH, Dietz D, Zucker J, May M, Nelson B, et al. Characterization of Bacterial and Fungal Infections in Hospitalized Patients With Coronavirus Disease 2019 and Factors Associated With Health Care-Associated Infections. Open Forum Infect Dis 2021;8(6):ofab201.
2. Song G, Liang G, Liu W. Fungal Co-infections Associated with Global COVID-19 Pandemic: A Clinical and Diagnostic Perspective from China. Mycopathologia 2020;1–8.
3. Singh AK, Singh R, Joshi SR, Misra A. Mucormycosis in COVID-19: A systematic review of cases reported worldwide and in India. Diabetes Metab Syndr 2021;15(4):102146.
4.Mucormycosis [Internet]. [cited 2022 Apr 10];Available from: https://www.who.int/india/emergencies/coronavirus-disease-(covid-19)/mucormycosis
5. H.W. Smith, J.A. Kirchner Cerebral mucor-mycosis: a report of 3 cases Arch Otolaryngol, 68 (1950), pp. 715-726.
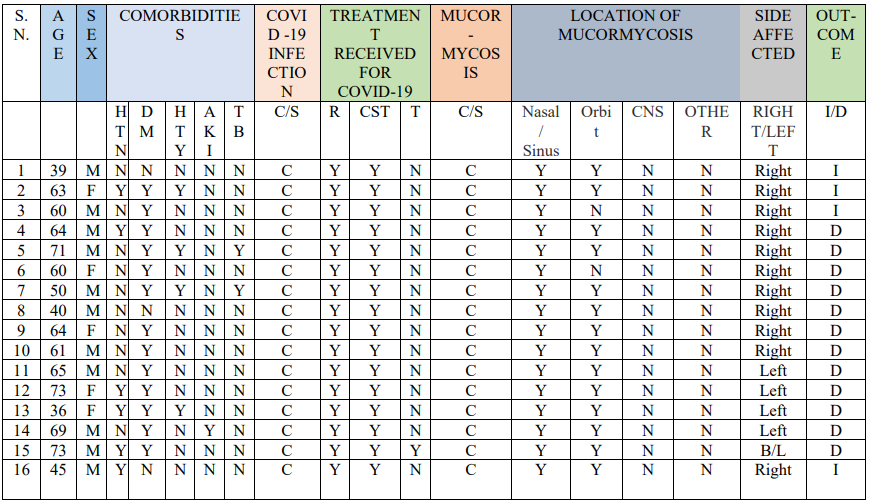
Figure 1
