Patients with Ventilator-Associated Pneumonia with Short-Course Antimicrobial Treatment
Patients with Ventilator-Associated Pneumonia with Short-Course Antimicrobial Treatment
Attapon Cheepsattayakorn1,2,3,4*, Ruangrong Cheepsattayakorn5, Porntep Siriwanarangsun2
1. Faculty of Medicine Vajira Hospital, Navamindradhiraj University, Bangkok, Thailand.
2. Faculty of Medicine, Western University, Pathumtani Province, Thailand.
3. 10th Zonal Tuberculosis and Chest Disease Center, Chiang Mai, Thailand.
4. Department of Disease Control, Ministry of Public Health, Thailand.
5. Department of Pathology, Faculty of Medicine, Chiang Mai University, Chiang Mai, Thailand.
Correspondence to: Attapon Cheepsattayakorn, 10th Zonal Tuberculosis and Chest Disease Center, 143 Sridornchai Road Changklan Muang Chiang Mai 50100 Thailand.
Copyright
© 2024 Attapon Cheepsattayakorn. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 30 Nov 2024
Published: 21 Dec 2024
Patients with Ventilator-Associated Pneumonia with Short-Course Antimicrobial Treatment
Pneumonia, the second most prevalent nosocomial infection among patients in critical care, affects almost 27% of all critically ill patients [1]. An estimated 86% of cases of nosocomial pneumonia are linked to mechanical ventilation and are referred to as ventilator-associated pneumonia (VAP) [1]. Due to instrumentation of the airway during mechanical ventilation, which lasts for >48 h, the architecture of the oropharynx and trachea may be affected. This may allow secretions and flora from the upper respiratory tract to infiltrate the lower respiratory system and affect the parenchyma of the lung which causes VAP [2]. Antimicrobial resistance is common in critically ill patients, hence prudent antibiotic use with appropriate coverage for the organisms targeted is vital [3]. VAP-related mortality has been estimated to be about 6% with excess risk estimates ranging between 0% and 50% [4-6]. Ventilator-associated pneumonia (VAP) is associated with increased mortality, prolonged hospitalization, excessive antimicrobial use and, consequently, increased antimicrobial resistance (Figure 1) [7].
The current literature on the optimal duration of antibiotic therapy for VAP is limited and restricted to the findings of a few clinical trials. Current guidelines for the length of management of VAP recommend a short-duration treatment of 7–8 days [8, 9] which was largely based on the evidence provided within the previous two meta-analyses [10, 11]. Meta-analysis conducted by Pugh et al. was published in 2015 and reported that short duration was non-inferior to the long duration for mortality and recurrence [12, 13]. Nevertheless, within the subgroup of patients with VAP due to non-fermenting Gram-negative bacilli (NF-GNB), a higher rate of recurrence of pneumonia in the short-duration therapy arm was found. Augmenting this concern, the results from a recently published randomized controlled trial (RCT), named “ iDIAPASON trial ”, conducted by Bougle et al. failed to demonstrate the non-inferiority of short-duration antimicrobial therapy in patients with VAP due to Pseudomonas aeruginosa because of a higher risk of recurrence of pneumonia with the shorter regimen. Nevertheless, this trial did not have a sample size large enough to make a definitive conclusion. A recent study was conducted between May 25, 2018, and Dec 16, 2022, 461 patients were enrolled and randomly assigned to the short-course treatment group (n=232) or the usual care group (n=229) [7]. After excluding one withdrawal (231 in the short-course group, and 229 in the usual care group), median age was 64 years (IQR 51-74) and 181 (39%) participants were female. 460 were included in the intention-to-treat analysis and in the per-protocol population; 435 participants received the allocated treatment and fulfilled eligibility criteria. Median antimicrobial treatment duration for the index episodes of VAP was 6 days (IQR : 5-7) in the short-course group and 14 days (10-21) in the usual care group. In comparison with 100 (44%) of 229 in the usual care group (risk difference -3% [one-sided 95% CI -∞ to 5%]), compared with 95 (41%) of 231 participants in the short-course group met the primary outcome. The study results were similar in the per-protocol population. In analyses, although superiority compared with usual care was not established, non-inferiority of short-course antibiotic treatment was met [7].
In conclusion, in light of the previous uncertainty and the availability of newer data, there is a need to re-evaluate systematically the optimal duration of antibiotic therapy for VAP, especially due to NF-GNB. VAP is associated with excessive antimicrobial use, increased antimicrobial resistance, prolonged hospitalization, and increased mortality. Individualized, short-course antimicrobial treatment for VAP could help to reduce the burden of side-effects and the risk of antibiotic resistance in high-resource and resource-limited settings (Figure 2) [13, 14].
Figure 1 : Demonstrating percentage of patients with VAP died or experienced pneumonia recurrence at day 60 [7].
Figure 2 : Demonstrating absolute risk difference (one-side 95 % CI) of short-course antimicrobial treatment strategy compared with usual course antimicrobial treatment strategy [13, 14].
References
1. G. Dimopoulos et al. Short- vs long-duration antibiotic regimens for ventilator-associated pneumonia. Chest (2013).
2. M. Fekih Hassen et al. Durée de l’antibiothérapie lors du traitement des pneumopathies acquises sous ventilation mécanique : comparaison entre sept jours et dix jours. Étude pilote. Ann Fr Anesth Reanim (2009).
3. M.J. Richards et al. Nosocomial infections in medical intensive care units in the United States. Crit Care Med (1999).
4. S. Amanullah et al. What are ventilator-associated pneumonias/ventilator-associated events and how to reduce their prevalence in your hospital. Medscape. Post online : December 2015.
5. S.M. Koenig et al. Ventilator-associated pneumonia: diagnosis, treatment, and prevention. Clin Microbiol Rev (2006).
6. L. Papazian et al. Effect of ventilator-associated pneumonia on mortality and morbidity. Am J Respir Crit Care Med (1996).
7. Mo Y, Booraphun S, Li AY, Domthong P, Kayastha G, Lau YH, Chetchotisakd P, Limmathurotsakul D, Tambyah PA, Cooper BS; REGARD-VAP investigators. Individualized, short-course antibiotic treatment versus usual long-course treatment for ventilator-associated pneumonia (REGARD-VAP): a multicenter, individually randomized, open-label, non-inferiority trial. Lancet Respir Med. 2024 May;12(5):399-408.
DOI : 10.1016/S2213-2600(23)00418-6
8. J.F. Timsit et al. Attributable mortality of ventilator-associated pneumonia
Curr Opin Crit Care (2011).
9. J. Steen et al. Attributable mortality of ventilator-associated pneumonia. Replicating findings, revisiting methods. Ann Am Thorac Soc (2020).
10. A.C. Kalil et al. Management of Adults with Hospital-acquired and Ventilator-associated Pneumonia: 2016 clinical practice guidelines by the Infectious Diseases Society of America and the American Thoracic Society.
Clin Infect Dis (2016).
11. A. Torres et al. International ERS/ESICM/ESCMID/ALAT guidelines for the management of hospital-acquired pneumonia and ventilator-associated pneumonia. Eur Respir J (2017).
12. R. Pugh et al. Short-course versus prolonged-course antibiotic therapy for hospital-acquired pneumonia in critically ill adults. Cochrane Database Syst Rev (2015).
13. Mo, YinMo, Yin et al. Individualised, short-course antibiotic treatment versus usual long-course treatment for ventilator-associated pneumonia (REGARD-VAP): a multicentre, individually randomised, open-label, non-inferiority trial. The Lancet Respiratory Medicine, Volume 12, Issue 5, 399 – 408.
14. Hornick I. Individualized short antibiotic course non-inferior to usual course in VAP. Post online : February 5, 2024.
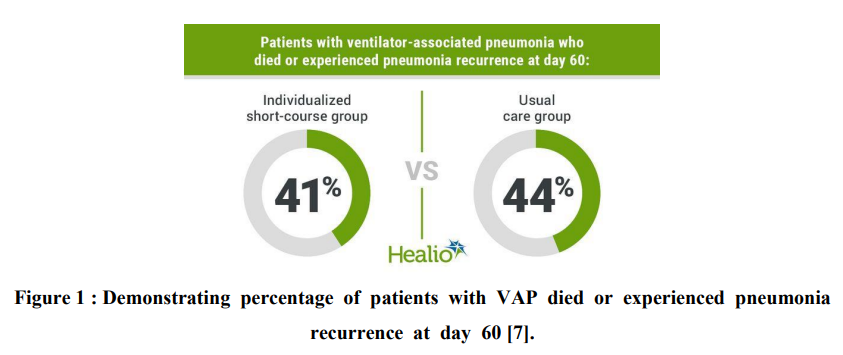
Figure 1
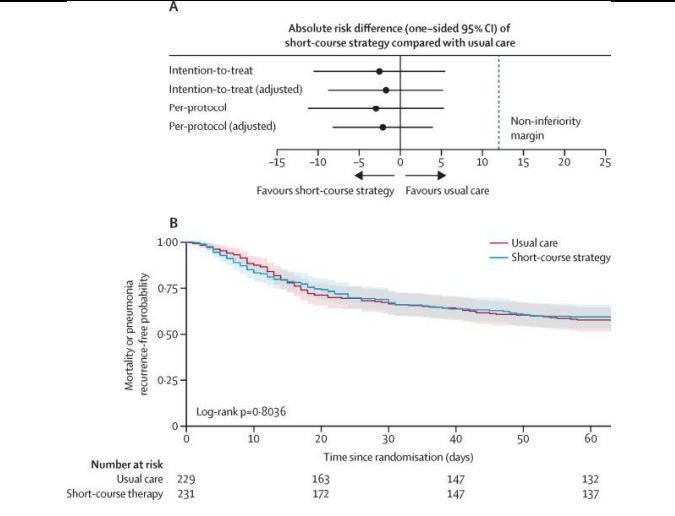
Figure 2
