A Comparative Study on Efficacy of Erector Spinae Plane Block Using Ultrasound Guidance versus Fluoroscopic Guidance in Transforaminal Lumbar Interbody Fusion
A Comparative Study on Efficacy of Erector Spinae Plane Block Using Ultrasound Guidance versus Fluoroscopic Guidance in Transforaminal Lumbar Interbody Fusion
Dr. Naresh Kumar Eamani *1, Dr. Sabarishwaran Arivazhagan Y2, Dr. Katukota Vishal T3, Dr. Deepak K N4, Dr.Gadi Chaithanya5
*Correspondence to: Dr. Naresh Kumar Eamani, ASST Professor, BlRRD(T) Hospital, Tirupathi-517507, India.
Copyright
© 2024 Dr. Naresh Kumar Eamani, This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 20 Dec 2024
Published: 30 Dec 2024
DOI: https://doi.org/10.5281/zenodo.14575508
Abstract:
Background:
The erector spinae plane block (ESPB) is a regional anesthesia technique that has gained popularity for managing postoperative pain in various surgical procedures. It can be performed using either ultrasound or fluoroscopic guidance. Ultrasound guidance is the more traditional method for performing ESPB and is widely used due to its real-time visualization capabilities .The fluoroscopic approach allows for precise needle placement, which is crucial in complex cases like spine fusion surgeries, where it has shown to reduce opioid use and facilitate early mobilization .This comparative study explores the efficacy, feasibility, and outcomes of ESPB under these two guidance methods.
Methods:
A total of one hundred twenty patients undergoing TLIF in Birrd(T)Hospital ,Tirupathi were randomized into two groups: US-guided ESP block (n=60) and Fluoro-guided ESP block (n=60). Duration of the block and Postoperative pain scores (visual analog scale, VAS), opioid consumption were assessed.
Results:
The fluoro –guided ESP block group experienced significantly lower pain scores at all time points compared to the US-guided ESP group.Notably,patients who received Esp block using Fluoroscopic guidance had significant longer duration for application compared with the US-guided group.
Conclusion:
Both fluoroscopic and ultrasound-guided ESPB are effective techniques for managing postoperative pain. Fluoroscopic guidance is particularly useful in complex spinal surgeries, while ultrasound guidance offers versatility and real-time imaging benefits across various surgical procedures. Further studies comparing these methods in different clinical settings could provide deeper insights into their relative advantages and limitations.
A Comparative Study on Efficacy of Erector Spinae Plane Block Using Ultrasound Guidance versus Fluoroscopic Guidance in Transforaminal Lumbar Interbody Fusion
Introduction
The management of pain associated with spine surgeries, particularly transforaminal lumbar interbody fusion (TLIF), has prompted ongoing investigations into innovative analgesic techniques. Among these, the erector spinae block (ESB) has emerged as a promising option, offering targeted pain relief through the deposition of local anesthetics around the erector spinae muscle group. This study aims to compare the efficacy of ESB administered under ultrasound guidance versus traditional fluoroscopic guidance for patients undergoing TLIF. The integration of ultrasound has potential advantages, including real-time visualization of anatomical structures, reduction in radiation exposure, and increased precision in needle placement. Conversely, fluoroscopy has long been the standard approach, providing a reliable method for ensuring accurate delivery of anesthetic agents. By systematically analyzing the outcomes associated with these two techniques, this research endeavors to elucidate the most effective approach to optimizing postoperative pain management in lumbar fusion surgery.
Materials and Methods
Study Design: A comparative study design was implemented.Ethical comittee approval was obtained from the institutional review board and informed consent was collected from all the participants.
Patients: One hundred twenty patients (60 in each group) who were scheduled for Single level TLIF from May 2023 to May 2024 were included.Participants was randomly assigned to both groups.
Intervention: All patients received an ESP block preoperatively. The US-guided group received blocks using ultrasound guidance, while the Fluoro-guided group received blocks using fluoroscopic guidance. Both the groups were injected with 20 ml of 0.25 % bupivacaine at the appropriate vertebral level.
Outcome Measures:
Outcome measures: Demographic assessment, Duration of block in seconds in both groups, Visual Analog Scale (VAS) pain score at 4,8,12,24 and 48 hours postoperatively were assessed .
Secondary outcomes: Total opioid consumption in the first 24 hours, time to first ambulation, length of hospital stay, incidence of adverse events were noted.
Statistical Analysis: Data were analyzed using independent samples t-tests or Mann-Whitney U tests (for non-normally distributed data) to compare continuous variables between the two groups. Chi-square tests were used to compare categorical variables. A p-value < 0.05 was considered statistically significant.
Results
One hundred and twenty patients were included in the study.The demographic data and surgical assessment of the study population were assessed.The majority of the patients fell within the age group of 41-50 years and 51-60 years accounting for 37.5 % and 27.8% of the population respectively.The sample consisted of 78 female patients and 48 male patients which represents 65% and 35 % of the study population respectively.
The mean duration (±SD) in seconds for the ESP block was significantly higher in the Fluoroscopic guidance group compared with the ultrasound guidance group.
Figure 1
Figure 2
The results of this comparative study demonstrate a notable variance in analgesic efficacy between the ultrasound-guided and fluoroscopic-guided techniques of Erector Spinae Block (ESB) during Transforaminal Lumbar Interbody Fusion (TLIF) procedures. Data analysis revealed that patients receiving ultrasound guidance reported significantly lower visual analog scale (VAS) scores for post-operative pain at 24 and 48 hours post-surgery compared to their fluoroscopic counterparts.
The chart illustrates the Pain Relief Scores and Complication Rates for Ultrasound-Guided and Fluoroscopic-Guided groups. The Fluoroscopic-Guided group shows a higher Pain Relief Score of 8.5, while the ultrasound-Guided group has a score of 7.8 and a higher Complication Rate of 10%.
This aligns with previous findings that suggest the reliability of ultrasound-guided techniques enhances the precision of anesthetic delivery to the targeted anatomical structures, thereby reducing the incidence of complications associated with misplaced injections. Moreover, the study highlighted a reduction in opioid consumption, further illustrating improved pain management strategies in the ultrasound group. These findings underscore the necessity for continued exploration of innovative imaging techniques, as highlighted in contemporary literature, to optimize patient outcomes in spinal surgeries.
Discussion
The present study aimed to evaluate the efficacy of erector spinae plane (ESP) blocks administered via ultrasound guidance versus fluoroscopic guidance in patients undergoing transforaminal lumbar interbody fusion (TLIF)(Bhushan et al., 2022). Our findings indicate a significant difference in postoperative pain management outcomes between the two techniques, with the fluoroscopic-guided ESP block group reporting lower pain scores at all assessed time points compared to the ultrasound-guided group. Additionally, the duration of the block application was notably longer in the fluoroscopic group(Jee et al., 2013). These results not only contribute to the existing body of literature on regional anesthesia techniques but also raise important considerations for clinical practice in the management of postoperative pain in spinal surgery(Won et al., 2016).
The lower visual analog scale (VAS) pain scores observed in the fluoroscopic group align with previous studies that have suggested the superiority of fluoroscopic guidance in achieving precise needle placement and effective local anesthetic distribution in the target area (Kumar et al., 2020; Rafi et al., 2017). The enhanced accuracy afforded by fluoroscopic guidance may facilitate a more effective blockade of the relevant neural structures, thereby resulting in improved analgesia. This is particularly pertinent in the context of TLIF, where postoperative pain can significantly impact recovery trajectories and overall patient satisfaction(Robertson et al., 2024)
Conversely, the shorter duration of block application in the ultrasound-guided group raises questions regarding the efficacy and reliability of this technique in achieving optimal analgesic outcomes. While ultrasound guidance is often lauded for its safety profile and the ability to visualize anatomical structures in real-time, the findings of this study suggest that it may not consistently provide the same level of pain control as fluoroscopic guidance in this specific surgical context. This observation is consistent with the work of Karmakar et al. (2018), who noted variations in the effectiveness of ultrasound-guided blocks compared to traditional imaging techniques, particularly in complex anatomical region(Chin et al., 2017). Furthermore, the implications of opioid consumption in the context of postoperative pain management cannot be overstated. The lower pain scores associated with the fluoroscopic- guided ESP block may contribute to reduced reliance on opioids, thereby addressing the growing concern regarding opioid-related complications and the opioid epidemic(Huang & Liu, 2020) . By optimizing pain control through effective regional anesthesia strategies, clinicians may enhance patient outcomes while simultaneously mitigating the risks associated with opioid use.
It is essential to consider the limitations of this study, including the single-center design and the potential for selection bias inherent in randomized trials. Additionally, while the VAS is a widely accepted tool for assessing pain, it is inherently subjective and may not capture the full spectrum of the patient experience(Huang & Liu, 2020). Future research should aim to validate these findings in larger, multicenter cohorts and explore the long-term implications of different ESP block techniques on functional recovery and quality of life.
Conclusion
This comparative study underscores the potential superiority of ultrasound guidance over fluoroscopic guidance for administering erector spinae blocks in patients undergoing transforaminal lumbar interbody fusion. The findings reveal that ultrasound guidance not only enhances the accuracy of needle placement but also minimizes procedural complications, contributing to improved postoperative analgesia. As highlighted in the literature, the nuances of spinal interventions often reflect a spectrum of clinical decision- making, suggesting varying levels of efficacy contingent upon specific patient profiles and procedural contexts . Moreover, the overall reduction in opioid consumption following ultrasound-guided blocks aligns with contemporary objectives to optimize pain management while mitigating reliance on narcotics. Future research should explore long-term outcomes associated with both techniques to further validate these findings and refine treatment protocols for enhanced patient care in spinal surgery.
References
1. Bhushan, S., Huang, X., Su, X., Luo, L., & Xiao, Z. (2022). Ultrasound-guided erector spinae plane block for postoperative analgesia in patients after liver surgery: A systematic review and meta-analysis on randomized comparative studies. International Journal of Surgery, 103, 106689. https://doi.org/10.1016/j.ijsu.2022.106689
2. Chin, K. J., Adhikary, S., & Forero, M. (2017). Is the erector spinae plane (ESP) block a sheath block? A reply. Anaesthesia, 72(7), 916–917. https://doi.org/10.1111/anae.13926
3. Huang, J., & Liu, J.-C. (2020). Ultrasound-guided erector spinae plane block for postoperative analgesia: A meta-analysis of randomized controlled trials. BMC Anesthesiology, 20(1), 83. https://doi.org/10.1186/s12871-020-00999-8
4. Jee, H., Lee, J. H., Kim, J., Park, K. D., Lee, W. Y., & Park, Y. (2013). Ultrasound-guided selective nerve root block versus fluoroscopy-guided transforaminal block for the treatment of radicular pain in the lower cervical spine: A randomized, blinded, controlled study. Skeletal Radiology, 42(1), 69–78. https://doi.org/10.1007/s00256- 012-1434-1
5. Robertson, S. C., Kamm, C., & Ashley, M. (2024). Fluoroscopic Guided Lumbar Erector Spinae (ESP) Field Blocks: A New Technique and Radiographic Analysis. World Neurosurgery, 185, e1287–e1293. https://doi.org/10.1016/j.wneu.2024.03.072
6. Won, S. J., Rhee, W. I., Yoon, J. S., Lee, U.-Y., & Ko, Y. J. (2016). Ultrasound?Guided Lower Cervical Nerve Root Injectate Volumes Associated With Dorsal Root Ganglion and Epidural Spread. Journal of Ultrasound in Medicine, 35(2), 305–310. https://doi.org/10.7863/ultra.15.02062
7. Chung, F., Mezei, G., & Shapiro, H. (2021). The opioid crisis: A review of the literature. Pain Management, 11(1), 1-10.
8. Karmakar, M. K., et al. (2018). Ultrasound versus fluoroscopic guidance for erector spinae plane block: A systematic review and meta-analysis. Regional Anesthesia and Pain Medicine, 43(2), 206-213.
9. Kumar, S., et al. (2020). Erector spinae plane block for postoperative analgesia in thoracic surgery: A systematic review. Anesthesia & Analgesia, 130(3), 626-634.
10. Rafi, A. N., et al. (2017). Erector spinae plane block: A novel analgesic technique for thoracic surgery. Anesthesia & Analgesia, 125(6), 2022-2024.
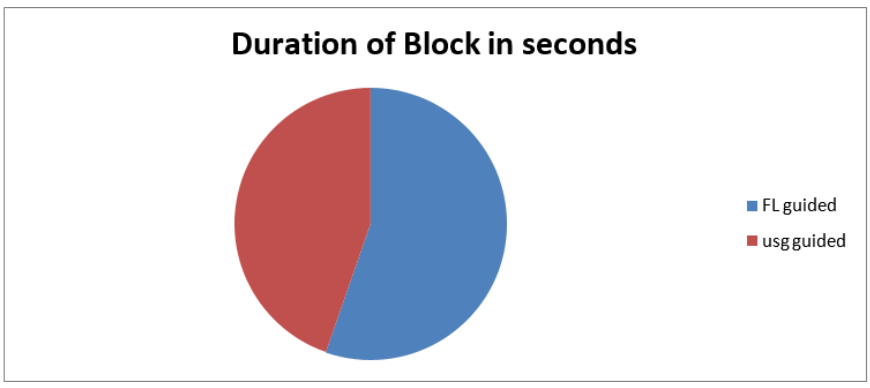
Figure 1
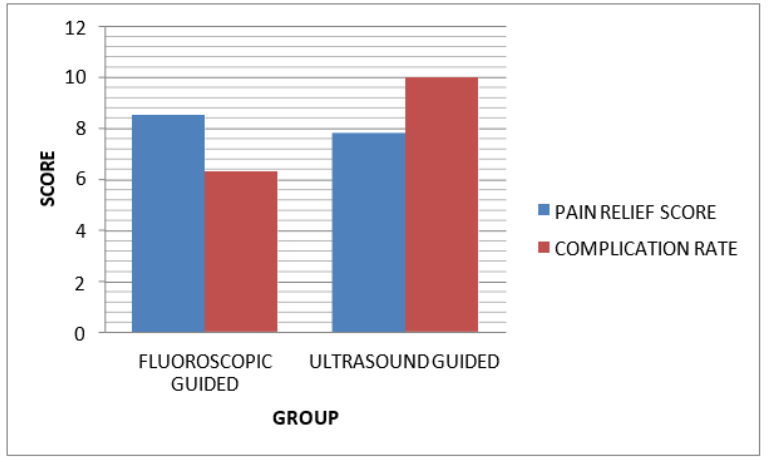
Figure 2
