The Importance of Nutritional Status in Oral and Maxillofacial Surgery and Postoperative Healing.
The Importance of Nutritional Status in Oral and Maxillofacial Surgery and Postoperative Healing.
Alayna B. Smiley *
*Correspondence to: Alayna B. Smiley MD, DMD, MPH.
Copyright.
© 2025 Alayna B. Smiley. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 07 Jan 2025
Published: 18 Jan 2025
DOI: https://doi.org/10.5281/zenodo.14711123
Abstract
Nutritional status plays a critical role in patient outcomes following oral and maxillofacial surgery. This article explores the physiological demands of surgery, highlighting the relationship between preoperative and postoperative nutritional status, wound healing, and recovery. The importance of assessing a patient’s nutritional status before surgery is outlined, alongside practical dietary recommendations to optimize healing. Special attention is given to the role of key nutrients such as proteins, fats, vitamins, and minerals, along with pre- and postoperative diet strategies. Additionally, a 7-day pre-surgical meal plan, a 14-day postoperative vegan meal plan, and the use of digital tools for healthy food selections are provided to aid clinicians in improving surgical outcomes through nutrition.
The Importance of Nutritional Status in Oral and Maxillofacial Surgery and Postoperative Healing.
Introduction
Oral and maxillofacial surgery (OMFS) involves a range of complex procedures that place significant physiological demands on the body. The patient’s nutritional status is an often overlooked but vital component of both surgical planning and postoperative recovery. Malnutrition, both undernutrition and overnutrition, can compromise immune function, delay tissue regeneration, and increase the risk of postoperative complications, such as infection and poor wound healing. Research indicates that optimized nutrition supports the body's healing capacity by providing essential nutrients needed for collagen production, wound closure, and immune system support (Martinez & Rodriguez, 2019).
This article aims to establish the significance of evaluating nutritional status in OMFS patients and to provide evidence-based dietary recommendations for pre- and postoperative care to enhance recovery outcomes. Additionally, the integration of digital tools and applications that assist patients in making healthy food selections is discussed to support ongoing nutritional management.
Objectives
- Explore the gaps in nutrition education in medical and dental schools and their impact on healthcare.
- Adding a nutrition health questionnaire to patient intake forms
- Evaluate the impact of nutritional status on surgical outcomes.
- Explain the physiological demands of surgery and the role of nutrition in supporting healing.
- Review critical nutrients necessary for postoperative recovery.
- Provide dietary recommendations for pre- and postoperative care, including vegan-specific plans.
- Introduce digital tools and applications that aid in maintaining a healthy diet for surgical patients.
The Lack of Nutritional Training in Dental and Medical Schools and Its Impact on Patient Healing
Despite the well-documented importance of nutrition in patient outcomes, both medical and dental schools often fail to adequately incorporate nutritional training into their curricula. This oversight limits practitioners' ability to use dietary interventions as part of comprehensive patient care, including post-surgical recovery in oral and maxillofacial surgery. Studies suggest that the lack of nutritional education contributes to a major gap in care, where patients are not adequately informed or supported in making dietary choices that could significantly enhance healing.
Lack of Nutritional Training in Medical and Dental Schools
- Minimal Nutrition Education Hours: Research shows that most U.S. medical schools provide only 19 to 24 hours of nutrition education across four years of training, which is far below the recommended 25–30 hours proposed by the National Academy of Sciences (Adams et al., 2010). Dental schools tend to allocate even fewer hours, focusing primarily on procedural and technical aspects of care, rather than integrative approaches that include nutrition (Maguire & Franklin, 2016).
- Impact on Patient Outcomes: The lack of formal nutritional education is problematic because inadequate dietary guidance can hinder healing, particularly in surgical patients. Patients are often unaware that consuming nutrient-dense foods before and after surgery can enhance immune function, reduce inflammation, and accelerate tissue repair. Without proper knowledge from healthcare providers, patients miss the opportunity to make informed dietary choices, leading to suboptimal recovery outcomes (Frantz et al., 2011).
- Surgeons and Dentists Feel Underprepared: Surveys of physicians and dental professionals consistently report that they feel ill-equipped to provide dietary counseling. A 2018 study revealed that fewer than 14% of practicing physicians felt confident in offering nutritional advice, and the numbers are even lower among dentists (Vetter et al., 2008). This gap highlights how the lack of nutritional training fails to meet patient needs, especially in surgery where recovery is directly impacted by nutritional status.
- Inadequate Focus on Clinical Nutrition: Many dental and medical programs place little emphasis on clinical nutrition, which involves understanding how specific nutrients affect recovery from trauma, surgery, or illness. For example, medical students may learn about vitamins and minerals in a general context but not about the practical application of dietary changes in surgical recovery (Crowley et al., 2019). This leaves future practitioners underprepared to integrate nutrition into their treatment plans for oral and maxillofacial surgeries, where targeted dietary interventions could significantly reduce complications and improve healing times.
Nutritional Health Questionnaire for Patient Intake
To address the gap in dietary assessment during the pre-surgical planning phase, the following Nutritional Health Questionnaire should be included in the preliminary intake forms for all patients undergoing oral or other types of surgery. This questionnaire aims to identify potential nutritional deficiencies or issues that could impact the patient’s healing process:
Nutritional Health Questionnaire
Patient Name: ___________
Date of Birth: ___________
Date of Surgery: ___________
1. Weight and Appetite Changes
- Have you experienced any significant weight loss or gain in the past six months?
- ? Yes
- ? No
- If yes, please explain: _________________________________________
- Has your appetite changed recently?
- ? Yes
- ? No
- If yes, please explain: _________________________________________
2. Dietary Habits
- How would you describe your typical daily diet?
- ? Balanced (includes a variety of proteins, fruits, vegetables, grains, and fats)
- ? High in processed foods (fast food, packaged snacks, etc.)
- ? Low in essential nutrients (fruits, vegetables, whole grains, proteins)
- ? Other: ___________________________________________
3. Protein Intake
- Do you regularly consume sources of protein such as meat, fish, eggs, dairy, or plant-based alternatives (e.g., beans, tofu)?
- ? Yes
- ? No
- If no, please explain why: _______________________________________
4. Vitamin and Mineral Intake
- Are you currently taking any vitamins or supplements (e.g., multivitamins, vitamin D, vitamin C, zinc, calcium)?
- ? Yes
- ? No
- If yes, please list: ___________________________________________
5. Hydration
- How many glasses of water or other hydrating fluids do you consume daily?
- ? 0-3
- ? 4-7
- ? 8-10
- ? More than 10
6. Food Allergies or Intolerances
- Do you have any known food allergies or intolerances?
- ? Yes
- ? No
- If yes, please list: ___________________________________________
7. Special Diets
- Are you following any specific dietary pattern (e.g., vegan, vegetarian, gluten-free)?
- ? Yes
- ? No
- If yes, please specify: __________________________________________
8. Recent Illnesses
- Have you had any recent illnesses that might affect your nutritional status (e.g., gastrointestinal disorders, infections)?
- ? Yes
- ? No
- If yes, please describe: ________________________________________
9. Alcohol and Tobacco Use
- Do you consume alcohol?
- ? Yes
- ? No
- If yes, how often? ___________________________________________
- Do you smoke or use tobacco products?
- ? Yes
- ? No
- If yes, how often? ___________________________________________
10. Physical Activity
- How often do you engage in physical exercise?
- ? Never
- ? 1-2 days per week
- ? 3-5 days per week
- ? Daily
11. Stress and Eating Patterns
- How would you describe your current stress level?
- ? Low
- ? Moderate
- ? High
- Does stress affect your eating habits?
- ? Yes
- ? No
- If yes, please explain: __________________________________________
This Nutritional Health Questionnaire aims to uncover potential nutritional risk factors that could compromise healing. By integrating it into the standard patient intake process, healthcare providers can identify areas where intervention, such as dietary recommendations or supplementation, may improve post-surgical outcomes.
1. The Role of Nutritional Status in Surgical Outcomes
Surgical outcomes, particularly in oral and maxillofacial procedures, are closely linked to the patient’s nutritional state. Key elements of nutrition, such as protein, micronutrients, and fat reserves, influence tissue healing, immune response, and recovery time.
1.1 Tissue Healing and Regeneration
The body's capacity for tissue repair during OMFS is contingent upon an adequate supply of essential nutrients. Protein, specifically amino acids like arginine and glutamine, is vital for collagen production, which forms the backbone of tissue regeneration (Weimann & Braga, 2021). Deficiencies in these nutrients can impair wound healing, increase infection risk, and prolong recovery time.
1.2 Immune Function
Surgical stress exacerbates the body's immune demands. Nutritional deficiencies, particularly in vitamins A, C, and D, as well as zinc, impair the immune response, increasing susceptibility to infection and inflammation (Kahn & Chang, 2021). Adequate intake of these micronutrients preoperatively can enhance immune function and reduce postoperative complications.
1.3 Nutritional Risk Factors
Patients with malnutrition, obesity, or chronic conditions such as diabetes exhibit higher rates of surgical complications. Studies indicate that poor preoperative nutritional status increases the risk of postoperative complications three- to fourfold (Zikria & Bianchi, 2020). Additionally, the American College of Surgeon (2024) demonstrated that patient with albumin levels lower than 3.0 have higher post-op complications in GI surgeries.
1.4 Inflammation and Catabolism
Surgery induces a catabolic state, wherein the body’s muscle protein breakdown accelerates, leading to muscle atrophy and delayed recovery (Ferlay et al., 2018). Adequate preoperative nutrition, particularly a diet rich in high-quality protein, mitigates these risks by providing the necessary reserves to support the increased metabolic demands.
Fig 1
2. Physiological Demands of Surgery and Nutritional Support for Healing
Surgical recovery is divided into three distinct phases, each with specific nutritional requirements.
2.1 Phases of Wound Healing
- Inflammatory Phase (Days 0–3): Key nutrients such as protein, vitamin C, and zinc are critical for modulating inflammation and supporting tissue repair (McKenzie & Jenkins, 2022).
- Proliferative Phase (Days 3–21): Collagen synthesis peaks, requiring increased protein intake, particularly amino acids like glutamine and arginine, alongside vitamin C (Weimann & Braga, 2021).
- Remodeling Phase (Weeks 3–12): Long-term nutritional support is needed to ensure tissue strength and function are fully restored, with a continued emphasis on protein, vitamins A, C, and D (Patel & John, 2021).
2.2 Key Nutrients for Surgery and Recovery
- Protein: Vital for collagen formation, immune support, and tissue repair (Kahn & Chang, 2021).
- Fats: Essential fatty acids, such as omega-3s, reduce inflammation and support cellular repair (Weimann & Braga, 2021).
- Vitamins and Minerals: Vitamins C and D, zinc, and iron are critical for collagen production, bone healing, and immune function (Martinez & Rodriguez, 2019).
3. Pre- and Postoperative Nutritional Recommendations
A well-structured diet plan, beginning at least 7 days pre-surgery and extending to 14 days post-surgery, can significantly enhance recovery outcomes. The goal is to optimize nutritional status to support recovery, boost the immune system, and reduce the risk of post-operative complications. For a detailed meal plan example see Appendix A. Exodontia patients should avoid eating small seeds postoperatively which can potentially get trapped in the extraction site.
3.1 Preoperative Diet (7 Days Before Surgery)
- Protein: Patients should consume 1.2–2.0 grams of protein per kilogram of body weight per day. Sources include lean meats, fish, legumes, and plant-based proteins (Ferlay et al., 2018).
- Hydration: Maintaining hydration with at least 8–10 glasses of water daily is essential for blood flow and healing (National Institutes of Health, 2019).
- Micronutrients: Ensure adequate intake of vitamins A, C, and D, and zinc to promote immune function and wound healing (Zikria & Bianchi, 2020).
3.2 Postoperative Diet (14 Days After Surgery)
- Days 1–3: Focus on soft, easy-to-eat foods such as blended vegetable soups, protein shakes, and mashed fruits to minimize discomfort (Kahn & Chang, 2021).
- Days 4–7: Gradually reintroduce soft solids, emphasizing high-protein meals and anti-inflammatory foods such as leafy greens and omega-3-rich fish (Patel & John, 2021).
- Days 8–14: Introduce more textured foods while maintaining high protein intake and focusing on hydration and fiber to prevent constipation (Weimann & Braga, 2021).
3.3 Nutritional Supplements
For patients unable to meet their nutritional needs through diet alone, consider recommending:
- Protein Supplements: Whey or plant-based protein powders to ensure adequate protein intake (Ferlay et al., 2018).
- Multivitamins: A high-quality multivitamin can help fill nutritional gaps (McKenzie & Jenkins, 2022).
- Omega-3 Fatty Acids: Supplements can aid in reducing inflammation (Zikria & Bianchi, 2020).
3.4 Digital Tools and Applications for Healthy Food Selection
Incorporating digital tools can assist patients in maintaining a healthy diet by providing easy access to nutritional information and personalized meal planning.
- Yuka: An app that scans food products to provide detailed information on their nutritional quality and potential health impacts. It helps users make informed choices by highlighting healthier alternatives (Yuka, n.d.).
- MyFitnessPal: A comprehensive app for tracking diet and exercise. It offers a vast database of foods, making it easier for patients to monitor their nutrient intake and stay within their dietary goals (MyFitnessPal, n.d.).
- Lifesum: Provides personalized diet plans based on user preferences and health goals. It helps users track their meals and offers suggestions for healthier food choices (Lifesum, n.d.).
- Fooducate: An app that grades foods based on their nutritional value and offers healthier alternatives. It educates users on reading food labels and understanding ingredient lists (Fooducate, n.d.).
- Cronometer: Offers detailed nutrient tracking, ensuring that patients meet their micronutrient needs. It is especially useful for those following specific dietary restrictions, such as vegan diets (Cronometer, n.d.).
These applications can empower patients to take control of their nutritional intake, ensuring they receive the necessary nutrients to support their surgical recovery. See Appendix B
4. Special Considerations: Vegan Meal Plans
For vegan patients, tailored meal plans focusing on plant-based proteins and nutrient-rich vegetables are essential to meet pre- and postoperative nutritional needs. A 7-day pre-surgery and 14-day post-surgery vegan meal plan are provided in this article, emphasizing foods rich in vitamins A, C, zinc, and omega-3s (Simopoulos, 2002). See Appendix C.
Conclusion
Proper nutrition before and after oral and maxillofacial surgery is crucial for optimizing healing and reducing complications. By incorporating nutritional assessments, tailored diet plans, and digital tools into surgical care, practitioners can significantly improve patient outcomes. Further studies are encouraged to explore the long-term impact of nutritional interventions on surgical recovery, particularly in vegan populations.
Appendix A: Detailed Meal Plans and Recipes
7-Day Preoperative Meal Plan
Day 1: Building Nutritional Reserves
- Breakfast: Oatmeal with chia seeds, topped with fresh blueberries and a drizzle of honey.
Why: Oats are a great source of fiber for gut health, while chia seeds and blueberries provide antioxidants and omega-3s for inflammation control (Simopoulos, 2002). - Snack: Greek yogurt with a handful of almonds.
Why: Greek yogurt is high in protein and probiotics for gut health, and almonds provide healthy fats and vitamin E (Weimann & Braga, 2021). - Lunch: Grilled chicken salad with mixed greens, cucumbers, tomatoes, and olive oil vinaigrette.
Why: Chicken provides lean protein, essential for tissue repair, while olive oil and leafy greens add vitamins A and C for reducing inflammation and promoting skin healing (Kahn & Chang, 2021). - Snack: Apple slices with natural peanut butter.
Why: Apples are rich in fiber and antioxidants, while peanut butter adds protein and healthy fats (Zikria & Bianchi, 2020). - Dinner: Baked salmon with steamed asparagus and quinoa.
Why: Salmon is rich in omega-3 fatty acids, which have anti-inflammatory properties, while asparagus and quinoa are loaded with essential vitamins and protein for recovery (Patel & John, 2021).
Day 2: Focus on Anti-inflammatory Foods
- Breakfast: Scrambled eggs with avocado and a side of whole grain toast.
Why: Eggs are an excellent source of high-quality protein, and avocados provide healthy fats and potassium to reduce inflammation and support tissue health (Weimann & Braga, 2021). - Snack: A small bowl of mixed berries (strawberries, raspberries, and blueberries).
Why: Berries are high in antioxidants and vitamin C, which support immune function and collagen production (McEvoy et al., 2018). - Lunch: Grilled turkey breast wrap with spinach, cucumbers, and hummus in a whole wheat tortilla.
Why: Turkey is a lean protein source, while hummus provides plant-based protein and fiber. Spinach offers iron and vitamin C, which are crucial for healing and immune support (Zikria & Bianchi, 2020). - Snack: Cottage cheese with pineapple chunks.
Why: Cottage cheese offers protein and calcium, and pineapple contains bromelain, an enzyme that reduces swelling (Ferlay et al., 2018). - Dinner: Lentil soup with carrots, celery, and onions, served with whole grain bread.
Why: Lentils are high in plant-based protein and fiber, which help maintain energy and support digestion during recovery (Weimann & Braga, 2021).
Day 3: Hydration and Vitamin Boost
- Breakfast: Smoothie with spinach, banana, Greek yogurt, and a scoop of protein powder.
Why: Spinach is rich in iron and folate, Greek yogurt provides probiotics, and bananas add potassium for hydration (Patel & John, 2021). - Snack: Carrot sticks with hummus.
Why: Carrots provide beta-carotene (vitamin A precursor), which is essential for skin healing, while hummus adds plant-based protein (Li & Zhou, 2016). - Lunch: Grilled tilapia with brown rice and steamed broccoli.
Why: Tilapia is a lean protein source, and broccoli offers vitamin C and fiber, essential for immune function and collagen formation (Weimann & Braga, 2021). - Snack: A handful of walnuts and a small orange.
Why: Walnuts are rich in omega-3 fatty acids, and oranges provide vitamin C for collagen production and immune support (Simopoulos, 2002). - Dinner: Chicken stir-fry with bell peppers, onions, and mushrooms, served over quinoa.
Why: Chicken is a high-quality protein, while bell peppers and mushrooms are rich in vitamins C and D, both essential for tissue repair and immune health (Patel & John, 2021).
Day 4: Focusing on Zinc and Vitamin C
- Breakfast: Whole wheat toast with smoked salmon and a side of sliced tomatoes.
Why: Smoked salmon provides omega-3s and protein, and tomatoes are rich in lycopene and vitamin C, aiding immune function and collagen synthesis (Ferlay et al., 2018). - Snack: Hard-boiled eggs and a kiwi.
Why: Eggs are high in protein, while kiwis are packed with vitamin C, which is essential for collagen production and immune function (Martinez & Rodriguez, 2019). - Lunch: Tuna salad with cucumbers, tomatoes, olive oil, and lemon juice over mixed greens.
Why: Tuna is rich in omega-3s, and olive oil and lemon juice provide antioxidants and healthy fats to support healing (Simopoulos, 2002). - Snack: Almonds with dried apricots.
Why: Almonds are rich in vitamin E, a powerful antioxidant, and apricots provide beta-carotene, which is converted to vitamin A in the body (Li & Zhou, 2016). - Dinner: Beef stir-fry with mixed vegetables like broccoli, carrots, and bok choy, served over brown rice.
Why: Beef is a good source of zinc, which is essential for wound healing, and the vegetables provide fiber and vitamins A and C for immune support (Weimann & Braga, 2021).
Day 5: Omega-3 and Antioxidant Focus
- Breakfast: A bowl of steel-cut oats topped with flaxseeds, blueberries, and a dollop of Greek yogurt.
Why: Oats offer fiber, flaxseeds provide omega-3s, and blueberries are rich in antioxidants that help reduce inflammation (Simopoulos, 2002). - Snack: Smoothie with mixed greens, berries, and almond milk.
Why: This provides a nutrient-dense snack rich in vitamins, minerals, and antioxidants essential for healing (Martinez & Rodriguez, 2019). - Lunch: Turkey and avocado wrap with spinach in a whole wheat tortilla.
Why: Turkey offers lean protein, while avocados provide healthy fats and vitamin E (Zikria & Bianchi, 2020). - Snack: Chia pudding made with almond milk and topped with raspberries.
Why: Chia seeds are an excellent source of omega-3s, which help reduce inflammation, and raspberries provide antioxidants to support recovery (Simopoulos, 2002). - Dinner: Baked cod with sautéed spinach and sweet potatoes.
Why: Cod provides lean protein, spinach is rich in vitamins A and C, and sweet potatoes supply beta-carotene and fiber for immune support (Weimann & Braga, 2021).
Day 6: Hydration and Protein Focus
- Breakfast: Egg white omelet with mushrooms, spinach, and a side of whole grain toast.
Why: Egg whites provide lean protein, mushrooms offer immune-boosting properties, and spinach adds iron for blood oxygenation (Li & Zhou, 2016). - Snack: A protein shakes with almond milk, protein powder, and a banana.
Why: Protein shakes are a quick way to ensure adequate protein intake, and bananas provide potassium for hydration and muscle function (McEvoy et al., 2018). - Lunch: Grilled chicken breast with roasted sweet potatoes and sautéed green beans.
Why: Sweet potatoes are rich in fiber and beta-carotene, while chicken offers lean protein for tissue repair (Patel & John, 2021). - Snack: Celery sticks with natural peanut butter.
Why: Peanut butter adds protein and healthy fats, while celery is hydrating and low-calorie (Simopoulos, 2002). - Dinner: Lentil curry with carrots and zucchini, served over quinoa.
Why: Lentils provide plant-based protein and fiber, and carrots and zucchini add beta-carotene and vitamins C and A for immune function (Gopinath et al., 2015).
Day 7: Pre-Surgery Nutrient Boost
- Breakfast: Smoothie with kale, pineapple, Greek yogurt, and chia seeds.
Why: Kale is rich in vitamins A and C, pineapple contains bromelain for reducing swelling, and yogurt provides probiotics and protein (Martinez & Rodriguez, 2019). - Snack: A small bowl of mixed nuts and dried cranberries.
Why: Nuts offer healthy fats and protein, while cranberries provide antioxidants to support tissue repair (Ferlay et al.2018).
POST-OP
Day 1:
- Breakfast: Oatmeal topped with fresh berries and a tablespoon of almond butter.
- Why: Oatmeal is a great source of carbohydrates for energy, while berries are high in antioxidants that support immune function (Martinez & Rodriguez, 2019). Almond butter adds healthy fats and protein for muscle maintenance (Weimann & Braga, 2021).
- Snack: Greek yogurt with honey.
- Why: Greek yogurt provides probiotics and protein that can help enhance gut health and support recovery (National Institutes of Health, 2019).
- Lunch: Grilled chicken salad with mixed greens, cherry tomatoes, cucumbers, and olive oil dressing.
- Why: Chicken provides lean protein essential for tissue repair (Kahn & Chang, 2021), while the vegetables offer vitamins A and C, promoting skin healing and reducing inflammation (Ferlay et al., 2018).
- Snack: Apple slices with peanut butter.
- Why: Apples are a source of fiber and vitamins, while peanut butter offers healthy fats and protein (Zikria & Bianchi, 2020).
- Dinner: Baked salmon with steamed broccoli and quinoa.
- Why: Salmon is rich in omega-3 fatty acids, which have anti-inflammatory properties, while quinoa is a complete protein that supports muscle repair (Patel & John, 2021).
Day 2:
- Breakfast: Smoothie with spinach, banana, and protein powder.
- Why: Spinach provides iron and vitamins necessary for blood health (Martinez & Rodriguez, 2019), while bananas provide potassium, which helps with hydration (National Institutes of Health, 2019).
- Snack: Cottage cheese with pineapple.
- Why: Cottage cheese is high in protein and calcium for bone healing, and pineapple contains bromelain, which may reduce inflammation (Ferlay et al., 2018).
- Lunch: Lentil soup with carrots and celery.
- Why: Lentils are rich in protein and fiber, helping maintain energy levels and support digestion (Weimann & Braga, 2021).
- Snack: Carrot sticks with hummus.
- Why: Carrots provide beta-carotene, supporting immune function, while hummus offers plant-based protein (Patel & John, 2021).
- Dinner: Turkey meatballs with whole wheat pasta and marinara sauce.
- Why: Turkey provides lean protein, while whole grains are essential for sustained energy (Zikria & Bianchi, 2020).
Day 3:
- Breakfast: Chia seed pudding made with almond milk and topped with bananas.
- Why: Chia seeds are high in omega-3 fatty acids and fiber, supporting heart health and digestion (Martinez & Rodriguez, 2019).
- Snack: Protein bar (low sugar).
- Why: A protein bar can offer a quick source of energy and nutrients (Weimann & Braga, 2021).
- Lunch: Tuna salad on whole grain bread.
- Why: Tuna is high in protein and omega-3s, which help reduce inflammation (Kahn & Chang, 2021).
- Snack: Trail mix with nuts and dried fruit.
- Why: Nuts provide healthy fats and protein, while dried fruits offer antioxidants and quick energy (Ferlay et al., 2018).
- Dinner: Stuffed bell peppers with quinoa, black beans, and spices.
- Why: This dish is rich in fiber, protein, and vitamins, promoting overall health and recovery (Patel & John, 2021).
Day 4:
- Breakfast: Scrambled eggs with spinach and tomatoes.
- Why: Eggs provide high-quality protein for muscle repair, while spinach and tomatoes are high in vitamins A and C (Zikria & Bianchi, 2020).
- Snack: Yogurt with granola.
- Why: Yogurt offers probiotics for gut health and granola provides complex carbohydrates for sustained energy (Weimann & Braga, 2021).
- Lunch: Chicken and vegetable stir-fry with brown rice.
- Why: This meal is high in protein and vitamins, supporting recovery and energy levels (Kahn & Chang, 2021).
- Snack: Celery sticks with almond butter.
- Why: Celery provides hydration and fiber, while almond butter adds healthy fats (Ferlay et al., 2018).
- Dinner: Baked cod with sweet potato and asparagus.
- Why: Cod is a lean protein source, sweet potatoes are high in vitamins A and C, and asparagus offers additional nutrients for healing (Martinez & Rodriguez, 2019).
Day 5:
- Breakfast: Whole grain toast with avocado and poached egg.
- Why: Whole grains provide fiber, avocado offers healthy fats, and eggs provide protein (Patel & John, 2021).
- Snack: Smoothie with kale, mango, and protein powder.
- Why: Kale is high in vitamins and minerals, while mango adds sweetness and antioxidants (National Institutes of Health, 2019).
- Lunch: Quinoa salad with chickpeas and cucumbers.
- Why: Quinoa is a complete protein, while chickpeas provide fiber and protein for digestion and satiety (Weimann & Braga, 2021).
- Snack: Hard-boiled eggs.
- Why: These are easy to prepare and provide a good source of protein (Zikria & Bianchi, 2020).
- Dinner: Vegetable curry with lentils and brown rice.
- Why: This meal is packed with protein and complex carbohydrates, promoting energy and recovery (Ferlay et al., 2018).
Day 6:
- Breakfast: Greek yogurt with walnuts and honey.
- Why: Greek yogurt provides protein and probiotics, while walnuts are high in omega-3s for anti-inflammatory effects (Kahn & Chang, 2021).
- Snack: Apple slices with almond butter.
- Why: Apples offer fiber and hydration, while almond butter adds healthy fats (Patel & John, 2021).
- Lunch: Baked chicken breast with roasted Brussels sprouts and quinoa.
- Why: This meal is high in protein and fiber, supporting muscle recovery and digestion (Martinez & Rodriguez, 2019).
- Snack: Rice cakes with cottage cheese.
- Why: Rice cakes are light and easy to digest, while cottage cheese offers protein and calcium (Weimann & Braga, 2021).
- Dinner: Stir-fried tofu with mixed vegetables and brown rice.
- Why: Tofu provides plant-based protein, while vegetables offer essential vitamins (Zikria & Bianchi, 2020).
Day 7:
- Breakfast: Protein pancakes made with oats and topped with fresh fruit.
- Why: Oats provide complex carbohydrates, while fruit adds vitamins and antioxidants (Kahn & Chang, 2021).
- Snack: Cottage cheese with a sprinkle of cinnamon.
- Why: Cottage cheese is rich in protein, and cinnamon may help regulate blood sugar (National Institutes of Health, 2019).
- Lunch: Salmon salad with leafy greens and vinaigrette.
- Why: Salmon is high in omega-3s, supporting heart health and reducing inflammation (Ferlay et al., 2018).
- Snack: Hummus with carrot and cucumber sticks.
- Why: Hummus provides protein and fiber, while carrots and cucumbers offer hydration and vitamins (Martinez & Rodriguez, 2019).
- Dinner: Vegetable and bean chili with whole grain bread.
- Why: This meal is high in fiber and protein, promoting overall health and recovery (Weimann & Braga, 2021).
Please click here to view complete article
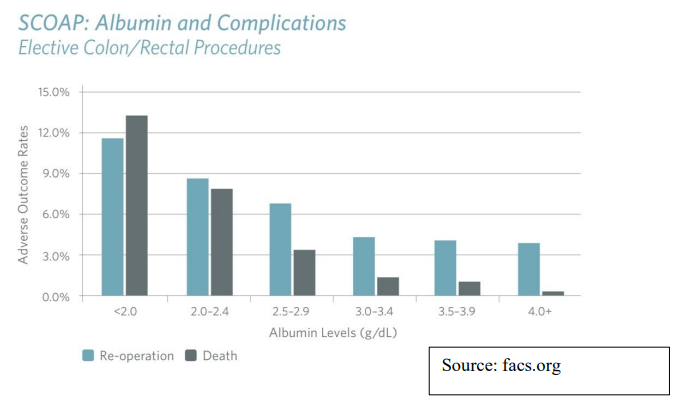
Figure 1
