To Determine the Prevalence of Micro Organisms Responsible for the Vulvovaginitis in Patient Presenting to one of the Tertiary Care Hospital in Riyadh
To Determine the Prevalence of Micro Organisms Responsible for the Vulvovaginitis in Patient Presenting to one of the Tertiary Care Hospital in Riyadh
Dr. Saima Najam*, Dr. Najla El Bizri 1, Dr. Omamma Abuhashim2, Dr. Fauzia Malik3, Samar Mohamed Elshahidy4, Syeda Ifra Hassan5, Dr. Nida Rizwan6
1. Dr. Najla El Bizri, Specialty Diploma In Laboratory Medicine, From The Lebanese University (Beirut, Lebanon) & Université Libre De Bruxelles (Brussels, Belgium), 2016. Clinical Pathology Consultant and Head Of Microbiology & Molecular Department, Dr. Sulaiman Al Habib Hospital Suwaidi.
2. Dr. Omamma Abuhashim, Consultant, Obgyn Department, Dr. Sulaiman Al Habib Hospital, Sweidi, Riyadh, Saudi Arabia.
3. Dr. Fauzia Malik, Consultant, Obgyn Department, Dr. Sulaiman Al Habib Hospital, Sweidi, Riyadh, Saudi Arabia.
4. Samar Mohamed Elshahidy, Laboratory Supervisor,Microbiology Section, Dr. Sulaiman Al Habib Hospital, Sweidi, Riyadh, Saudi Arabia
5. Syeda Ifra Hassan, First Year Mbbs Student, AlMaarefa College Of Science And Technology, Riyadh, Saudi Arabia
6. Dr. Nida Rizwan, Medical Officer, Jshq, Mrc, Rawalpindi, Pakistan
*Correspondence to: Dr. Saima Najam, FCPS, PG Certification in Medical Education ( Dundee), Consultant, Obgyn Department, Dr. Sulaiman Al Habib Hospital, Sweidi, Riyadh, Saudi Arabia.
Copyright
© 2025 Dr. Saima Najam. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 14 January 2025
Published: 22 January 2025
DOI: https://doi.org/10.5281/zenodo.14715878
Abstract
Alteration of the vaginal flora leads to the growth of the microorganisms.
Objective: The objective of the study was to determine the most common organism responsible for the vulvovaginitis in our population of the patient.
Material and methods: We have conducted a retrospective study to see the most common infection in the non-pregnant Cohort of the symptomatic patients .We have excluded the pre pubertal and menopausal women and the women for whom the swab was also taken for gram staining for bacterial vaginosis. The data was then analyzed through the version 30 of the SPSS.
Results: The total number of the high vaginal swabs which were taken in symptomatic patients during the study period were 4055 out of which 41.67% (n=1690) of the swabs were positive for one organism and in 1.3% (n=22) more than one organism was found. Fifty percent of our study population (n= 851) belonged to the age group between 18-28 years and 41.3%(n= 697) belonged to the age bracket of 28.1-38 years. Regarding the parity 87.9% of the study population was para 3 or less (n=1487), and only 12% (n=203) of the population was para 4 and above. The total number of positive swabs were 1690, and out of 1690 positive HVS swabs,70.7% (n=1211) were positive for candida albicans and in 18.5%(n=318) non albicans species were found. While other organisms were found in 10.6 %(n=183). The most common organism at the young age group i.e. less than 38 years is the candida albicans and non albicans species.
Most of the vaginal infections 88%%(n=1487) were found in the patients with parity 3 or below and in 94.1%(n=1140) of these patients the organism was candida albicans. The relationship of the parity with the vaginitis is significant as after applying the Chi square test , the p value was found to be 0.001. Among the other organisms Strep Agalactae and E- Coli lead the list.
Conclusion: Candida albicans and the non albicans were the most common infections found in all age groups. We emphasize the importance of integrating the diagnostic tools for the proper diagnosis of the causative organism to improve the diagnosis and management instead of going for the empirical treatment of the patients presenting with the vaginitis.
Key words: vulvitis, vaginitis, vulvovaginitis, candidiasis, non albicans candidiasis.
To Determine the Prevalence of Micro Organisms Responsible for the Vulvovaginitis in Patient Presenting to one of the Tertiary Care Hospital in Riyadh
Introduction
The vaginal flora which prevents the growth of the pathogenic microorganisms and are considered as the primary defense mechanism of the reproductive function, includes several aerobic, non-aerobic and facultative bacteria. So once the vaginal flora is altered it will lead to the proliferation of the other microorganisms and will lead to vulvovaginitis.1 The entry of microorganisms into the female genital tract is effected by different physical, behaviors i.e. sexual activity, number of sexual partners, and physiological factors like phase of the menstrual cycle, immunity, age and the anatomical location of the female genital tract.2 Vulvovaginitis is the most common genitourinary complaint encountered in the gynecological clinic, this happens when the vaginal microbiota is replaced by the other microorganisms and is associated with the inflammatory process, if there is no evidence of the inflammation it will be known as vaginosis.3 Almost three fourths of women have experienced VV(vulvo-vaginitis) at least once in their lifetime.4 Rodrigues et al found Gardinella vaginalis, candida species and trichomonas vaginalis as the most common causative agents.5 We have done this study to determine the most prevalent infection in our population cohort of the non-pregnant women. Candida species leading to VV is the second most common infection after BV which is affecting the genital tract of millions of the females worldwide and poses a significant medical challenge. 6 It is characterized by the cheesy vaginal discharge associated with itching and burning sensation. 70% of the females will have at least one episode of the candidal vulvovaginitis during their lifetime.7
This fungal infection is attributed to yeast species of Candida genus, with Candida(C) albicans being the most prevalent compared to C. glabrata, C. tropicalis, C. parapsilosis and other non-C. albicans species. 8 Notable is the fact that C. albicans are our commensal and inhabit the skin and gastrointestinal, reproductive and urinary tracts, but they display virulence attributes when opportunities arise, particularly in individuals with compromised immune systems.9 Other factors which can trigger the yeast infection in addition to the compromised immunity are antibiotics, pregnancy, diabetes etc.10
We have planned this study to see the prevalence of the organisms found in our population.
Material and Methods
We have collected the data retrospectively form the database of the hospital from first September 2023 till 30th September 2024, meeting our inclusion and exclusion criteria. We have taken the data of the positive high vaginal swabs only, for bacterial vaginosis a separate swab for Nugent score was requested and for the purpose of the study we have excluded those patients. All non-pregnant ,symptomatic, pre-menopausal, women were included. The prepubertal and the menopausal women were excluded as well.
The data was then entered in the SPSS version 30. T test was applied to the quantitative data and chi-square test was applied to the qualitative data. The p-value of less than 0.05 is accepted as level of significance.
Results
The total number of the high vaginal swabs which were taken in symptomatic patients during the study period were 4055 out of which 41.67% (n=1690) swabs were positive for one organism and in 1.3% (n=22) more than one organism was found. Fifty percent of our study population (n= 851) belonged to the age group between 18-28 years and 41.3%(n= 697) belonged to the age bracket of 28.1-38 years, as shown in graph 1.
GRAPH:1 AGE DISTRIBUTION AMONG THE STUDY POPULATION
Regarding the parity 87.9% of the study population was para 3 or less (n=1487), and only 12% (n=203) of the population was para 4 and above. The relationship of parity with different age groups is shown in table 1.
|
Age in years |
Parity less than 3 |
Parity more than 4 |
Total |
|
18-28 |
55.6 % (n=828) |
11.3%(n=23) |
50.3% (n=851) |
|
28.1-38 |
40.0% (n=596) |
49.7%(n=101) |
41.2%(n=697) |
|
38.1-48 |
03.9% (n=59) |
32.0%(n=65) |
7.3% (n=124) |
|
48.1 and above |
0.26% (n=04) |
06.8% (n=14) |
1.06% (n=18) |
|
Total |
100% (n=1487) |
100% (n=203) |
100% (n=1690) |
TABLE:1 DEMOGRAPHICS OF THE STUDY POPULATION
The total number of positive swabs were 1690, and out of 1690 positive HVS swabs 70.7% (n=1211) were positive for candida albicans and in 18.5%(n=318) non albicans species were found. While other organisms were found in 10.6 %(n=183) as shown in graph 2.
Graph 2 : PREVALENCE OF THE ORGANISMS IN HVS
The most common organism at the young age group i.e. less than 38 years is the candida albicans and non albicans species as depicted in graph 3 below.
The relationship is significant as the p value is 0.001 after applying the chi-square test.
Graph:3 RELATIONSHIP OF AGE WITH MOST COMMON ORGANISMS
Most of the vaginal infections 88%%(n=1487) were found in the patients with parity 3 or below and in 94.1%(n=1140) of these patients the organism was candida albicans, as shown in table 2. The relationship of the parity with the vaginitis is significant as after applying the Chi square test , the p value was found to be 0.001.
|
Parity |
Candida albicans |
Candida non albicans |
others |
Total |
|
Less than 3 |
94.1%(n=1140) |
63.8%(n=203) |
89.5%(n=144) |
88.0%(n=1487) |
|
4 or more |
5.86%(n=71) |
36.2%(n=115) |
10.5% (n=17) |
12.0%(n=203) |
|
Total |
100% (n=1211) |
100% (n=318) |
100 %(n=161) |
100% (n=1690) |
Table:2 Relationship of the parity with the most common organisms
Among the other organisms Strep Agalactae and E- Coli lead the list ,as shown in the graph 2.
Graph 4: PREVALENCE OF THE OTHER ORGANISMS.
Discussion
Candida species are the most common cause of the mycological infections in the world and are the third most common cause of the health-related infections.11Candida Albicans is the most common species in the humans however the significant increase in the NAC has been noticed in the last 20 years. 12 The factors which are found to contribute are severe immuno-compression, prematurity, empirical use of broad-spectrum antibiotics and anti-mycotic drugs. The clinical presentation of all the candidal infections is almost the same but several NAC acquire resistant or inherently are resistant to the commonly used antifungal drugs.13
In the pre-menopausal women, the vagina is colonized in at least 20% of the females with the candidal species, which increases to 30% in late pregnancy and in immunocompromised women. different host factors like local defense mechanisms, gene polymorphisms, allergies, serum glucose levels, antibiotics, psycho-social stress and estrogens influence the risk of candidal vulvovaginitis (VVC).The NAC is responsible for almost 10% of the candidal vulvovaginitis. The symptoms usually are milder than the albicans infection and include premenstrual itching, burning, redness and odorless discharge. 14 which is lower than what we found in the current study. As most of the females will experience at least one episode of the VVC in their lifetime. It is very important to realize that the symptoms alone are not enough to diagnose the VVC. The treatment should be given in confirmed cases and specially in patients having recurrent and complicated infections the diagnosis should always be confirmed by the fungal culture with species identification. However the women with asymptomatic colonization and an asymptomatic sexual partner should not be treated.15
The vulvovaginitis is an intractable issue of the females due to its symptoms like discharges, pain and pruritis.16. It was found to be the common infection in the prepubertal and adolescent females.17 However for the purpose of the study we have excluded that age group.
Our data suggested that typical physical findings appeared infrequently among women with these infections and their empirical treatments were frequently inappropriate. Our findings were supported by the results of the study done by Huang, 2023.18
We found the candida species as the commonest organism in the premenopausal women as their vaginal epithelium is estrogenized, the similar association was found by Sheppard, 19 who concluded that the post-menopausal woman would have fungal infection only if they are taking hormone replacement therapy.
Strengths of the study:
It will act as a base line to see the increase in the albicans and non albicans infections in future. It included a good number of symptomatic patients.
Limitations of the study:
As it was a retrospective study, so the risk factors like presence of the co morbidities ( diabetes, etc. ) use of antibiotics, use of contraceptive pills etc. cannot be ruled out.
Conclusion
We emphasize the importance of integrating the diagnostic tools for the proper diagnosis of the causative organism to improve the diagnosis and management instead of going for the empirical treatment of the patients presenting with the vaginitis. It was found to be more prevalent in the younger age group (18-38 years ) Candida albicans and the non albicans were the most common infections found in all age groups.
In future a prospective study is recommended.
Acknowledgements:
The authors hereby acknowledge the support of the staff nurses, Miss Jonalyn Pacliwan, Miss Abigail Lazo and Miss Risma Azifa Zahraa for their contribution in retrieving the data.
Financial disclosure: NA
Conflict of interest: NA
References
1. Pereira EBC, Carvalho CN, Neto APMC,de Omena ACS, Magalhaes PKA, Cavalcanti MGS, et al. Microorganisms causing vulvovaginitis: analysis of 1688cervicovaginal cytology. Brazil J of Bio,2023;83.
2. Oliveira, JAG. and Carneiro CM, 2020. Fatores associados a alterações da microbiota no trato genital feminino inferior. Pensar Acadêmico .2020;18(2):289-299.
3. Linhares IM, Amaral RL, Robial R and Eleutério Junior J. Vaginites e vaginoses.Femina, 2019;47(4):235-40.
4. Agana MG, Riyali B, Patel DR. Vulvo vaginitis in adolescents. PM, 2019;2:53
5. Rodrigues HJC, Silva HFM, Pereira IS, Castro GJB, Silva SAM, Araujo EA, etal. Prevalence of vulvovaginite in women rural. Research social development. 2022;11(3),
6. Martins N, Ferreira I, Barros L, Silva S, Henriques M. Candidiasis: predisposing factors, prevention, diagnosis and alternative treatment Natália Martins. Mycopathologia. 2014;177(5–6):223–40.
7. Cruz GS, Brito EHS de, Freitas LV, Monteiro FPM. Candidíase vulvovaginal na Atenção Primária à Saúde: diagnóstico e tratamento. Rev. Enferm. Atual. 2020 ;94(32):e-020074.
8. Dabas PS. An approach to etiology, diagnosis and management of different types of candidiasis. J Yeast Fungal Res. 2013;4(6):63–74.
9. Alonso-Monge R, Gresnigt MS, Román E, Hube B, Pla J. Candida albicans colonization of the gastrointestinal tract: A double-edged sword. PLoS Pathog. 2021;17(7),1-6.
10. Soliman AS, Mohammed, B El M, Hasheesh MAl, Abdelhady IHT. Incidence of Causative Organisms of Vaginitis in Females with Intrauterine Device," Al-Azhar International Medical Journal:2024; 5(5) :Article 17.
11. Cortegiani A, Misseri G, Chowdhary A. Whats new on emerging resis tant candida species. Intensive care med , 2019;456(4):512-5.
12. Badiee P, Alborzi A, Shakiba E, Ziyaeyan M, Rasuli M. Molecular identification and in vitro susceptibility of Candida albicans and C. dubliniensis isolated from immunocompromised patients. Iran Red Crescent Med J. 2009;11(4):391–7.
13. Sullivan D. J., Henman M. C., Moran G. P., O'Neill L. C., Bennett D. E., Shanley D. B., Coleman D. C. Molecular genetic approaches to identification, epidemiology and taxonomy of non-albicans Candida species. Journal of Medical Microbiology. 1996;44(6):399–408.
14. Mendling W, Brasch J, Cornely OA, Effendy I, Friese K, Ginter-Hanselmayer G, etal. . Guideline: vulvovaginal candidosis (AWMF 015/072), S2k (excluding chronic mucocutaneous candidosis). Mycoses. 2015;58(5):324.
15. Farr A, Effendy I, Frey Tirri B, Hof H, Mayser P, Petricevic L, etal. Guideline: Vulvovaginal candidosis (AWMF 015/072, level S2k). Mycoses. 2021 ;64(6):583-602.
16. Picheta N, Piekarz J, Burdan O, Satora M, Tarkowski R, Ku,?k K. Phytotherapy of Vulvovaginal Candidiasis: A Narrative Review. Int J Mol Sci. 2024;28;25(7):3796.
17. Zuckerman A, Romano M. Clinical Recommendation: Vulvovaginitis. J Pediatr Adolesc Gynecol.2016;29:673-9.
18. .Huang, SH, Hsu HC, Lee T F, Fan H M, Tseng, CW, Chen IH, et al. Prevalence, Associated Factors, and Appropriateness of Empirical Treatment of Trichomoniasis, Bacterial Vaginosis, and Vulvovaginal Candidiasis among Women with Vaginitis. Microbiology spectrum, 2023;11(3): e0016123.
19. .Sheppard C. Treatment of vulvovaginitis. Australian prescriber, 2020;43(6):195–9.
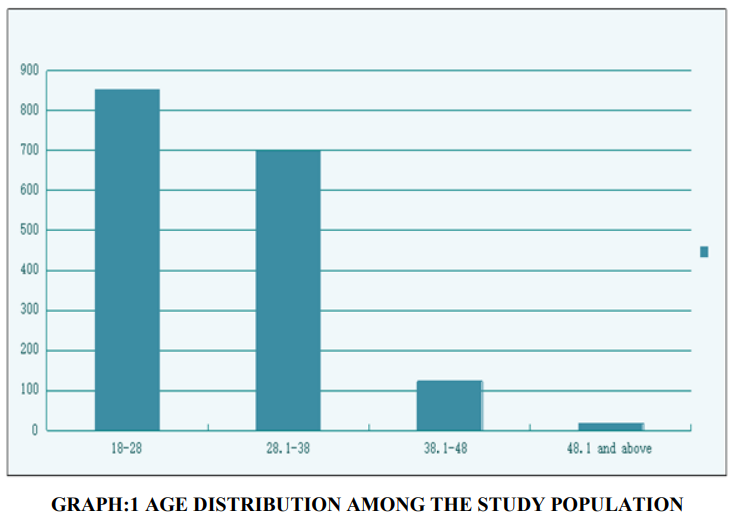
Figure 1
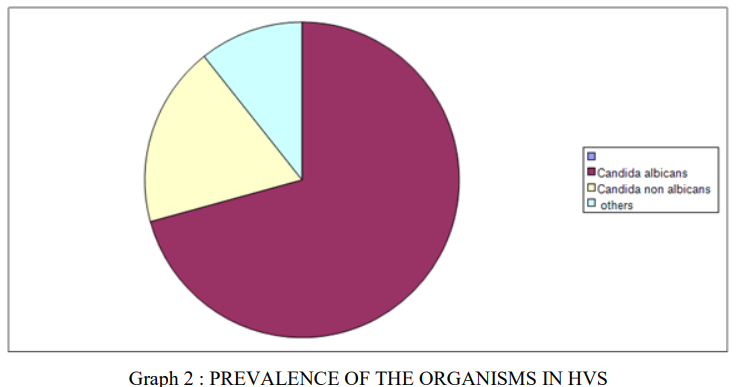
Figure 2
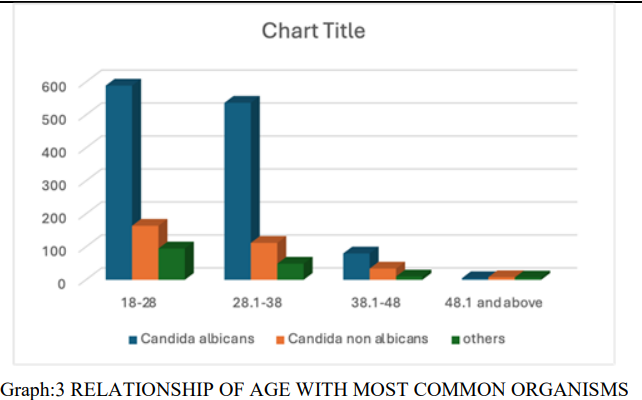
Figure 3
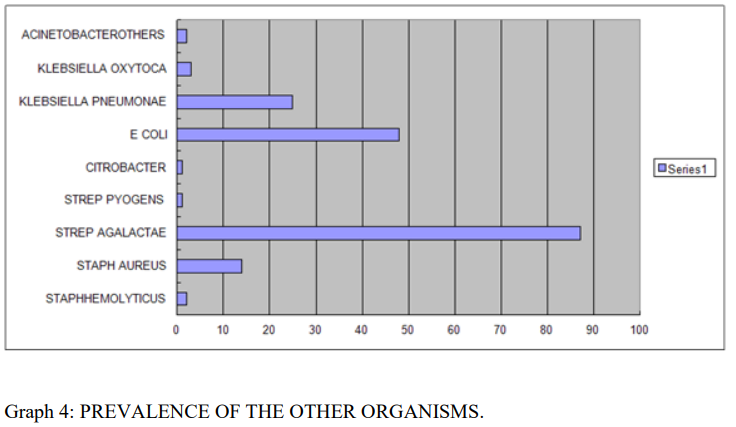
Figure 4
