Non Pharmacological Treatment of Pain in Temporomandibular Disorders (Muscular, Arthritic).
Non Pharmacological Treatment of Pain in Temporomandibular Disorders (Muscular, Arthritic).
Karadimitriou Maria-Despoina1*, Athanasoulis Christos2, Kagioglou Nikoleta3, Kalogeris Iasonas4
1: Dentist,Faculty of Dentistry,School of Health Sciences Aristotle University of Thessaloniki, Postgraduate student at MSc” Dental & Craniofacial Bioengineering and Applied Biomaterials”, Department of Prosthodontics, School of Health Sciences, Aristotle University of Thessaloniki
2,3:Dentist, Faculty of Dentistry,School of Health Sciences Aristotle University of Thessaloniki
4:Dentist, Faculty of Dentistry,School of Health Sciences Aristotle University of Thessaloniki, Postgraduate student at MSc "Research Methodology in Medicine and Health Sciences"
*Correspondence to: Karadimitriou Maria-Despoina, BDS (MIDA), PGDCC, PGDMT, PGDND.
Copyright.
© 2025 Karadimitriou Maria-Despoina. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 17 Jan 2025
Published: 22 Jan 2025
DOI:https://doi.org/10.5281/zenodo.15779247
ABSTRACT:
The temporomandibular joint is defined as an amphi-condylar joint formed by the mandibular head, the temporal glenoid and the intervertebral disc1. The craniomandibular disorders (CMD) or temporomandibular disorders (TMD) is an umbrella term for all fuctional disorders of the masticatory system, including temporomandibular joint syndrome, myofascial pain-dysfunction syndrome, and temporomandibular pain-dysfunction syndrome2. The purpose of this study is to examine the non pharmacological treatment methods and, according to the available literature, evaluate them. Methods were seperated in two categories: the biomedical ones and the biopsychological and biosocial ones
Non Pharmacological Treatment of Pain in Temporomandibular Disorders (Muscular, Arthritic).
Figure 1. Temporomandibular joint anatomy: GF-glenoid fossa; C-mandibular condyle; D-articular disc; RT-retrodiscal tissue; LPM-lateral pterygoid muscle3.
Introduction
Factors contributing to the complexity of craniomaxillary disorders are related to dentition, clenching and other related systems, which often cause symptoms of muscle, joint and periarticular pain4. The disorders are typically categorized into three main clinical syndromes, which include the presumed etiology as well as signs and symptoms in the muscles of mastication and associated hard and soft tissues. These consist of:
1) Musculoskeletal pain disorders,
2) Internal joint disorders, and
3) Degenerative joint diseases, such as osteoarthritis or arthralgia. It is important to emphasize that it is very common for people with temporomandibular disorders to be diagnosed with more than one of the three main
syndromes5. Another broad classification is based on the Research Diagnostic Criteria (RDC) for temporomandibular disorder. This is a biobehavioral model of pain that includes two main axes: that of physical signs and symptoms (axis I) and that of psychological factors and dysfunction (axis II)4.
The prevalence of pain due to temporomandibular disorders in the adult population is estimated to be between 3.7% and 12%, while the numbers vary between men and women, with the latter being 1 to 5 times more frequently affected5,4. As for their costs, a conservative estimate in the US has been $400 per year for health care visits and $2 billion or more per year for their treatment5.
Disorders in the temporomandibular joint have a negative effect on functional processes, such as chewing, speaking and normal occlusion and also in areas such as social life, psychology and productivity at work. For all the above mentioned reasons, science focused on the diagnosis, prevention and treatment of all of these states. The treatment pathways were divided into two treatment groups; the one that includes the conservative and reversible approaches, which include medication, physical, behavioral and other interventional methods LLT6,7, TNS6,7, low and medium molecular weight intra-articular injection ΗΑ in synovial fluid8, prefabricated oral splints9, acupuncture10, tDCS11,65) and in that of irreversible approaches, such as surgical procedures and occlusal changes5.
The purpose of this study is to review the available recent literature to: a) determine the effectiveness of non-pharmacological methods of treating the pain of craniomaxillary disorders, b) assess their necessity as therapeutic means and c) compare them, in the cases that were available in the literature.
Methods and Materials:
For this bibliographic report, the international literature was searched. The electronic bases searched are: PubMed, European Journal of Medical Research, Cochrane Library, Google Scholar, Springer Link, The Free Dictionary by Farlex, ResearchGate, Wiley Online Library and Taylor & Francis Online.
Keywords (some are “tmd”, “cmd”, “pain arthritic”, “pain myofascial”, “pain management”, “tmj”, “non pharmacological treatment”) were used in the complex search of electronic databases, both alone, as well as in combination with the logical operators AND and NOT(logical operator OR was not used). Also, in the bases where this possibility was given (e.g. PubMed), the articles suggested as relevant to those searched for, were evaluated.
The searches were initially aimed at more general results and were gradually specialized in terms of the subject of interest. In addition, before analyzing non-pharmacological approaches, pharmaceutical ones were also examined to have a more complete view.
Articles from the latest 24 years and not earlier were preferred to keep the review data as up-to-date as possible. Those selected as useful and reliable were stored and their essentials tabulated in chronological order. Finally, handwritten notes were taken throughout.
Results
a. Biomedical methods:
The review and study of the literature led to the collection of results for the evaluation of non-pharmacological ways of dealing with temporomandibular disorders. Some surgical procedures were studied in the research of Guo et al12. There, arthrocentesis was compared with arthroscopy. Regarding their effect on pain, no significant difference between them was highlighted, while no data were reported on quality of life. Mild and transient adverse reactions, such as discomfort or pain at the injection site, were present as adverse effects in both groups. However, in maximal mouth opening, arthroscopy had statistical superiority(-5,28).
Fonseca et al8 aimed to evaluate the quality of life after intra-articular injection of low and medium molecular weight hyaluronic acid (HA) into the synovial fluid. Based on its four-month clinical use in both joint and temporomandibular disorders, they found that in the original sample, at the time of diagnosis: a) of the patients with muscle disorders (group 1), 50% experienced myofascial pain, b) of the patients with disc displacement (group 2), 90% of patients were diagnosed with displacement with reduction c) of the patients with other common conditions (group 3), 10% had arthralgia at rest of the mandible and 20% were diagnosed with joint inflammation or degeneration. During the first 6 months of treatment: a) no patient was diagnosed with musculoskeletal pain, b) no changes were observed, except from one patient, c) a patient with arthralgia showed no symptoms and one of those previously diagnosed with inflammation was diagnosed with degeneration. Pain-free mouth opening improved in the first month compared to baseline. Craniomaxillary dysfunction and pain intensity decreased significantly within six months, as did McGill pain scores. On image analysis, assessment of osteoarthritic changes by CBCT showed a significant reduction in the presence of osteophytes, flattening, hardening and erosion of the mandibular head, while MRI showed a change in disc position and shape.
Regarding the choice of Transcutaneous Electrical Nerve Stimulation (TENS) and Low Level Laser Therapy (LLLT) in patients to whom medication has not been effective, Rezazadeh et al6 concluded that there was a decrease in VAS and Helkimo indices in both groups. There was no significant difference between the two methods during treatment, although TENS was more effective in reducing pain afterwards. Núñez et al7, in a related study, found an improvement in range of motion, with values obtained after LLLT being significantly higher than those obtained after TENS. The work of Gil-Martínez et al4 also demonstrated the beneficial effects of TENS and LLLT of different frequency and intensity on pain relief
High-Definition transcranial Direct Current Stimulation (HD-tDCS), according to Donnell et al32, produced significant improvements in clinical pain and mandibular mobility measures, compared to placebo results. These are: a) at 4 weeks of follow-up, pain relief -according to VAS- in more than 50% of chronic patients with CGD disorders, b) at 1 week, pain-free opening of the mouth and c) limitation of the area and intensity of segmental pain. No emotional changes occurred between the two groups. A similar reduction in pain thresholds and improvement in quality of life was also demonstrated by Oliveira et al11. In the comparison with exercise series application, the expected results were not shown, as the absolute increase in benefit was +0.375 for tDCS, compared to the +2.66 which was expected to demonstrate its superiority.
A wide range of researchers reported on the effect of oral and occlusal splints. In the analysis of Gomes al13 with a closure splint, significant increases in range of motion were found in all movements. A small to moderate clinical effect was found for left and right side slips relative
to the massage therapy and asymptomatic comparison groups. Giannakopoulos et al9, in agreement with the previous ones, report that overall there was a statistically significant increase in pain-free maximal contraction. Furthermore, they concluded that, after 2 weeks of using three types of splints, the overall mean current pain was reduced by 41.95%. For the prefabricated oral splints with elastic water-filled cushions group (A), the pain reduction was 37.88%, for the vacuum formed copolymer splints group (B) 66.6%, and for the with Michigan type hard splints (C) 22.29%. The last measured pain level for group (B) was significantly lower than that of group (C).
The work of Weggen et al14 shows the therapeutic effects of splints of different clinical complexity to vary between patient groups, with complex oral appliances being superior, while significant but temporary pain relief was achieved with the addition of TENS. The course of symptom improvement was not paralleled for the non-chronic treated patients, with significant changes appearing in the EMG data. The shift to lower frequencies of maximal evoked power differed significantly between healthy subjects and patients. Finally, Gil-Martínez et al4 report that the phenomenon of reduction in electromyographic activity of the muscles of mastication does not last more than 2 weeks and suggest the placement of occlusive splints to prevent the denture from trismus damage. Correlation between dentoskeletal characteristics and craniomaxillary disorders in children and adolescents - orthodontic patients, investigated by Di Venere et al15. They found that of the 128 examined patients, 15 showed signs and/or symptoms of craniomaxillary disorders (11.7%). Furthermore, in patients with these disorders, features of skeletal hyperexcitability were often identified. In comparison, in 15 patients who did not suffer from CMD, no statistically significant differences were detected, either in their skeletal or occlusal characteristics.
Gil-Martínez et al4 report the use of dry needling to treat local and referred pain produced by myofascial trigger points and that this led to a reduction and improvements in mandibular function in patients with myofascial temporomandibular disorder. Its effects, in fact, are comparable to those achieved by injecting trigger points with lidocaine and corticosteroids. They concluded that acupuncture is a good therapeutic modality for short-term pain relief in patients with myofascial temporomandibular disorder, but not in those cases in which there is limitation of mandibular movement. In the application of acupuncture, οι Simma et al10 come to disagree and note that pain reduction measured by VAS was significantly more pronounced after acupuncture than after placebo treatment. Finally, they report that acupuncture reduced the sum of pain in 14 muscles more significantly compared to sham laser treatment.
Physiotherapy has a positive impact on relieving pain, reducing inflammation and restoring motor function, according to Gil-Martínez et al4. They then focus on its subcategories. In manual therapy, with joint mobilization techniques and soft tissue intervention (i.e. in the cervical spine and the cervix, where it is most effective), causing relief through neurophysiological mechanisms. In therapeutic exercise (stretching, tongue relaxation, masticatory relaxation, coordination exercises), with less beneficial effects, focused on improving mobility control and masticatory muscle strength. The exercises showed a favorable increase in mobility and range, but no improvement in the strength of the cervical spine stabilizer muscles. They report that the combined intervention of manual therapy and exercise, with the adoption of an active role of the patient, is effective in alleviating symptoms, further enhancing the effects of the two previous interventions.The combination of manual therapy with exercise in patients with temporomandibular disorders also had its potential in the research of Furto et al16, since patients who undergo a rehabilitation program with or without iontophoresis with dexamethasone show clinically significant improvements in dysfunction and overall perceived change in a relatively short time period of time. Occlusal
splint therapy and physiotherapy combined together significantly affect: the vertical and sagittal position of the mandible(fig.6), as well as the width of functional space between C1 and C2(fig.7) as the study of Marcin Derwich et al underlines17.
On the other hand, Michelotti et al18, studied the effect of learning exercises at home and noted that the actual evidence for their effectiveness is weak and there is a need for further investigation. The reason is the very limited number of randomized clinical trials (RCTs) available in the literature. The treatment of Nicolakis et al19 included active and passive jaw movement exercises, posture correction and relaxation techniques. As a result of the treatment, pain, weakness and mouth stiffness improved significantly more than during the control period (where the exercises were not performed). After treatment, four patients had no pain at all and only seven patients revealed reduced incisal clearance. At follow-up, seven patients had no pain and no side effects. Along the same lines as the previous study, Carlson et al20 investigated the effectiveness of physical self-regulation (PSR) exercises, a skills training program for managing chronic facial muscle pain, mainly through breathing, relaxation, posture and proprioceptive retraining. The results showed that pain intensity decreased in both groups, while mouth opening improved.
Figure 2. Effect of time(horizontal axis-months) on mean values of mouth opening(vertical axis-mm) in both groups(soft and hard splints) throughout study intervals21.
Figure 3. Effect of time(horizontal axis-months) on mean values of pain scores(vertical axis-VAS(visual analog scale for rating pain) scores) in both groups(soft & hard splints) throughout the study intervals21.
Figure 4. Effect of time(horizontal axis-months) on mean values of joint tenderness(vertical axis-Severe=3, Moderate=2, Absent=1) in both groups(soft and hard splints) throughout the study intervals21.
Figure 5. Clinical trial of transcutaneous electrical nerve stimulation (TENS) for pain relief in masticatory muscles. (a) The TENS device ESPURGE (ITO CO., LTD, Tokyo, Japan) is used because it is a portable device and easy to use at the chairside. (b) Four electrodes are applied to the skin for 20 min at a phase duration of 50 μs with frequencies of 100–200 Hz (sweep modulation mode)22.
Figure 6.Lateral cephalogram with marked points, lines, and angles used to assess vertical and sagittal position of the mandible. A—point A; ANB—angle between lines NA and NB; B—point B; Gn—gnathion; FO plane—functional occlusal plane; ML—mandibular line; N—nasion; NL—nasal line; NL/ML—angle between lines: NL and ML17
Figure 7. Lateral cephalogram with marked points, lines, and angles used to assess head position, cervical vertebrae, and functional spaces. AP—anteroposterior; CV angle—craniovertebral angle; MGP—McGregor’s Plane; NS—nasion-sella line; C0—basiocciput; C1—C3; C5—first, second, third, fifth cervical vertebrae17.
b. Biopsychosocial Methods:
A prominent role in this category is muscle relaxation therapy combined with electromyographic (EMG) feedback. Five of the 6 controlled studies of Crider & Glaros23, found this to be superior to non-therapeutic or psychological placebo controls. Clinical test results were significantly greater for EMG feedback treatments than in control conditions (after a meta-analysis of 12 studies). 69% of patients who received EMG feedback therapy were rated as asymptomatic or significantly improved, compared to 35% of placebo-treated patients who experienced various side effects. Results at follow-up showed no deterioration from levels immediately after treatment. Reinforcing this, the findings of Sherman & Turk5 showed that almost twice as many patients who received EMG feedback shCrider & Glarosowed improvement compared to those who received no treatment or received placebo (68.6% vs. 34.7%). The positive effects were maintained at follow-up 3 to 24 months after the end of treatment.
The effect of EMG feedback in a group of subjects co-administered with cognitive behavioral therapy (CBTCrider & Glaros), in one co-administered with therapeutic exercises, and in a no-treatment control group produced pain reduction and improvement in mood states, in contrast to no treatment was applied (Sherman & Turk5 ). Furthermore, in the study by Mishra et al24, patients in the EMG feedback group with concurrent CBST were more significantly improved compared to the no treatment group.
The broader group of biobehavioral methods of approaching patients with disorders in the CGD also includes the diagnostic testing of mental health and the way it interacts with the appearance of joint problems. In this way, Yeung et al25 showed that, of those suffering from GD disorders, 17% were diagnosed with possible major depressive disorder, 20% with anxiety disorder, while 1% faced a high risk of suicide or self-harm. They thus proved that the early recognition of mental health problems and the simultaneous implementation of a mental and physical correction program can help in the holistic treatment of patients with temporomandibular disorder. Also, Augusto et al26 recorded that the prevalence of temporomandibular disorders in a sample of university students was 71.9% and was distributed as follows: the mildest form of disorder concerned 50.0%, moderate 16.4% and severe 5.5%, as they were also more frequent in women (76.4%). Common mental disorders were present in 29.9% of participants, thus demonstrating the existence of an association.
Gil-Martínez et al4 emphasize that cognitive behavioral therapy (CBT) - by managing patients' thoughts, behaviors and/or emotions that may worsen pain symptoms - is non-invasive, without side effects and as good as complementary, when it focuses on the psychological characteristics of the patient. The work of Glaros27 reports that patients with certain forms of CGD disorder show very high levels of parafunctional anxiety, due to increased stress levels. Lack of awareness of these behaviors may result from uncertain definitions of the term "tightness," from a proprioceptive deficit, or from the presence of complementary behaviors. Current data suggest that reducing tooth contact through habit reversal techniques may be a promising mechanism for reducing pain in these patients. Finally, education and self-management strategies based on the various types of temporomandibular disorders and psychosocial impairments hold promise, especially when grounded in neuroscience. This approach has been shown, according to Gil-Martínez et al4, to reduce pain, dysfunction and psychological factors in chronic musculoskeletal disorders, both alone and in combination with other techniques.
Carlson28, evaluating the role of biobehavioral problems in the onset and maintenance of orofacial pain, found that for positive results in the chronic management of orofacial pain, a multidimensional approach to treatment, rather than just psychological treatment, is often required because of the complexity of malfunctions. Furthermore, biobehavioral therapy could have a beneficial effect in the treatment of temporomandibular disorders, due to the apparently high existence of psychological problems in patients with such manifestations, as argued by Orlando et al29.
The correlation of eating habits and CKD problems was studied by two different groups of scientists. A model of modification of the eating behavior of rats, related to the inflammation and loss of function of their temporomandibular joint was the object of study by Thut et al30. The dependent variable in the model was the time between food rewards, or the intervening interval (IFI). Inflammation of the CG muscle, or masseter, showed significant dose- and magnitude-dependent increases in food reward in the intervention interval (IFI). Inflammation of the skin overlying the joint had no association with IFI. Preadministration of indomethacin reversed the inflammation-induced shift of IFI. An inflammation-induced increase in IFI was associated with an increase in feeding time. The study of Souza et al31 reports that there was a higher prevalence of masticatory myofascial pain, as well as pain in other parts of the body, in patients with eating disorders, compared to healthy controls. However, there was no difference between subgroups (restrictive anorexia, purging anorexia, bulimia).
Discussion
a. Biomedical methods:
The study elaborated on a variety of non-pharmacological approaches to the treatment of temporomandibular disorders and assessed their effectiveness. Surgical interventions, such as arthroscopy and arthrocentesis, appear to be effective, however, according to Guo et al12, there is still insufficient evidence for this. Therefore, if it is not internal degeneration of the jaw or something equally serious, there is no reason to resort to them and less invasive treatments are preferred, such as those we will analyze next.
The injection of low and medium molecular weight hyaluronic acid (HA) into the synovial fluid was examined by Fonseca et al8, who observed a reduction in pain intensity, improvement in mouth opening range and quality of life. The results were even more pleasing because it is a particularly economical solution, however the available literature is not yet sufficient to be absolutely sure.
Transcutaneous electrical nerve stimulation (TENS) and low-level laser therapy (LLLT) were two methods that were compared several times. LLLT was found by Núñez et al7 to be more effective in improving mouth opening. Also, Rezazadeh et al1 concluded that both modalities were effective in treating myalgia when used in drug-resistant disorders, with TENS being slightly better, especially for immediate effects. However, Gil-Martínez et al4, while agreeing that LLLT improves mandibular range of motion, concluded that neither method has better results in treating the disorders than their placebo counterparts.
The results of using transcranial direct current stimulation (tDCS) are controversial. Donnell et al32 found that the application of high-frequency tDCS (HD-tDCS) to the primary motor cortex of the brain (M1) of chronic patients had excellent results both in reducing myofascial pain and improving mobility. In contrast, Oliveira et al11 added tDCS to exercises and observed no additional benefit, other than small, transient improvements.
As far as the use of splints is concerned, in the literature, this exists mainly as an adjunct along with other means of dealing with disorders. Gomes et al13 report the improvement of closure splints in mouth opening and sideslips. In reducing pain, splints have visible but short-term results, either in the context of an orthopedic stabilization treatment4, or in parallel with the use of counseling therapy9 or TENS14.
The results of acupuncture are also controversial. Simma et al10 report that acupuncture can provide pain relief that placebo drugs cannot, and therefore provides an opportunity to initiate other therapeutic agents. Gil-Martínez et al4, while agreeing to offer temporary relief, found no advantage over placebo treatments involving skin puncture.
A very broad part of the literature deals with physical therapy, both as such and its techniques separately. The reason is its very high efficiency combined with the low cost, which together with the splints make it, according to Sherman & Turk5, one of the most indicative treatments for temporomandibular disorders. Carlson et al20 studied the effects of PSR exercises and found them to be particularly positive in improving mouth opening and reducing pain, both in the short and long term. Manual therapy offers relief from orofacial pain4, while local massage in particular, according to Gomes et al13, also contributes to opening the mouth.
Therapeutic exercise was also found to be effective in improving opening and relieving pain, by Nicolakis et al19. However, its benefit is not considered better than other methods, such as closure splints, TENS and acupuncture4. Michelotti et al18 looked at teaching patients exercises that they can do alone at home. The method was considered promising, however the literature is insufficient to draw clear conclusions. The combination of two physical therapy methods: manual therapy and exercises also has remarkable effects. Research by Furto et al16 showed an immediate improvement in dysfunction after the combination of methods, which basically focuses on mobility control and reduction of muscle pain4.
In conclusion, regarding physical therapy, we can keep the conclusion of Gil-Martínez et al4, that it is a method with satisfactory results in relieving pain, reducing inflammation and restoring motor function.
b. Biopsychosocial methods:
Biopsychosocial (or biobehavioral) methods have gained the most attention in the last decade, which according to Stowell et al33 is due to the presence of countless researches, which show promising results in pain reduction combined with very low costs. Thus, treatments are beginning to diverge from biomedical methods, which in the past were considered a panacea.
One of the most widespread methods is muscle relaxation combined with electromyographic (EMG) feedback, where the patient, seeing the reactions of his facial muscles on the EMG, learns how to move them without pain. Crider & Glaros23 and Sherman & Turk5 demonstrated the excellent effectiveness of this method. In fact, Mishra et al32 reported that it is more effective than cognitive behavioral therapy methods.
Cognitive behavioral therapy (CBT) is non-invasive, without side effects and excellent as an adjunct, according to Sherman & Turk5, when it focuses on the patient's psychological characteristics. In particular, self-management training (CBST) states that it is of major importance for the patient's understanding of the disorder and, by extension, its easier treatment. Gil-Martínez et al4 report that it is a more effective method than closure splints, but lags behind manual therapy and therapeutic exercise. Its simultaneous use with other methods is suggested, such as, according to Mishra et al32, EMG feedback.
Glaros27, focused on patients with parafunctional emotions, mainly the result of an anxiety disorder, and highlighted the importance of habit reversal techniques to improve temporomandibular disorders in these patients. At the same time, something that we can distinguish from his research and Augusto et al26 come to confirm us, is the direct correlation of stress with disorders, especially in women. Thus, the study by Yeung et al25 regarding the IMPARTS system, which manages to distinguish the existence of mental problems and contributes to the monitoring of the patient during treatment, is considered even more important. The research satisfactorily proved that the system is essential in diagnosing the cause of temporomandibular disorder and consequently in its subsequent treatment.
Regarding the association between food intake and worsening of temporomandibular pain, research by Thut et al30 in rats showed that greater frequency of food consumption worsened muscle inflammation and pain. However, we cannot link bulimia with TMDs, because Souza et al31 found that all eating disorders, including anorexia, cause the same unwanted results. Therefore, although it is possible, an association between eating and temporomandibular disorders is not yet proven.
In conclusion, the complexity of craniomaxillary disorders requires, according to Carlson28, the inclusion of biobehavioral methods in the treatment to be followed. Orlando et al29 as well as Sherman & Turk5 conclude that they are absolutely necessary and, if we take into account the conclusions regarding the individual methods, we would have to agree.The attending dentist is asked to decide between the available methods individually, depending on the patient in front of him. The only general conclusion that can be drawn is that the complexity and chronicity of craniomaxillary disorders requires a combination of biomedical and biopsychosocial methods for their treatment, without any of the two broad categories being less important than the other.
References
1. The free dictionary by Farlex. [Internet] Miller-Keane Encyclopedia and Dictionary of Medicine, Nursing, and Allied Health, Seventh Edition. (2003) [cited 2019 May 25] Available from: https://medical-dictionary.thefreedictionary.com/temporomandibular+joint
2. The free dictionary by Farlex. [Internet] Medical Dictionary for the Dental Professions. (2012) [cited 2019 May 28] Available from:
https://medical-dictionary.thefreedictionary.com/temporomandibular+disorder
3. Daniel Talmaceanu, Lavinia Manuela Lenghel, Nicolae Bolog, Mihaela Hedesiu, Smaranda Buduru, Horatiu Rotar, Mijaela Baciut and Grigore Baciut. Imaging modalities for temporomandibular joint disorders: an update. Clujul Med. 2018 Jul; 91(3): 280–287. Published online 2018 Jul 31. doi: 10.15386/cjmed-970
4. Alfonso Gil-Martínez, Alba Paris-Alemany, Ibai López-de-Uralde-Villanueva, Roy La Touche. Management of pain in patients with temporomandibular disorder (TMD): challenges and solutions. Journal of Pain Research. 2018; 11: 571–587. doi: 10.2147/JPR.S127950
5. Jeffrey J. Sherman, Dennis C. Turk. Nonpharmacologic approaches to the management of myofascial temporomandibular disorders. Current Pain and Headache Reports. 2001, Volume 5, Issue 5, pp 421–431. doi: 10.1007/s11916-001-0053-7
6. Rezazadeh F, Hajian Κ, Shahidi S, Piroozi S. Comparison of the Effects of Transcutaneous Electrical Nerve Stimulation and Low-Level Laser Therapy on Drug-Resistant Temporomandibular Disorders. Journal of Dentistry. 2017 Sep; 18(3): 187–192.
7. Núñez SC, Garcez AS, Suzuki SS, Ribeiro MS. Management of mouth opening in patients with temporomandibular disorders through low-level laser therapy and transcutaneous electrical neural stimulation. Photomedicine and laser surgery. 2006 Feb;24(1):45-49. doi: 10.1089/pho.2006.24.45
8. Fonseca RMDFB, Januzzi E, Ferreira LA, Grossmann E, Carvalho ACP, de Oliveira PG, Vieira ÉLM, Teixeira AL, Almeida-Leite CM. Effectiveness of Sequential Viscosupplementation in Temporomandibular Joint Internal Derangements and Symptomatology: A Case Series. Pain Research & Management. 2018; 2018: 5392538. doi: 10.1155/2018/5392538
9. Giannakopoulos NN, Katsikogianni EN, Hellmann D, Eberhard L, Leckel M, Schindler HJ, Schmitter M. Comparison of three different options for immediate treatment of painful temporomandibular disorders: a randomized, controlled pilot trial. Acta odontologica Scandinavica. 2016 Aug; 74(6): 480-486. doi: 10.1080/00016357.2016.1204558
10. Simma I, Gleditsch JM, Simma L, Piehslinger E. Immediate effects of microsystem acupuncture in patients with oromyofacial pain and craniomandibular disorders (CMD): a double-blind, placebo-controlled trial. British Dental Journal. 2009 Dec 19; 207(12): E26. doi: 10.1038/sj.bdj.2009.959
11. Oliveira LB, Lopes TS, Soares C, Maluf R, Goes BT, Sá KN, Baptista AF. Transcranial direct current stimulation and exercises for treatment of chronic temporomandibular disorders: a blind randomised-controlled trial. Journal of oral rehabilitation. 2015 Oct; 42(10): 723-732. doi: 10.1111/joor.12300
12. Guo C, Shi Z, Revington P. Arthrocentesis and lavage for treating temporomandibular joint disorders. The Cochrane Database of Systematic Reviews. 2009 Oct 7;(4):CD004973. doi: 10.1002/14651858.CD004973.pub2
13. Gomes CA, Politti F, Andrade DV, de Sousa DF, Herpich CM, Dibai-Filho AV, Gonzalez Tde O, Biasotto-Gonzalez DA. Effects of massage therapy and occlusal splint therapy on mandibular range of motion in individuals with temporomandibular disorder: a randomized clinical trial. Journal of manipulative and physiological therapeutics. 2014 Mar-Apr; 37(3): 164-169. doi: 10.1016/j.jmpt.2013.12.007
14. Weggen T, Schindler HJ, Kordass B, Hugger A. Clinical and electromyographic
follow-up of myofascial pain patients treated with two types of oral splint: a randomized controlled pilot study. International journal of computerized dentistry. 2013; 16(3): 209-224.
15. Di Venere D, Gaudio RM, Laforgia A, Stefanachi G, Tafuri S, Pettini F, Silvestre F, Petruzzi M, Corsalini M. Correlation between dento-skeletal characteristics and craniomandibular disorders in growing children and adolescent orthodontic patients: retrospective case-control study. Oral and Implantology (Rome). 2016 Nov 16; 9(4): 175-184. doi: 10.11138/orl/2016.9.4.175
16. Eric S. Furto, Joshua A. Cleland, Julie M. Whitman, Kenneth A. Olson. Manual Physical Therapy Interventions and Exercise for Patients with Temporomandibular Disorders. The Journal of Craniomandibular & Sleep Practice. 2006; 24(4): 283-291. doi: 10.1179/crn.2006.044
17. Marcin Derwich, Lawrence Gottesman, Karolina Urbanska and Elzbieta Pawlowska. Craniovertebral and Craniomandibular Changes in Patients with Temporomandibular Joint Disorders after Physiotherapy Combined with Occlusal Splint Therapy: A Prospective Case Control Study.Medicina (Kaunas). 2022 May; 58(5): 684.Published online 2022 May 21. doi: 10.3390/medicina58050684
18. Michelotti A, de Wijer A, Steenks M, Farella M. Home-exercise regimes for the management of non-specific temporomandibular disorders. Journal of Oral Rehabilitation. 2005 Nov; 32(11): 779-785. doi: 10.1111/j.1365-2842.2005.01513.x
19. Nicolakis P, Erdogmus B, Kopf A, Ebenbichler G, Kollmitzer J, Piehslinger E,
Fialka-Moser V. Effectiveness of exercise therapy in patients with internal derangement of the temporomandibular joint. Journal of Oral Rehabilitation. 2001 Dec; 28(12): 1158-1164.
20. Carlson CR, Bertrand PM, Ehrlich AD, Maxwell AW, Burton RG. Physical
self-regulation training for the management of temporomandibular disorders. Journal of orofacial pain. 2001 Winter;15(1):47-55.
21. Sameh A Seifeldina,b and Khaled A. Elhayesb. Soft versus hard occlusal splint therapy in the management of temporomandibular disorders (TMDs). National Library of Medicine.2015 Jun 25. doi: 10.1016/j.sdentj.2014.12.004
22. Susumu Abe, Akane Miyagi, Kaoru Yoshinaga, Yoshizo Matsuka, Fumihiro Matsumoto, Emi Uyama, Yoshitaka Suzuki, Masamitsu Oshima, Kazuo Okura, Eiji Tanaka. Immediate Effect of Masticatory Muscle Activity with Transcutaneous Electrical Nerve Stimulation in Muscle Pain of Temporomandibular Disorders Patients. J Clin Med. 2020 Oct 16;9(10):3330. doi: 10.3390/jcm9103330
23. Crider AB, Glaros AG. A meta-analysis of EMG biofeedback treatment of temporomandibular disorders. Journal of orofacial pain. 1999 Winter ;13(1): 29-37.
24. Mishra KD, Gatchel RJ, Gardea MA. The relative efficacy of three
cognitive-behavioral treatment approaches to temporomandibular disorders. Journal of Behavioral Medicine. 2000 Jun; 23(3): 293-309.
25. Yeung E, Abou-Foul A, Matcham F, Poate T, Fan K. Integration of mental health screening in the management of patients with temporomandibular disorders. The British Journal of Oral and Maxillofacial Surgery. 2017 Jul; 55(6): 594-599. doi: 10.1016/j.bjoms.2017.03.014
26. Viviane Gontijo Augusto, Keity Cristina Bueno Perina, Daniel Silva Gontijo Penha, Daiane Carolina Alves dos Santos, Valéria Aparecida Souza Oliveira. Temporomandibular dysfunction, stress and common mental disorder in university students. Acta Ortopedica Brasileira. 2016 Nov-Dec; 24(6): 330–333. doi: 10.1590/1413-785220162406162873
27. Glaros AG. Temporomandibular disorders and facial pain: a psychophysiological perspective. Applied Psychophysiology and Biofeedback. 2008 Sep; 33(3): 161-171. doi: 10.1007/s10484-008-9059-9
28. Carlson CR. Psychological considerations for chronic orofacial pain. Oral and Maxillofacial Surgery Clinics of North America. 2008 May; 20(2): 185-195. doi: 10.1016/j.coms.2007.12.002
29. Orlando B, Manfredini D, Salvetti G, Bosco M. Evaluation of the effectiveness of biobehavioral therapy in the treatment of temporomandibular disorders: a literature review. Behavioral Medicine. 2007 Fall; 33(3): 101-118. doi: 10.3200/BMED.33.3.101-118
30. Thut PD, Hermanstyne TO, Flake NM, Gold MS. An operant conditioning model to assess changes in feeding behavior associated with temporomandibular joint inflammation in the rat. Journal of orofacial pain. 2007 Winter; 21(1): 7-18.
31. de Souza, Antequerdds, Aratangy, de Siqueira SRD, Cordás, JT de Siqueira. Pain and temporomandibular disorders in patients with eating disorders. Brazilian Oral Research. 2018; 32:e51. doi: 10.1590/1807-3107bor-2018.vol32.0051
32. Adam Donnell, Thiago Nascimento, Mara Lawrence, Vikas Gupta, Tina Zieba, Dennis Q. Truong, Marom Bikson, Abhi Datta, Emily Bellile, Alexandre F. DaSilva. High-Definition and Non-Invasive Brain Modulation of Pain and Motor Dysfunction in Chronic TMD. Brain Stimulation. 2015 Nov-Dec; 8(6): 1085–1092. doi: 10.1016/j.brs.2015.06.008
33. Stowell AW, Gatchel RJ, Wildenstein L. Cost-effectiveness of treatments for temporomandibular disorders: biopsychosocial intervention versus treatment as usual. Journal of the American Dental Association. 2007 Feb; 138(2): 202-208. doi: 10.14219/jada.archive.2007.0137
34. Ghurye S, McMillan R. Pain-Related Temporomandibular Disorder - Current Perspectives and Evidence-Based Management. Dental Update. 2015 Jul-Aug; 42(6): 533-536, 539-542, 545-546. doi: 10.12968/denu.2015.42.6.53
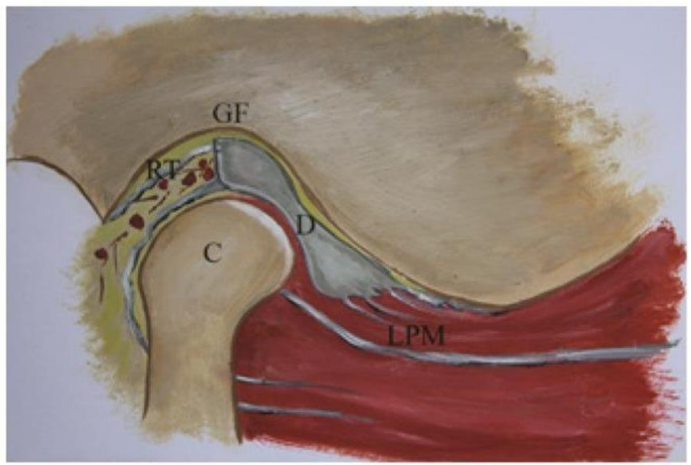
Figure 1
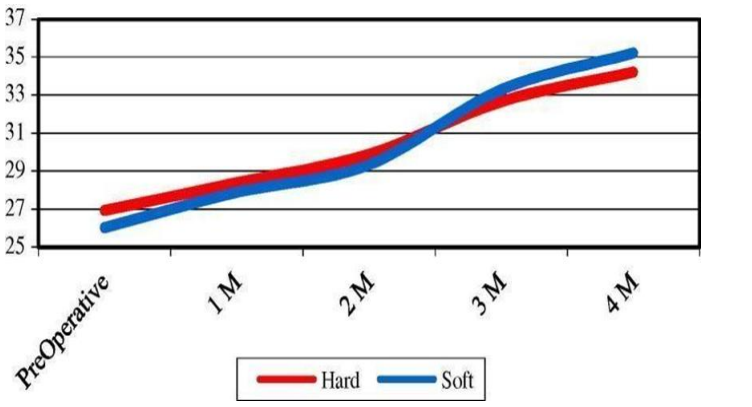
Figure 2
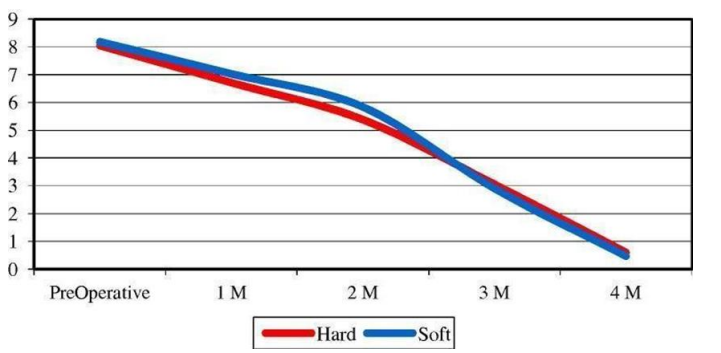
Figure 3
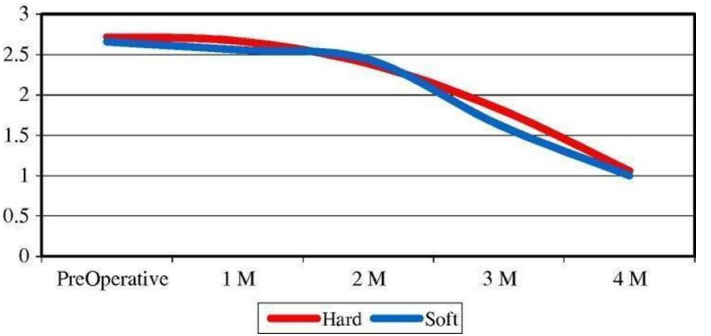
Figure 4
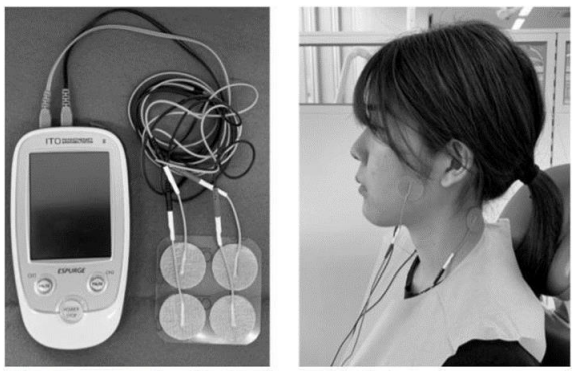
Figure 5
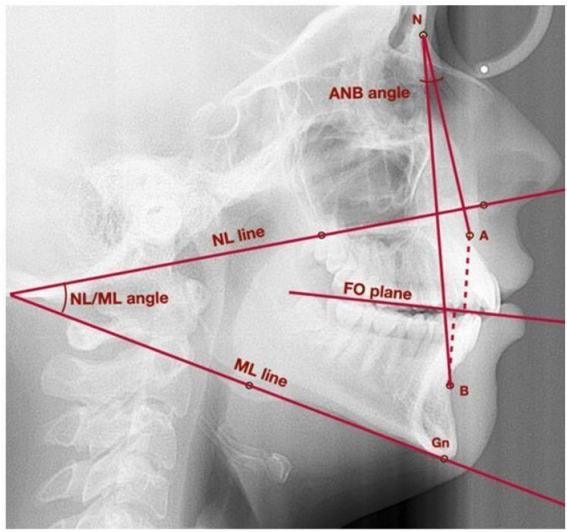
Figure 6
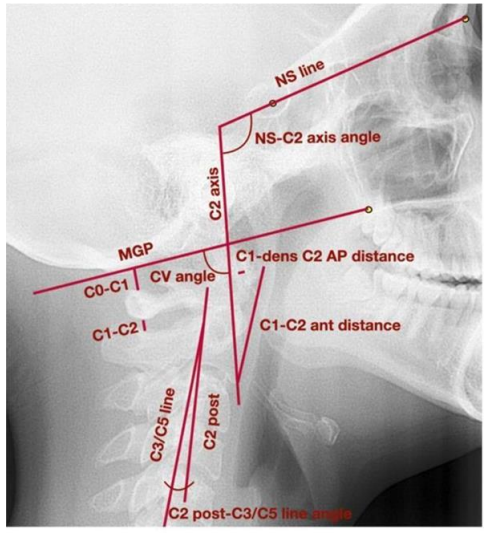
Figure 7
