Acute Cor Pulmonale as the First Presentation of Adenocarcinoma Lung: A Case Series
Acute Cor Pulmonale as the First Presentation of Adenocarcinoma Lung: A Case Series
Dr Muniza Bai*1, Dr Archana Mallick2, Dr Dharm Prakash Dwivedi3, Dr Debasis Gochhait4
1. Junior Resident, Department of Pulmonary Medicine, Jawaharlal Institute of Postgraduate Medical Education and Research(JIPMER),Puducherry,India-605006.
2. Senior Resident, Department of Pulmonary Medicine, Jawaharlal Institute of Postgraduate Medical Education and Research(JIPMER),Puducherry,India-605006.
3. Additional Professor, Department of Pulmonary Medicine, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Puducherry, India-605006
4. Additional Professor, Department of Pathology, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Puducherry, India-605006
Correspondence to: Dr Archana Mallick, Department of Pulmonary Medicine, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER),Puducherry, India-605006
Copyright
© 2024 Dr Archana Mallick. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 24 Jan 2025
Published: 03 Feb 2025
DOI: https://doi.org/10.5281/zenodo.15043568
ABSTRACT
Malignancy is a well-known risk factor for venous thromboembolism. However, when a patient with no known cancer presents with an acute pulmonary embolism, the possibility of an underlying malignancy as an inciting agent is often unexplored. There have been reports of increasing number of cases where lung malignancy is being diagnosed within a year or two after an event of idiopathic or unprovoked thrombosis. Once malignancy and pulmonary embolism happen to be in the same page, treatment gets challenging, hospital stay increases and prognosis worsens. We experienced two such cases where pulmonary embolism was the initial presentation of an occult lung malignancy. We herein share our experience and review the literature for possible pathogenesis.
KEYWORDS: lung, pulmonary embolism, venous thromboembolism, adenocarcinoma.
Acute Cor Pulmonale as the First Presentation of Adenocarcinoma Lung: A Case Series
Introduction
Venous thromboembolism (VTE) compromises of deep vein thrombosis (DVT) and pulmonary embolism (PE), which are common complications in the course of tumour progression and antitumor treatment. Cancer patients who develop VTE have shortened survival time compared to those who do not develop VTE. Approximately 25% of the patients who present with VTE have cancer.[1] However, about 10% of patients presenting with unprovoked or idiopathic thrombosis have a malignancy diagnosed within the next 1 to 2 years.1 Herein, we describe details of a patient in whom pulmonary embolism was the principal manifestation of an underlying lung malignancy.
Case Details
CASE 1
A 40 year non smoker female with no known comorbidities who had complaints of dry cough for 10 days, and breathlessness for 1 month, presented to us with sudden onset worsening of breathlessness. Her heart rate was 150bpm, blood pressure 80/60mmHg, Sp02 75% and respiratory rate 30/min. ECG showed sinus tachycardia. Chest radiograph was suggestive of left massive pleural effusion. Diagnostic and therapeutic pleural tapping was done, but breathlessness persisted. Her blood investigations showed elevated D-dimer levels. We then performed computed tomography pulmonary angiography (CTPA) which showed filling defect in right distal main pulmonary artery extending into right upper lobar and inter lobar artery (Figure 1A). Bilateral peribronchovascular consolidation, predominantly in left upper lobe, left paraesophageal nodal mass and left moderate pleural effusion was also noted (Figure 1B). In addition to the respiratory and hemodynamic support, she was thrombolysed with intravenous streptokinase (250 000 IU as a loading dose over 30 min, followed by 100 000 IU/h over 24 h), after ruling out any contraindications to thrombolysis. She was continued on therapeutic anticoagulation. Pleural fluid cytological and cell block evaluation was suggestive of adenocarcinoma primary lung and was negative for EGFR, ALK and ROS1 (Figure 2). Her whole-body positron emission tomography (PET) and contrast enhanced magnetic resonance imaging (CE-MRI) brain did not show any additional foci of metastasis. A diagnosis of stage IVA adenocarcinoma lung was made. She was started on chemotherapy and was duly discharged on non-vitamin K antagonist oral anticoagulants (NOACs).
Figure 1 A. CTPA showing filling defect in right distal main pulmonary artery extending into right upper lobar and inter lobar artery.
B. Lung window showing bilateral peribronchovascular consolidation, predominantly in left upper lobe, and left moderate pleural effusion.
Figure 2.A&B. Hematoxylin and Eosin stained image (high power) from the cell block section shows the scattered small clusters of large tumor cells with abundant cytoplasm, pleomorphic nuclei and prominent nucleoli. C. Immunohistochemistry for TTF 1 antibody (400X) shows tumor cells with strong nuclear positivity (arrow) indicating it to be lung origin. D1 and D2. Immunohistochemistry for Napsin A antibody shows cytoplasmic positivity in the tumor cells (arrow) confirming the primary as lung adenocarcinoma.
Case 2
A 47 year male, chronic smoker presented with complaints of acute onset breathlessness, chest pain, palpitations and giddiness. He is a known diabetic on regular medication. He has no prior history of cardiovascular disease. At the time of presentation, he was conscious oriented but tachypneic. His heart rate was 140bpm, blood pressure 80/50mmHg, room air saturation 88% and respiratory rate 36/min. Electrocardiogram showed sinus tachycardia, no ST-T changes. Bedside echocardiography showed RA RV dilation, RV dysfunction, moderate TR and adequate LV function. PE was suspected and features of CTPA done were consistent with pulmonary embolism involving bilateral branch pulmonary arteries, extending into lobar and segmental branches (Figure 3A, B). A well-defined mass was noted in left lower lobe with adjacent pleural based nodules (Figure 3C). Bilateral diffuse parenchymal tumor nodules, bilateral minimal pleural effusion, and mediastinal lymphadenopathy were seen. Reperfusion therapy for acute PE with intravenous streptokinase (250 000 IU as a loading dose over 30 min, followed by 100 000 IU/h over 24 h) was administered after ruling out contraindications to thrombolysis in addition to the initial respiratory and hemodynamic support. He achieved symptomatic relief gradually. He was continued on therapeutic anticoagulation. Pleural fluid cytology and cell block was suggestive of adenocarcinoma, primary lung, negative for driver mutations EGFR, ALK and ROS1. PET CT and CE-MRI brain did not show any additional metastatic foci. A diagnosis of stage IVA adenocarcinoma lung was made. He was started on chemotherapy and continued on oral anticoagulants. He is on regular follow up and is symptomatically better.
Figure 3. A,B. CTPA showing filling defects in distal part of bilateral main pulmonary arteries (arrow). C. Left lower lobe mass is seen with adjacent pleural nodules.
Discussion
In 1868, Trosseau first elucidated the relationship between venous thromboembolism and cancer.[2] The reported incidence of VTE in cancer patients ranges from 4 to 20%.[3] Lung cancer being the most commonly diagnosed cancer and the leading cause of cancer death in males since 2008, is the commonest cancer associated with venous thromboembolism. Other cancers include that of the colon, breast and prostate. PE complicating cancer is the second most common cause of death after tumour progression in cancer patients, amounting to 10% of deaths.[4] It is also associated with treatment challenges, reduced quality of life, and decreased survival time. However, early anticoagulation therapy decreases the mortality rate four-fold when compared to patients who do not receive early anticoagulation.[5] Hence early diagnosis and prompt management of PE in the backdrop of lung cancer is imperative for better and improved survival rates.
PE commonly presents as breathlessness, chest pain, syncope or hemoptysis. Misdiagnosis or missed diagnosis is commonly experienced as the clinical presentation of PE and lung cancer masquerade each other.[6] Nevertheless, unexplained PE can be the first signal from an occult lung cancer, as in our case. Often, pulmonary embolism is incidentally diagnosed on a routine radiographic examination done for diagnostic purpose or follow up of lung cancer. This entity is referred to as unsuspected PE (UPE) and it commonly involves segmental arteries. Suspected PE frequently involves main pulmonary or lobar arteries.
Increased propensity for the development of venous thromboembolism in a setting of lung cancer is multifactorial and involves a complex interaction between tumor, host and antitumor treatment. In the mid-nineteenth century, Rudolf Virchow brought the concept of ‘thrombosis’, ‘embolism’ and Virchow’s triad, which holds good in stratifying elements of risk and understanding the pathogenesis of VTE in lung cancer, one hundred and fifty years later too. The risk factors for VTE in lung cancer can be broadly classified as tumour related, host related and treatment related factors.[7] Malignancy as a hypercoagulable state is well known. It occurs due to the ability of tumour cells to activate the coagulation system and this imbalance between procoagulant and anticoagulant factors triggers VTE in lung cancer. Tissue factor, the begetter of the coagulation pathway is over expressed in lung cancer milieu.[7]
Tumor related risk factors mainly comprises of histological subtype, cancer stage, driver mutations, and time since diagnosis of lung cancer. Adenocarcinoma cells secrete mucin which activates platelets and other procoagulant factors, thereby increasing the chances of developing PE.[8] Advanced stages (stages 3 and 4) of lung cancer are associated with decreased clotting time and increased plasminogen activator inhibitor (PAI-1) levels, therefore at a higher risk of developing PE than early stages of lung cancer.[7] Also, EML4/ALK rearrangements result in increased tyrosine kinase expression that in turn augments tissue factor procoagulant activity. It is associated with a 2-fold higher risk of PE, while EGFR or KRAS mutations are not associated with PE.[9] Studies have shown that the initial 6 months of diagnosis of lung cancer is associated with the highest incidence of PE and the risk plummets thereafter.10 Also, tumor cells can promote the prothrombotic state by vessel wall injury by direct invasion or direct adhesion.
Patient related characteristics posing risk for PE are varied ranging from female sex, prolonged immobilisation, comorbid illness to hematologic parameters. The presence of comorbid illnesses including anemia (haemoglobin less than 10g/dL), obesity (BMI≥30), chronic obstructive pulmonary disease and pre-existing DVT increases the risk of PE, whereas diabetes mellitus, systemic hypertension, cardiovascular diseases and smoking are not predisposing factors.[7] Hematologic parameters associated with increased likelihood of PE are haemoglobin ≥ 14g/dL, leucocytosis, elevated D-dimer levels, PaO2 < 80mmHg and raised carcinoembryonic antigen levels.[8]
Patients who have received systemic chemotherapy have a 5.35 fold risk of developing PE compared to those who did not receive.[8] Chemotherapy has a prothrombotic effect by causing tissue factor mediated activation of coagulation system on one hand and downregulation of anticoagulant levels and fibrinolytic activity on the other hand. Targeted chemotherapy also contributes by increasing the expression of PAIs.
Multidetector CTPA is the imaging of choice to detect PE as it allows adequate visualization of the pulmonary vessels down to the subsegmental level.[11]. As our patients had hemodynamically unstable definite PE with no contraindications to thrombolysis, we treated them with systemic thrombolytic therapy followed by therapeutic anticoagulation. They were switched to NOACs for an indefinite period or until cancer cure is achieved.[11]
Conclusion
Pulmonary embolism can be the first inkling of an underlying malignancy. Occult malignancy should be kept in mind while treating idiopathic or unprovoked VTE. Early detection and immediate management is crucial for better prognosis of PE complicating lung cancer.
Conflict of Interests: None
Funding: None
Acknowledgement: The authors are grateful to all our residents for helping with patient care.
References
1. Lee AYY, Levine MN. Venous thromboembolism and cancer: risks and outcomes. Circulation. 2003 Jun 17;107(23 Suppl 1):I17-21.
2. Trousseau A. Phlegmasia Alba Dolens: Lectures on Clinical Medicine. London, England: The New Sydenham Society; 1868:5:281-331
3. Heit JA, Silverstein MD, Mohr DN, Petterson TM, O’Fallon WM and Melton LJ 3rd. Risk fac-tors for deep vein thrombosis and pulmonary embolism: a population-based case-control study. Arch Intern Med 2000; 160: 809-815.
4. Nichols L, Saunders R, Knollmann FD. Causes of Death of Patients With Lung Cancer. Archives of Pathology & Laboratory Medicine. 2012 Dec;136(12):1552–7.
5. Sun JM, Kim TS, Lee J, Park YH, Ahn JS, Kim H, et al. Unsuspected pulmonary emboli in lung cancer patients: the impact on survival and the significance of anticoagulation therapy. Lung Cancer. 2010; 69:330–336.
6. Ai P. Clinical analysis of risk factors and prognosis of lung cancer complicated with pulmonary embolism.Journal of Huaihai Medicine. 2017; 35: 49–51.
7. Li Y, Shang Y, Wang W, Ning S, Chen H. Lung Cancer and Pulmonary Embolism: What Is the Relationship? A Review. J Cancer. 2018;9(17):3046–57.
8. Hua X, Han S-H, Wei S-Z, Wu Y, Sha J, Zhu X-L. Clinical features of pulmonary embolism in patients with lung cancer: A meta-analysis. Katoh M, editor. PLoS ONE. 2019 Sep 30;14(9):e0223230.
9. Verso M, Chiari R, Mosca S, Franco L, Fischer M, Paglialunga L, et al. Incidence of Ct scan-detected pulmonary embolism in patients with oncogene-addicted, advanced lung adenocarcinoma. Thromb Res. 2015 Nov;136(5):924–7.
10. van Herk-Sukel MPP, Shantakumar S, Penning-van Beest FJA, Kamphuisen PW, Majoor CJ, Overbeek LIH, et al. Pulmonary embolism, myocardial infarction, and ischemic stroke in lung cancer patients: results from a longitudinal study. Lung. 2013 Oct;191(5):501–9.
11. Konstantinides SV, Torbicki A, Agnelli G, Danchin N, Fitzmaurice D, Galiè N, et al. 2014 ESC guidelines on the diagnosis and management of acute pulmonary embolism. Eur Heart J. 2014 Nov 14;35(43):3033–69, 3069a–3069k.
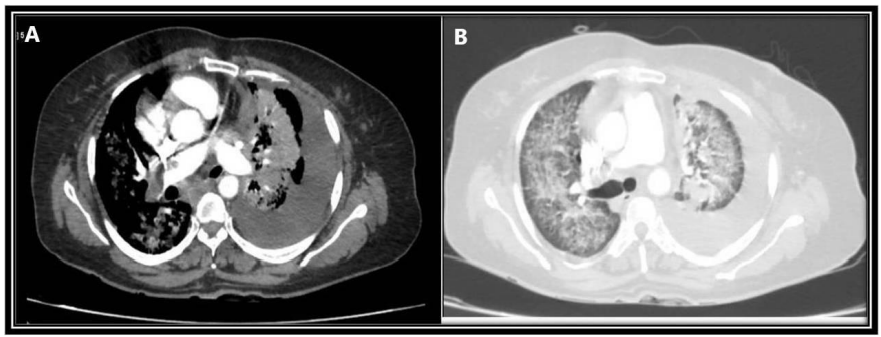
Figure 1
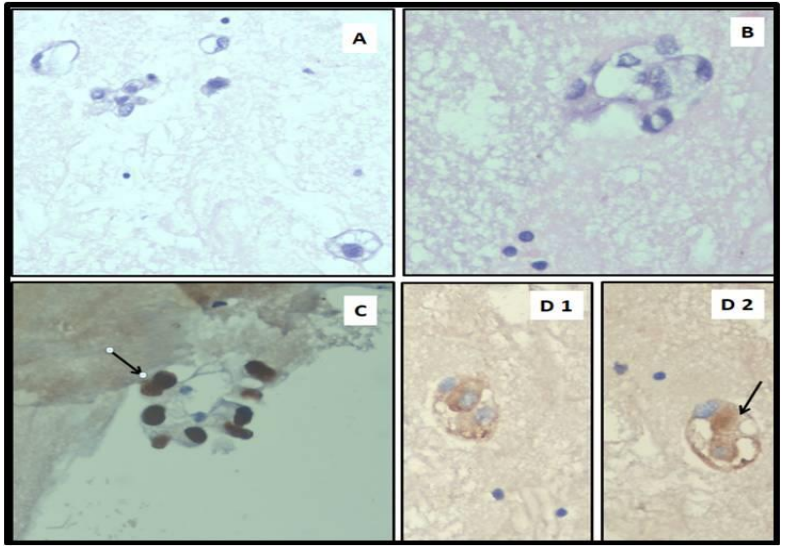
Figure 2
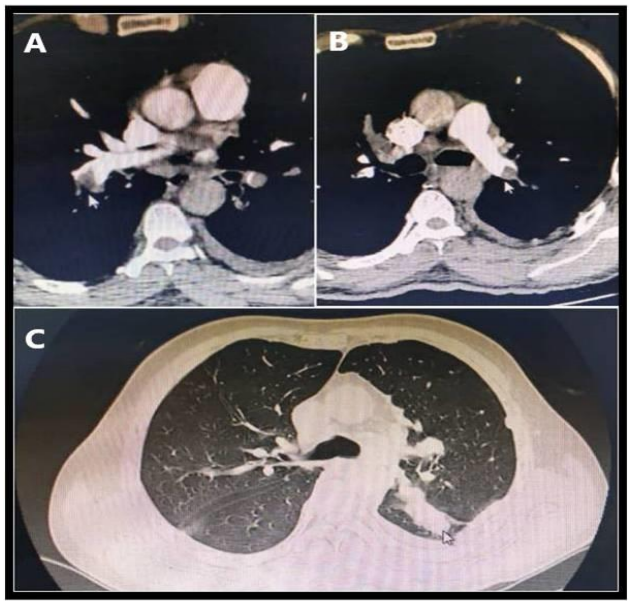
Figure 3
