Barbed Reposition Pharyngoplasty
Barbed Reposition Pharyngoplasty
Dr Osama Hmidan*
*Correspondence to: Dr. Osama Hmidan, Mediclinic Hospital UAE.
Copyright
© 2025 Dr. Osama Hmidan. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 29 January 2025
Published: 05 February 2025
DOI: https://doi.org/10.5281/zenodo.14874452
Abstract
Purpose:
The aim of this 5 cases is to highlight the efficacy of a new modified pharyngoplasty technique with barbed sutures: BARBED REPOSITION PHARYNGOPLASTY, Surgical management of Obstructive Sleep Apnea (OSA) and Snoring has undergone many major and minor changes over a period of last decade. Clinicians have explored surgical options for cure with varying success. Uvulopalatopharyngoplasty was considered as a standard of surgical care but long-term results were not satisfactory. This technique can prove to be a technically less demanding one, which provides excellent long-term results in snoring and OSA with manageable complications.
Barbed Reposition Pharyngoplasty
Technique
The technique of using the 3-0 Polybutester knotless bidirectional reabsorbable sutures introduced for similar purposes by Mantovani et al.To perform a Reposition pharyngoplasty because it displaces the posterior pillar (palatopharyngeal muscle) in a more lateral and anterior position to enlarge the oropharyngeal inlet as well as the retropalatal space, inspired by Cahali. Suspension of the posterior pillar to the pterygomandibular raphe, following Pang et al. Initial weakening of the inferior aspect of the palatopharyngeal muscle, following Cahali and Pang et al. The tip of the uvula is not trimmed, but a mucosal island is removed from its anterior aspect, inspired by Pang et al.
Steps
One needle was introduced at the center point then passed laterally within the palate, turning around pterygomandibular raphe till it comes out at the most superior part of the raphe at one side, the thread is pulled until it hangs at the central transition zone which is a free zone present between the two directions of the thread. The needle again is re-introduced close to point of exit, passing around the pterygomandibular raphe, till it comes out into the tonsillectomy bed, then through the upper part of the palatopharyngeus muscle and comes out near to mucosa of posterior pillar not through it. The posterior pillar is entered at the junction between the upper third and the lower two-thirds. Then, again the needle is passed back through the tonsillectomy bed and then this suture will be suspended around the raphe again, a gentle traction is then applied on the thread only and no knots are taken.
This leads to a stable repositioning of the posterior pillar to more lateral and anterior location without any knot, then this stitch is repeated at least three times between raphe and muscle till the lower pole of the muscle is reached. The opposite side is done by the same way. Finally, cach thread comes out at the raphe of the same side, for locking of the stitches and looseness prevention; a superficial stitch in the opposite direction is taken, and then the thread is cut while bushing the tissue downward for more traction
Fig 1
Fig 2
Fig 3
Conclusion
Our preliminary results suggest that technique is feasible, safe and effective in management of OSA patients. Moreover, it is easy to learn even for not experienced surgeons, less time consuming and with no significant complications. patients who underwent it had successful treatment in 90% of cases, compared to 86% with BRP, with a cure rate of 40% vs. 18%.
References
1. Fujita S et al (1981) Surgical correction of anatomical abnormalities in obstructive sleep apnoea syndrome: uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg 89(6):923–934
Article CAS PubMed Google Scholar
2. Cahali MB (2003) Lateral pharyngoplasty: a new treatment for obstructive sleep apnea hypopnea syndrome. Laryngoscope 113(11):1961–1968
3. Pang KP, Woodson BT (2007) Expansion sphincter pharyngoplasty: a new technique for the treatment of obstructive sleep apnea. Otolaryngol Head Neck surg 137(1):110–114
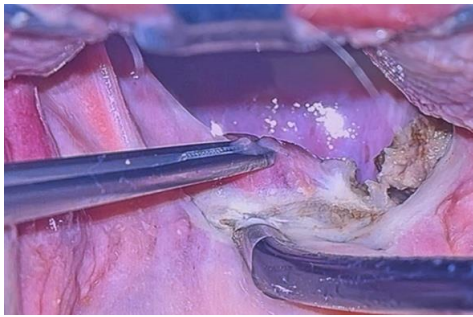
Figure 1
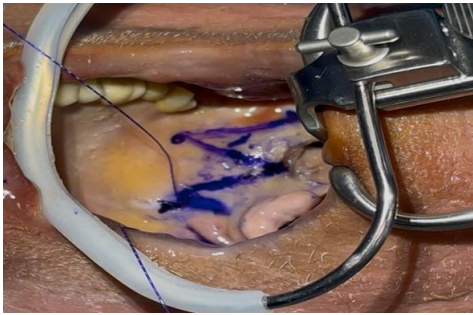
Figure 2
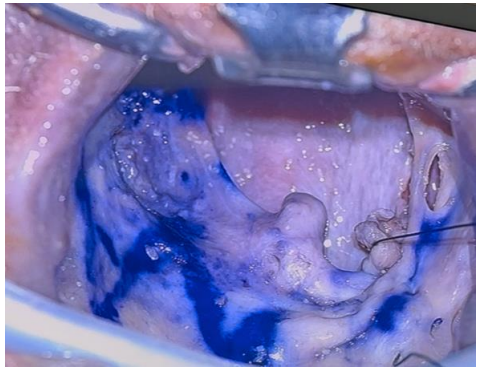
Figure 3
