Carotid Artery Stenosis Related Ischaemia: A Diagnostic Conundrum
Carotid Artery Stenosis Related Ischaemia: A Diagnostic Conundrum
Mr Bhavesh Sharma1*, Mr Habib Khan 2, Mr T Kumar3 , Ms Monali Chakrabarti4
1. Medical Student at University of Manchester, Manchester, UK.
2. Senior Associate specialists, Ophthalmology department, Worcestershire Royal hospital, Worcester, England, UK;
3. Consultant ophthalmologist, Ophthalmology department, Worcestershire Royal hospital, Worcester, England, UK.
4. Senior Author & Consultant Ophthalmologist, Ophthalmology department, Worcestershire Royal hospital, Worcester, England, UK.
*Correspondence to: Mr Bhavesh Sharma, Medical Student at University of Manchester, Manchester, UK.
Copyright
© 2025 Mr Bhavesh Sharma. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 17 January 2025
Published: 01 March 2025
Abstract:
Diagnostic delay can often occur in rare clinical presentations, due to masking by common pathology. We present a rare case of carotid artery stenosis related bilateral ocular ischaemic syndrome in a patient with co-existing Graves’ disease. The visual loss was initially wrongly attributed to the presence of glaucoma and the recent cataract surgery. Hence, this case highlights the importance of both detailed history taking, and a detailed systemic work up of all cases presenting in the Ophthalmology Acute settings.
Carotid Artery Stenosis Related Ischaemia: A Diagnostic Conundrum
Background
Impaired ocular perfusion leading to ocular ischemic syndrome (OIS) is most commonly secondary to atherosclerotic disease related stenosis of the carotid arteries1. OIS is usually seen in the older individuals, with an estimated incidence of 7 cases per million2.
It is a potentially sight-threatening condition and has potential fatal underlying systemic implications. Though Intracranial vascular stenosis causing cerebral infarction has been reported in some cases of hyperthyroidism3 , Internal carotid artery (ICA) stenosis with Graves' disease is extremely rare. 4,5
We present a case report of an 88-year-old female with chronic OIS and accompanying stenosis of the bilateral internal carotid artery (ICA) with history of hyperthyroidism. She also has past ocular history of undergoing bilateral cataract and glaucoma surgery. The diagnosis of OIS was delayed, as her visual symptoms were attributed erroneously to advancing glaucoma and previous surgery related macular changes.
Case Presentation
An 88-year-old lady presented to general ophthalmology clinic. She was bilaterally pseudophakic and also had glaucoma surgery in both her eyes 3 years previously. Her Intraocular pressure (IOP) had stabilised following the glaucoma surgery at 11mmHg and 12 mmHg in the right and left eye respectively (with no additional topical glaucoma medications). She had developed postoperative cystoid macular oedema in the postoperative period in the right eye. However, it had settled within he next few weeks, with documented best corrected visual acuity (BCVA) of 6/9 in right and 6/6 in the left eye. She also noted to have bilateral mild non-exudative age-related macular degeneration changes. On her recent presentation, her BCVA had deteriorated to 6/36 in the right eye and 6/24 in the left eye. Her IOP was 03mmHg in the right and 06 mmHg in the left eye. A diagnosis of Hypotony maculopathy was made, and the patient was referred to specialist glaucoma clinic.
A detailed history-taking revealed that the patient was a chronic smoker >30 pack year history). A past Medical/surgical history included Graves’ disease, gall bladder surgery and left sided deafness following left mastoidectomy. She was on medication for systemic hypertension (Amlodipine) and hypothyroidism ( Thyroxine). However, no clear history of amaurosis fugax, transient ischaemic attack or any thrombo-embolic events were ever recorded.
Further clinical examination in the specialist clinic showed bilateral corneal oedema involving the stroma and endothelium, but excluding the bowman membrane fold. The seidel test from the trabeculectomy bleb was negative in both eyes. Optical Coherence Tomography (OCT) of the macula showed bilateral intraretinal oedema with macular thickening. However, no retinal or choroidal fold were noted, as is usually found in hypotony maculopathy. Fundus Fluorescein angiography (FFA) revealed both the bilaterally reduced/delayed filling of the optic disc-vasculature and the macular oedema. A clinical diagnosis of bilateral ocular ischaemia was arrived at. Blood test revealed a high cholesterol level. A carotid-doppler study showed an 80-90% of the right and a 50% left internal carotid artery stenosis. Further tests included a Magnetic resonance Angiogram (MRA) and cardiac echocardiography. A Duplex ultrasound of the ophthalmic arteries revealed a resistance index of 0.85 in the right and 0.8 in the left ophthalmic artery (up to 0.7 is considered as the normal level). She was advised to quit smoking and also started on clopidogrel 75mg once-daily as a secondary-prevention measure. the patient was prescribed Cholesterol-reducing medication and had her Antihypertensive medications optimised. The surgical option of a Carotid endarterectomy was discussed. A supra-regional opinion from vascular surgeons was taken. In the absence of a clear-cut vascular event and the possible risks of the procedure, extensive vascular surgery was decided against (of note here, that there is a paucity of data regarding the impact of carotid endarterectomy on ocular ischaemia6.7,8). Further, the patient was prescribed topical cycloplegic and steroid drops. Her vision improved slightly and then remained stable with no further significant progression noted over the next 6 months. She maintains a BCVA of 6/18 bilaterally and a IOP of 07mmHg and 09mmHg in the right and left eye respectively.
Discussion
This case highlights the need for a ever-vigilant clinician, and emphasizes the importance of detailed history-taking and a thorough interpretation of all clinical signs and investigations. In the general clinic, the visual loss was wrongly attributed to the history of chronic glaucoma and the previous ocular surgeries.
The corneal oedema associated with post-glaucoma-surgery-hypotony (PGSH) usually shows bowman membrane folds, which were absent in this case. PGSH is usually an acute or subacute phase (e.g. in leaking blebs), thus resulting in the bowman membrane folds. On the other hand, the corneal oedema due to ocular ischaemia is related to poor corneal endothelial function, and hence is confined to the corneal stroma and endothelium. Hypotony maculopathy usually shows macular area retinal and choroidal folds, especially at the retinal pigment epithelial (RPE) level. In this case, no such RPE level folds were observed. The FFA showed delayed filling of optic disc vessels. This strongly suggests any compromised ocular perfusion as the primary pathology. More over Bilateral simultaneous changes in glaucoma-surgical-bleb, causing similar over-filtration in both eyes, that too in the absence of any bleb-leak, is extremely unlikely.
This led to more detailed history-taking which correctly revealed the existing risk-factors including smoking, and hypertension. Hypercholesterolemia was then diagnosed as per the blood investigations. The secondary prevention was discussed and further trestments commenced 9,10,10,11,12. The involvement of vascular team enhanced the decision-making process. The carotid-doppler and duplex-ultrasound of the ophthalmic artery further help confirm the diagnosis. MRA and cardiac-echocardiogram provided the relevant positive and negative findings. This multidisciplinary approach also helped the patient to take an informed decision. However, the Ophthalmic consultation also caused some patient-anxiety when a carotid-endarterectomy surgery was suggested. The role of such surgery is not as yet fully established in ocular ischaemia. The patient was thankfully reassured by the timely supra-regional referral and the discussion with the leading vascular surgeon. Patient was reassured and secondary preventative measures stabilised her vision, which can be explained as improving the blood flow through existing channels.
The key lesson here, for any general-ophthalmology team is to have the awareness about the masquerading of any rare/serious conditions behind the common co-pathology/conditions. Also highlighted is the importance of a detailed history-taking and a proper clinical assessment. This could be crucial for both a timely identification of ocular ischaemia and hence, potentially for the survival of the patient. This case also highlights that catching the early manifestations may help preserve sight and produce better outcomes.
Fig 1, Fig 2
References
1. Arthur A, Alexander A, Bal S, et al. Ophthalmic masquerades of the atherosclerotic carotids. Indian J Ophthalmol 2014;62:472. 10.4103/0301-4738.121183
2. Gunna NT, Paritala A, Takkar B, Sheth J. Ocular ischaemic syndrome following coil embolisation for direct carotid cavernous fistula. BMJ Case Rep. 2021 May 27;14(5):e242121. doi: 10.1136/bcr-2021-242121. PMID: 34045204; PMCID: PMC8162104.
3. Terelak-Borys B, Skonieczna K, Grabska-Liberek I. Ocular ischemic syndrome - a systematic review. Med Sci Monit. 2012;18(8):RA138–RA144. doi:10.12659/msm.883260
4. Yamashita S, Tamiya T, Shindo A, Miyake K, Nakamura T, Ogawa D, Kuroda Y, Nagao S. Improvement of cerebral arterial stenosis associated with Basedow's disease. Case Report Neurol Med Chir (Tokyo). 2005;45:578–582.
5. Kamasaki H, Takeuchi T, Mikami T, Komeichi K, Tsutsumi H. A case of Graves' disease diagnosed in the course of bilateral carotid artery stenoses (moyamoya disease); a case report and review of the literature. Clin Pediatr Endocrinol. 2013;22:39–44.
6. Suhail S, Tallarita T, Kanzafarova I, Lau J, Mansukhani S, Olatunji S, Calvin AD, Moustafa B, Manz J, Sen I. Ocular Ischemic Syndrome and the Role of Carotid Artery Revascularization. Ann Vasc Surg. 2024 Aug;105:165-176. doi: 10.1016/j.avsg.2023.12.098. Epub 2024 Apr 2. PMID: 38574808.
7. Lauria AL, Koelling EE, Houghtaling PM, White PW. Carotid Endarterectomy for Ocular Ischemic Syndrome: A Case Report and Review of the Literature. Ann Vasc Surg. 2020 Aug;67:567.e9-567.e12. doi: 10.1016/j.avsg.2020.03.005. Epub 2020 Mar 21. PMID: 32209415.
8. Hou X, Jie C, Liu Z, Bi X, Deng Y, Li Y, Wang J, Zhang W. Changes in the retina and choroid in patients with internal carotid artery stenosis: a systematic review and meta-analysis. Front Neurosci. 2024 Apr 15;18:1368957. doi: 10.3389/fnins.2024.1368957. PMID: 38686328; PMCID: PMC11056587.
9. Messas E, Goudot G, Halliday A, Sitruk J, Mirault T, Khider L, Saldmann F, Mazzolai L, Aboyans V. Management of carotid stenosis for primary and secondary prevention of stroke: state-of-the-art 2020: a critical review. Eur Heart J Suppl. 2020 Dec 6;22(Suppl M):M35-M42. doi: 10.1093/eurheartj/suaa162. PMID: 33664638; PMCID: PMC7916422.
10. Beckman JA. Antithrombotic therapies in cerebrovascular disease: what should we use as secondary prevention in patients with carotid artery disease? Catheter Cardiovasc Interv. 2009 Jul 1;74 Suppl 1:S12-6. doi: 10.1002/ccd.22056. PMID: 19530155.
11. Vande Griend JP, Saseen JJ. Combination antiplatelet agents for secondary prevention of ischemic stroke. Pharmacotherapy. 2008 Oct;28(10):1233-42. doi: 10.1592/phco.28.10.1233. PMID: 18823219.
12. Serebruany VL, Malinin AI, Pokov AN, Hanley DF. Antiplatelet profiles of the fixed-dose combination of extended-release dipyridamole and low-dose aspirin compared with clopidogrel with or without aspirin in patients with type 2 diabetes and a history of transient ischemic attack: a randomized, single-blind, 30-day trial. Clin Ther. 2008 Feb;30(2):249-59. doi: 10.1016/j.clinthera.2008.02.006. PMID: 18343263.
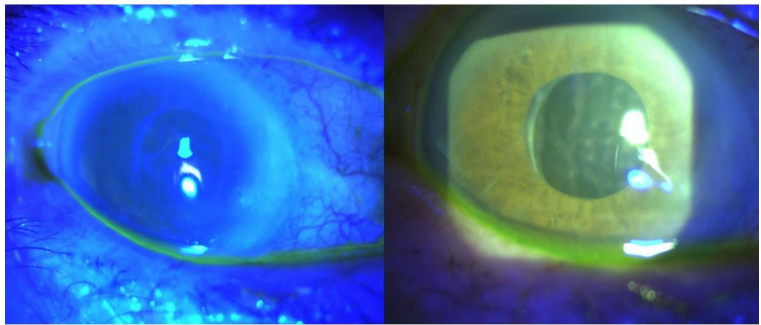
Figure 1
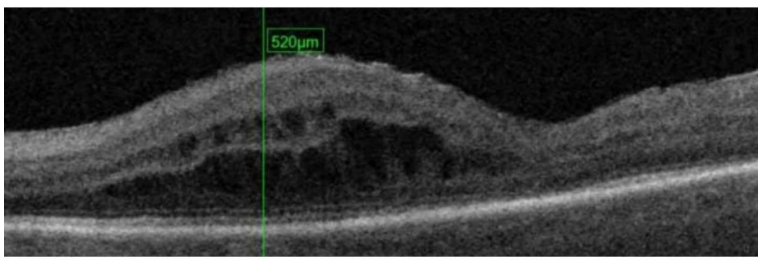
Figure 2
