Unraveling the Puzzle: A Journey into Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome
Unraveling the Puzzle: A Journey into Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome
Khetam Berro1, Hitaf Nasrallah *2
1,2. Khetam Berro, Department of Pediatric Dentistry, Lebanese University, Beirut, Lebanon.
*Correspondence to: Hitaf Nasrallah, Department of Pediatric Dentistry, Lebanese University, Beirut, Lebanon.
Copyright.
© 2025 Hitaf Nasrallah This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 15 Feb 2025
Published: 01 Mar 2025
ABSTRACT
Amelogenesis imperfecta is a genetically and clinically varied set of inherited enamel defects, initially perceived as an isolated trait but increasingly recognized to coexist with oro-dental and systemic features. In the diagnostic journey of a 7-year-old female previously diagnosed with congenital adrenal hyperplasia, her oro-dental findings led to the suspicion of more complex pathological condition. Ultimately, the revelation of a FAM20A mutation alongside CYP21A2 mutations through whole exome sequencing (WES) marked a decisive turning. This unexpected genetic discovery prompted a shift in diagnostic considerations, directing attention towards conditions such as Enamel Renal Syndrome or Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome (AIGFS). Based on a collaborative effort, involving endocrinologist, pediatric nephrologist, and genetic counselor, orchestrating a meticulous and comprehensive assessment, a multidisciplinary approach was followed, inclusive of medical and clinical evaluations, laboratory analysis, gingival biopsy, and trans-abdominal ultrasound to explore the complex interplay between genetic factors, endocrine anomalies, and dental abnormalities. A significant challenge emerged in discerning whether the patient's presentation aligned more with AIGFS or with ERS. Following thorough examinations and syntheses of the clinical and genetic data, the diagnostic trajectory solidified, ultimately confirming a rare diagnosis of AIGFS. This case exemplifies the complex nature of rare genetic disorders and underscores the indispensable role of a multidisciplinary approach in achieving precise diagnosis, despite the challenges posed in distinguishing between distinct syndromes
Unraveling the Puzzle: A Journey into Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome
Introduction
Amelogenesis imperfecta (AI) is a genetically and clinically heterogeneous group of inherited dental enamel defects.1 Commonly described as an isolated trait, it may be observed concomitantly with other oro-dental and/or systemic features such as nephrocalcinosis in Enamel Renal Syndrome (ERS, MIM#204690), or gingival hyperplasia in Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome (AIGFS, MIM#614253).1
Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome (AIGFS) and Enamel Renal Syndrome (ERS) are both rare genetic disorders that affect tooth enamel. AIGFS is an autosomal recessive condition characterized by mild gingival fibromatosis and dental anomalies, including hypoplastic amelogenesis imperfecta, intrapulpal calcifications, delay of tooth eruption, hypodontia/oligodontia, pericoronal radiolucencies, and unerupted teeth.2 ERS, on the other hand, is a rare disorder featured by amelogenesis imperfecta, gingival fibromatosis, and nephrocalcinosis.3 It is caused by bi-allelic mutations in the secretory pathway pseudokinase FAM20A.3 The pathogenesis of ERS-associated gingival fibromatosis is currently unknown, but a proteomic approach has been used to identify dysregulated proteins in the conditioned media of gingival fibroblasts obtained from ERS patients carrying distinct mutations and control subjects.3
One study found that the abundance of 109 proteins had increased or decreased at least 1.5-fold compared to control gingival fibroblasts. Proteins over-represented were mainly involved in extracellular matrix organization, collagen fibril assembly, and biomineralization whereas those under-represented were extracellular matrix-associated proteins.
Transforming growth factor-beta 2, a member of the TGFβ family involved in both mineralization and fibrosis, was strongly increased in samples from gingival fibroblasts of ERS patients and so were various known targets of the TGFβ signaling pathway including Collagens, Matrix metallopeptidase 2 and Fibronectin.3 While both syndromes involve abnormalities in tooth enamel, ERS is characterized by nephrocalcinosis, which is not present in AIGFS.2
This report details a 7-year-old's case of Amelogenesis Imperfecta Gingival Fibromatosis Syndrome, presenting a unique case with genetic rarity affecting less than 1 in a million.2
The goal is to highlight the complexities of rare genetic disorders and stress the collaborative nature of diagnostics, involving specialists for a holistic assessment. This case also highlights the importance of oral findings in the diagnosis of complex medical conditions.
Case Presentation
This case report was approved by the ethics committee of the Lebanese University; it focuses on a rare case involving a 7-year-old female patient who had the initial diagnosis of congenital adrenal hyperplasia (CAH) made at birth. The diagnosis was prompted by sexual ambiguity, with a karyotype of 46, XX which was done at birth. The diagnostic journey took a decisive turn with the strategic decision to undertake (WES) which is a genetic test progressively expanding in clinical diagnostics across various indications to identify the genetic basis of diseases.4 This advanced genetic analysis unexpectedly revealed a homozygous mutation in the FAM20A gene (NM_017565.3:c.1081C>T p.Arg361Cys), an important discovery redirecting diagnostic considerations towards AIGFS or ERS.
The patient is the only child of consanguineous parents. The parents are not affected by CAH nor AIGFS. The patient's general physical condition includes CAH, which is an autosomal recessive disease5 characterized by an impairment of steroid synthesis due to an altered production of 21-hydroxylase enzyme.6 She was on 10mg of corticosteroids daily and triptorelin, GnRH analogue, a synthetic hormone that acts on reproductive organs, due to signs of early puberty. The patient presented to the Pediatric Dentistry Department at the Faculty of Dental Medicine – Lebanese University, with a primary concern about the appearance of her smile, reporting instances of bullying at school due to her dental aesthetics. Her stature was 111 cm, notably shorter than that typical for her age, and her weight was 19 kgs, contributing to a wasted appearance. During extraoral examination, facial proportions were found to be balanced, presenting a straight profile, low hairline, and distinctive features such as thick eyebrows and facial hair. Intraoral examination revealed generalized gingival hyperplasia with normal-colored and firm mucosa. She displayed a mixed dentition that was delayed compared to her chronological age. There was wear of the occlusal surface due to defective enamel surface. The enamel surface appeared as chalky, rough, scratchy both deciduous and permanent teeth had thin and low-density enamel layer as appeared on radiography.
Diagnostic Assessments
Genetic test:
Commencing with genetic testing, WES revealed homozygosity for a confirmed pathogenic variant in the CYP21A2 gene (NM_000500.7.2:c.518T>A p.Ile173Asn) which validates CAH. On the other hand, homozygosity for a recognized likely pathogenic variant in the FAM20A gene (NM_017565.3:c.1081C>T p.Arg361Cys) directs diagnostic considerations towards Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome or Enamel Renal Syndrome.
Following consultation with a pediatric nephrologist and genetic counselor, additional tests were conducted.
Clinical tests:
Hematological tests were carried out to reveal parameters within normal ranges. Biochemical investigations, encompassing serum components, electrolytes, and liver function markers, indicated normal values. Recognizing potential renal involvement as in ERS, an abdominal ultrasound was strategically employed to assess for nephrocalcinosis. The trans-abdominal ultrasound revealed normal liver size and homogeneity without focal lesions or bile duct dilatation. The gall bladder, pancreas, and spleen were within normal parameters, and the kidneys exhibited normal size without hydronephrosis or nephrocalcinosis.
Diagnostic criteria of ERS/AIGFS:
Clinical diagnosis highlights the relationship between oral and dental features and renal observations, which could potentially result in renal impairment.
Dental Phenotype:
Oral (figure 1) and radiographic (figure 2) examination of the patient showed consistent dental findings: generalized, thin hypoplastic or absent enamel; both primary and permanent teeth affected; flat cusps on posterior teeth; relative microdontia and spaced teeth; delayed tooth eruption; impacted posterior teeth; and semi-lunar shape of central incisor edge. Hypomaturation or hypocalcified AI have never been described in ERS.1
Figure 1: Clinical presentation
Figure 2: Radiographic examination
Gingival phenotype:
Fibrous gingival hyperplasia is pathognomonic, with variable severity.7 This explains why, when prominent, patients have been diagnosed clinically as having AIGFS. It has been described as an important feature of AIGFS.8 Biopsies from two areas, one from the lower right partially erupted canine and the other from the gingiva of the lower left molar, revealed subacute erosive gingiva with dystrophic calcifications. The erosive gingiva is possibly attributed to long-term corticosteroid treatment, while dystrophic calcifications are associated with AIGFS.9
Renal phenotype:
Although the oral characteristics of the condition are noticeable during childhood, any renal involvement remains clinically silent at this stage and necessitates additional investigation for identification.1 Nephrocalcinosis was reported in patients affected by “AI and nephrocalcinosis” and by ERS but not explored in AIGFS patients.1 The trans-abdominal ultrasound of the kidneys exhibited normal size without nephrocalcinosis. After all such an exhaustive assessment, a definitive diagnosis of AIGFS was confirmed.
Diagnostic challenges:
Ambiguous initial diagnosis of CAH at birth based on sexual ambiguity presented a challenge in determining the accurate cause of the patient's symptoms. In addition, the overlap between ERS and AIGFS can be challenging because of the similarities in their clinical and radiographic features when even some authors were convinced these two disorders are actually the same entity.8 Both conditions present with hypoplastic amelogenesis imperfecta, which is a defect in the enamel formation of the teeth. In addition, both conditions can cause gingival enlargement, which is an abnormal growth of the gum tissue.
However, ERS is also associated with nephrocalcinosis2, which is the deposition of calcium salts in the kidneys, while AIGFS is associated with gingival fibromatosis, which is a benign overgrowth of the gum tissue.9
Moreover, multidisciplinary collaboration efforts between endocrinologist, pediatric nephrologist, and genetic counselors require effective communication and cooperation to ensure a comprehensive assessment and accurate diagnosis.
On the other hand, this article highlights a notable gap in the existing literature, pointing out the absence of clear guidelines for diagnosing AIGFS leaving practitioners to navigate diagnostic processes without standardized protocols or criteria. In addition, assessing the long-term prognosis and potential complications associated with AIGFS seem challenging, given the limited available data on the natural course of the syndrome. In our case, we had difficulty providing appropriate genetic counseling to the parents, especially in a consanguineous setting, to understand the implications of the identified genetic mutations and potential risks for future offspring.
Treatment
As part of her comprehensive treatment plan, the patient continued with the prescribed medication outlined by the endocrinologist for her congenital adrenal hyperplasia. Additionally, addressing the dental aspects of her Amelogenesis Imperfecta and Gingival Fibromatosis Syndrome, she underwent an extensive dental treatment aimed at improving both function and aesthetics. The treatment included a gingivectomy procedure, as well as the placement of posterior and anterior crowns.
Despite the absence of renal involvement noted in the abdominal ultrasound, the pediatric nephrologist recommended annual renal ultrasounds. This precautionary measure was taken due to the limited information available in the literature regarding AIGFS and its potential correlation with age. Regular monitoring through renal ultrasounds was deemed necessary to better understand the long-term implications and any potential renal involvement associated with the syndrome.
In addressing the psychosocial aspects of the patient's well-being, a psychologist was involved in her care to provide support and guidance, particularly in coping with issues related to sexual ambiguity, experiences of bullying at school, and concerns about her dental appearance. The psychological treatment aimed to empower the patient with coping strategies, enhance her self-esteem, and foster emotional resilience in navigating the challenges associated with her unique medical and social circumstances.
Conclusion
This case serves as a paradigm highlighting the intricate nature of rare genetic disorders. It underscores the indispensable role of a multidisciplinary approach, advanced genetic testing, and ongoing research endeavors.
It emphasizes the critical need for heightened awareness, collaborative care, and a comprehensive understanding of the complex interplay between genetic, medical, and psychosocial factors. These elements are crucial not only for achieving precise diagnosis but also for optimizing patient outcomes in the realm of rare genetic conditions.
References
1. de la Dure-Molla M, Quentric M, Yamaguti PM, Acevedo AC, Mighell AJ, Vikkula M, Huckert M, Berdal A, Bloch-Zupan A. Pathognomonic oral profile of Enamel Renal Syndrome (ERS) caused by recessive FAM20A mutations. Orphanet J Rare Dis. 2014, 9:84. 10.1186/1750- 1172-9-84
2. Amelogenesis Imperfecta, Type IG; AI1G #204690. (2022). Accessed: May 25, 2022: https://omim.org/entry/204690? search=AMELOGENESIS%20IMPERFECTA%2C%20TYPE%20IG%3B%20AI1G&highlight=ai1g%2Camelogenesi%....
3. Simancas Escorcia V, Guillou C, Abbad L, Derrien L, Rodrigues Rezende Costa C, Cannaya V, Benassarou M, Chatziantoniou C, Berdal A, Acevedo AC, Cases O, Cosette P, Kozyraki R. Pathogenesis of Enamel-Renal Syndrome Associated Gingival Fibromatosis: A Proteomic Approach. Front Endocrinol (Lausanne). 2021, 29;12:752568. 10.3389/fendo.2021.752568
4. Retterer, K., Juusola, J., Cho, M. et al. Clinical application of whole-exome sequencing across clinical indications. Genet Med 2016, 18(7):696-704. 10.1038/gim.2015.148
5. Momodu II, Lee B, Singh G. Congenital Adrenal Hyperplasia. In: StatPearls. Treasure Island (FL): StatPearls Publishing; July 17, 2023
6. Di Cosola M, Spirito F, Zhurakivska K, Nocini R, Lovero R, Sembronio S, Santacroce L, Brauner E, Storto G, Lo Muzio L, Cazzolla AP. Congenital adrenal hyperplasia. Role of dentist in early diagnosis. Open Med (Wars). 2022,17(1):1699-1704. 10.1515/med-2022-0524
7. Paula LM, Melo NS, Silva Guerra EN, Mestrinho DH, Acevedo AC: Case report of a rare syndrome associating amelogenesis imperfecta and nephrocalcinosis in a consanguineous family. Arch Oral Biol. 2005, 50: 237-242. 10.1016/j.archoralbio.2004.11.023
8. Kantaputra PN, Kaewgahya M, Khemaleelakul U, Dejkhamron P, Sutthimethakorn S, Thongboonkerd V, Iamaroon A. Enamel-renal-gingival syndrome and FAM20A mutations. Am J Med Genet A. 2014,164A(1):1-9. 10.1002/ajmg.a.36187
9. Roomaney IA, Kabbashi S, Chetty M. Enamel Renal Syndrome: Protocol for a Scoping Review. JMIR Research Protocols. 2021, 10(11):e29702. 10.2196/29702.
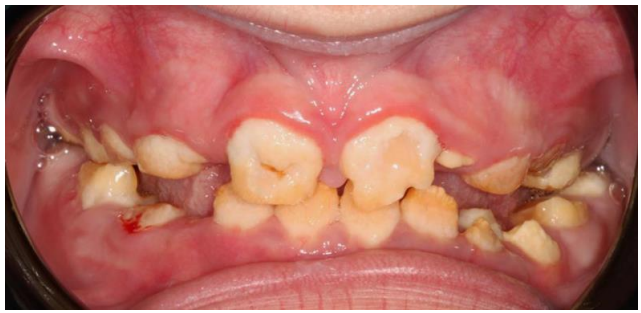
Figure 1
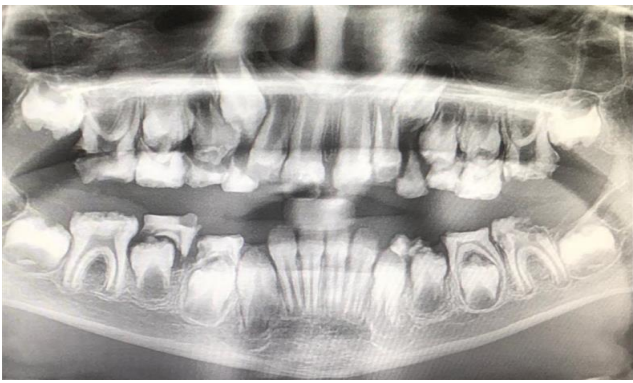
Figure 2
