Successful Labour Analgesia in a Patient with Posterior Corrective Surgery for Thoracolumbar scoliosis -A Case Report
Successful Labour Analgesia in a Patient with Posterior Corrective Surgery for Thoracolumbar scoliosis -A Case Report
Dr.Afroz Shahana Mehboob Khan MD1, Dr. Rahul Shivdas Patil MD2, Dr. Sangamitra Kashinath Kamble M.D3 & Dr. Rajendra Prasad Koduri MD,EDAIC4*
1,3. Specialist Anesthesiologist NMC Hospital
2,4. Specialist Anesthesiologist SSMC
*Correspondence to: Dr. Rajendra Prasad Koduri, Specialist Anesthesiologist SSMC.
Copyright
© 2025 Dr. Rajendra Prasad Koduri. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 15 February 2025
Published: 17 March 2025
DOI: https://doi.org/10.5281/zenodo.15044313
ABSTRACT:
Background: Administration of lumbar epidural analgesia in a parturient with previous spinal surgery presents a particular challenge to the anaesthesiologist. The difficulties could range from inability to identify the epidural space, multiple attempts before catheter placement, vascular trauma, subdural local anaesthetic injection and accidental dural puncture.
Methods: We report successful labour analgesia in a parturient with congenital scoliosis corrected with extensive posterior instrumentation. Combined spinal- epidural analgesia was performed through L4-L5 interspace, although it was done under ultrasound guidance it was technically difficult as two attempts were required for spinal puncture.
Results: The patient had a normal vaginal delivery with satisfactory sensory analgesia. There was no post-procedure complication encountered.
Conclusion: Lumbar epidural analgesia is known to be technically difficult in patients with prior spinal surgery. We recommend early assessment by a multidisciplinary team of experts, including obstetricians, obstetric anaesthesiologists, and spine surgeons to develop an individually tailored peripartum care plan for labour analgesia.
Successful Labour Analgesia in a Patient with Posterior Corrective Surgery for Thoracolumbar scoliosis -A Case Report
Introduction
Scoliosis is characterized by the deformity of lateral curvature of the spine. Many of the cases are idiopathic [1] with an incidence of up to 4% in the general population.[2] Incidence is similar in males and females with milder curves of 10 degrees, with more preponderance in females compared to males with scoliosis greater than 30 degrees.[3] Thus, an obstetric anaesthesiologist needs to be well-versed with the impact of scoliosis and its demanding challenges in providing safe anaesthetic management.[4,5]
Neuraxial anaesthesia can be challenging in patients with posterior instrumentation due to difficulties in palpating anatomical landmarks, increased chances of dural puncture, and difficulty in predicting the extent of the block thus failure to achieve an adequate level of analgesia.[6]
We report a case of successful labour analgesia in a patient who had undergone extensive corrective surgery for idiopathic congenital thoracolumbar scoliosis.
Case Report
A 26-yr-old gravida 2, para 1 woman was referred by her obstetrician to the pre-anaesthesia assessment clinic at 38 weeks gestation for evaluation. The patient was very keen to know whether she would be able to receive an epidural for labour analgesia. She had a history of severe congenital scoliosis which was corrected at 13 years of age with posterior instrumentation (Fig 1). She had on-and-off complaints of low back pain with shooting pain in her right leg. Her previous normal vaginal delivery was managed with intramuscular pethidine as the patient was denied epidural labour analgesia. On examination, she weighed 73.3 kg with a height of 155 cm (body mass index 30.5 kg/ m2). The patient's back had a long scar running in the thoracolumbar region. However, on palpation of her spine no useful landmarks could be identified. Ultrasound was done in the pre-anaesthesia clinic and L4-L5 and L5- S1 interspaces could be identified.
Fig 1
MRI of the spine revealed posterior corrective surgery with metallic implants from D4 down to L3 with preserved vertebral bodies and alignment with residual thoracolumbar scoliosis.
On airway assessment, she had a good mouth opening with a Mallampati score of 2 and a thyromental distance greater than 6 cm with good neck and jaw movements. The patient was explained that labour analgesia would be with a combined spinal epidural technique and the procedure was expected to be difficult and may require more than the usual time. Chances of failure to achieve adequate analgesia and patchy effects were also discussed & other options such as Entonox supplementation, intramuscular pethidine were also discussed as part of failure to site the labor epidural.
The orthopaedician reviewed the patient for labour analgesia and did a complete neurological assessment which was normal.
After admission to labour room, the epidural was requested. As per plan combined spinal epidural was explained to the patient. Palpation of her spine revealed no landmarks other than iliac crests. On ultrasound with 3.75 MHz curved array probe L4-L5 and L5- S1 interspace were recognized. Epidural was sited at L4-L5 interspace with 18-gauge Tuohy needle after two attempts and with needle through needle technique spinal analgesia with bupivacaine 2 mg with fentanyl 25 micrograms was administered. Epidural catheter was threaded thereafter.
The epidural was continued with Ropivacine 0.1% and fentanyl 2mcg/ml using a patient controlled epidural analgesia. Adequate analgesia was achieved through out the labour with no undue side effects. The patient did not require additional local anaesthetic boluses. The patient had normal vaginal delivery after 6 hrs with satisfactory analgesia.
Discussion
Neuraxial analgesia can be beneficial in patients with scoliosis during labour as it can be used as an anaesthetic option if a caesarean section or instrumental delivery is required. The rate of an operative delivery is 2.5 times higher in parturients with scoliosis [7] due to a higher incidence of cephalopelvic disproportion.
Neuraxial procedures in patients with spine surgeries with metal rods reduces the patient's ability to flex their spine thus hindering the requisite optimum positioning. [8] The presence of scar tissue and bony mass in the operated area may cause difficulty in insertion of the epidural needle through the midline or lateral approach. [9] Palpation of spinous processes may not be possible in the fused area. There can be narrowing of epidural space resulting from scarring due to accidental ligamentum flavum injury during surgery causing issues with the spread of local anaesthetic solutions in the epidural space giving patchy or unilateral block. [10] Therefore, it can be technically difficult and may not provide the desired effects. Other option can be to place epidural catheter either above or below the site of previous surgery. [11,12,13] spinal anaesthesia at the L5-S1 level, which is the widest space in the spine, may also be utilised as last resort. [14] Patients must be evaluated on an individual basis to determine if they are appropriate candidates for a neuraxial technique.
CSE or single-shot spinal anaesthesia ( later in the second stage of labor )is a better choice than epidural anaesthesia alone as post-surgical planes could give false loss of resistance, CSF flow is a definite confirmation of placement in comparison to the loss of resistance in this situation.
Additionally, injection of the local anaesthetic into the CSF provides a more reliable spread.
Some patients may have persistent back pain and neuraxial procedures for labour analgesia in such patients with persistent back pain could result in medicolegal litigation. Because of technical challenges, many times anaesthesiologists are not comfortable in providing neuraxial procedures for labour analgesia in this kind of cases.
In our case, epidural was successful after two attempts. The onset of action, the spread, dose requirement, the highest sensory level, and the duration of action of the local anaesthetic solutions were not different from what we have seen in normal patients in our institution.The patient was followed up for 7 days post partum & she did not develop any post-procedure complications.
Conclusion
In summary, lumbar epidural analgesia is known to be challenging in patients with prior spine instrumentation. These difficulties range from inability to identify the epidural space, multiple attempts before catheter insertion, vascular trauma, and accidental dural puncture.
Parturients with spinal surgery who are keen on taking neuraxial labour analgesia should be evaluated by a multidisciplinary team of experts, including the obstetricians, obstetric anaesthesiologists, spine surgeons and individually tailored peripartum care plan must be devised (continuous lumbar epidural, combined spinal-epidural, or caudal epidural) to provide appropriate labour analgesia.
References
1. Preston R, Crosby ET. Musculoskeletal disorders. In: Chestnut DH, Polley LS, Tsen LC, Wong CA, eds. Obstetric anesthesia: principles and practice. 4th ed. Philadelphia: Mosby-Elsevier, 2009:1035–52
2. Konieczny M R, Senyurt H, Krauspe R. Epidemiology of adolescent idiopathic scoliosis. J Child Orthop. 2013;7(1):3–9.
3. Reamy B V, Slakey J B. Adolescent idiopathic scoliosis: review and current concepts. Am Fam Physician. 2001;64(1):111–116.
4. Gambrall M. Anesthetic implications for surgical correction of scoliosis. AANA 2007;75:277-285
5. Ko J, Leffert L. Clinical implications of neuraxial anesthesia in the parturient with scoliosis. Anesth A nalg 2009;109:1930-1934
6. Crosby ET, Halpern SH. Obstetric epidural anaesthesia in patients with Harrington instrumentation. Can J Anaesth 1989; 36: 693–6
7. Smith PS, Wilson RC, Robinson APC, G R Lyons. Regional blockade for delivery in women with scoliosis or previous spinal surgery. International Journal of Obstetric Anesthesia 2003;12:17-22
8. Ismail S. Editorial View- Labor analgesia for the parturients with scoliosis, prior spinal surgery and spina bifida. http://www.apicareonline.com/editorial-view-labor-analgesia- for-the-parturients-with-scoliosis-prior-spinal-surgery-andspina-bifida/ (accessed on 06/23/16)
9. Crosby ET, Halpern SH. Obstetric epidural anaesthesia in patients with Harrington instrumentation. Can J Anaesth 1989;36:693– 6
10. Sen O, Kizilkilic O, Aydin MV, Yalcin O, Erdogan B, Cekinmez M, Caner H, Altinors N. The role of closed-suction drainage in preventing epidural fibrosis and its correlation with a new grading system of epidural fibrosis on the basis of MRI. Eur Spine
J. 2005;14:409–14
11. Moeller-Bertram T, Kuczkowski KM, Ahadian F. Labor analgesia in a parturient with prior Harrington rod instrumentation: is caudal epidural an option? Ann Fr Anesth Reanim 2004;23: 925– 6
12. Sudunagunta S, Eckersall SJ, Gowrie-Mohan S. Continuous caudal analgesia in labour for a patient with Harrington rods. Int J Obstet Anesth 1998;7:128 –30
13. Sharrock NE, Urquhart B, Mineo R. Extradural anaesthesia in patients with previous lumbar spine surgery. Br J Anaesth 1990;65:237–9
14. Kardash K, King BW, Datta S. Spinal anaesthesia for caesarean section after Harrington instrumentation. Can J Anaesth 1993;40:667–9.
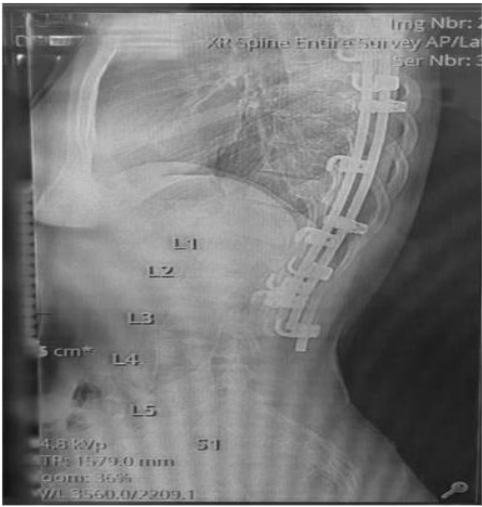
Figure 1
