Laparoscopic Management of a Seminal Vesicle Stone: A Case Report with Literature Review
Laparoscopic Management of a Seminal Vesicle Stone: A Case Report with Literature Review
Ramazan Demirci*1, Nikolas Papadimas2, Robert R.V. Hefty3
*Correspondence to: Ramazan Demirci, Germany.
Copyright
© 2025 Ramazan Demirci. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 14 April 2025
Published: 26 April 2025
DOI: https://doi.org/10.5281/zenodo.15285437
Abstract
Seminal vesicle stones are a rare cause of lower urinary tract symptoms, including hematospermia, ejaculatory pain, and perineal discomfort. This case report describes a 26 year-old male presenting with such symptoms. Transrectal ultrasound and pelvic MRI revealed a 0.7 cm calculus within the enlarged left seminal vesicle. Laparoscopic excision was performed, utilizing a transperitoneal approach with three 5-mm ports. The stone was successfully removed, and the seminal vesicle was closed with a 4-0 absorbable suture. The patient's postoperative recovery was uneventful, and his symptoms resolved completely. This case demonstrates the efficacy and safety of laparoscopic management for seminal vesicle stones, offering a minimally invasive alternative to open surgery. A review of the literature highlights the diagnostic and therapeutic challenges associated with this rare condition.
Laparoscopic Management of a Seminal Vesicle Stone: A Case Report with Literature Review
Introduction
Seminal vesicle stones show up pretty rarely, but when they do, they can trigger a range of urinary issues that really take a toll on a patient’s everyday life [1]. They might cause blood in the semen, pain when ejaculating, and other lower urinary tract problems—issues that seem to stem from a mix of factors like ongoing inflammation, infection, urine stagnation, and even some congenital quirks in the seminal vesicles that stop them from working right [2]. Doctors don’t stick to just one imaging trick; they often pick from transrectal ultrasound, CT scans, or MRI, as each one paints a different picture of the seminal vesicles and the nearby anatomy [3]. Treatment isn’t a one-size-fits-all deal either; sometimes, a round of analgesics and antibiotics will do the trick, while in other cases a more hands-on approach—be it transurethral resection, open surgery, or increasingly laparoscopic methods—is chosen based on the stone’s size, its location, and exactly what symptoms it’s causing. In our report, we share a case involving a symptomatic seminal vesicle stone that was handled with laparoscopic excision – we go into the surgical technique used, touch on the post-op outcomes, and offer a look back at related literature.
Case Presentation
A 26-year-old man came into our urology clinic complaining of persistent pelvic pain, occasional streaks of blood in his semen, and painful ejaculation—a trio of issues he’d been dealing with for roughly 2 months. His past health record was pretty spotless, with no previous troubles in the urological department, no STIs, and no noteworthy systemic problems. These symptoms, in most cases, tend to hint at an underlying urological matter, which is why a careful check-up and prompt diagnosis are so important. Some previous studies even point out that signs like these should lead doctors to consider a range of possibilities—from genitourinary infections to conditions such as hydatid disease that can show up in a similar way [4]. Even when things seem simple at first glance, the messy nature of chronic pelvic pain often calls for a more nuanced, thoughtful approach to evaluating and managing the patient [5].
Initial Diagnosis and Examination:
Male urological issues often bring a mix of factors into play – things like past infections or having had pelvic surgeries might really sway what doctors end up diagnosing. A hands-on exam was done, including a digital rectal check, and nothing too unusual popped up—no lumps or signs that the prostate was getting bigger, which pretty much rings true with earlier reports [5]. Lab tests like a full blood count, serum electrolytes and urinalysis all came back within expected ranges, lending further backup to the initial clinical view. Then again, the semen test painted a slightly different picture: it showed traces of hemospermia along with a higher than usual white blood cell level, hinting at potential inflammation or even a low-level infection—as has been
seen in other reports [6]. All in all, these findings need to be weighed carefully against the wider clinical background to help steer the next steps in patient management.
Diagnostic Evaluation:
We wanted to get to the bottom of the patient's symptoms, so we started off by doing a transrectal ultrasound exam. The scan revealed that the left seminal vesicle was noticeably swollen and had a bright lesion inside it—which, along with a trailing shadow, pointed pretty clearly to a stone (Figure 1).
Figure 1: A transrectal sonography revealed that a 7 mm Stone (yellow arrow) with seminal vesicle (red circle) enlargement.
Next, we checked things out further with a pelvic MRI that confirmed a roughly 1.5 cm calculus lodged in the enlarged vesicle (Figure 2).
Figure 2: In the T2 sequences of MR imaging, it was found that a stone ca 7 mm.
It’s also worth noting that no other issues showed up—no cysts or ejaculatory duct blockages, which in most cases are key things to keep an eye on [5][7]. All in all, this kind of deep dive is crucial for figuring out exactly what’s going on, so we can better decide on the right treatment path.
Surgical Technique:
General anesthesia was first administered, and the patient was set up in the lithotomy position—everything arranged from the get-go. In a bid to boost clarity and accuracy during the procedure, the team fired up a high-resolution laparoscopic stack, a nod to the leaps made in minimally invasive methods [7]. Next, using an open approach, a 5mm port was inserted right through the intraumbilical area; then, carbon dioxide was introduced to create a pneumoperitoneum at a pressure of about 15 mmHg. For direct sight, two more 5-mm ports popped in the suprapubic region, which, along with a steep Trendelenburg tilt, gently shifted the bowel aside to open up the pelvic space. In most cases, this reorientation helps a lot. Before diving into the main intervention, the surgical team carefully identified the vas deferens and seminal vesicles—no detail was too small. With a pair of laparoscopic scissors in hand, an incision was made over the peritoneum covering the left seminal vesicle, enabling a careful dissection from surrounding tissues; sometimes the steps feel almost like an unscripted dance. During that exploration, a stone was palpably felt within the seminal vesicle, so a small, deliberate incision was crafted directly above the stone to allow for its removal. The stone was then grasped and extracted with measured care, meant to avoid undue trauma to the nearby tissues (Figure 3).
Figure 3: Postoperative picture from the Stone.
After the removal, the seminal vesicle was closed using a 4-0 absorbable suture applied in a continuous running stitch—a technique generally recognized as best practice [8]. A meticulous check then confirmed satisfactory hemostasis; the pneumoperitoneum was gradually let out (a process that can sometimes feel a bit uneven), and finally, all incisions were sealed and a sterile dressing applied to guard the surgical area.
Postoperative Course:
The patient handled the procedure quite well and was discharged on post-op day two – they were sent home with a prescription for oral pain meds to keep discomfort at bay. Three months later, at a follow-up visit, it became pretty clear that things had improved; indeed, both the blood in the semen and the pain during ejaculation had entirely disappeared. This result, in most cases, strongly suggests that the stone was removed successfully and fits with earlier studies noting positive post-surgery outcomes in similar instances [5]. Additionally, the value of solid post-surgical care is underscored by literature which shows that, with effective pain control and timely follow-ups, patient recovery tends to be much smoother [8].
Discussion
Stones in the seminal vesicles are rare and, frankly, a bit of a headache for clinicians. There's still plenty of debate about how best to handle them – treatment decisions usually hinge on factors like stone size, symptom intensity, and patient preference. A laparoscopic seminal vesiculectomy has come up as a safe, effective option; it uses a minimally invasive approach with zoomed-in views and fine dissection that cuts down on risks during the operation [9].
Obstructions in the male genital tract can pop up from a mix of causes: infections, earlier inguinal or scrotal surgeries, or even a congenital lack of the vas deferens on both sides [10]. In cases of obstructive azoospermia, microsurgical reconstruction is often needed to restore fertility [11]. Also, laparoscopy has really changed the game in handling many urological issues – patients often enjoy less pain after surgery, shorter hospital stays, and even a better cosmetic outcome than with open surgery. For removing seminal vesicle stones, the laparoscopic method kicks off by creating a pneumoperitoneum and carefully positioning trocars to access the pelvic space; this lets surgeons disassemble and extract the stone while keeping nearby tissues mostly undisturbed and lessening the chance of any accidental injury [12]. Detailed post-surgery check-ups – which include semen analyses and imaging studies – are key to spotting potential stone recurrence, infections, or other complications. Observations on fertility following these interventions generally point to promising outcomes for many patients [13]. It’s important to note, albeit with a few quirks in technique sometimes, that using top-notch microsurgical skills is crucial during a vasovasostomy after a failed attempt, underscoring just how complex these obstruction cases can be [14]. Interestingly, the literature touches only lightly on cases with duplicated ureteral pathways and their effects on urological presentations, which really stresses the need for more research and fresh surgical ideas [5][8].
Conflicts of Interest
The authors declare that they have no conflicts of interests.
References
1. Al-Naimi, A., et al. "Granulomatous and xanthogranulomatous prostatitis: a case report." Urology Case Reports 40 (2022): 101887.
2. Ocal, Osman, et al. "Imaging findings of congenital anomalies of seminal vesicles." Polish Journal of Radiology 84 (2019): 25-31.
3. Ahmed, Omar Ahmed Fahmy. Comparison of the functional and oncological outcomes of the sub-trigonal versus conventional robotic radical prostatectomy for prostate
cancer. Diss. Universität Tübingen, 2020.
4. Kumar, Santosh, and Shivanshu Singh. "Genitourinary hydatid disease." Current Topics in Echinococcosis. IntechOpen, 2015.
5. Venugopalan, A. V., et al. "Ureteral duplication with intrasinusal ureteral junction and epididymal ureteric ectopia." Indian Journal of Case Reports 4.1 (2018): 17-19.
6. Salem, Hesham, et al. "A systematic review of the applications of Expert Systems (ES) and machine learning (ML) in clinical urology." BMC Medical Informatics and Decision Making 21 (2021): 1-36.
7. Kumar, Santosh, and Shivanshu Singh. "Genitourinary hydatid disease." Current Topics in Echinococcosis. IntechOpen, 2015.
8. Choi, Kyung Hwa, et al. "Laparoendoscopic single-site surgeries: a single-center experience of 171 consecutive cases." Korean Journal of Urology 52.1 (2011): 31-38.
9. Inamullah, Syed Muhammad Ali, et al. Management of Common Bile Duct Stones: A Comprehensive Review. Biomedical Sciences. Vol. 6, No. 4, 2020, pp. 102-110. doi: 10.11648/j.bs.20200604.15
10. Shah, Shrenik J., et al. "Seminal vesicle sparing laparoscopic radical prostatectomy using a low-energy source: Better continence and potency." Indian Journal of Urology
25.2 (2009): 199-202.
11. Dohle, G. R., et al. "Surgical sperm retrieval and intracytoplasmic sperm injection as treatment of obstructive azoospermia." Human reproduction (Oxford, England) 13.3 (1998): 620-623.
12. Marmar, Joel L. "Techniques for microsurgical reconstruction of obstructive azoospermia." Indian Journal of Urology 27.1 (2011): 86-91.
13. Liu, Hanchao, et al. "Microsurgical Varicocelectomy: Experience of Our Sub?Subinguinal Approach and Review of the Literature." Andrologia 2023.1 (2023): 9937114.
14. Flati, Giancarlo, et al. "Improvement in the fertility rate after placement of microsurgical shunts in men with recurrent varicocele." Fertility and sterility 82.6 (2004): 1527-1531.
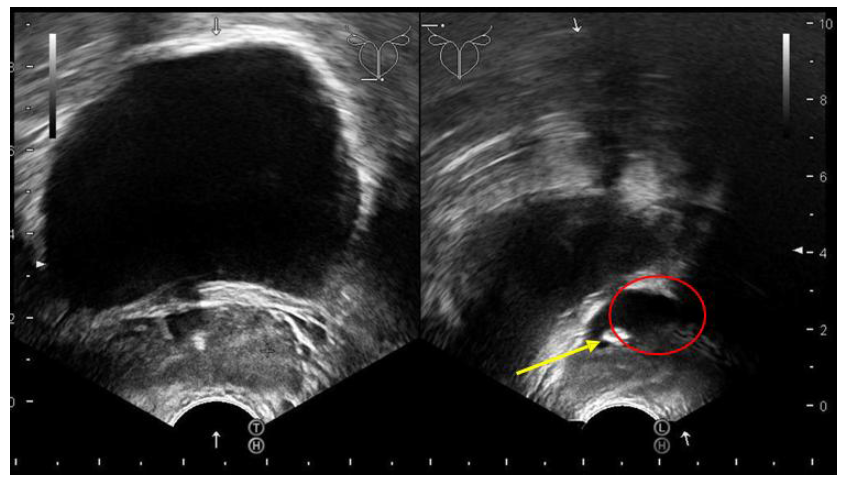
Figure 1
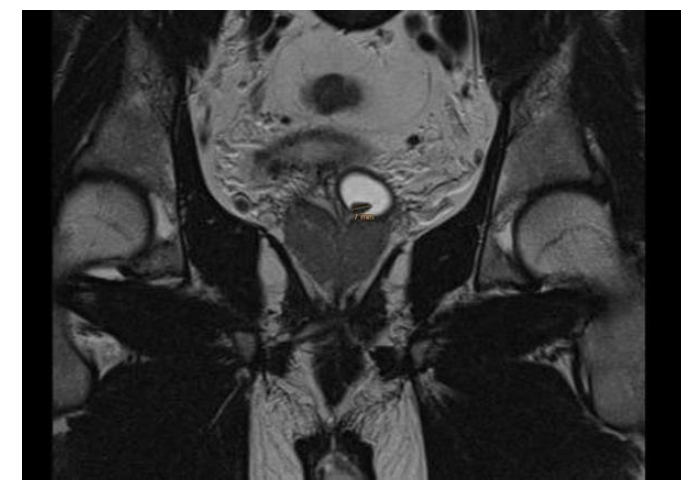
Figure 2
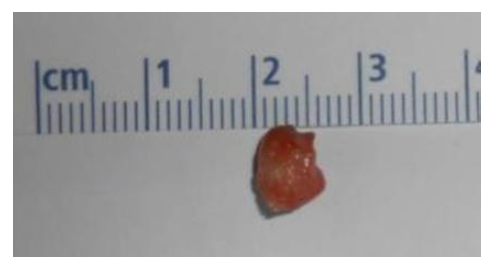
Figure 3
