Functional and Radiological Outcome of Low profile, Fragment Specific anatomical fixation of tri malleolar Ankle fractures
Functional and Radiological Outcome of Low profile, Fragment Specific anatomical fixation of tri malleolar Ankle fractures
A.Bilal*, N.Fitzpatrick1, R.Dahiya2, U.Nath3, T. Balakrishnan4, A.Pillai5
1,2,3,4,5. Wythenshawe Hospital Manchester foundation Trust, United Kingdom.
*Correspondence to: A. Bilal, Wythenshawe Hospital Manchester foundation Trust, United Kingdom.
Copyright
© 2025 A. Bilal is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 23 Apr 2025
Published: 02 May 2025
Abstract:
Tri-malleolar fracture commonly results from rotational injuries of the ankle. Understanding and treatment of these fractures has changed and keep evolving over the last decade. We looked at outcome of Low profile, anatomically contoured fragment specific fixation implantation in these complex fractures.
Methods
We prospectively analysed patients admitted with tri malleolar ankle fractures from October 2021- March 2023. Fractures were classified using CT imaging and fragment specific implant (VolitionTM) were used to fix the fractures. These patients were followed up for functional and radiological assessment.
Results
Twenty-nine skeletally mature patients were identified with tri malleolus fracture needing surgical fixation. At final follow up average MOXFQ index was 27.1(SD 19.7) and foot and ankle disability index (FADI) score were 83.1(SD 18.4) All fractures achieved radiological union but one with average time to radiological union 7.7 (5-12) weeks.
Conclusion.
Early results of fragment specific fixation of trimalleolar fractures show promising functional and radiographic outcome and less need for implant removal.
Key Words
Tri malleolar ankle fracture, fragment specific fixation. Syndesmosis Stability. Posterior inferior tibiofibular ligament stability (PITFL)
Functional and Radiological Outcome of Low profile, Fragment Specific anatomical fixation of tri malleolar Ankle fractures
Introduction
The ankle is a complex joint that is stabilized by several ligaments. These ligaments play a crucial role in ankle’s stability.
Ankle fractures are quite common and account for up to 10% of all bone injuries1,2. Females generally have an increased incidence during their life, the peak incidence of trimalleolar fractures is in the age from 60 to 69 years, becoming the second most common ankle fracture type in this age group3,4.The term trimalleolar fractures was first used Henderson5 in 1932 defined the posterior malleolus as “the anatomic prominence formed by the posterior inferior margin of the articulating surface of the tibia” although Cooper first described the posterior malleolus fracture in 18226. Approximately 44%-50% of all ankle fractures involve the posterior malleolus7,8,9. The posterior malleolar fractures with associated tibial shaft fractures, the incidence of which is 1%-25%10,11The isolated posterior malleolus fractures (Volkmann’s fragment), which are rare with an estimated incidence of 0.5%-1%;9,10,11,
Posterior malleoli contribute to congruity of ankle joint as well as of its stability through its ligamentous attachment. These factors are considered in the management of trimalleolar fractures.
The Posterior inferior tibiofibular ligament (PITFL) originates from the posterior malleolus and runs obliquely distally to its insertion on the posterior fibula. It is composed of a superficial component and a deep component12. PITFL contribute 42% of syndesmotic stability which get compromised when posterior malleolus fractured13.
Management of bimalleolar fracture is quite standard however when it comes to trimalleolar fracture, management of posterior malleolar fragment has notable variability in surgeon’s practice. Access to the advance imaging helps better understanding of fracture’s configuration and planning (Fig1). Different approaches and techniques have been described to address these fractures. In this Study we looked at these fractures treated with fragment specific fixation and reported functional and radiological outcome.
Fig 1 Radiographs and CT scan demonstrating different patterns of trimalleolar fractures.
Methods
All patients presented to our department with trimalleolar ankle fractures from October 2021-March 2023 were included in the study. We excluded the patients from study who were under 18 years of age, does not require posterior malleolus fixation or need fixation method other than plate osteosynthesis. On presentation trimalleolar fractures were identified on Anterior-posterior and lateral radiographs. Patient presented with subluxation or dislocation of ankle needing manipulation were treated by the on-call team Post reduction Splinting (Back slab) was applied and radiographs were obtained to assess the reduction. Subsequently computed tomography (CT) was acquired with coronal, sagittal, axial planes, and 3D reconstruction. The fracture fragments were evaluated using Mason & Molloy classification14 and divided into subtypes 1, 2a, 2b and 3 fractures (Fig 2). Definitive fixation was delayed until the soft tissue settles. If concern with soft tissue and unstable fracture not able to maintain the position in back slab, temporary external fixation was applied until soft tissue settles. Osteosynthesis using fragment specific implant (VolitionTM) and relevant surgical approach was performed. Post operatively these patients were followed in outpatient department at 2, 6,12,26 weeks. They were clinically assessed for any pain, stiffness, infection, nerve damage, CRPS metalwork irritation or failure, and clinical union Functional assessment was carried out using The Manchester-Oxford Foot Questionnaire (MOXFQ) and Foot and ankle disability index (FADI). Anterior -posterior, lateral and mortise radiographs were taken to assess the fixation, adequacy of reduction and radiological union.
Fig2. Axial CT scan showing different types of trimalleolar fractures based on Mason and Molly Classification 36
Results
We analysed 29 patients with tri malleolus fracture who underwent surgical fixation. Out of which there were 12 Males and 17 females with mean age of 51 years (30-76). Most common mechanism was twisting injury to the ankle, involving predominantly the right side (22) compared to left (7). Among subtypes of trimalleolar fractures there were Fifteen(2a), Seven (2b), seven (3) treated with relevant fragment specific plates. One patient with background of Type 2 DM had superficial wound infection settled with one week of oral of antibiotics. None of patients had nerve injury, deep infection, CRPS, there was no implant failure, impingement or loss of fixation needs removing. At final follow up average MOXFQ index was 27.1(SD 19.7) and foot and ankle disability index (FADI) score were 83.1(SD 18.4). All fractures achieved radiological union but one, where the medial malleolus fracture component fixed with cannulated screws remained as asymptomatic fibrous union. Average time for radiological union was 7.7 (5-16) weeks.
Patient Characteristics (N= 29)
|
Age (Years) |
51 (30-76) |
|
Sex Male Female |
12 17 |
|
Fracture side Right Left |
22 7 |
|
Fracture Type 1 2a 2b 3 |
0 15 7 7 |
Table 1 showing Patient and fracture characteristic.
|
|
MOXFQ |
FADI |
|||||
|
|
Pain |
Walking / Standing |
Social Interaction |
MOXFQ-Index |
FADI Activity Subscale |
FADI Pain Subscale |
Total FADI Score |
|
Average |
6.1 |
8.6 |
2.7 |
27.1 |
69.9 |
13.2 |
83.1 |
|
Min |
0 |
0 |
0 |
3 |
25 |
5 |
30 |
|
Max |
17 |
25 |
12 |
81 |
88 |
16 |
103 |
|
SD |
3.9 |
7.8 |
3.0 |
19.7 |
16.7 |
2.5 |
18.4 |
Table 2– PROMS Scoring at Final Follow up (MOXFQ, FADI)
|
Outcome Measure |
No. Complete Datasets |
Frequency |
[%] |
|
Clinical Union |
29 |
29 |
100% |
|
Radiological Union |
29 |
28 |
96% |
|
Malunion |
29 |
0 |
0% |
|
Non- Union |
29 |
1 |
3.4% |
|
Implant Fracture |
29 |
0 |
0% |
|
Implant Loosening / Loss of Fixation |
29 |
0 |
0% |
|
Superficial Infection |
29 |
1 |
3.4% |
|
Deep Infection |
29 |
0 |
0% |
|
Nerve Injury |
29 |
0 |
0% |
|
Thrombosis |
29 |
0 |
0% |
|
Wound Problems |
29 |
1 |
3.4% |
|
CRPS |
29 |
0 |
0% |
|
Hardware Removal |
29 |
0 |
0% |
|
Time to Union |
28 |
7.7 (5-16) Weeks |
|
Table 3 Clinical outcome and complication
Discussion
Over the last few years there is lot of interest and debate on the management of trimalleolar fracture and techniques to address the posterior component of these complex injuries. These fractures are often under rated on plain radiographs however, increased availability of computed tomography (CT) scans has heightened the recognition and change the management15.
Ankle fractures with Posterior malleolus are considered poor prognostic factor when comparing the outcome of ankle fractures16. As PITFL plays significant role in syndesmotic stability which is disrupted in these injuries and this syndesmotic instability could be responsible for unfavourable outcome13. Inadequate treatment of these fracture may cause severe complications such as checkrein deformities17,18,19,20. Studies has shown there is significant clinical difference between trimalleolar fractures compare to their counterparts’ unimalleolar fractures 21 and marked improvement in clinical outcomes for patients who underwent fixation for posterior malleolus fractures, in contrast to those treated non- operatively22. Different classification systems have described the posterior fragment of ankle fractures. Most Renowned were proposed by Haraguchi et al23. followed by Bartonicek et al24. and Mason and Molloy (M&M)14. We used M&M classification for all of our trimalleolar fractures and planned the management based on fracture configuration.
Various approaches and methods for fixation of posterior malleolus have been described in literature25,26. The classical teaching has been to fix these fractures with indirect reduction and anterior to posterior (A to P) screws27,28,29 This may be because previously the indications for fixation of these fractures were if the fracture involved more than 25 to 33% of articular surface.30,31 Although this provide a favourable environment for fixation of these fractures through A to P screw. However, this technique has its own limitations which need attention when applying this method of fixation. Comminuted and intraarticular impacted (die Punch) fracture fixations are not eligible by this approach. This technique may not allow adequate reduction and difficult to achieve compression at fracture site as a larger fragment is being fixed against a smaller fragment. Hence, it makes the construct less stable. Also, smaller Fragments are difficult to fix with this technique, as for bigger screws all threads may not cross the fracture site and smaller screws do not provide adequate compression32.
Recent studies show Anatomical and functional outcome of direct approach are superior to indirect approach33.
In literature Fragment specific fixation of certain distal radius fractures is well described particularly when monoblock fixations are inadequate34,35. In recent years these implants gaining attention and popularity for certain types of fractures.
Fragment-specific fixation is usually indicated in cases where stabilization of specific articular segments is required However there is not much published and lack of evidence on fragment specific fixation of trimalleolar fractures. We reported our experience and early results of fixing these fractures with direct approach using fragment specific implant. (Fig3)
Fig 3 Radiographs showing different type of fixation with fragment specific plates (Volition TM ).
The Patient position and surgical approach to address these fractures was guided by fracture configuration and surgeon’s preference. Wherever possible we addressed the posterior malleolus fracture first and used the relative fragment specific implant. It allows the better radiographic visualisation of reduction and no interference from metalwork. This is followed by lateral malleolus fixation when fixing 2a fractures but in type 2b fractures, medial malleolus fracture was fixed before the lateral fragment stabilisation and in Type 3 sequence of fixation was dependent on type surgical approach. (Fig 4)
Fig 4 Showing Pre-op and post op Imaging of different trimalleolar fractures and their fixation using fragment specific Plates.
The fragment specific implants are designed and anatomically contoured to address each fragment of trimalleolar fracture separately. When applied and seated appropriately it also provide extra assurance of anatomical reduction in addiction radiological assessment. In medial malleolus vertical shear fractures or when fractures exit higher up posteromedially needing plate osteosynthesis these implants are particularly helpful to avoid metalwork prominence due to low profile and anatomical contour. In Posterior malleolus fractures when deploy properly they cause less irritation to soft tissue and tendons. The hardware related issue is one of the main causes for reoperation in these fractures. Jeyaseelan et al22 reported 10% increase risk of complications and a two-fold increase in re-operation rates, primarily attributed to hardware-related issues. Potentially these complications can be avoided with the judicious and appropriate use of these low profile, anatomical contoured fragment specific implants.
We acknowledge few limitations to this study. Firstly, the study involves only twenty-nine patients but can be appreciated, fragment specific fixation for trimalleolar fractures is not routinely used though its catching interest. Secondly, these are early outcome, and functional scores can change over time, but some functional outcome can be justified at this stage e.g hardware prominence, irritation or failure needing removal of metalwork which is one common cause of reoperation.
Conclusion
Ankle fractures are a very common injuries Fragment-specific fixation can be utilized in cases in which stabilization of specific articular segments is required. Although these techniques can be technically demanding and require steep learning curve, fragment-specific plates are usually adjuncts to allow the surgeon to expand the armamentarium in the management of complex trimalleolar fracture patterns. They complement but not the alternative to the anatomical reductions and favourable outcomes. Our study demonstrated promising early results with fragment specific low profile anatomical fixation, and it will be fascinating to see long term results. A comparative study of similar cohort of patients with and without fragment specific fixation will be captivating.
'Declaration
No conflict of interest and no Generative AI and AI-assisted technologies used in the writing process.
References
1. Heckman Jd, mckee m, mcQueen mm, ricci w, tornetta p Rockwood and Green’s fractures in adults. Philadelphia, III : Lippincott Williams & Wilkins, 2014.2.
2. Elsoe R, Ostgaard SE, Larsen P. Population-based epidemiology of 9767 ankle fractures. Foot Ankle Surg. 2018 Feb;24(1):34-39. doi: 10.1016/j.fas.2016.11.002. Epub 2016 Nov 18. PMID: 29413771.
3. Juto H, Nilsson H, Morberg P. Epidemiology of Adult Ankle Fractures: 1756 cases identified in Norrbotten County during 2009-2013 and classified according to AO/OTA. BMC Musculoskelet Disord. 2018 Dec 13;19(1):441. doi: 10.1186/s12891-018-2326-x. PMID: 30545314; PMCID: PMC6293653.
4. 4 Elsoe R, Ostgaard SE, Larsen P. Population-based epidemiology of 9767 ankle fractures. Foot Ankle Surg. 2018 Feb;24(1):34-39. doi: 10.1016/j.fas.2016.11.002. Epub 2016 Nov 18. PMID: 29413771
5. Henderson MS: Trimalleolar fracture of the ankle. Surg Clin North Am 1932;12: 864.
6. Cooper AP: A Treatise on Dislocations, and on Fractures of the Joints. London, UK, Longman, Hurst, Reese, Orme and Brown, E. Cox and Son, 1822, pp 238-357.
7. Switaj, Paul J., et al. ‘Evaluation of Posterior Malleolar Fractures and the Posterior Pilon Variant in Operatively Treated Ankle Fractures’. Foot & Ankle International, vol. 35, no. 9, Sept. 2014, pp. 886–95. DOI.org (Crossref), https://doi.org/10.1177/1071100714537630.
8. 8. Court-Brown CM, McBirnie J, Wilson G. Adult ankle fractures--an increasing problem? Acta Orthop Scand. 1998 Feb;69(1):43-7. doi: 10.3109/17453679809002355. PMID: 9524517.
9. Koval KJ, Lurie J, Zhou W, Sparks MB, Cantu RV, Sporer SM, Weinstein J. Ankle fractures in the elderly: what you get depends on where you live and who you see. J Orthop Trauma. 2005 Oct;19(9):635-9. doi: 10.1097/01.bot.0000177105.53708.a9. PMID: 16247309.
10. . Kukkonen J, Heikkilä JT, Kyyrönen T, Mattila K, Gullichsen E. Posterior malleolar fracture is often associated with spiral tibial diaphyseal fracture: a retrospective study. J Trauma 2006; 60: 1058-1060.
11. Boraiah S, Gardner MJ, Helfet DL, Lorich DG. High association of posterior malleolus fractures with spiral distal tibial fractures. Clin Orthop Relat Res 2008; 466: 1692-1698.
12. Sarrafian SK, Kelikian AS: Syndesmology, in Kelikian AS, Sarrafian S, eds: Sarrafian's Anatomy of the Foot and Ankle: Descriptive, Topographic, Functional, ed 3. Philadelphia, PA, Lippincott Williams & Wilkins, 2011, pp 163-166.
13. Ogilvie-Harris DJ, Reed SC, Hedman TP. Disruption of the ankle syndesmosis: biomechanical study of the ligamentous restraints. Arthroscopy. 1994 Oct;10(5):558-60. doi: 10.1016/s0749-8063(05)80014-3. PMID: 7999167.
14. Mason LW, Marlow WJ, Widnall J, Molloy AP. Pathoanatomy and Associated Injuries of Posterior Malleolus Fracture of the Ankle. Foot Ankle Int. 2017 Nov;38(11):1229-1235. doi: 10.1177/1071100717719533. Epub 2017 Jul 31. PMID: 28758439.
15. Ferries JS, DeCoster TA, Firoozbakhsh KK, Garcia JF, Miller RA. Plain radiographic interpretation in trimalleolar ankle fractures poorly assesses posterior fragment size. J Orthop Trauma. 1994 Aug;8(4):328-31. doi: 10.1097/00005131-199408000-00009. PMID: 7965295.
16. Tejwani NC, Pahk B, Egol KA. Effect of posterior malleolus fracture on outcome after unstable ankle fracture. J Trauma. 2010 Sep;69(3):666-9. doi: 10.1097/TA.0b013e3181e4f81e. PMID: 20838137.
17. Beckenkamp PR, Lin CW, Engelen L, Moseley AM. Reduced physical activity in people following ankle fractures: a longitudinal study. J Orthop Sports Phys Ther. 2016;46(4):235–42
18. Beckenkamp PR, Lin CW, Chagpar S, Herbert RD, van der Ploeg HP, Moseley AM. Prognosis of physical function following ankle fracture: a systematic review with meta-analysis. J Orthop Sports Phys Ther. 2014;44(11):841–51.
19. Murray AM, McDonald SE, Archbold P, Crealey GE. Cost description of inpatient treatment for ankle fracture. Injury. 2011;42(11):1226–9.
20. Polichetti C, Greco T, Inverso M, Maccauro G, Forconi F, Perisano C. Retro-Malleolar Z-Plasty of Flexor Hallucis Longus Tendon in Post-Traumatic Checkrein Deformity: A Case Series and Literature Review. Medicina (Kaunas). 2022;58(8).
21. Mason LW, Kaye A, Widnall J, Redfern J, Molloy A. Posterior Malleolar Ankle Fractures: An Effort at Improving Outcomes. JB JS Open Access. 2019 Jun 7;4(2):e0058. doi: 10.2106/JBJS.OA.18.00058. PMID: 31334465; PMCID: PMC6613847.
22. Jeyaseelan L, Bua N, Parker L, Sohrabi C, Trockels A, Vris A, Heidari N, Malagelada F. Outcomes of posterior malleolar fixation in ankle fractures in a major trauma centre. Injury. 2021 Apr;52(4):1023-1027. doi: 10.1016/j.injury.2020.12.006. Epub 2020 Dec 24. PMID: 33376016.
23. Haraguchi N, Haruyama H, Toga H, Kato F. Pathoanatomy of posterior malleolar fractures of the ankle. J Bone Joint Surg Am. 2006 May;88(5):1085-92. doi: 10.2106/JBJS.E.00856. Erratum in: J Bone Joint Surg Am. 2006 Aug;88(8):1835. PMID: 16651584.
24. Bartoní?ek J, Rammelt S, Kostlivý K, Van??ek V, Klika D, Trešl I. Anatomy and classification of the posterior tibial fragment in ankle fractures. Arch Orthop Trauma Surg. 2015 Apr;135(4):505-16. doi: 10.1007/s00402-015-2171-4. Epub 2015 Feb 24. PMID: 25708027.
25. Odak S, Ahluwalia R, Unnikrishnan P, Hennessy M, Platt S. Management of Posterior Malleolar Fractures: A Systematic Review. J Foot Ankle Surg. 2016 Jan-Feb;55(1):140-5. doi: 10.1053/j.jfas.2015.04.001. Epub 2015 Jun 19. PMID: 26100091.
26. Fernández-Rojas E, Herrera-Pérez M, Vilá-Rico J. Posterior malleolar fractures: Indications and surgical approaches. Rev Esp Cir Ortop Traumatol. 2023 Mar-Apr;67(2):160-169. English, Spanish. doi: 10.1016/j.recot.2022.10.019. Epub 2022 Nov 9. PMID: 36371071.
27. Gardner MJ, Brodsky A, Briggs SM, et al. Fixation of posterior malleolar fractures provides greater syndesmotic stability. Clin Orthop Relat Res 2006; 447: 165–171.
28. Miller AN, Carroll EA, Parker RJ, et al. Posterior malleolar stabilization of syndesmotic injuries is equivalent to screw fixation. Clin Orthop Relat Res 2010; 468: 1129–1135.
29. Verhage S, van der Zwaal P, Bronkhorst M, et al. Medium-sized posterior fragments in AO Weber-B fractures, does open reduction and fixation improve outcome? The POSTFIX-trial protocol, a multicenter randomized clinical trial. BMC Musculoskelet Disord 2017; 18: 94.
30. De Vries JS, Wijgman AJ, Sierevelt IN, et al. Long-term results of ankle fractures with a posterior malleolar fragment. J Foot Ankle Surg 2005; 44: 211–217.
31. Langenhuijsen JF, Heetveld MJ, Ultee JM, et al. Results of ankle fractures with involvement of the posterior tibial margin. J Trauma 2002; 53: 55–60.
32. Bartoní?ek J, Rammelt S, Tu?ek M. Posterior Malleolar Fractures: Changing Concepts and Recent Developments. Foot Ankle Clin. 2017 Mar;22(1):125-145. doi: 10.1016/j.fcl.2016.09.009. Epub 2016 Dec 20. PMID: 28167058.
33. Shi HF, Xiong J, Chen YX, Wang JF, Qiu XS, Huang J, Gui XY, Wen SY, Wang YH. Comparison of the direct and indirect reduction techniques during the surgical management of posterior malleolar fractures. BMC Musculoskelet Disord. 2017 Mar 14;18(1):109.
34. Hozack BA, Tosti RJ. Fragment-Specific Fixation in Distal Radius Fractures. Curr Rev Musculoskelet Med. 2019 Jun;12(2):190-197. doi: 10.1007/s12178-019-09538-6. PMID: 30835080; PMCID: PMC6542921.
35. Geissler WB, Clark SM. Fragment-Specific Fixation for Fractures of the Distal Radius. J Wrist Surg. 2016 Mar;5(1):22-30. doi: 10.1055/s-0035-1571186. Epub 2016 Jan 8. PMID: 26855832; PMCID: PMC4742261
36. Mason LW, Kaye A, Widnall J, Redfern J, Molloy A. Posterior Malleolar Ankle Fractures: An Effort at Improving Outcomes. JB JS Open Access. 2019 Jun 7;4(2):e0058. doi: 10.2106/JBJS.OA.18.00058. PMID: 31334465; PMCID: PMC6613847..
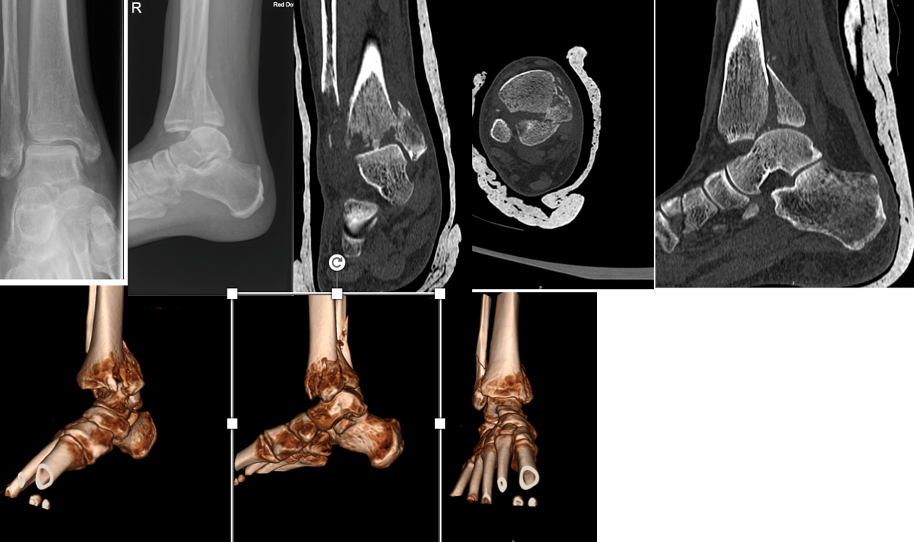
Figure 1
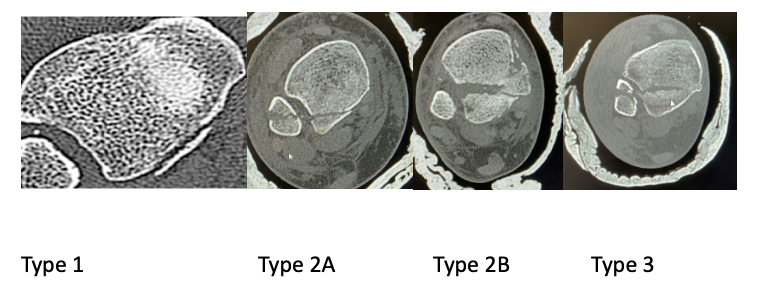
Figure 2
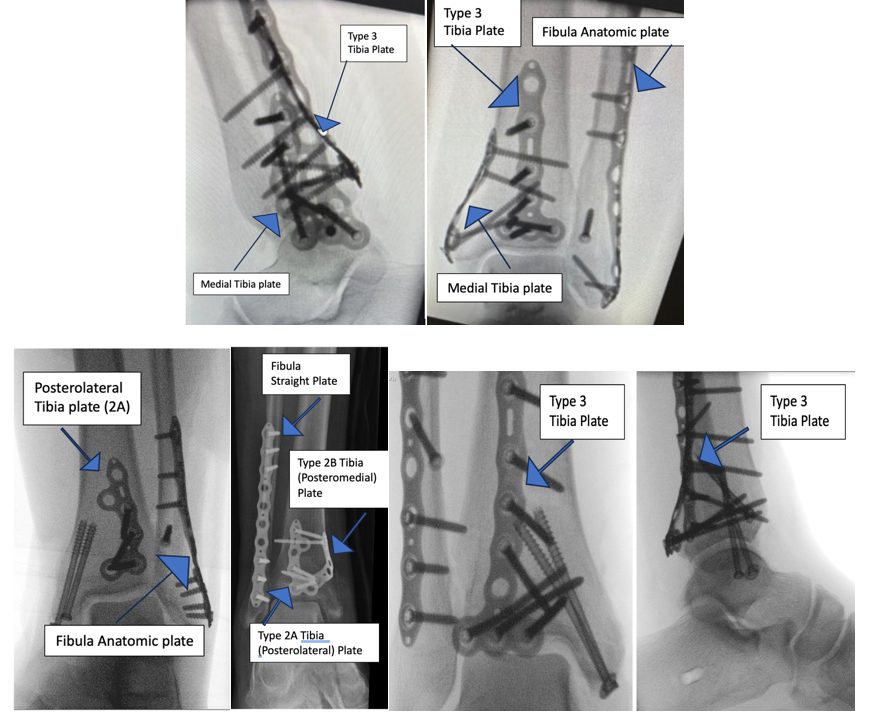
Figure 3
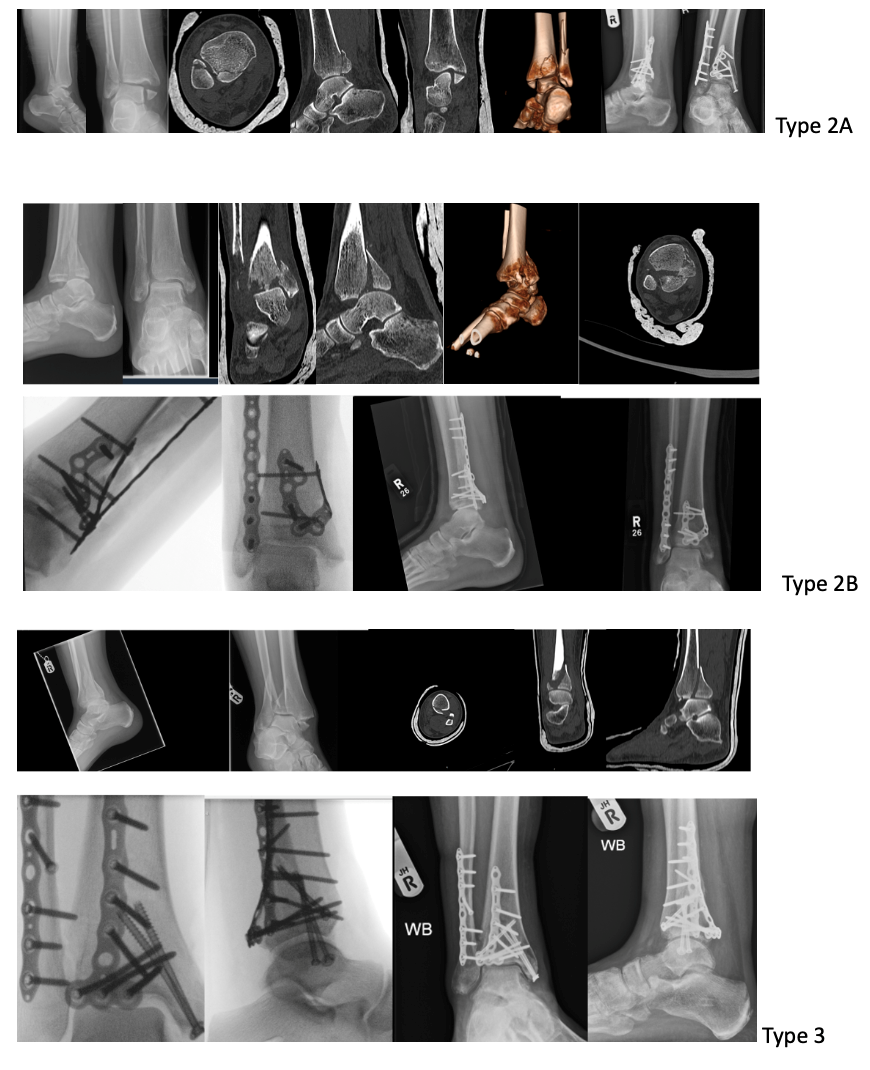
Figure 4
