Cognitive Impairment Following Stroke in Geriatric Patients
Cognitive Impairment Following Stroke in Geriatric Patients
Ibrahim Krenawi *1, Mimoun Azizi 2, Franklin Famdie Simo3, Shady Samy Georgy4, Hassan Belamkadem5
1- Ibrahim Krenawi, Consultant Neurologist, Burjeel Royal Hospital, Al Ain, UAE.
2- Mimoun Azizi, Chief Physician & Managing Chief Physician, Senior Consultant Neurologist & Neurogeriatrician, Klinikverbund Südwest, Sindelfingen, Germany.
3- Franklin Famdie Simo, Chief Physician, Senior Consultant Neurologist & Neurogeriatrician, MEDIAN Frankenpark Klinik, Bad Kissingen, Germany.
4- Shady Samy Georgy, Specialist Neurologist, Burjeel Royal Hospital, Al Ain, UAE.
5- Hassan Belamkadem, Consultant Neurologist, Praxis for Neurology and Psychiatry, Unna, Germany.
*Correspondence to: Ibrahim Krenawi, ORCID: 0009-0007-6850-4749.
Copyright
© 2025 Ibrahim Krenawi, This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 14 July 2025
Published: 19 July 2025
DOI: https://doi.org/10.5281/zenodo.16303165
Abstract
Cognitive impairment following stroke is a common and serious complication in geriatric patients. It has a very adverse impact on quality of life, puts people more at-risk of institutionalization, and 1`- dozen- pretty much destroys their functional recovery. The review discusses the epidemiology, pathophysiology, clinical manifestation, diagnostics, and treatment of post-stroke cognitive impairment (PSCI) among the elderly. The focus is on evidence-based results of meta-analyses and randomized controlled trials. The role of early diagnosis and a combination of pharmacological and non-pharmacological interventions is addressed in future lines of research.
Keywords: Stroke, Cognitive Impairment, Elderly, Post-Stroke Dementia, Neurorehabilitation, Cholinesterase Inhibitors.
Cognitive Impairment Following Stroke in Geriatric Patients
Introduction
Stroke has been cited as among the biggest causes of chronic impairment and death amongst the aging community across the globe. The age of the global population is rising, and at the same time, the number of older patients who experience a stroke is also on the rise, thus contributing to the prevalence of post-stroke complications. Cognitive impairment refers to a decline in a person's mental abilities, including thinking, learning, memory, judgment, and decision-making. It can manifest as problems with memory, concentration, language, or the ability to complete everyday tasks.
Cognitive impairment is one of the most underdiagnosed and influential stroke consequences that takes the form of mild cognitive decline and severe vascular dementia [1]. Post-stroke cognitive impairment (PSCI) impacts a very broad scope of functions including memory, attention, executive function, language, and visuospatial, and comes along with a significant increase in dependency, a decrease in quality of life, and higher mortality rates.
Elderly are rather prone to PSCI because of age-related neurodegenerative alterations, co-morbid vascular risk factors, and less cognitive reserve. It has been shown that a third of the old stroke survivors experience some kind of cognitive dysfunction within a year of suffering the stroke. The disease not only makes rehabilitation complex, but it also has a significant burden on both caregivers and health systems. Although it is common, PSCI is usually not given much consideration when handling an acute stroke.
This review seeks to address the epidemiology, pathophysiological, risk factors, clinical presentation, and evidence-based management of cognitive impairment among patients with stroke who experience impairment in older age, with the focus on early diagnosis as an underlying cause of poor management and outcomes.
Epidemiology
Cognitive disarray is among the most frequently noted consequences of the stroke, especially among the elderly population. In many population-based studies, it has been noted that between 20% and 80% of stroke survivors have some form of cognitive dysfunction, with dependence on the instruments measuring this and the time of assessment [2]. Also, a systematic review conducted by Sachdev et al. (2014) revealed that the risk of dementia in stroke victims is over twofold compared to that of those who have never had a stroke [3]. Patients with 65 years and older have a high risk of post-stroke cognitive impairment development (PSCI), mostly because of age-related neurodegeneration processes, diminished neuroplasticity, and accumulation of vascular risk factors [4].
According to the results of the longitudinal cohort study conducted by Sun et al. (2014), about 36% of elderly stroke survivors developed mild cognitive impairment (MCI), whereas in 16 percent of the cases, the patients entered the phase of vascular dementia within a year of a stroke event [5]. It is significant among those patients who already had a stroke, frequent cerebrovascular occurrences, and patients with a low education level, which favors the theory of decreased cognitive reserve in some individuals [6]. In addition, it has been identified that comorbid illnesses like hypertension, diabetes mellitus, atrial fibrillation, and hyperlipidemia have steadily been revealed as major risk factors of PSCI [7].
It could be explained by the heterogeneity in the prevalence of studies due to the variability in the sample population, stroke subtypes, cognitive screening instruments, and follow-up periods. However, it is well-known across the literature that the risk of clinical outcomes is disproportionately high in geriatric patients both in prevalence and severity, which means that action should be taken early through prevention measures to provide better results in terms of cognition and functionality after a stroke has been incurred [8].
Pathophysiology and Risk Factors
The pathogenesis of the post-stroke cognitive impairment (PSCI) in the elderly remains multifactorial and in the use of a complex of acute vascular lesions, chronic neurodegenerative, and systemic influences risk. The nature and the extent of cognitive deterioration are tightly intertwined with the specifics of cerebral lesion localization and its severity, yet also with the co-morbidities and pre-stroke susceptibilities [9].
Brain Lesions and Strategic Infarcts
Direct effects on neural circuits supporting memory, executive function, and attention can be explained by damage to brain structure caused by stroke, especially the location like hippocampus, thalamus, prefrontal cortex, and also in the temporo-parietal regions [10]. Left hemisphere infarcts are more likely to produce language and verbal memory defects, and right hemisphere infarcts can impair visuospatial processing and attention [11]. Severity is also determined by the size and multiplicity of lesions, as large or multiple infarcts have a strong correlation with greater and sustained cognitive dysfunction [12].
White Matter Disease and Small Vessel Pathology
The SVD in the brain is a factor that influences severe effects because of age-related cognitive decline after a stroke. SVD is recognized as white matter hyperintensities (WMHs), lacunar infarcts, cerebral microbleeds, and a dilatation of perivascular space, which interrupt cortical and subcortical connectivity. Such alterations are typical during old age, and the effect is compounded by stroke, especially in individuals with hypertension and diabetes mellitus [13].
Neuroinflammation and Oxidative Stress
Stroke promotes a series of neuroinflammations encompassing the mobilization of microglia, the secretion of pro-inflammatory cytokines (e.g., IL-1beta, TNF-alpha), and the breakdown of the blood-brain barrier. These mechanisms lead to increased oxidative stress, which induces neuronal apoptosis, loss of synapses, and damage to the white matter, and this is specifically shown in parts that are susceptible to hypoperfusion [14]. They are more intense in old patients because of the immunosenescence and poor recovery ability of the neurorepair.
Amyloid Pathology and Neurodegeneration
There is growing evidence of co-morbidity of vascular and Alzheimer-type pathology among the geriatric recovering stroke patients. Stroke may hasten the development of beta-amyloid plaques, especially among individuals with the APOE ε4 allele, which leads to mixed dementia traits [15]. The interaction favors the model of the two pathologies (dual pathology), according to which cerebrovascular disease and neurodegenerative phenomena coexist, contributing to cognitive decline.
Modifiable Risk Factors
Multiple modifiable risk factors with a significant role in PSCI development and promotion have already been formulated:
* Hypertension: It is also related to ischemic stroke and damage to the white matter.
* Type 2 Diabetes Mellitus: Enhances microvascular damage and neuroinflammation.
* Atrial Fibrillation: Poses huge risks of cardioembolic strokes in the cortical areas.
* Hyperlipidemia: Increases the rate of atherosclerosis and causes repeated strokes.
* Smoking and Physical Inactivity: These two activities correlate with low vascular health and cognitive reserve.
* Low Educational Attainment: Typifies a proxy of lower cognitive resilience following injury.
These risk factors should be addressed during the prevention and management of PSCI in the elderly.
Clinical Presentation and Diagnosis
Recommended Timeframes for Screening
The cognitive impairment after stroke is characterized by a great variety of symptoms, and it is dependent on the nature of the location, size, and quantity of brain lesions. The most common cognitive domains that are affected by them are memory, executive function, attention, language, and visuospatial processing [16]. The patients can be expressed as possibilities of having poor planning and problem solving, processing new information, getting words, or issues of orientation in space. Patients will also exhibit executive dysfunction and delayed recall of memory, especially when the lesion causes impairment in the frontal lobe and the hippocampal areas [17].
Nys and others (2005) have reported that cognitive deficit is identifiable after 1 to 2 weeks after a stroke, and many cases are identified during the subacute stage of rehabilitation (3-6 weeks) [18]. The highest intensity of cognitive dysfunction in most of the patients is registered during the initial three months after the stroke. To some degree or another, a percentage of patients (estimated 20-25% at most) show some or complete cognitive improvement during the first 6 to 12 months, particularly when the rehabilitation process has been active and when the damage is not severe [19]. But in the case of elderly individuals with a high initial level of deficits or low education, or with numerous vascular risk factors, the impairments are likely to be long-standing and may develop into dementia.
Standard Cognitive Assessment Tools
Standardized neuropsychological assessments are essential for the early detection and classification of post-stroke cognitive impairment (PSCI).
The Mini-Mental State Examination (MMSE) and the Montreal Cognitive Assessment (MoCA) are two of the most frequently employed tools for identifying cognitive dysfunction. As much as the MMSE is popular, it has reduced sensitivity related to the detection of mild cognitive impairment. MoCA is thus recommended to be utilized in post-stroke groups because it has a wider measure of executive dysfunction and visuospatial skill [20].
* MoCA: A score below 26/30 is indicative of cognitive impairment.
* MMSE: A score below 24/30 suggests moderate-to-severe cognitive dysfunction.
DemTect (Dementia Detection Test) is another valuable tool, especially for detecting early cognitive decline. It includes five tasks assessing verbal memory, word fluency, cognitive flexibility, and number transcoding. Its scoring is age-adjusted, making it suitable for elderly stroke survivors. Studies have shown that DemTect is more sensitive than MMSE in identifying mild cognitive impairment, particularly in the early stages, and it is easy to administer in outpatient and community settings.
The Clock Drawing Test (CDT) is a rapid, non-verbal tool that evaluates visuospatial abilities, executive function, and conceptualization. It is especially valuable in detecting cognitive deficits related to right hemispheric strokes and frontal lobe dysfunction. Due to its ease of administration and diagnostic utility, CDT is frequently used as a supplementary tool alongside MoCA or DemTect in comprehensive cognitive assessments.
These tools evaluate memory, attention, language, executive function, and visuospatial skills. For optimal results, assessments should be conducted in a quiet, controlled environment and interpreted by trained professionals.
Neuroimaging and Advanced Techniques
Neuroimaging plays a crucial role in terms of determining the nature of the lesions and vascular peculiarities associated with cognitive deficiency. The modality of choice of imaging studies is MRI because it is sensitive in the detection of cortical and subcortical infarcts, white matter hyperintensities, and hippocampal atrophy [21].
* Structural MRI: Reveals strategic infarcts (e.g., thalamus, medial temporal lobe).
* Diffusion Tensor Imaging (DTI): Assesses white matter integrity and tract disruption.
* Functional MRI (fMRI): Looks at the connection between brain networks, particularly during research.
Certainly, in other situations, the CT scan can be employed acutely; however, it is less sensitive to changes occurring in the brain with regard to cognition.
Differential Diagnosis Considerations
Neuropsychiatric conditions that overlap with cognitive symptoms following stroke are post-stroke depression, delirium, aphasia, or preexisting dementia. Multifactorial clinical assessment needs to be implemented, including psychiatric assessment, premorbid cognitive state assessment, and the elimination of metabolic or medication-related etiology.
It is noteworthy that an interdisciplinary approach involving neurologists, psychiatrists, and neuropsychologists is suggested before an accurate diagnosis and the development of an effective and individual care plan is possible.
Prognosis and Impact on Quality of Life
The elderly population has a significant influence on post-stroke cognitive impairment (PSCI) on the long-term functional costs, independence, and quality of life. The prognosis requires severity of initial impairment, comorbidities, ability to receive rehabilitation, and the social support system. There are population-based studies that indicate that about 20-30% of the geriatric patients with mild cognitive impairment exhibit measurable recovery about 6 to 12 months after stroke, especially when early cognitive rehabilitation is implemented [22]. Still, over half of the patients persist in deficits, and 25-30% of patients develop dementia after 2-5 years [23].
Difficulty in cognition is a major cause of disruption to the way a patient goes about their instrumental activities of daily living (IADLs), like moving about in an independent way, managing finances, managing medicine, among others. Consequently, patients are prone to be reliant on caregivers, get institutionalized, or face frequent hospitalization. Lastly, the risk of institutionalization among stroke survivors with cognitive impairment was twice as common as that of cognitively normal stroke survivors, as well as mortality in the former group was one and a half times greater than in the latter in a longitudinal study by Allan et al. (2011) [24].
Both memory and attention deficits, as well as related emotional disturbance (post-stroke depression, apathy, anxiety), have a strong impact on quality of life (QoL). The comorbidity only makes such conditions even less motivating and participating socially, resulting in isolation and reduced compliance with the rehabilitation process. There is also the perception of higher instances of emotional strain, burnout, and financial pressure in taking care of cognitively impaired stroke patients in spouses and caregivers, mostly due to judgment-related impairments, personality alterations, or behavior dysregulation.
In spite of this, early multidisciplinary intervention, caregiver education, and supportive community-based intervention lead to improved cognitive outcomes and improved the quality of life of geriatric stroke survivors. To maintain the acquired success of the primary rehabilitation as well as the avoidance of secondary complications, psychosocial care and long-term monitoring are critical [25].
Management Strategies
The treatment of post-stroke cognitive impairment (PSCI) in geriatric patients should be complex, where non-pharmacological treatment, pharmacological drug treatment and lifelong rehabilitation measures are combined. Quick start of treatment is desirable, because most of the neuroplastic recovery is seen in the first 3-6 months of a stroke, with losses in returns following it [26].
Non-Pharmacological Interventions
Cognitive Rehabilitation Therapy
The non-drug management of PSCI rests on cognitive rehabilitation. Memory-based, attention-based, and executive-based structured interventions have improved significantly with small cognitive gains. Loetscher and Lincoln ( 2013) have conducted a Cochrane review, which revealed that cognitive training has an important benefit in stroke patients on their executive functions and attention, especially when initiated during the first 3 months after the stroke [27].
Interventions may include:
• Cognitive exercises done on paper or on a computer
• Goal Management Training (GMT)
• Attention Process Training (APT)
• Strategies for memory loss (e.g., note-taking, reminders)
Such therapies work best when they are administered 2-3 times a week, resulting in an 8-12 week therapy with optimum integration into the entire multidisciplinary rehabilitation scheme.
Physical Exercise and Lifestyle Modification
During aerobic exercise (e.g., walking, cycling), neurocognitive advantages have been proven by means of enhancing brain perfusion and fostering neurogenesis. A meta-analysis study revealed that the group of elderly stroke survivors who participated in moderate-intensity exercise performed 3 times a week within a 30-minute session exhibited higher global cognitive scores in comparison to sedentary participants [28].
Lifestyle modifications such as:
• Stopping smoking
• Mediterranean diet
• Blood pressure control
• Glycemic management
They are adequately capable of slowing down the rate of cognitive decline and will suppress the recurrent strokes.
Psychosocial Support/Education
Patient and caregiver education about PSCI plays a fundamental role in enhancing adherence and safety as well as quality of life. Anxiety can also be alleviated with the help of psychosocial support and structured routines, and boosting cognitive functioning, particularly in the case of co-morbid depression or apathy [29].
Pharmacological Interventions
No pharmacological approach to PSCI has been universally accepted, although this disorder has been studied with a variety of drug classes that have the potential of providing cognitive advantages to stroke survivors.
Cholinesterase Inhibitors
The use of medications like donepezil, rivastigmine, and galantamine, which have proved successful in Alzheimer's disease, improves the cognitive scores of patients with vascular dementia, though the improvements prove to be statistically insignificant. A placebo-controlled randomized study conducted by Wilkinson et al. (2003) showed that there is an average of 2.5 points improvement in the donepezil-treated patients with vascular cognitive impairment over a span of 24 weeks in MMSE scores [30]. Such medications can be chosen in the case of some patients, especially with mixed pathology.
Memantine
Memantine, an antagonist of the NMDA receptor, has been mixed. Although moderate positive effects on executive functioning were indicated in some studies, others did not show any significant differences compared to placebo. It is off-label in the treatment of PSCI and is normally the last-resort AD in moderate-to-severe situations in which cholinesterase inhibitor use is contraindicated.
Antidepressants
These benefits of selective serotonin reuptake inhibitors (SSRIs), including fluoxetine and sertraline, may be twofold because, in addition to reducing post-stroke depression, they seem to improve cognitive recovery. The study reported by the FLAME trial (Chollet et al., 2011) showed an improvement in motor and cognitive outcomes in non-depressed patients who received fluoxetine treatment after stroke during 3 months follow-up [31]. These findings, however, could not be repeated later in further experiments like the FOCUS and TALOS trials, and controversy has arisen regarding the routine use of SSRIs in non-depressed patients.
SSRI of geriatric patients should be approached carefully, because of possible interactions with anticoagulants, antacids, and the possibility of hyponatremia and gastrointestinal bleeding [32].
Timing and Duration of Treatment
|
Treatment Strategy |
Recommended Timing |
Duration |
Notes |
|
Cognitive Rehabilitation |
Subacute phase (2–6 weeks post-stroke) |
3–6 months |
Ideally integrated into a structured multidisciplinary rehab program |
|
Pharmacotherapy |
Early initiation in appropriate cases |
Minimum of 3–6 months |
Reassess cognitive/functional status after trial period |
|
Long-Term Management |
Ongoing post-treatment follow-up |
Every 6–12 months |
Especially important in high-risk or progressively impaired patients |
Future Directions and Research Gaps
Although an increasing awareness of post-stroke cognitive impairment (PSCI) as a considerable health burden in the elderly has been witnessed, there exist multiple conspicuous research and clinical gaps that have not been bridged. Among the worst problems is insufficient agreement on diagnostic criteria and diagnostic classification systems specific to PSCI. The most recent definitions supersede the other cognitive disorders, including Alzheimer's disease or vascular dementia, and there is inconsistency in the diagnosis and the underrepresentation in clinical practices [33].
Further, the majority of clinical trials assessing pharmacological and/ or non-pharmacological treatment modalities of cognitive impairment following stroke constitute small inputs, brief tracking, and inconsistent outcome measures. Elderly populations need to be studied using large-scale, multicenter randomized controlled trials (RCTs) without omitting any age-related factors, including frailty, comorbidities, and polypharmacy.
Mechanistically, a future study ought to investigate the relationship between the cerebrovascular pathology and neurodegeneration, especially concerning the APOE 2 genotype, the amyloid-beta accumulation, and tau pathology. Advanced neuroimaging (e.g., PET, DTI, fMRI) or use of biomarkers has the potential to identify patients at high risk of cognitive decline earlier and to stratify those patients in high and low risk categories [34].
Furthermore, the impact of the gut-brain axis on cognitive consequences in stroke has also come to the fore as a new area of thought. The effects of dysbiosis and microbial metabolites like trimethylamine-N-oxide (TMAO) on systemic inflammatory status as well as neurovascular dysfunction have been suggested, and these processes await clarification of their clinical significance in people with a stroke history.
Long-term after-discharge support systems for geriatric patients with PSCI also have a high lapse rate. Although acute care of stroke and inpatient rehabilitation are widely developed in most health systems, no structured community-based cognitive rehabilitation programme, training of caregivers, and provision of psychological support to address the needs of the population under consideration are in place.
Figure 1
The use of digital and home-based cognitive training tools should also be emphasized in future strategies, taking into account the limited mobility of older stroke survivors. The implementation and use of artificial intelligence and remote monitoring in care models can potentially provide scalable, cost-effective mechanisms of long-term management of cognition [35].
Closing those gaps by implementing collaborative, interdisciplinary studies will be central to enhancing the precision of the diagnosis, therapeutic measures, and the quality of living that stroke-related cognitive impairment strikes among the geriatric patients.
Conclusion
The poststroke cognitive impairment occurs commonly and importantly in elderly individuals, with broad-scale ramifications on autonomy, restorative capacity, and overall quality of life. The pathology is the complicated interaction of vascular damage, neurodegeneration, and whole-body hazards. Time-dependent management involves preparing appropriate interventions by detecting early with the help of validated instruments such as MoCA and MMSE, and the application of neuroimaging. There is evidence utilising cognitive rehabilitation, lifestyle change, and in some situations, pharmacological treatment. The results notwithstanding, a significantly high number of patients still exhibit chronic cognitive impairment, and there is a potential risk of the development of dementia. The weakness of the current studies is a small sample size and the absence of standard criteria. Longer-term research should focus on mass testing, biomarkers, and the use of technology that could be used to monitor remotely, as well as provide cognitive assistance. This will be important in increasing the outcome and the quality of care for the aged stroke patients across the world by filling these gaps in a multi-disciplinary and patient-focused manner.
References
1. D’Souza, C.E. et al. (2021) ‘Cognitive impairment in patients with stroke’, Seminars in Neurology, 41(01), pp. 075–084. doi:10.1055/s-0040-1722217.
2. Mijajlovi?, M. D. et al., 2017. Post-stroke dementia–a comprehensive review. BMC Medicine, 15(1), pp.1-12.
3. Sun, J. H. et al., 2014. Post-stroke cognitive impairment: epidemiology, mechanisms and management. Annals of Translational Medicine, 2(8), p.80.
4. Sachdev, P. S. et al., 2014. The incidence of dementia in stroke survivors: a systematic review and meta-analysis. Stroke, 45(1), pp.183-193.
5. Sun, J.H., Tan, L. and Yu, J.T., 2014. Post-stroke cognitive impairment: epidemiology, mechanisms and management. Annals of Translational Medicine, 2(8), p.80.
6. . Nys, G. M. et al., 2005. Early cognitive impairment predicts long-term depressive symptoms and quality of life after stroke. Journal of the Neurological Sciences, 228(1), pp.27-33.
7. 7. Chamorro, Á. et al., 2016. The immunology of acute stroke. Nature Reviews Neurology, 12(5), pp.258-271.
8. Pendlebury, S. T. & Rothwell, P. M., 2009. Prevalence, incidence, and factors associated with pre-stroke and post-stroke dementia: a systematic review and meta-analysis. Lancet Neurology, 8(11), pp.1006–1018.
9. Xu, X., Chen, Z. and Gao, F. (2024) The relationship between postoperative cognitive dysfunction and cerebral small vessel disease: A comprehensive review [Preprint]. doi:10.22541/au.172114334.44473774/v1.
10. Tsiakiri, A. et al. (2024) ‘Mapping Brain Networks and cognitive functioning after stroke: A systematic review’, Brain Organoid and Systems Neuroscience Journal, 2, pp. 43–52. doi:10.1016/j.bosn.2024.08.001.
11. (2024) Review for ‘effect of acupuncture on cognitive function in patients with post?Stroke Cognitive Impairment: A systematic review and meta?analysis’ [Preprint]. doi:10.1002/brb3.70075/v1/review2.
12. ‘Poststroke cognitive decline across stroke types and ischemic subtypes: Comprehensive insights from levine et al. (2025)’ (2025) Blogging Stroke [Preprint]. doi:10.1161/blog.20250613.744583.
13. Pasi, M. and Cordonnier, C. (2020) ‘Clinical relevance of Cerebral Small Vessel diseases’, Stroke, 51(1), pp. 47–53. doi:10.1161/strokeaha.119.024148.
14. Merelli, A. et al. (2021) ‘Hypoxia, oxidative stress, and inflammation: Three faces of Neurodegenerative Diseases’, Journal of Alzheimer’s Disease, 82(s1). doi:10.3233/jad-201074.
15. Goulay, R. et al. (2019) ‘From stroke to dementia: A comprehensive review exposing tight interactions between stroke and amyloid-β formation’, Translational Stroke Research, 11(4), pp. 601–614. doi:10.1007/s12975-019-00755-2.
16. Naveh-Benjamin, M. and Cowan, N. (2023) ‘The roles of attention, executive function and knowledge in cognitive ageing of working memory’, Nature Reviews Psychology, 2(3), pp. 151–165. doi:10.1038/s44159-023-00149-0.
17. José, R.-G., Samuel, A.-S. and Isabel, M.-M. (2020) ‘Neuropsychology of executive functions in patients with FOCAL LESION IN THE PREFRONTAL CORTEX: A systematic review’, Brain and Cognition, 146, p. 105633. doi:10.1016/j.bandc.2020.105633.
18. Nys, G. M. et al., 2005. Early cognitive impairment predicts long-term depressive symptoms and quality of life after stroke. Journal of the Neurological Sciences, 228(1), pp.27-33.
19. Claassen, J. et al. (2019) ‘Detection of brain activation in unresponsive patients with acute brain injury’, New England Journal of Medicine, 380(26), pp. 2497–2505. doi:10.1056/nejmoa1812757.
20. Khaw, J. et al. (2021) ‘Current update on the clinical utility of MMSE and MOCA for stroke patients in Asia: A systematic review’, International Journal of Environmental Research and Public Health, 18(17), p. 8962. doi:10.3390/ijerph18178962.
21. Czap, A.L. and Sheth, S.A. (2021) ‘Overview of imaging modalities in stroke’, Neurology, 97(20_Supplement_2). doi:10.1212/wnl.0000000000012794.
22. Stolwyk, R.J. et al. (2021) ‘Poststroke cognitive impairment negatively impacts activity and participation outcomes’, Stroke, 52(2), pp. 748–760. doi:10.1161/strokeaha.120.032215.
23. McKnight, R., Price, J. and Geddes, J. (2019) ‘Delirium, dementia, and other cognitive disorders’, Psychiatry [Preprint]. doi:10.1093/oso/9780198754008.003.0034.
24. Allan, L. M. et al., 2011. Long-term cognitive consequences of ischemic stroke: evidence from a population-based study. Alzheimer's & Dementia, 7(5), pp.599-606.
25. Fieten, K.B., John, S.M. and Nowak, D. (2021) ‘Secondary and tertiary prevention: Medical rehabilitation’, Handbook of Experimental Pharmacology, pp. 449–470. doi:10.1007/164_2021_511.
26. Godefroy, O. et al. (2024) ‘Are we ready to cure post-stroke cognitive impairment? many key prerequisites can be achieved quickly and easily’, European Stroke Journal, 10(1), pp. 22–35. doi:10.1177/23969873241271651.
27. Loetscher, T. & Lincoln, N. B., 2013. Cognitive rehabilitation for attention deficits following stroke. Cochrane Database of Systematic Reviews, (5).
28. Brunt, A., Albines, D. and Hopkins-Rosseel, D. (2019) ‘The effectiveness of exercise on cognitive performance in individuals with known Vascular disease: A systematic review’, Journal of Clinical Medicine, 8(3), p. 294. doi:10.3390/jcm8030294.
29. Sagen-Vik, U. et al. (2022) ‘The longitudinal course of anxiety, depression and apathy through two years after stroke’, Journal of Psychosomatic Research, 162, p. 111016. doi:10.1016/j.jpsychores.2022.111016.
30. Wilkinson, D. et al., 2003. Donepezil in vascular dementia: a randomized, placebo-controlled study. Neurology, 61(4), pp.479-486.
31. Chollet, F. et al., 2011. Fluoxetine for motor recovery after acute ischaemic stroke (FLAME): a randomised placebo-controlled trial. The Lancet Neurology, 10(2), pp.123–130.
32. Antimisiaris, D. et al. (2021) ‘Medication related problems’, The Senior Care Pharmacist, 36(2), pp. 68–82. doi:10.4140/tcp.n.2021.68.
33. Spalletta, G. et al., 2015. Predictors of cognitive deterioration after stroke: a review of current literature. Journal of Alzheimer's Disease, 50(1), pp.75-80.
34. Ibrahim, B. et al. (2021) ‘Diagnostic Power of resting?state fmri for detection of network connectivity in alzheimer’s disease and mild cognitive impairment: A systematic review’, Human Brain Mapping, 42(9), pp. 2941–2968. doi:10.1002/hbm.25369.
35. Jeddi, Z. and Bohr, A. (2020) ‘Remote patient monitoring using artificial intelligence’, Artificial Intelligence in Healthcare, pp. 203–234. doi:10.1016/b978-0-12-818438-7.00009-5.
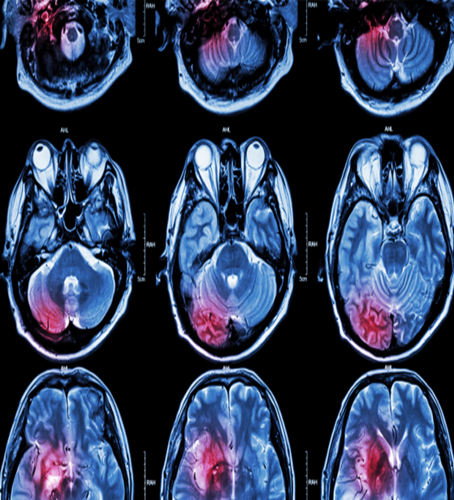
Figure 1
