Groin Keloids Post Bilateral Inguinal Herniotomy in a 4 Year Old Male– A Case Report with Review of the Literature
Groin Keloids Post Bilateral Inguinal Herniotomy in a 4 Year Old Male– A Case Report with Review of the Literature
S Adefarakan1*, V Mingle2, O Kushitor3, W Asman4, S Osei-Nketiah5
1,2,3,4,5. Paediatric Surgery Unit, Department of Surgery, University of Ghana Medical Centre (UGMC), Accra, Ghana.
*Correspondence to: Dr Shina Adefarakan, Department of Surgery, Paediatric Surgery Unit, University Of Ghana Medical Centre (UGMC).
Copyright
© 2025: Dr Shina Adefarakan. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 17 July 2025
Published: 04 Aug 2025
Abstract
Aberrant reaction to cutaneous injury spreading beyond the original wound's boundaries results in the formation of keloids. We present the case of a four-year-old male patient who had bilateral inguinal herniotomy at another facility presenting 1 year later to our facility with huge keloids in the groin. The keloids were surgically excised. The patient was scheduled for post surgical triamciniolone injection but defaulted treatment.
Groin Keloids Post Bilateral Inguinal Herniotomy in a 4 Year Old Male– A Case Report with Review of the Literature
Introduction
Keloids result from aberrant healing in response to an injury or wound. Keloids are fibroproliferative disorders that can result from cutaneous injuries to the reticular dermis [1]. Keloids are usually very obvious and are more likely to occur in areas like the anterior chest, shoulder, deltoid, mouth, and ears causing both cosmetic as well as significant psychosocial burden for the patient [2]. Keloids can form in any part of the body where scarring occurs and spontaneous regression is unlikely, and with multiple management protocols, recurrence is high [3] Keloids occuring in the groin is quite rare. Different treatment options have been described however combination therapy which includes surgery is the best option for management. In this case report, we present a 4 year old who developed huge keloids in the groin after bilateral inguinal herniotomies.
Case Report
A 4-year-old healthy boy presented to out clinic after being operated for bilateral inguinal hernia in another country before presenting to our facility. The surgery had been performed 1 year prior to presentation. The mother noticed the keloid scar a few months after the surgery and it kept increasing in size prompting her to seek medical management. [Figure 1]. On examination, there was huge complex multilobulated keloid spanning from the right groin across the pubic area to the left groin. Under general anesthesia, an elliptical incision was made around keloid, incision deepened and the keloid was completely excised and specimen sent for histopathology [Figure 2].The wound was closed with subcuticular sutures and patient’s recovery was uneventful [Figure 3]. He was discharged home the same day and was scheduled for post surgical triamcinolone injection. Patient defaulted his clinic visits so injections could not be given. Upon telephonic follow-up, the mother said the patient received the injection in another country after the procedure. However, the keloid has started recurring 7 months after the surgery.
Figure 1 : Keloids at post bilateral herniotomy incision site
Figure 2 : Keloids after Excision
Figure 3: Post Excision of Keloids
Discussion
Keloids are pathological scars that occur due to an excessive aggregation of collagen type I and fibroblasts within the inflammatory reticular dermis. Keloids usually develop in areas of extremely tense, mobile parts of the skin. In a report by Louw, Asians and Blacks are more prone to developing keloid than caucassians. In another study, Black people are significantly more likely to develop Acne Keloidalis Nuchae (AKN) than Asians, a particular type of keloid [4,5]. Rubinstein-Taybi syndrome (RSTS), Ehlers-Danlos syndrome, Lowe syndrome, new X-linked syndrome, Dubowitz syndrome, Noonan syndrome, and Goeminne syndrome are among the illnesses connected to a higher incidence of keloid. It then appears that genetic and environmental variables contribute to the development of keloids.[4]. One gene also linked to keloid risk is ASAH1 [6]. It is sometimes difficult differentiating keloids and hypertrophic scars. The main method used to distinguish keloids and hypertrophic scars is histopathology combined with clinical symptoms but this can sometimes be confusing [7]. Practically, the main differences between keloid and hypertrophic scars are hypertrophic scars does not extend beyond the wound boundary and it may disappear spontaneously, and after excision. Hypertrophic scars do not reoccur like keloids. Hypertrophic scars present within a few weeks in contrast to keloids which may appear much later [8,9]. The extremely high recurrence rate of surgery as a stand-alone treatment is its main drawback. Surgery alone is not sufficient and multimodal treatment is the way to go. Intralesional corticosteroid injections by means of anti-inflammatory action and inhibiting the production of fibroblasts by reducing collagen and synthesizing glycosaminoglycans are the most common additional treatment options available in the treatment of keloids. Other adjuvant treatment modalities are superficial radiation therapy, autologous platelet-rich plasma, bleomycin, and verapamil. [10,11].Triamcinolone acetonide injections limit fibroblast proliferation while promoting collagen degradation. Adverse effects of intralesional corticosteroids include hypopigmentation, cutaneous atrophy, telangiectasia, and injection site discomfort [12,13].
In this case report, we completely excised the keloids at the groin. Patient defaulted planned follow up treatment subsequently leading to recurrence 7 months later.
Conclusion
Keloids after herniotomy is very rare. Only one other case report has been reported on this. Genetic and Environmental factors may play a role in the development of these keloids. Surgical excision and post-surgical steroid injection is the mainstay of treatment. Patients have to be followed up closely due to the high risk of recurrence. Although rare, keloids can occur after surgery for inguinal hernia and parents have to be counselled on this as a complication.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient’s mother has given her consent for the patient’s images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
None
Conflicts of interest
There are no conflicts of interest.
References
1. Robles DT, Moore E, Draznin M, Berg D. Keloids: pathophysiology and management. Dermatol Online J. 2007 Jul 13;13(3):9
2. Tsai CH, Ogawa R. Keloid research: current status and future directions. Scars Burns Heal. 2019 Jan;5:205951311986865.
3. Al-Attar A, Mess S, Thomassen JM, Kauffman CL, Davison SP. Keloid pathogenesis and treatment. Plast Reconstr Surg 2006;117:286–300.
4. Huang C, Wu Z, Du Y, Ogawa R. The Epidemiology of Keloids. In: Textbook on Scar Management: State of the Art Management and Emerging Technologies [Internet]. Cham (CH): Springer; 2020. Chapter 4. Accessed 5th June 2024.
5. Ogawa R, Okai K, Tokumura F, Mori K, Ohmori Y, Huang C et al. The relationship between skin stretching/contraction and pathologic scarring: The important role of mechanical forces in keloid generation. Wound Repair Regen. 2012 Mar;20(2):149-57.
6. Santos-Cortez RLP, Hu Y, Sun F, Benahmed-Miniuk F, Tao J, Kanaujiya JK et al. Identification of ASAH1 as a susceptibility gene for familial keloids. Eur J Hum Genet. 2017 Oct;25(10):1155-61.
7. Yong ZHANG, Xuwen TANG, Yang LIU, Dongyun YANG,Treatment of Keloids in A Child with Surgery Alone: Clinical Application of the LBD Suturing Technique. Chinese Journal of Plastic and Reconstructive Surgery. Volume 3, Issue 1,2021,Pages 46-50
8. Burd A, Huang L. Hypertrophic response and keloid diathesis:Two very different forms of scar. Plast Reconstr Surg 2005;116:150e–7e.
9. Mostinckx S, Vanhooteghem O, Richert B, De La Brassinne M. Keloid and hypertrophic scar. Ann Dermatol Venereol 2005;132:384–7.
10. Xu J, Yang E, Yu NZ, Long X. Radiation therapy in keloids treatment:History, strategy, effectiveness, and complication. Chin Med J (Engl) 2017;130:1715–2.
11. Narahari, Janjala; Vepakomma, Deepti. Post-inguinal herniotomy keloid in pediatric age groups – A case report with review of the literature. Journal of Dr. YSR University of Health Sciences 13(3):p 285-287, Jul–Sep 2024.
12. Leventhal D, Furr M, Reiter D. Treatment of keloids and hypertrophic scars: a meta-analysis and review of the literature. Arch Facial Plast Surg. 2006 Nov-Dec;8(6):362-8
13. Aishwarya Kishor Kedar et al. Spontaneous multiple keloids: a case report. Pan African Medical Journal. 2024;48(110). 10.11604/pamj.2024.48.110.43157.

Figure 1
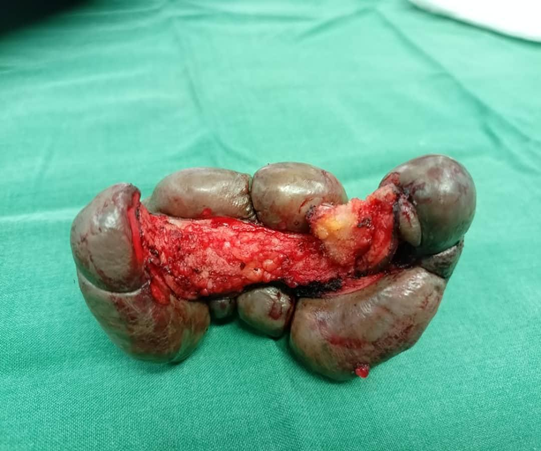
Figure 2
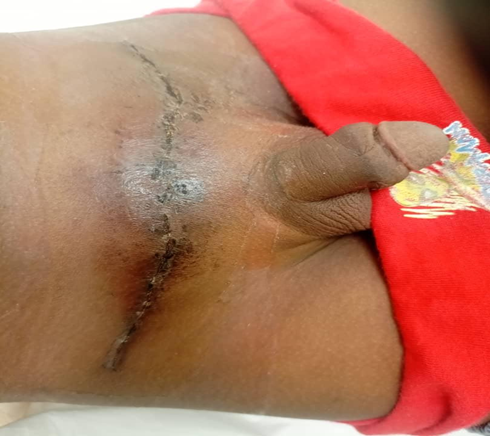
Figure 3
