Kidney Transplantation: Narrative Review of Challenges and Future Perspectives on Living Donor Renal Transplantation
Kidney Transplantation: Narrative Review of Challenges and Future Perspectives on Living Donor Renal Transplantation
Dr. Nibras Yaseen*
*Correspondence to: Dr. Nibras Yaseen (PhD), Sri Lanka.
Copyright.
© 2025 Dr. Nibras Yaseen This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 09 Aug 2025
Published: 16 Aug 2025
DOI: https://doi.org/10.5281/zenodo.17038435
Abstract
The re-transplantation of kidney grafts for patients who have experienced previous failures offers a promising alternative to conventional dialysis, albeit with significant challenges that can affect long-term outcomes. Patients undergoing repeated kidney transplants often present with complex immunological profiles, extensive comorbidities, and the adverse effects of prolonged immunosuppressive therapy. Despite these hurdles, the potential for expanding the donor pool to include high-risk candidates is a topic of growing interest. A critical yet underexplored area in this regard is the use of living kidney donors for repeated transplants. High-quality grafts from living donors offer numerous advantages, including the possibility of preemptively addressing kidney failure, reducing waiting times, and improving overall graft survival rates. This study aims to delve deeper into the role of living kidney donation within the unique context of repeated kidney transplantation. Living kidney donations have long been regarded as the optimal treatment for patients with end-stage renal disease due to their superior outcomes and ability to expand the organ pool. However, the utilization of this valuable resource remains limited, particularly in the case of repeated transplants. Our research seeks to bridge this knowledge gap by providing a comprehensive analysis of the benefits and challenges associated with living kidney donation for patients requiring a second or subsequent transplant. In addition to medical considerations, this study will address the ethical and legal challenges inherent in living kidney donation. We will also examine the psychosocial and emotional aspects, recognizing that both donors and recipients require robust support systems to manage the psychological impacts of transplantation. Economic and financial factors play a significant role in the feasibility and success of living kidney donation programs. Furthermore, this study will provide insights into the short- and long-term challenges faced by recipients of living donor kidneys, emphasizing the importance of continuous monitoring and tailored post-transplantation care to ensure optimal outcomes.
Keywords: kidney transplantation, risk factors, living donor, medical challenges, psychosocial and emotional challenges, financial challenges, short- and long-term challenges.
Kidney Transplantation: Narrative Review of Challenges and Future Perspectives on Living Donor Renal Transplantation
1. Introduction
Kidney failure is a significant global public health issue. Kidney transplantation, particularly living donor kidney transplantation (LDKT), greatly enhances the survival and quality of life for individuals with kidney failure and is also cost-effective for healthcare systems. In certain countries, nearly all kidney transplants involve organs from living donors. Increasing the rate of LDKT worldwide could significantly reduce the mortality associated with kidney failure. However, from 2008 to 2023, global living kidney donation rates have remained below five living kidney donors per million population. Moreover, the absolute number of living donor kidney transplants performed in many countries has seen minimal growth over the past two decades. Until recently, efforts to increase LDKT have primarily focused on patient-level interventions. A systematic review found that these interventions were only modestly effective. Additionally, many of the studies reviewed were at a high risk of selection bias, as they restricted participation based on factors such as the ability to speak English and use a computer. Focusing solely on patient-level interventions may exacerbate disparities in access to LDKT, favoring individuals with the social and financial resources to navigate the process and find donors. This individual-level focus overlooks critical organizational and environmental factors that are essential components of a health system. Emerging research underscores the importance of addressing system-level barriers and implementing broad system-level interventions to succeed in transplantation. A comprehensive systems approach can help overcome challenges in care delivery and create a patient-centered, high-performing healthcare system. A recent commentary suggests that issues in transplantation can only be resolved through systems thinking.
The essential benefit of getting a kidney from a living giver is that the organ is ordinarily better and more impervious to ischemic reperfusion injury. The kidney function, tissue and immunological compatibility, and overall physical health of living donors are all thoroughly screened. This is very different from grafts from deceased donors, where the stress and damage caused by the donor's death, combined with the long periods of cold storage required for retrieval and transfer, can temporarily decrease and possibly make organ function impossible to restore. Thirty percent of kidneys from deceased donors can have delayed graft function, and recipients may need weeks to become fully dialysis-independent, making them more vulnerable after surgery. Then again, kidneys from living givers as a rule capability right away, diminishing the gamble of hospitalization and renal substitution treatment after the transfer to under 4%, consequently setting the beneficiary up for the best short-and long haul results. Treating end-stage renal disease (ESRD) with living donor kidney transplantation is superior to dialysis and deceased donor transplantation in terms of survival and quality of life. In this procedure, a living donor—often a biological relative, friend, or altruistic individual—donates a healthy kidney to a patient with renal failure.
Live donor organ transplantation offers therapeutic advantages due to higher graft survival rates, shorter wait periods, and improved patient outcomes. However, the process from donor assessment to post-transplant care presents various medical, ethical, psychological, monetary, and logistical challenges. Although the surgery is generally safe, it poses risks for both donor and recipient, necessitating meticulous preparation and care. Ethical considerations are crucial in living donor transplants due to the potential for coercion or undue pressure, especially in close relationships. Ensuring informed consent and voluntariness is essential to uphold donor and recipient rights and welfare. The transplantation process must adhere to principles of independence, kindness, impartiality, and justice. Donors may experience guilt, fear, and anxiety, while recipients might have concerns about outcomes and future immunosuppressive therapy. Addressing these emotional and psychological challenges requires comprehensive psychosocial evaluations and ongoing care. Preoperative counseling and postoperative follow-up are vital for psychological support and mutual well-being. Living donor kidney transplants are costly, with indirect expenses such as lost wages, travel, and productivity impacting donors and recipients. Post-transplantation challenges include managing long-term health and immunosuppressive medications. Patients must adhere to strict treatment regimens to prevent rejection and manage the adverse effects of immunosuppressive drugs. Long-term monitoring for complications such as cancer, cardiovascular disease, and infections is essential. Regular interdisciplinary care is necessary to assess and support the quality of life for both recipients and donors. This study examines the challenges associated with living donor kidney transplantation. It analyzes medical, ethical, emotional, financial, and post-transplantation difficulties to identify and address operational obstacles. By optimizing technologies and policies, the study aims to enhance the benefits of living donor organ transplantation for both donors and recipients.
Medical and health-related challenges
1.1 Donor health evaluation and selection criteria
Donor health examination begins with a complete medical screening. Health is checked to confirm donor suitability [5]. A complete medical history, physical exam, lab testing, and imaging are necessary. Kidney, heart disease, and other organ examinations reveal potential donation barriers. Because they can create difficulties before or after surgery, hypertension and diabetes checks are crucial. A thorough checkup assures donor safety and transplantation success. Besides physical checks, donor selection requires psychological assessments. Donor mental and emotional readiness is assessed by psychology. This exam ensures the donor makes an informed, voluntary decision without pressure. Psychologists or psychiatrists interview and conduct standardized tests to assess donors' mental health, donation understanding, and post-donation mental state [6]. Contributors should be mentally ready for the donation's psychological and emotional effects. Health monitoring after donation is needed to track recovery and detect long-term effects. Donors must have regular kidney health checks. This ongoing surveillance detects and treats donation-related health issues. Long-term monitoring helps detect health issues including renal function decline and provide prompt intervention and support [7]. The donor-recipient compatibility is crucial to donor selection. Blood type, tissue type, and immunology indicators are checked to verify the donor's kidneys are suitable. Tests for compatibility reduce organ rejection and improve transplant success. HLA matching, cross-matching and kidney function testing can ensure donor-recipient compatibility. Another crucial donor evaluation stage is surgical risk assessment. This requires understanding donor surgical risks and outcomes. The donor's medical history, health, and potential problems are assessed preoperatively [8]. This comprehensive assessment helps plan the procedure, anticipate issues, and assure donor health. Ethics matter in donor selection. Maintaining ethics needs donations that are voluntary and donor awareness of risks. Ethical selection must emphasize donor liberty and well-being. This details the operation, risks, and post-donation care. Ethical monitoring protects donors' rights and well-being throughout the donation procedure, preserving the transplantation program.
1.2 Recipient health and compatibility issues
Kidney transplant outcome depends on recipient health and compatibility. HLA matching, which compares donor and recipient tissue types to decrease organ rejection, is a major problem [9]. HLA matching determines how effectively the recipient's immune system accepts the donated organ. Incompatible HLA types can cause acute or chronic rejection, requiring intensive pre-transplant testing and possibly immunosuppressive medicines. Proper matching improves transplant success and graft survival. Managing pre-existing diseases that could affect transplant success is also important. Many transplant recipients must manage diabetes, hypertension, or cardiovascular disease before and after the transplant. Uncontrolled diabetes and hypertension can slow wound healing and increase infection risk, and transplant failure can result [10]. Comprehensive pre-transplant examinations and continuous management of these diseases are essential to improve recipient health and transplant outcomes. Cross-matching tests determine whether the recipient's antibodies will react with the donor's cells, beyond HLA matching [11]. This test is essential for detecting hyper acute rejection, which happens when the recipient's antibodies target the donor's kidney. Positive cross-matches may require other donors or desensitization. Immunological compatibility testing minimizes immediate and severe rejection, making transplants easier. Health exams before transplantation include psychological and physiological tests. Psychological tests evaluate transplant readiness and ability to follow medication and lifestyle changes [12]. A thorough assessment reveals transplant issues and allows for individualized pre- and post-operative treatment. Post-transplant infections and graft failure must be considered. Preventing organ rejection needs immunosuppressive medicines that increase infection risk. Comprehensive post-transplant care includes infection monitoring and prompt treatment [13]. Monitoring the newly placed kidney and treating post-operative problems requires regular follow-ups. Finally, long-term health care aids transplants. This involves renal function monitoring, immune suppression, and drug side effects control. Avoiding graft rejection and maintaining health needs adherence to medication and regular follow-ups. Long-term care with education and support improves transplant outcomes and quality of life.
1.3 Surgical risks and complications
Any major surgery includes risks and complications, including kidney transplantation. Surgery risks include infections, bleeding, and organ damage. Blood vasculature or surgical issues might induce intra-operative bleeding, needing further therapy or transfusions [14]. Infection risks increase when bacteria invade the operating room and incision site. Despite precautions, big surgeries are risky. Neighboring organ harm is another kidney transplant danger. Kidneys, spleen, liver, and intestines are close together. Surgical manipulation can accidentally injure these organs. Injuries from excessive manipulation or retraction may require extra organ repair treatments. Proper surgical techniques and prior planning reduce the likelihood of such injuries and ensure transplant success. Donors and receivers worry about postoperative complications. Donors often experience discomfort, incision site infection, and wound healing difficulties. Postoperative problems for recipients include organ rejection, infection, and immunosuppressive medication difficulties [15].
Fig. 1 Programmatic consideration for the care of international living donors and candidates
Monitor for rejection or infection and treat surgical problems immediately after surgery. Kidney transplantation risks organ rejection. The recipient's immune system may attack the transplanted kidney as foreign. Acute or chronic rejection may require immunosuppressive medicines or additional operations. Chronic rejection can develop over years, while acute rejection occurs between weeks to months following transplant. Managing and treating rejection events requires regular monitoring and quick action to ensure transplant success. Postoperative immune suppressive therapy problems must be managed [16]. Although important to prevent rejection, these drugs increase infection risk, organ damage, and metabolic abnormalities. To prevent rejection and minimize side effects, immunosuppressant dosage must be balanced. To prevent complications and maintain health, the pharmaceutical regimen must be monitored and adjusted regularly. Late-onset surgical problems must be identified and treated with long-term follow-up [17]. This includes continued monitoring for delayed graft function and chronic renal disease. A thorough follow-up schedule includes blood tests, imaging studies, and clinical assessments. Long-term monitoring helps to identify any issues and address them quickly, ensuring the transplanted kidney's success and lifespan. International living donor programs involve complex, multifaceted considerations that ensure the health, safety, and well-being of both donors and recipients. Fig. 1 outlines the key elements and steps necessary for the effective and ethical management of these programs. Table 1 outlines various risks associated with international living organ donation and suggests methods to mitigate them. To address this, it is essential to evaluate the donor's motives and autonomy early and create guidelines specifying the nature and duration of the donor-recipient relationship. Communication barriers can complicate the donation process. Logistical challenges include the costs of transport and housing.
2. Ethical and legal challenges
2.1 Informed consent and autonomy
Medical ethics require informed consent, especially in high-risk treatments like kidney transplantation [18]. It assures that patients understand the procedure, its risks, advantages, and alternatives before consenting. The healthcare team and patient discuss kidney transplantation's surgical technique, potential risks, post-operative treatment, and long-term effects. The patient must comprehend to make an informed and voluntary care decision. Informed consent requires giving the patient clear, relevant information. This includes clarifying medical terminology, answering patient queries, and describing operation outcomes. To avoid confusion, information should be suited to the patient's knowledge and effectively delivered. To ensure patient understanding, written consent forms should be supplemented with spoken explanations. Informed consent requires patient autonomy to make healthcare decisions [19]. It stresses that patients should be able to choose treatment based on their values and interests. Respecting autonomy in kidney transplantation entails supporting a patient's right to accept or decline the donation based on their beliefs and circumstances. Respect for autonomy enables that patients make voluntary, self-determined decisions. Voluntary consent is essential to informed consent. Family, medical professionals and others cannot coerce or influence patients' decisions [20]. Healthcare practitioners must foster an environment where patients can share their actual preferences and concerns. To maintain voluntariness and guarantee consent is freely provided, financial, emotional, and social pressures must be identified and addressed. Patient-healthcare team communication is also necessary for informed consent. It is a continuous process throughout the patient's treatment [21]. As new information or the patient's condition changes, additional discussions may be needed to advise the patient about dangers or treatment plan revisions. This continual communication fosters transparency and keeps patients' consent informed and relevant throughout their care. In complex instances with unclear risks and benefits, informed consent might be difficult. Patients with cognitive disabilities or language problems may need extra help understanding the information. Family members, translators, or trained counselors may be needed to improve communication and assure informed consent [22]. Surrogate decision-makers when patients cannot make decisions are also ethically considered in informed consent and autonomy. If patients cannot make decisions owing to medical issues or other factors, legally approved substitutes or family members may do so. To ensure patient autonomy, even when the patient cannot consent, these surrogates must make judgments that are consistent with the patient's wishes and best interests.
2.2 Equity and Access
Healthcare providers and policymakers has to tackle kidney transplantation access inequities. Promote equal access and funding for minority programs to reduce inequities [27]. Organ assignment system efficiency and openness can also improve transplant organ distribution. Transplant centers, government organizations, and non-profits must collaborate to improve transplantation equity. Finally, monitoring and evaluating equality and access issues is necessary to identify and close gaps. Regular monitoring may uncover issues with transplant results, wait times, and access. Tracking these measurements and applying evidence-based approaches to address concerns can help the transplantation community enhance equity and guarantee that all persons have an equal opportunity at life-saving kidney transplants.
2.3 Legal frameworks and compliance
Transplantation of kidneys regulation and monitoring require legal frameworks and compliance to assure moral norms, patient and donor rights, and procedure integrity [28]. These frameworks address kidney transplantation laws, rules, and regulations ranging from obtaining organs to allocation. These regulations must be obeyed to safeguard patients, prevent abuses, and ensure ethics and professionalism. National law regulates kidney transplantation regulations cover the donation of organs, informed consent, and donor/recipient anonymity. Rules may govern organ distribution, transplantation worker credentials, and adverse event notification and handling. These rules standardize transplant center processes and ensure legality and ethics. Due to organ donation and transplantation's worldwide character, international laws and guidelines affect transplanting kidneys [29]. The WHO and world transplantation congress suggests that member countries follow international norms and ethics. These rules stop organ trafficking, distribute organs fairly, and promote international transplantation. Coordinating global transplantation efforts with these criteria increases results. Transplantation law is intricate and disputed about donor pay and motivations. While not rewarding donors for their organs is universally accepted to prevent exploitation and commercialization, several countries study measures to support donors financially or non-financially for lost salaries or medical bills. To balance ethics and donor support, legal frameworks must carefully traverse these concerns. Maintaining transplantation ethics requires transparent and fair pay structures. Regulators also closely monitor legal compliance. The governing bodies enforce legal and ethical norms for transplant centers and medical professionals. Inspections, audits, and reviews of transplant practices can identify and fix compliance issues [30]. Transplantation of organs complaints and legal difficulties are handled by regulators. Transplant facilities must follow institutional rules and accreditation standards in addition to national and international laws. Many transplant centers are accredited by the Joint Commission and National Kidney Foundation for ethics and quality [31]. These certification standards ensure transplant facilities provide excellent treatment and follow best practices. Clinical procedures, patient outcomes, and ethics are evaluated during accreditation. Legal and transplantation advances must be followed by kidney transplant doctors. Regular training and continued education help team members understand legal and ethical requirements and provide high-quality care. Compliance and ethics help the transplantation community preserve fairness, transparency, and patient rights. Fig. 2 highlights the challenges faced by clinical transplant coordinators in making decisions for living donor kidney transplantation (LDKT) donor candidates. These difficulties include assessing the donor's medical suitability, ensuring informed consent and voluntariness, managing communication barriers, and addressing logistical issues such as travel and accommodation. It must navigate ethical concerns, such as potential coercion and the donor-recipient relationship, while ensuring post-donation follow-up and long-term care for international donors. These multifaceted challenges require comprehensive strategies to ensure the safety and well-being of both donors and recipients.
Fig. 2 Difficulties in clinical transplant coordinators decision making for living donor kidney transplantation (LDKT) donor candidates
3. Psychosocial and emotional challenges
3.1 Donor psychological impact
The mental health of living kidney donors is carefully considered and supported [32]. The recipient may experience several emotions after donating a kidney. Donors often worry about surgery risks and advantages. Worries about the operation, complications, health, and receiver outcome may cause this fear. Comprehensive counseling and guidance can help donors make educated decisions and reduce donation anxiety. Pre-donation psychiatric exams can detect mental health or emotional issues that could affect the donor's ability to donate [33]. Detailed discussions with mental health professionals assess the donor's emotional stability, motivations for donating, and surgery preparation. The goal is to ensure donors make freely, well-informed decisions without external pressure or psychological suffering. Early detection of psychological barriers provides focused donor help. During donating, donors may feel anxiety, uncertainty, or ambivalence. Donors need ongoing psychological support to manage these emotions. Support groups, counseling, and education can provide comfort and community. Sharing experiences and receiving professional coaching helps donors manage their emotions and stay optimistic during the donation process [34]. Another important part of donor psychological health is post-donation emotional well-being. Donors may feel bereavement, body image alterations, or kidney function difficulties after surgery. If the transplant fails, donors may feel guilty or anxious. Donors need post-donation counseling and support to process these emotions and adjust to life. Donors can obtain continuous psychological therapy by visiting mental health providers regularly. Positive psychological effects are also important. Many contributors feel fulfilled, proud, and satisfied after assisting someone so deeply [35]. Giving can boost self-esteem and purpose. This good psychological benefit may overcome the initial donation anxiety and stress for some donors. Celebrating these successes and allowing donors to share their tales helps promote kidney donation. The donor's psychological experience depends on family and social support. Family discussions and support can greatly impact a kidney donor's mental health. Stress and anxiety might increase with familial pressure or lack of support. Social support systems like family counseling and support groups can help donors cope with these challenges and create a positive donating environment. Kidney donors' well-being and donation success depend on this complete psychological treatment [36]. Fig. 3 identifies risk factors related to the psychological and social well-being of families and children receiving kidney transplants. These factors include emotional stress, anxiety, and fear associated with the transplant process, as well as the impact on family dynamics and support systems. Maintaining open communication, providing psychological support, and fostering a strong network of social support are crucial in promoting tolerance and ensuring the overall well-being of both the patient and their family during the transplant journey.
Fig. 3 Risk factors related to psychological and social well-being that promote tolerance in families and children receiving kidney transplants
3.2 Recipient psychological impact
Before, during, and after kidney transplantation, recipients' mental and emotional health is profoundly affected. Due to their declining health and the uncertainty of finding a suitable donor, transplant recipients generally experience severe anxiety and stress before the transplant [37]. Recipients struggle emotionally between the hope of a life-saving treatment and the dread of complications or not receiving a transplant in time. Psychological treatment is needed to manage anxiety and be cheerful. Psychological difficulties arise with transplant surgery and recovery. Recipients may feel pleased and afraid—relief that the treatment is finished and they have a new kidney and anxiety about consequences. Adjusting to new circumstances and recovery can be difficult. Psychotherapy and group therapy can assist transplant patients manage these emotions [38]. The psychological difficulty of controlling health and following a stringent medical regimen continues post-transplant. Lifelong immunosuppressive medicine to avoid organ rejection can be frightening and have serious side effects [39]. The dread of rejection or other issues might cause persistent worry. Regular psychological counseling and support can help recipients manage these worries and establish medicine adherence and side effect management techniques, improving long-term outcomes. Kidney transplants improve quality of life, but they're double-edged. Many recipients see a tremendous improvement in their physical health and daily functioning, but the psychological adjustment can be difficult. If their donor is a living relative or acquaintance, recipients may feel guilty. The donor's health or debt may concern them. Counseling can help recipients reconcile appreciation with guilt and adopt a healthy outlook [40]. Social dynamics and connections are also affected by recipients' psychology. The transplant might change family roles and dynamics, causing conflict if expectations and realities differ [41]. Receivers may feel pressure to return to normalcy fast in their personal and professional life, which can be daunting. Family counseling and open communication can reduce these demands and enhance the recipient's adjustment and recovery. Mental health support and monitoring are crucial for kidney transplant patients' long-term mental health. Mental health treatments must be available to recipients to address new difficulties and preserve emotional well-being. This support can include counseling, support groups, and post-transplant life skills workshops. These tools are vital for recipients' health and quality of life, allowing them to completely benefit from the life-saving transplant and retain a positive, balanced outlook on their new existence.
3.3 Family and social dynamics
Kidney transplantation affects donors and recipients greatly according to family and social dynamics [42]. Family relationships can influence kidney donation decisions, and their support or resistance can greatly impact the donor's experience. Family support can make donors feel confident and valued in their decision. Conflict or lack of support can add stress and emotional strain, leading to regret. The transplantation process also alters family dynamics. During rehabilitation, family members generally manage home activities and care for the patient. This role change can strain family connections, especially if caring is significant or extended. Family transitions require open communication and support structures to avoid exhaustion and resentment. Family members may feel relief, appreciation, fear, and guilt during the transplant process. Family members may be relieved and appreciative that the recipient received a life-saving transplant, but they may feel terrible for not donating. Without open communication, these complicated emotions can cause conflict. Family counseling and support groups can help family members express their emotions and discover coping methods [43]. Social support from friends, family, and community is extremely important during transplantation. Donors and beneficiaries need emotional support, practical help, and a sense of belonging from a robust social support network. A strong support system can assist recipients follow their post-transplant care routine and improve their quality of life. Social support can legitimize donors' decisions and help them heal physically and emotionally. Some cultures strongly encourage or reject organ donation, which might affect the decision-making process and the family's reaction to the transplant [44]. Understanding and valuing these cultural aspects helps healthcare providers provide culturally sensitive care and assistance. Culturally sensitive education and counseling can help families make educated and agreeable decisions. Finally, kidney transplantation affects family and social dynamics long-term. Post-transplant health gains can improve family ties and functioning. Maintaining the recipient's health, preventing problems, and adjusting to family roles require constant help and adaptability. Table 2 offers a detailed overview of the psychological aspects associated with kidney transplantation, focusing on prevalence rates, influencing factors, assessment methods, and potential treatments. Depression and anxiety are prevalent in 17%-36.4% and 20%-36.4% of patients, respectively, with contributing factors including family psychopathology and medication side effects. ADHD affect 22.5% of patients, influenced by environmental stimulation and pre-transplant conditions. Neuro-cognitive deficits, affecting 6%-32.5% of patients, are linked to dialysis duration and coexisting conditions and are evaluated using tools such as the Wechsler Intelligence Scale and the Woodcock-Johnson IV. Interventions focus on educational support and cognitive training. Parental psychopathology impacts 27.7%-50.6% of families, influenced by factors such as poor health literacy and financial strain. Transition readiness, affecting 25.56%-65.28% of patients, is influenced by changes in healthcare responsibilities and knowledge gaps.
Table 2 Overview of the psychological aspects: frequency, variables that increase or decrease vulnerability, methods of evaluation, and potential treatments
|
Factors |
Occurrence |
Imperative and pliability issues |
Instances of valuation gears |
Instances of interferences |
|
Depression
|
Depression: 17%-36.4% |
Psychopathology in parents, Education of parents Environment and family structure, Absence from employment or school, Periods of rejection adverse effects from medications or the body |
Guideline for child behavior, Young people's self-report, Children's behavior evaluation scale, third edition tool for psychosocial evaluation, Version 2.0 of the patient health questionnaire |
CBT Treatment with dialectical behavior, Therapies centered on mindfulness, Training in parent supervision, Motivational interviews |
|
Neuro-cognitive deficits and disabilities |
6% to 32.5% [75[76] |
Time frame prior to transplanting, Dialysis duration Conditions that coexist in medicine, Hospital stay length of stay Dialysis age, Seizures, hypertension crises, and premature seizure [75[76], Environmental stimulation and malnourishment |
Children's Wechsler cognitive scale, Wechsler intelligence abbreviation scale, The Woodcock-Johnson IV cognitive ability exam cognitive function behavior rating inventory, Test 3 of Conner's Continuous Performance |
A personalized education program in addition to traditional educational resources, Training program for cognitive problem-solving abilities, Online educational courses |
|
Parental psychopathology |
27.7% to 50.6% [77] |
Duration of time following transplant, Poor health literacy and a pessimistic outlook on health care, Increased monetary effect Parents' views on their children's well-being [77], Divorce issues and a lack of time to care for younger siblings |
Questionnaire on patient health, generalized anxiety disorder, 7 general health questionnaire-30 post-traumatic stress disorder diagnostic scale beck depression inventory-II effect of the updated event scale |
Family counseling CBT, Treatment with dialectical behavior treatments centered on mindfulness
|
|
Transition readiness |
25.56% to 65.28% |
Compliance alterations in the duties related to health care, Differing expectations and aims [78][79], Knowledge of health factors related to parenting between the patient, family, healthcare professionals |
Transition index Readiness to transition questionnaire |
Transitioning to maturity and managing oneself with a prescription, treatment program Ascent to the shift |
4. Economic and financial challenges
4.1 Cost implications for donors
Kidney donors face costs beyond the donation procedure. Donors face several direct and indirect charges that might be costly [45]. Donors may pay for some tests, drugs, or follow-up sessions even when the recipient's (insurance) covers most medical expenditures. To reduce direct costs and encourage donation, full (insurance) and financial support are essential. Donor indirect costs can be high and complex. The loss of income from pre-operative examinations, surgery, and rehabilitation is one of the biggest indirect expenses of donation. The donor may be unable to work for several weeks following recovery. This loss of income can be especially difficult for people without paid leave or disability insurance [46]. Policy must compensate or protect donors financially so they are not financially damaged by their altruism. Travel and lodging costs are another major expense for kidney donors, especially if they must travel far to a transplant hospital [47]. These costs may include transportation, housing, and food for the donor and their family or support people. Some transplant programs help with these costs, although the extent varies. More consistent and comprehensive financial assistance initiatives can help donors cover travel and lodging expenditures. Very rarely, donors may develop health concerns that require additional medical treatment or monitoring [48]. To mitigate these financial risks and provide contributors peace of mind, policies must shield them from higher insurance costs and guarantee long-term care. Donors' psychological and emotional costs can indirectly cause financial difficulties. Health, transplant success, and recipient outcomes may worry donors, affecting their well-being and ability to work or handle finances [49]. Psychotherapy and mental health resources can help donors cope with emotional concerns, reducing indirect financial impact. Finally, health care social and economic inequalities may increase donor costs. Lower-income persons may struggle financially and lack resources, making donation tougher. These gaps must be addressed with financial aid, support from donor funds, and rules that allow everybody who contributes, regardless of socioeconomic status, to receive financial aid [50].
4.2 Healthcare system and insurance barriers
Kidney donors and recipients encounter hospitals and insurance restrictions that limit healthcare and financial assistance during transplantation [51]. Different healthcare plans' coverage and advantages are a healthcare system challenge. Most transplant recipients' insurance covers most medical expenses, although donors may pay for pre-donation exams, surgery, and post-op care. All contribution procedures must have thorough and consistent insurance to remove financial obstacles and support contributors. Donors and recipients must understand insurance coverage, pre-authorization, and claims processes. Complexity delays care, denies important therapies, and raises costs. Transplant facilities and healthcare providers can give insurance counseling to help patients and donors understand their coverage, negotiate the claims process, and advocate for needed care [52]. Simplifying these processes and giving clear insurance policy information can decrease stress and financial uncertainty. Donors and recipients may also have trouble getting healthcare through their insurance network [53]. Patients must travel far or seek care out-of-network to reach specialized transplant centers, which can increase costs and logistical difficulties. Expanding insurance networks to cover more transplant facilities and specialists and supporting out-of-network travel and lodging can assist patients and donors obtain the finest care without financial strain. Another major healthcare system impediment is the lack of long-term care and follow-up coverage. This may include monitoring, medication, and treatment for difficulties for recipients and monthly check-ups and management of long-term health impacts for donors. Insurance plans must cover these vital services to keep donors and recipients healthy [54]. Advocating for comprehensive long-term care coverage can help close this gap and support patients and donors. To improve adherence to medications and transplant results, insurance plans must cover immunosuppressive medicines without cost-sharing [55]. Low-income and uninsured persons suffer most from socioeconomic inequalities in healthcare and insurance. Care disparities delay treatment, exacerbate financial stress, and harm health. Addressing these disparities requires expanding public insurance, subsidizing low-income persons, and promoting health justice. Eliminating these systemic barriers allows us to treat and help all transplant patients and donors equally.
4.3 Economic disparities and access to transplantation
Poor people have trouble getting kidney transplants due of economic inequality. Lack of access, insurance coverage, and finances prevent prompt and appropriate medical care [56]. Economically poor patients are less likely to be evaluated for transplantation due to diagnosis and treatment delays. Equality for getting life-saving kidney transplants entails tackling economic inequalities. Without insurance or funding, these costs may be high. Financial issues may delay or hinder essential medical assessments, affecting transplant eligibility [57]. Financial aid and support are needed to lower these expenses and eliminate financial obstacles to transplantation. Access to transplantation depends on insurance coverage, but economic gaps often cause unequal coverage. Uninsured or underinsured low-income people have less access to medical care. Even with insurance, hefty deductibles, co-pays, and coverage limits can be costly. Increasing comprehensive insurance coverage and lowering out-of-pocket expenditures can help all patients afford transplantation [58]. Geographic and economic gaps hinder transplantation. Patients in remote or underserved locations may have to travel far for transplant center and specialized examinations and operations. Telemedicine, mobile clinics, and travel assistance can help all patients obtain transplants by bridging geographic and economic divides. Economic inequities affect patients' family and support networks [59]. Financial aid, respite care, and counseling can help families cope with transplantation. Policy initiatives, healthcare system improvements, and specialized assistance programs are needed to address economic transplantation inequities. Policymakers must support fair healthcare policies that increase insurance coverage, fund transplants, and promote health equity [60]. The healthcare industry must offer sliding scale prices, payment options, and financial counseling to minimize economic barriers. Community-based support initiatives and non-profit groups can also help financially disadvantaged people get life-saving kidney transplants.
5. Post-transplantation challenges
5.1 Long-term health monitoring and support
Both kidney donors and receivers need long-term health monitoring and support after transplant. Medical supervision is needed to diagnose and treat kidney transplant problems [61]. This includes regular transplant specialist visits, kidney function blood tests, and imaging investigations when needed. Early diagnosis of organ rejection, infection, and other problems can improve results and prolong kidney transplantation. Kidney transplant recipients must monitor and adjust immunosuppressive medication throughout their lives to maximize efficacy and avoid negative effects. Regular follow-ups address immunosuppressive drug adverse effects such infection susceptibility, cardiovascular issue, and metabolic abnormalities [62].
Fig. 4 Structure of criteria and relationship for the alternatives of living donors
Customized medical care and drug modifications are necessary to reduce these risks and sustain health. Healthcare practitioners must teach patients about drug adherence and imminent problems. To ensure their remaining kidney works well and detect any health complications after donation, kidney donors need long-term health monitoring. Most donors have healthy lives after donation, but they need regular kidney, blood pressure, and health checks [63]. These evaluations assist donors obtain timely care and interventions by identifying potential issues. Donors need standardized long-term follow-up measures to obtain proper treatment throughout their lives. Long-term donor and receiver health monitoring need psychological assistance. As shown in Fig. 4, living with a transplanted organ or post-donation can be difficult emotionally and psychologically. Patients may worry about organ rejection or problems, while donors may worry about their decision and its health effects. Mental health treatments like therapy and support groups can help address these issues and improve emotional well-being [64]. Long-term kidney donor and recipient health depends on social support systems. Post-transplant support from family, friends, and community services can provide practical, emotional, and encouraging help [65]. Support groups and patient networks can provide recipients with insights, experiences, and coping skills. Similar networks can reassure and unite donors. Comprehensive post-transplant treatment includes connecting patients to these support systems. Long-term kidney donor and recipient health monitoring and support also address lifestyle factors that affect health. Promoting healthy habits like eating well, exercising, and avoiding smoking and alcohol is essential. Lifestyle education and counseling reduce hazards and improve health. Long-term outcomes depend on treating comorbidities like diabetes, hypertension, and cardiovascular disease. Comprehensive care regimens that include lifestyle advising and comorbidity management help donors and recipients achieve the optimal health and quality of life following transplantation [66].
5.2 Immunosuppressive therapy management
Kidney recipients must manage immunosuppressive medicine to prevent organ rejection and reduce side effects and consequences [67]. The recipient's immune system would assault the transplanted kidney if not suppressed with immunosuppressive medicines. To maintain efficacy without harming the receiver, drug dosages must be monitored and adjusted. Calcineurin inhibitors, antiproliferative drugs, and corticosteroids are usually used in immunosuppressive therapy. Immune suppression is varied for each medication class. The complexity of these regimens requires regular blood drug testing to maintain therapeutic limits and avoid toxicity. Adjusting dosages and detecting side effects requires frequent blood tests and clinic visits. In contrast, over-immunosuppressant can lead to infections and other issues. Healthcare providers must educate and support strict medication schedule adherence [68]. Strong patient-provider relationships can improve communication, allowing patients to share medication adherence issues. Immunosuppressive drugs can cause infections, hypertension, diabetes, gastrointestinal difficulties, and bone diseases. Skin cancer and lymphoma can also result from long-term drug use. Post-transplant treatment requires monitoring and managing these side effects. Additional medications to treat blood pressure, blood sugar, and other disorders and lifestyle changes may minimize risk. Personalizing immunosuppressive medication to improve kidney transplant outcomes is progressing. Personalized immunosuppressive regimens are possible thanks to pharmacogenomics and therapeutic medication monitoring. Healthcare providers can better modify dosages and choose the best medicine combinations by considering genetic variants that affect drug metabolism and immune response. Adherence and financial stability depend on good insurance and inexpensive meds. Policy attempts to extend Medicare immunosuppressive drug coverage for kidney transplant recipients beyond three years are critical. Financial support programs and campaigns for lower medicine prices can help beneficiaries keep their treatment routine without stress. There are five primary classes of immunosuppressive drugs commonly used in renal transplant recipients. The mechanisms of action for these immunosuppressive drugs are illustrated in Figure 5.
Fig. 5 Mode of action of immunosuppressive treatment for patients after renal transplantation
5.3 Quality of life and outcomes
Kidney transplant recipients and donors consider QoL and long-term outcomes. Transplantation can eliminate chronic kidney disease and dialysis, improving QoL for patients. Transplant recipients generally enhance their physical health, energy, and well-being [69]. Despite the benefits, recipients may encounter QoL issues. Infections, weight gain, and mood fluctuations might result from immunosuppressive drug adverse effects. Recipients must also endure psychological stress from transplant rejection and constant health monitoring [70]. Medical, psychological, and social help are needed to address these difficulties. Counseling and mental health exams can help beneficiaries manage these challenges and maintain a high QoL. Most contributors are satisfied and fulfilled after donating [71]. However, QoL must be monitored and supported. Most donors recover following donation surgery in several weeks, but some may endure long-term complications like kidney function or persistent discomfort [72]-[75]. Donors need intensive follow-up treatment and assistance to address health concerns and maintain QoL. Social interactions may change for donors and receivers after transplant. Improved health can help individuals socialize and participate in activities previously limited by their illness. They may also have to adjust to family changes and health expectations from others. If issues emerge, donors may feel stress or remorse or a stronger link with the receiver. Social support and counseling for both sides can make these relationship adjustments succeed. Transplant recipients' long-term outcomes depend on medical and lifestyle changes [76]-[[78]. Recipients should eat well, exercise, and avoid smoking and drinking, which can damage the transplanted kidney. Lifestyle change education is essential post-transplant. Regular medical visits check kidney function, treat comorbidities, and encourage healthy habits for long-term success. Final research and enhancements to quality are needed to quantify and improve transplanted kidney receiver and donor QoL and outcomes. Medical professionals and academics analyze long-term success and contentment [79]. With this understanding, healthcare systems enhance QoL and outcomes for all transplanted kidney patients, maximizing this life-saving procedure.
6. Immediate and lasting threats to a living benefactor
While guiding an expected living benefactor, giving an agenda of all examined points is prudent. It is critical to permit more than adequate time between acquiring assent and playing out the gift system, empowering the contributor to pull out assent whenever without repercussions. Similarly as with every surgery, living organ gift conveys innate dangers, with a revealed death pace of 1 out of 3,000. The threats of intra-abdominal tissue damages and duodenal barrier have been testified in huge sequence of laparoscopic giver nephrectomy, but these are uncommon and mostly connected with the transperitoneal method. Regarding mortality, Short-term complications remain low when compared to current minimally invasive procedures. The assistances of peritoneal entry and an earlier method to renal hilum basins are provided by physical retroperitoneoscopic giver procedure, which chains the benefits of a triflingly hostile procedure with physical regulator. Modern laparoscopic techniques speed up work rehabilitation as well as medical and social recovery. Certain features of the population, like an elevated BMI, have been identified as theoretically weakening the remaining kidney's role in relations of lasting threats for donors. The threat of increasing ESRD (End-Stage Renal Disease) rises significantly by 7% for all element growth in BMI above 27 kg/m2. Corpulent living benefactors face an expanded transient gamble because of the intricacy of the surgery and a possible long haul hazard of creating ESRD. However, there is a lack of agreement about the BMI brink for the reception norms for living donors, which is principally imperative in populaces where the typical BMI is rising. Age considerations are also a part of this debate. More youthful benefactors, who have a more extended period since gift and a higher eGFR at the hour of gift, will generally encounter a more prominent compensatory expansion in the eGFR of the excess kidney. Conversely, donation of kidneys can occur at any age, and research has shown that older donors pose less of a risk than younger ones. Inside the transfer communal, it is generally believed that some clusters, such as black givers, givers with a genetic connection, and givers to patients with immune-related reasons for dialysis, are more likely to develop ESRD after donation. However, the idea of safety in donation is very important because well-screened living donors have similar survival rates and ESRD risk to controls in the general population who are matched for age, gender, race, or ethnicity. As can be seen in Table 3, the complete threat of kidney failure following living kidney contribution is still very low, happening in less than one in 200 donors (0.5 percent), which is significantly lower than the risk that exists in the general population.
Table 3 Major points when counseling a potential living kidney donor
|
Common threats |
Demise |
|
|
Common anaesthesia |
|
|
Intra-operative harm to abdominal tissues |
|
|
pain management after surgery, ileus, and relief |
|
|
An injection including emo-derivates |
|
|
Permanent nerve injury from being in a chair over long periods of time |
|
Detailed threats |
Age |
|
|
Body mass index |
|
|
Abstaining blood glucose |
|
|
Hereditary connection to the receiver |
|
|
Culture |
|
|
Pre-eclampsia |
|
Probable implant harm |
Needs to provide to wait-list |
|
|
Needs to use the kidney for study drives |
|
|
Needs to leave the kidney not be utilized for any resolve |
|
|
Needs to have the kidney fixed again |
7. Conclusion
This study seeks to explore the critical role of living kidney donation in the specific context of repeated kidney transplantation. Living kidney donations are recognized for their superior outcomes and their potential to expand the organ pool for patients with end-stage renal disease. However, their utilization remains limited, particularly in cases requiring second or subsequent transplants. Our research aims to address this gap by thoroughly analyzing the benefits and challenges associated with living kidney donation for such patients. We will investigate the medical advantages, including the potential for better graft survival rates and reduced wait times, which living kidney donations offer. Our study will also examine the psychosocial and emotional aspects, emphasizing the need for comprehensive support systems for both donors and recipients to manage the psychological impacts of transplantation. Economic and financial considerations are crucial in assessing the feasibility and success of living kidney donation programs. We will analyze the cost-effectiveness of these programs, particularly in reducing dialysis expenses and optimizing healthcare resources. Furthermore, our research will highlight the short- and long-term challenges faced by recipients of living donor kidneys, stressing the importance of continuous monitoring and tailored post-transplantation care to ensure optimal outcomes. We conclude from our literature review that several parameters that significantly improve center performance can be used to evaluate an effective living donor kidney transplant program. Living contributors significantly, first and foremost, grow the departed giver program, offering the likelihood to match exceptionally complex competitors and decrease generally holding up list times. Second, pre-emptive transplantation can be improved by customizing donor-recipient matches to ensure the best graft and patient outcomes. Thirdly, a significant community-wide benefit is the considerable savings in dialysis costs. To sustain a living donor program, careful donor evaluation and selection are essential. In order to stop organ trafficking and guarantee the donor's right to freely choose to donate, this procedure may involve independent donor advocacy. It seems reasonable to limit transplants using living donors to large-scale hubs in order to reduce donor threats. Additionally, suitable before and post-operative monitoring plans are highly recommended, perchance linking the gathering of data through nationwide and worldwide archives. This study aims to provide a inclusive considerate of the multifaceted aspects of living kidney donation in the context of repeated transplants, ultimately contributing to the enhancement of transplantation practices and policies.
References
1. Yang, J., Endo, Y., Munir, M. M., Woldesenbet, S., Altaf, A., Limkemann, A., ...&Pawlik, T. M. (2024). Waitlist time, age, and social vulnerability: impact on the survival benefit of deceased donor kidney transplantation versus long-term dialysis among patients with end-stage renal disease. Transplantation, 10-1097.
2. Goiffon, R. J., Depetris, J., Dageforde, L. A., &Kambadakone, A. (2024). Radiologic evaluation of the kidney transplant donor and recipient. Abdominal Radiology, 1-18.
Please view attached pdf to view all references
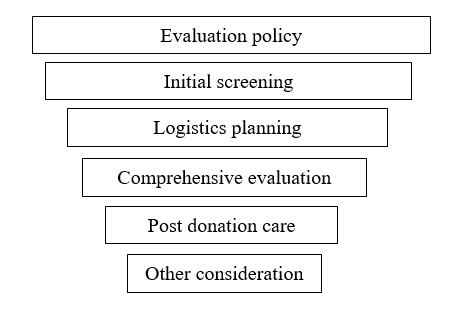
Figure 1
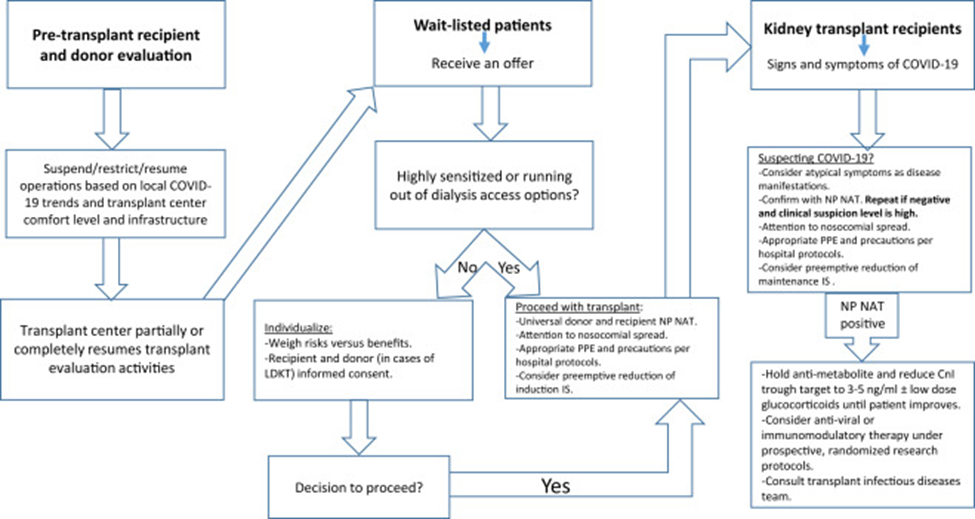
Figure 2
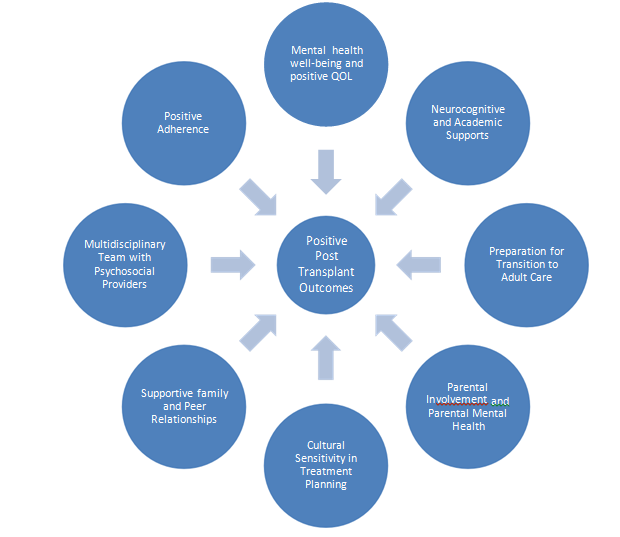
Figure 3
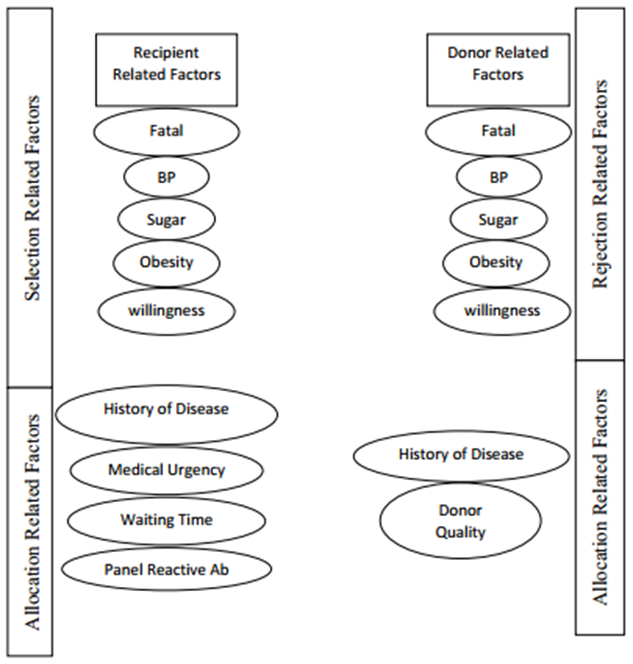
Figure 4
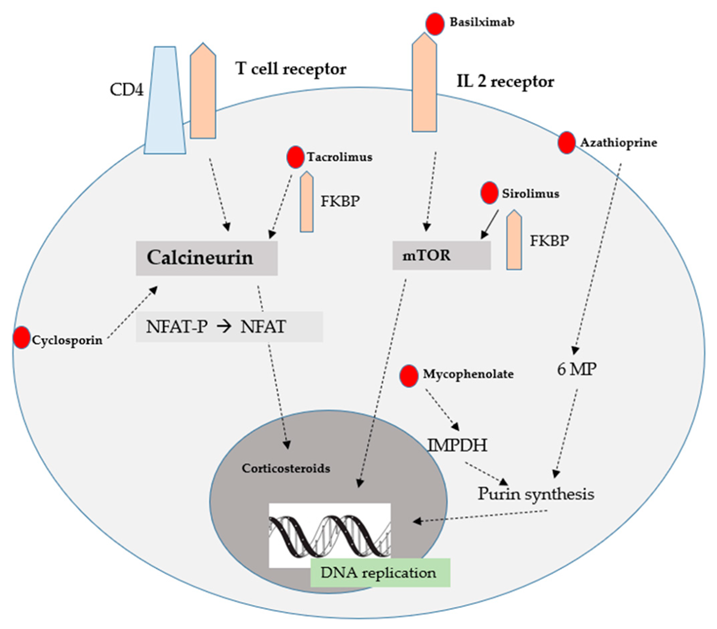
Figure 5
