The Subtle Storm: Identifying Incomplete Kawasaki Disease in Children
The Subtle Storm: Identifying Incomplete Kawasaki Disease in Children
Dr. Edwin Dias1, Dr.Keerthana Ramesh2, Pruthvi Ram3, Anika Rao4
1) Professor and Head, 2) Junior Resident, 3) Intern, 4) Intern.
Department of Paediatrics, Srinivas Institute of Medical Sciences and Research Centre, Mukka.
*Correspondence to: Dr Edwin Dias, Profesor and HOD Pediatrics.
Research Director SIMSRC PG clinical coordinator, Research Professor Srinivas University.
Copyright.
© 2025 Dr Edwin Dias This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 05 Aug 2025
Published: 20 Aug 2025
DOI: https://doi.org/10.5281/zenodo.17038409
Abstract
Incomplete Kawasaki disease (KD) poses a significant diagnostic challenge, particularly in pediatric patients who do not fulfill the classical diagnostic criteria[1]. Timely recognition and early initiation of therapy are crucial to prevent serious cardiovascular complications[2], especially coronary artery involvement.It is the leading cause of acquired heart disease in children in developed countries. The highest incidence is in Asia with almost 1 in a 100 children in Japan having the disease by age 5 [2]. In Africa, two cases were reported in South Africa in Caucasian children in 1980 but the first case in an African child was reported in Ivory Coast in 1981. Despite of sporadic cases being reported across many countries in Africa, mainly North Africa and the West African region, the epidemiological data for KD is limited for African countries [3,4,5].
The etiology of the disease remains unknown and several hypothesis exist in trying to explain the cause. Epidemiologic data suggest that an infectious agent may be causing the disease in genetically susceptible individuals [6]. The classic presentation of the disease occurs in children below 5 years. This suggests that there is an environmental trigger to which children mount an immune response after which the disease no longer manifests [7]. Postulated infectious agents include variants of normal flora which are induced by environmental factors such as improved hygiene [8].
Pathogenetic-mechanisms postulated to result in endothelial injury include that of a protein homeostasis system in which immune cells target pathogenic proteins bound to endothelial cells resulting in host cell injury [9]
We present a case of a 6-year-old child with prolonged fever, mucocutaneous manifestations, and elevated inflammatory markers, ultimately diagnosed with incomplete KD. Prompt treatment with intravenous immunoglobulin (IVIG) led to rapid clinical improvement and prevented coronary complications. This case underscores the importance of maintaining high clinical suspicion and initiating early management in children with atypical or incomplete presentations of Kawasaki disease.
KEYWORDS: Incomplete Kawasaki Disease, Pediatric vasculitis, IVIG, Coronary artery complications, Maculopapular rash.
The Subtle Storm: Identifying Incomplete Kawasaki Disease in Children
In children, Kawasaki disease is rarely reported(1,2). We herein report one such case.
Case Report
A 6-year-old male child presented with c/o of fever since 15 days & c/o rash since 10 days , on examination vitals were stable and systemic examination was normal.Routine investigations were sent and CRP was positive(21.1) and ESR was raised(40)
Child was clinically diagnosed as incomplete kawasaki disease and shifted to wards and was started on ecosporin and oral antibiotics and IVIG infusion was given over 10 hours and vitals were strictly monitored. LFT and RFT was sent and reports were normal.Serum electrolytes were sent and found to be normal Urine routine was sent and was normal 2d eho and US abdomen pelvis was done and found to be normal On day 3 of admission child had headache and vomiting for which symptomatic treatment was given.
On day 4 of admission child was taken to pediatric cardiologist opinion was taken for coronary studies and it was reported to be normal. Sr ferritin and Pro BNP was sent and was reported to be high. Blood culture sent showed no growth for 24 and 48hrs. Child was afebrile for 48 hours and hence dose of ecosporin was reduced.
Figure 1 :- Palmar erythema and peeling : Classic hand manifestation in Kawasaki disease
Figure 2 :- Perineal desquamation : Early mucocutaneous change in Kawasaki disease.
Discussion
Patient was apparently alright 15 days back after which he developed fever which was sudden in onset continuous high grade associated with chills and rigor and not relieved on medications. Mother c/o rash in the child on day 3 of fever ,acute in onset,maculopapular and erythematous first appearing on the neck and groin region and then trunk associated with itching. Rash over the hands and soles was also present which was painful. Child was admitted in a hospital as he was not getting better with oral symptomatic treatment. Rash subsided with skin peeling, pigmentation in 3-5 days and and as fever subsided child was discharged.
H/o redness and swelling of tongue and redness over the lips present. After an afebrile period of 4 days child developed fever again and rash over the palms and soles of the child.
H/o odynophagia since yesterday H/o travel 2 days back
H/o periungual desquamation
On evaluation, leukocytosis, thrombocytosis, elevated CRP and ESR, hypertriglyceridemia, hypercholesterolemia, and urine routine showed 4-8 pus cells/hpf. USG abdomen and pelvis was normal.
2 D Echo was done to look for coronary artery dilatation and was found to be normal.
Child was treated with IV immunoglobulin and aspirin.
Child responded within 48 hours of treatment and was discharged with low dose aspirin for 4 weeks. Follow-up echo was found to be normal. Early identification of incomplete Kawasaki disease is important for preventing complications from this disease.
Conclusion
This case highlights the importance of high clinical suspicion and timely management in children presenting with atypical features of Kawasaki disease. Early intervention with IVIG can significantly reduce morbidity, even in incomplete presentations.
Contributors: Authors were involved in case management and writing the manuscript.
Funding: None.
Competing interests: None stated.
References
[1] Li T, Feng J, Li N, Liu T. Correct identification of incomplete Kawasaki disease. The Journal of International Medical Research [Internet]. 2021 Mar 1;49(3):3000605211001712
[2] Kawasaki disease: two case reports from the Aga Khan Hospital, Dar es Salaam-Tanzania
[3] Badoe EV, Neequaye J, Oliver-Commey JO, et al. Kawasaki disease in Ghana: case reports from Korle Bu teaching hospital. Ghana Med J. 2011;45:38.
[4] Chemli J, Kchaou H, Amri F, Belkadhi A, Essoussi AS, Gueddiche N, Harbi A. Clinical features and course of Kawasaki disease in central Tunisia: a study about 14 cases collected over a period of three years (2000-2002). Tunis Med. 2005;83(8):477–83.
[5] Boudiaf H, Achir M. The clinical profile of Kawasaki disease in Algerian children: a single institution experience. J Trop Pediatr. 2016;62(2):139–43.
[6] Kim KY, Kim DS. Recent advances in Kawasaki disease. Yonsei Med J. 2016;57(1):15–21.
[7] Burgner D, Harnden A. Kawasaki disease: what is the epidemiology telling us about the etiology? Int J Infect Dis. 2005;9:185–94.
[8] Lee KY, Han JW, Lee JS. Kawasaki disease may be a hyperimmune reaction of genetically susceptible children to variants of normal environmental flora. Med Hypotheses. 2007;69(3):642–51.
[9] Lee KY, Rhim JW, Kang JH. Kawasaki disease: laboratory findings and an immunopathogenesis on the premise of a “protein homeostasis system”. Yonsei Med J. 2012;53(2):262–75.
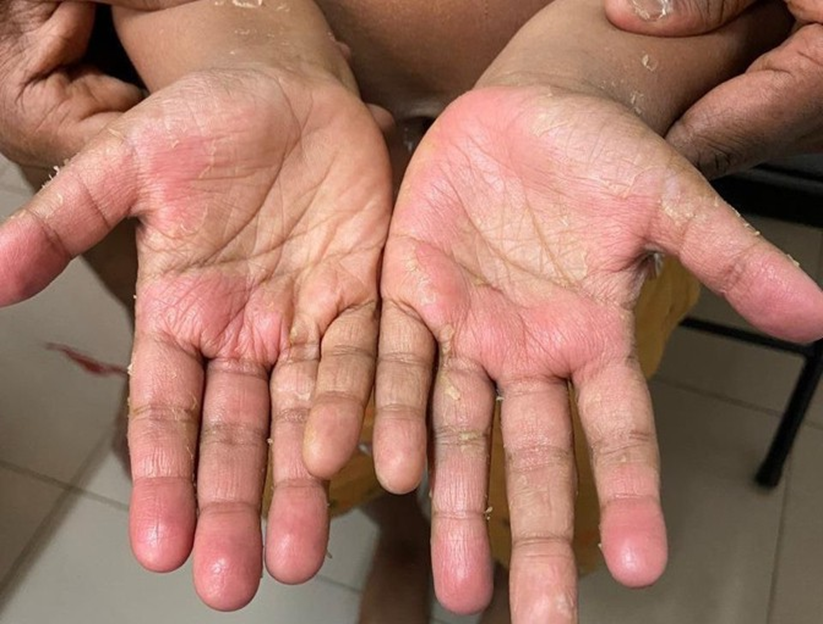
Figure 1

Figure 2
