Shared Decision Making, its Ethical Implications and Challenges, and its Impact on Patient Health Outcomes
Shared Decision Making, its Ethical Implications and Challenges, and its Impact on Patient Health Outcomes
Ibrahim Krenawi *1, Mimoun Azizi2
1-Ibrahim Krenawi, Consultant Neurologist, Burjeel Royal Hospital, Al Ain, UAE.
2-Mimoun Azizi, Chief Physician & Managing Chief Physician, Senior Consultant Neurologist and Neurogeriatrician, Klinikverbund Südwest, Sindelfingen, Germany.
*Correspondence to: Ibrahim Krenawi, Consultant Neurologist, Burjeel Royal Hospital, Al Ain, UAE.
Copyright
© 2025 Ibrahim Krenawi, This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: 05 Aug 2025
Published: 20 Aug 2025
DOI: https://doi.org/10.5281/zenodo.17043192
Abstract
Shared Decision Making (SDM) has been hailed as a foundational element of patient-centered care in clinical practice. It represents a new model of the physician-patient relationship built around evidence-based collaboration in decision-making. Instead of unilaterally exercising decision-making power, SDM empowers clinicians to make informed choices by actively involving patient preferences, values, and goals, thereby facilitating optimal medical decisions. This review examines the philosophical basis of SDM, including its ethical premises of autonomy, beneficence, and equity. It addresses real-life implementation issues such as time constraints, role adjustments for physicians, and gaps in patient readiness. Strategies for implementing SDM in regular practice are outlined, including validated decision aids, improved communication frameworks, and workflow-suitable tools.
Evidence gathered across specialties indicates that SDM is associated with increased adherence, decreased decisional conflict, improved patient-reported outcomes, and cost-saving, preference-concordant care. As healthcare systems transition to value-based reimbursement models, SDM is increasingly regarded as a standard for clinical performance. To realize its maximum potential, SDM must be ingrained in training regimens, documentation, and digital systems. This review situates SDM as a clinical ethic rather than merely a communication approach, underscoring its importance in providing high-quality, personalized, and ethically compatible medical care in contemporary settings.
Keywords: Shared Decision Making in clinical practice, Ethical implications of SDM, Patient-centered care models, Decision aids in medicine, Physician-patient communication, Improving patient outcomes through SDM.
|
Abbreviation |
Full Term |
|
ACP |
American College of Physicians |
|
ACP |
Advance Care Planning |
|
AHRQ |
Agency for Healthcare Research and Quality |
|
AMA |
American Medical Association |
|
BRAN |
Benefits, Risks, Alternatives, Doing Nothing |
|
CMS |
Centers for Medicare & Medicaid Services |
|
EHR |
Electronic Health Record |
|
EQ-5D |
EuroQol 5-Dimension Scale |
|
FACT-G |
Functional Assessment of Cancer Therapy – General |
|
HEDIS |
Healthcare Effectiveness Data and Information Set |
|
IPDAS |
International Patient Decision Aid Standards |
|
NCI |
National Cancer Institute |
|
NCQA |
National Committee for Quality Assurance |
|
NHS |
National Health Service |
|
PROMs |
Patient-Reported Outcome Measures |
|
RCT |
Randomized Controlled Trials |
|
SDM |
Shared Decision Making |
|
WHO |
World Health Organization |
Shared Decision Making, its Ethical Implications and Challenges, and its Impact on Patient Health Outcomes
Introduction
Shared Decision Making (SDM) involves patients and clinicians collaborating to make healthcare choices, integrating clinical evidence and patient preferences. SDM has emerged as a fundamental paradigm in contemporary clinical practice, representing a collaborative process where both clinician and patient contribute to healthcare decisions. This model moves away from paternalism toward patient-centered care. Rather than acting unilaterally, the clinician assumes the role of a clinical guide—synthesizing current evidence, evaluating diagnostic and therapeutic trade-offs, and aligning those with the patient’s individual goals, values, and preferences.
The ethical principle of respected patient autonomy serves as the origin of SDM. This model contrasts with traditional paternalism, where decision-making was frequently dominated by medical authority. Within SDM, the patient and physician work together to make complex clinical decisions, especially in situations where there is no single optimal management pathway. Examples include chronic illness care, end-of-life care, elective procedures, and pharmacologic cases with risk-benefit considerations.
Integrating SDM into regular practice is not merely hypothetical; it is a clinical reality gaining increasing acceptance. SDM is now a focus of national guidelines, professional societies, and quality-based reimbursement models that identify it as an essential aspect of ethical and effective care. Nonetheless, translating these principles into practice presents challenges, including time pressures, workflow inconsistencies, physician uncertainty, and patient decisional burdens.
This review discusses the background of Shared Decision Making, its ethical aspects, implementation issues, and its effects on patient health outcomes. SDM is presented not merely as a communication strategy but as a clinical ethic rooted in high-quality, outcome-focused care.
Figure 1
Core Principles of Shared Decision Making
SDM is not just a discussion but rather a structured clinical interaction that integrates the best available evidence with the values and goals informed by the patient. At its heart, SDM relies on three key aspects:
1. Clear and balanced presentation of evidence-based options.
2. Exploration of patient values and preferences.
3. A mutually agreed-upon care decision, documented and actionable.
Elwyn and colleagues (2000) introduced a competence-based SDM framework, defining the decision problem, acknowledging equipoise, conveying options, and supporting deliberation—measured using the OPTION scale (e.g., Health Expectations, 2005) [1].
In 2017, the Agency for Healthcare Research and Quality (AHRQ) emphasized that SDM requires clinicians and patients to jointly participate in the decision-making process, arriving at a treatment plan based on clinical evidence and the patient’s informed preferences [2]. This contrasts sharply with information-only models or consent-driven approaches that occur late in the decision cycle.
Bidirectional Communication
Montori and colleagues (2019) developed conversation aids for SDM in chronic disease contexts, drawing from service design and video analysis, thus shifting SDM toward collaborative problem-solving tailored to patients' real-life contexts [3].
SDM is based on bidirectional communication. Doctors are responsible for interpreting complex and often probabilistic information into comprehensible and unvarnished forms. The role extends beyond simply informing; it involves contextualizing information, quantifying risks, and addressing uncertainties openly. For instance, in the treatment of localized prostate cancer, each treatment type may not universally have an advantage over others; the patient's risk tolerance, functional priorities, and psychosocial background all influence the most suitable method [4].
Evidence + Individual Values = Clinical Decision
In a 2020 position statement, the American College of Physicians argued that SDM is enhanced when clinicians clarify at the beginning of the encounter that patient goals are sought [5]. For example, in managing congestive heart failure, two patients with identical clinical parameters may choose different paths: one prioritizes survival, while the other emphasizes symptomatic burden and quality of life. The physician's role is to elucidate these preferences and ensure the chosen therapy aligns with them.
Contextual Suitability
While SDM can be employed in various care settings, it is especially crucial in preference-sensitive conditions where multiple reasonable treatment options exist. These include:
- Preventive screening decisions (e.g., PSA screening, mammography in older adults)
- Drugs with significant benefit-risk profiles (e.g., anticoagulation in older patients with atrial fibrillation)
- Tools and decision aids
- Goals of care discussions in oncology, geriatrics, and palliative care
In 2021, the National Quality Forum listed SDM as a “quality indicator” of value-based care models in cases of clinical equipoise [6]. This signifies a systemic shift towards evaluating outcomes based on decision quality, patient understanding, concordance of preferences, and decisional satisfaction.
Role of Decision Aids and Tools
One of the key components of SDM is the use of decision support tools, including option grids, risk calculators, and visual probability charts. These tools minimize conflicts in decision-making, enhance understanding, and ensure that trade-offs are well understood before care plans are finalized. However, these tools are not intended to replace clinical judgment or the interpersonal dialogue between physician and patient.
Fig 2
Ethical Implications of Shared Decision Making
SDM is not merely a communication framework; it is an ethical obligation grounded in respect for patient autonomy, clinical integrity, and equitable care delivery. Its moral relevance becomes particularly pronounced in scenarios characterized by therapeutic ambiguity, life-altering consequences, or divergent patient values. In these contexts, SDM serves as the mechanism through which ethically responsible medicine is practiced.
Autonomy Without Abandonment
SDM operationalizes respect for patient autonomy, but not in isolation. Unlike traditional informed consent, where patients interpret complex choices alone, SDM involves the physician at every step. The clinician does not merely present information but also guides interpretation by contextualizing risks, ensuring that the final decision is clinically sound and ethically aligned with the patient’s values [7].
In 2020, the Hastings Center emphasized that SDM addresses both paternalism and abandonment, noting that in high-stakes decisions, providing a list of choices without interpretation does not enhance autonomy. Patients must be actively assisted through value clarification and decisional coaching [8].
Balancing Beneficence and Respect for Values
The ethical dilemma of balancing physician-based beneficence and patient-defined priorities is central to SDM [9]. There are instances where the medically optimal course of action, as dictated by guidelines, may be unacceptable to the patient. For example, a patient with advanced COPD may prioritize avoiding hospitalization over aggressive treatment, preferring to receive supportive care that maximizes their quality of life.
The ethical responsibility of the physician in such scenarios lies not only in recognizing that patient preferences may diverge from clinical recommendations but also in ensuring that patients are informed about the clinical implications of those preferences, allowing them to exercise autonomy within medically appropriate boundaries.
Avoiding Coercion and Preserving Neutrality
True SDM should not involve implicit coercion arising from imbalanced language, risk-framing bias, or unconscious gestures that convey the clinician's preferences. According to a 2019 report in the Journal of Medical Ethics, framing effects, especially in high-stress decision-making situations, can heavily influence patient decisions, often without their awareness [10]. Ethical SDM necessitates neutral communication grounded in evidence and free of the physician’s personal biases.
Equity and Ethical Access
Equity in SDM encompasses not only access to care but also linguistic access, health literacy facilitation, and cultural concordance. Shahar (2021) argued that without computational decision support, SDM models face ethical challenges due to cognitive limitations. He proposed a three-way model involving the patient, clinician, and decision support systems.
Cognitively impaired patients, those with limited health literacy, or non-English speakers are at a heightened risk of meaningful exclusion, despite being those who stand to benefit the most from SDM. In 2025, a research organization emphasized that ethical SDM should be supported by adaptive communication plans, including translated decision aids, trained interpreters, and cultural liaisons to avoid disparities in decision quality.
Challenges in Implementing Shared Decision Making
Despite its clinical relevance and ethical foundation, SDM remains inconsistently implemented in real-world settings. Numerous systemic, interpersonal, and cognitive barriers hinder its full integration into routine clinical care [11]. These challenges do not merely reflect logistical inefficiencies—they undermine the ethical and therapeutic integrity of physician-patient partnerships, particularly in complex, time-pressured environments.
Time Constraints and Workflow Disruption
Gravel, Légaré, and Graham (2006) conducted a systematic review of health professionals' perceptions, identifying barriers such as time constraints and lack of training, as well as facilitators like decision aids and organizational support [12]. The use of SDM is often perceived as an obstacle due to time limitations during clinical visits, particularly in high-volume practices where diagnostic throughput takes precedence over discussion. A 2022 national survey by the American Medical Association reported that over 65% of physicians felt unable to allocate adequate time for comprehensive decision discussions, especially when navigating multi-option treatment plans [13]. This lack of time often leads to expedited consent processes rather than genuine, preference-generating decisions.
Additionally, the preparations required for SDM, including the availability of decision aids and follow-up support, may not easily integrate into existing EHRs or clinic routines.
Physician Reluctance and Role Identity
A systematic review in 2018 across 32 studies revealed that SDM during surgical consultations is still emerging. While patients reported higher perceived involvement than surgeons, objective scores (like using the OPTION instrument) were low (7–39%) [14].
Although many clinicians conceptually agree with SDM, applying it in practice can be uncomfortable, as it challenges traditional physician authority. Clinicians trained in a model emphasizing professional absolutes and protocols may find it disconcerting to encourage uncertainty and disagreement with patients. A qualitative study in BMJ Open found that some clinicians believed SDM risks undermining clinical expertise when patients choose options that conflict with evidence-based practices [15].
Furthermore, the shift from being the “decision-maker” to a decision facilitator necessitates not only communication skills but also cognitive flexibility and cultural humility—competencies not universally emphasized in medical training.
Patient-Related Barriers
Not every patient is ready or willing to engage in complex medical decisions. Limited health literacy, decisional fatigue, anxiety, or cognitive impairment may significantly restrict meaningful engagement [16]. For example, new cancer patients may be emotionally distraught, impairing their ability to process information and make decisions.
In 2023, the National Cancer Institute advised clinicians to revisit decisions across multiple visits, particularly in preference-sensitive scenarios, to mitigate the risk of patients making choices under distress or incomplete knowledge [17].
Frerichs et al. (2016) qualitatively studied oncology providers and identified similar challenges: complex clinical workflows and resistance to change impede SDM adoption. In some cultural settings, patients may defer all decision-making authority to the doctor or relatives, viewing this as a courtesy rather than submissiveness. This context necessitates an SDM that is adaptable and culturally competent rather than rigidly applying Western autonomy models.
Institutional and System-Level Limitations
Healthcare systems often lack the infrastructure to support SDM, including:
- Absence of uniform documentation guidelines on SDM
- Limited access to culturally appropriate decision aids
- Reimbursement mismatches that incentivize quantity over individualized care.
Ankolekar et al. (2020) explored barriers and facilitators of implementing decision aids in prostate cancer, highlighting time pressure, structural constraints, training needs, and economic incentives as key factors [18]. In 2020, the Centers for Medicare & Medicaid Services (CMS) implemented reimbursement codes related to SDM activities, particularly in cardiovascular and end-of-life care. However, adoption remains low, partly due to administrative burdens and low clinician awareness.
Integrating SDM into quality metrics, clinical education, and payment structures is essential for fostering widespread adoption.
Impact of Shared Decision Making on Patient Health Outcomes
The clinical value of SDM extends beyond patient satisfaction or ethical compliance; it is directly linked to tangible improvements in health outcomes, adherence, decision quality, and healthcare resource utilization. Numerous studies across specialties demonstrate that when patients are actively engaged in their care decisions, outcomes become more aligned, sustainable, and preference-concordant, especially in chronic disease management, oncology, and surgical care.
A systematic review by Shay & Lafata (2015) revealed mixed results: among 11 RCTs, five showed positive effects of SDM, one showed delayed improvement, and five showed no difference. SDM appeared most beneficial in long-term or chronic decision contexts.
Enhancement of Treatment Adherence and Engagement
One of the most frequently reported benefits of SDM is the increased adherence to prescribed medical treatments. When patients actively participate in their care journey, they are more likely to adhere to chronic condition management, which often requires long-term commitment.
In 2020, a meta-analysis involving over 100 randomized controlled trials published in Patient Education and Counseling found that SDM interventions resulted in higher adherence by approximately 17-20% [19]. This can be attributed to the alignment of prescribed regimens with the patients' lifestyle priorities, reducing perceived burden and reluctance toward treatment.
Reduction in Decisional Conflict and Regret
Decisional conflict, which reflects the degree of uncertainty among different courses of action, is a reliable predictor of low satisfaction, anxiety, and treatment discontinuation. SDM effectively reduces this phenomenon through value clarification, personalized risk communication, and less ambiguous decision-making.
The Cochrane Collaboration published a systematic review of decision aids used in SDM in 2019, concluding that patients who underwent the structured SDM process reported lower levels of decisional conflict, had more accurate risk perceptions, and were less likely to experience regret post-intervention. These results were particularly robust in areas of cancer screening, surgical decision-making, and reproductive health.
Improved Patient-Reported Outcome Measures (PROMs)
In addition to classic clinical endpoints, SDM significantly enhances Patient-Reported Outcome Measures, including symptom control, emotional well-being, functional status, and quality of life. Patients participating in structured SDM processes reported improvements in the following aspects:
- Higher quality-of-life scores (FACT-G and EQ-5D) [20].
- Lower rates of depression and anxiety
- Increased satisfaction with care, regardless of treatment aggressiveness.
These findings suggest that SDM fosters better psychological preparation, even in situations with clinically undesirable outcomes, as it provides patients with a sense of agency and informed control over their care decisions.
Optimization of Resource Utilization and Cost-Effective Care
SDM is also instrumental in reducing low-value or unnecessary medical treatments. With comprehensive information on risks, alternatives, and probable outcomes, patients often prefer less invasive or conservative treatments, particularly in preference-sensitive cases. This not only enhances safety but also aligns with cost-effective care delivery.
For instance, a 2021 article in the New England Journal of Medicine reported that SDM reduced elective cardiac catheterizations by over 20% in patients with stable angina when alternative medical therapies were presented[21].
A 2023 meta-analysis indicated that SDM interventions in cardiology significantly reduced decisional conflict and increased patient knowledge compared to usual care.
Similarly, orthopedic studies have shown that total joint arthroplasty rates decrease among undecided patients once non-operative options are adequately explained.
Barradell et al. (2023) reviewed SDM interventions for chronic respiratory disease (e.g., pulmonary rehabilitation). Across eight studies (n = 1,596), interventions—typically involving decision aids, training, and consultation prompts—improved decision-making and health-related outcomes, though evidence quality varied [22].
These findings indicate a trend toward aligning care intensity with patient preferences, resulting in more effective use of healthcare resources, reduced procedure-related morbidity, and fewer lawsuits due to greater transparency.
Alignment with Value-Based Care Metrics
As healthcare transitions toward value-based reimbursement models, SDM is increasingly recognized as a standard for clinical performance. In 2022, the National Committee for Quality Assurance (NCQA) incorporated SDM elements into the Healthcare Effectiveness Data and Information Set (HEDIS) metrics, specifically in:
- Documentation of consensus decisions regarding statin treatment in elderly patients.
- Advance care planning for end-of-life care.
- Lung cancer screening among high-risk individuals.
These measures incentivize clinicians and health systems to involve patients in high-quality decision-making processes, creating evidence-based documentation. This trend influences the future of outcome-driven care, equipment, and technology.
Clinical Strategies to Enhance Shared Decision Making
To effectively implement Shared Decision Making (SDM) in clinical settings, it must be integrated into working processes, taught to medical professionals, and developed into structured protocols. The following evidence-based interventions can be applied across various clinical practices:
Early Identification of Decision Points
Clinicians should learn to identify decisional moments early in the patient interaction process, particularly during the diagnostic or staging phases. Framing decisions early allows for a more deliberative approach rather than a reactive one. In 2021, the Mayo Clinic highlighted that decisions framed early can enhance deliberation, particularly in oncology, cardiology, and surgical specialties [23].
To support this, electronic health records (EHRs) can be programmed to identify preference-sensitive scenarios, such as elective procedures and palliative care transitions, prompting clinicians to engage in SDM practices.
Use of Validated Decision Aids
Effective SDM relies on structured, evidence-based tools that summarize risks, benefits, and alternatives without distorting information. These tools should complement, not replace, clinical dialogue. In 2022, the International Patient Decision Aid Standards (IPDAS) Collaboration reiterated the principles of effective decision aids:
- Present absolute risk estimates, not just relative risks.
- Be culturally and linguistically tailored
- Include value clarification components, not solely option listings.
- Be tested for comprehension and neutrality.
Examples include:
- Option grids: for prostate cancer, knee osteoarthritis, and breast reconstruction
- Statin Choice™ for post-cardiovascular prevention.
- Ottawa Personal Decision Guides for primary care settings.
Embedding these tools into EHRs or patient portals facilitates pre-visit preparation, reduces decisional burden during visits, and enhances post-visit information retention.
Structured Communication Frameworks
Communication models promote consistency and address all aspects of SDM. One common model is the Three-Talk Model:
1. Team Talk - Establishing a partnership and recognizing the need for a decision.
2. Option Talk - Presenting evidence-based options with associated benefits and trade-offs.
3. Decision Talk - Assisting with preference clarification and finalizing the course of action.
Elwyn et al. developed this model, which is now utilized by health systems such as the NHS and Kaiser Permanente to train providers across various disciplines, including emergency medicine and primary care.
Another useful tool is the BRAN framework, which involves Benefits, Risks, Alternatives, and doing Nothing to ensure that discussions are thorough and unbiased.
Physician Skill-Building and Simulation Training
SDM is not an inherent ability but a clinical skill that can be learned. Interventions aimed at enhancing medical professionals' abilities to communicate risks and disclose uncertainties have been shown to improve physician confidence and patient satisfaction. In 2023, Stanford University introduced simulation-based SDM training for internal medicine residents, resulting in:
- Increased documentation of SDM in real cases
- Improved decision-related comprehension among patients
- More frequent use of visual aids and clarifying questions during consultations
Training should emphasize not only content delivery but also the tone, framing bias, and decisional neutrality, which are fundamental aspects of ethically competent SDM.
Documentation and Quality Monitoring
For SDM to impact clinical outcomes and reimbursement, it needs to be measurable and auditable. Documentation should include:
- The clinical options discussed.
- The decision aid(s) used.
- The values elucidated by patients
- The final decision made and the rationale behind it.
In 2021, CMS introduced billing codes (e.g., CPT 99497, 99498) for advanced care planning and SDM conversations, provided that adequate documentation is available. Integrating SDM checklists into EHR templates can support compliance, quality reporting, and legal protection.
Conclusion
Research into Shared Decision Making (SDM) spans multiple domains—cardiology, respiratory health, surgery, mental health, and advance care planning—with generally positive but context-dependent outcomes. SDM appears most beneficial in chronic or complex decision scenarios, though evidence quality and consistency vary.
SDM has evolved from a theoretical ideal to a clinical requirement rooted in ethics and accountability, patient autonomy, and outcomes-based care. Its incorporation enhances compliance, reduces choice regret, and improves patient-reported outcomes and healthcare efficiency.
However, significant barriers remain, including time constraints, clinician reluctance, systemic inertia, structural limitations, and individual patient differences. Implementation may benefit from multifaceted strategies that include training, policy support, decision aids, and computational tools.
SDM is not merely a communication tool; it is a systematic, evidence-based process that requires clinical discipline, ethical awareness, and adaptation to workflow. Innovative directions include integrating SDM with advance care planning and leveraging decision-support technologies and user-centered design to enhance SDM’s effectiveness and ethical implementation.
As value-based care models increasingly dictate the provision of care, SDM should be considered an integral component of medical education, quality indicators, and digital ecosystems. Rosca et al. (2023) not only reviewed but also proposed a novel integrative model combining SDM and advance care planning to improve patient-centered, informed, iterative care decisions.
The authority of physicians to unilaterally decide on treatments has diminished; the future lies in shared decision-making, where the roles of clinicians and patients converge as collaborators. SDM is no longer optional; it represents the new standard of quality, precision, and individualization in modern medicine.
References
1. Nornor-Quadjie, M. (2023). The Normative Requirement for Shared Decision Making (SDM) in Healthcare Ethics.
2. AHRQ. (n.d.). Retrieved from https://www.ahrq.gov/sdm/about/index.html (https://www.ahrq.gov/sdm/about/index.html)
3. Yin, S., Chen, Y., Ding, S., Zhang, Z., & Huang, S. (2022). Crosstalk-aware routing, spectrum, and core assignment based on AoD nodes in SDM-EONs with bidirectional multicore fibers. Optical Switching and Networking, 43, 100647.
4. Hargraves, I.G., Fournier, A.K., Montori, V.M., & Bierman, A.S. (2020). Generalized shared decision-making approaches and patient problems: Adapting AHRQ’s SHARE Approach for Purposeful SDM. Patient Education and Counseling, 103(10), 2192-2199.
5. National Quality Forum. (2021). Retrieved from https://www.qualityforum.org/Projects/n-r/Patient_Experience_and_Function/Final_Report_-_Spring_2021_Cycle.aspx (https://www.qualityforum.org/Projects/n-r/Patient_Experience_and_Function/Final_Report_-_Spring_2021_Cycle.aspx)
6. Alfaro-LeFevre, R. (2016). Critical thinking, clinical reasoning and clinical judgment: A practical approach, pageburst E-book on Kno. Elsevier Health Sciences.
7. Mohamed, S. (2024). Clinical ethics and patient-centered communication: Evidence-based application through an educational perspective [Preprint]. doi:10.2139/ssrn.4961228.
8. Kass, J.S., & Rubin, M.A. (2023). Medicolegal and ethical issues in neurology. Neurologic Clinics, 41(3), i. doi:10.1016/s0733-8619(23)00045-2.
9. Pope, T.M. (2017). Certified patient decision aids: Solving persistent problems with informed consent law. Journal of Law, Medicine & Ethics, 45(1), 12-40.
10. Journal of Medical Ethics. (n.d.). Retrieved from https://jme.bmj.com/ (https://jme.bmj.com/)
11. Song, C. (2025). Formulating Ethical Frameworks for Translators in Medical Technology. Pacific International Journal, 8(1), 01-06.
12. Moleman, M., Regeer, B.J., & Schuitmaker-Warnaar, T.J. (2020). Shared decision-making and the nuances of clinical work: Concepts, barriers and opportunities for a dynamic model. Journal of Evaluation in Clinical Practice, 27(4), 926-934. doi:10.1111/jep.13507.
13. American Medical Association. (2020). What’s the role of time in shared decision-making? Retrieved from https://journalofethics.ama-assn.org/article/whats-role-time-shared-decision-making/2020-05 (https://journalofethics.ama-assn.org/article/whats-role-time-shared-decision-making/2020-05)
14. BMJ Open. (2019). Retrieved from https://bmjopen.bmj.com/content/14/6/e080765 (https://bmjopen.bmj.com/content/14/6/e080765)
15. Grignoli, N., et al. (2025). Clinical decision fatigue: A systematic and scoping review with meta-synthesis. Family Medicine and Community Health, 13(1). doi:10.1136/fmch-2024-003033.
16. National Cancer Institute. (2023). Retrieved from https://www.cancer.gov/about-cancer/coping/adjusting-to-cancer/communication-hp-pdq (https://www.cancer.gov/about-cancer/coping/adjusting-to-cancer/communication-hp-pdq)
17. Centers for Medicare & Medicaid Services. (2020). Retrieved from https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleid=53775&ver=34&bc=0 (https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleid=53775&ver=34&bc=0)
18. Hamilton, J.G., et al. (2017). What is a good medical decision? A research agenda guided by perspectives from multiple stakeholders. Journal of Behavioral Medicine, 40(1), 52-68.
19. Collins, E.F., et al. (2025). Top ten tips palliative care clinicians should know about end-of-life doulas. Journal of Palliative Medicine, 28(6), 808-814.
20. Tay, Y.J.E. (2019). The behavioral aspects of shared decision-making (Doctoral dissertation, University of Warwick).
21. Niburski, K., et al. (2020). Shared decision-making in surgery: A meta-analysis of existing literature. The Patient-Patient-Centered Outcomes Research, 13(6), 667-681.
22. Hallenbeck, H.W. (2020). Decision-Making Difficulty in Major Depression: Understanding Indecisiveness and the Role of Expected Affect (Doctoral dissertation, Washington University in St. Louis).
23. Stalnikowicz, R., & Brezis, M. (2020). Meaningful shared decision-making: A complex process demanding cognitive and emotional skills. Journal of Evaluation in Clinical Practice, 26(2), 431-438.
24. New England Journal of Medicine. (n.d.). Retrieved from https://www.nejm.org/ (https://www.nejm.org/)
25. National Committee for Quality Assurance. (n.d.). Retrieved from https://www.ncqa.org/hedis/ (https://www.ncqa.org/hedis/)
26. Meyer, A.N.D., et al. (2021). Patient and clinician experiences of uncertainty in the diagnostic process: Current understanding and future directions. Patient Education and Counseling, 104(11), 2606–2615. doi:10.1016/j.pec.2021.07.028.
27. Mayo Clinic. (2025). Beyond the code: Advancing early pancreatic cancer diagnoses. Retrieved from https://cancerblog.mayoclinic.org/2025/04/15/beyond-the-code-advancing-early-pancreatic-cancer-diagnoses/ (https://cancerblog.mayoclinic.org/2025/04/15/beyond-the-code-advancing-early-pancreatic-cancer-diagnoses/)
28. Hulpke, J.F., & Fronmueller, M.P. (2020). Review of evidence-based management: How to make better organizational decisions by Eric Barends and Denise Rousseau. Journal of Business Ethics, 164(2), 417–419. doi:10.1007/s10551-020-04488-3.
29. Centers for Medicare & Medicaid Services. (2020). Retrieved from https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleid=58664 (https://www.cms.gov/medicare-coverage-database/view/article.aspx?articleid=58664)
30. Shay, L.A., & Lafata, J.E. (2015). Shared decision-making in chronic disease: A systematic review. Patient Education and Counseling, 98(12), 1454-1466.
31. Cardiology (Meta-analysis, 2023) Reduced decisional conflict; increased patient knowledge.
32. Respiratory Diseases: Barradell et al. (2023). SDM interventions improved outcomes; evidence quality varied.
33. Surgery (2018 review): SDM limited; patients more engaged than surgeons.
34. Mental Health (2021 review): Wide diversity in interventions; need for standard measures.
35. Advance Care Planning: Rosca et al. (2023). Proposed integrated SDM + ACP model.
36. Barriers & Facilitators: Gravel et al. (2006); Frerichs et al. (2016); Ankolekar et al. (2020). Identified systemic, training, and incentive-related challenges.
37. Innovation & Ethics: Shahar (2021); Montori et al. (2019). Advocated computational support and user-centered conversation aids.
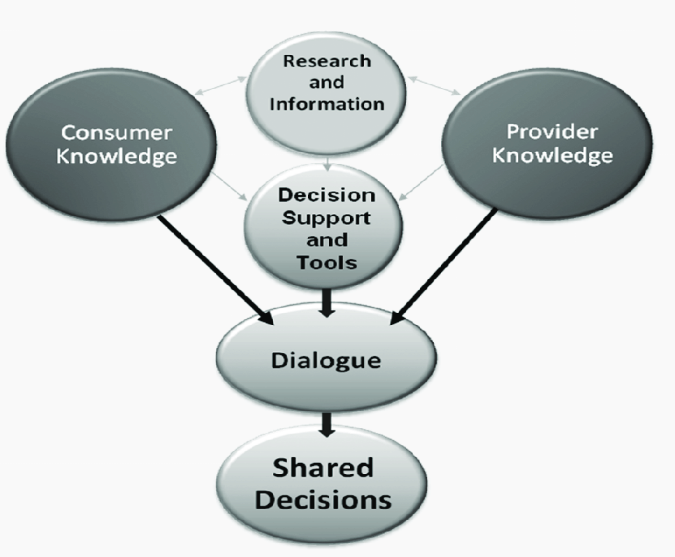
Figure 1
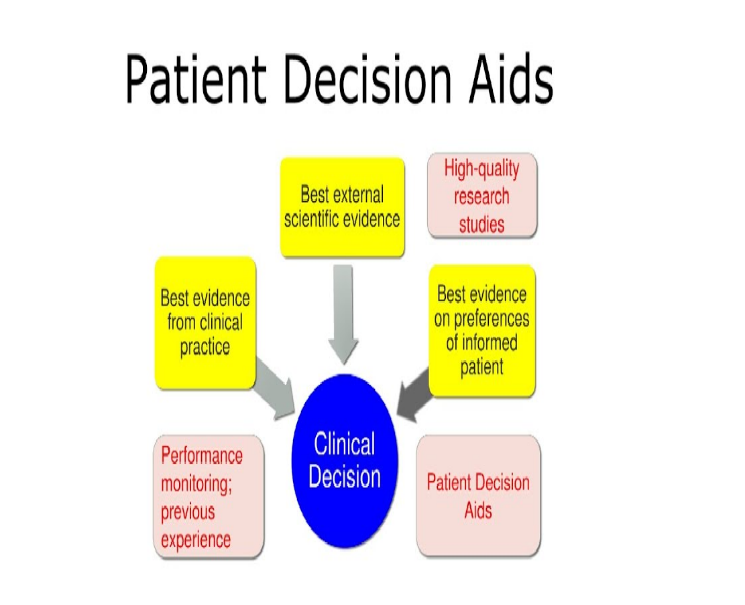
Figure 2
